How to Manage Stress for Better Long-Term Health

Last updated: May 4, 2026
Quick Answer
Chronic stress is not just a mental inconvenience — it is a documented driver of heart disease, high blood pressure, diabetes, depression, and a range of other serious conditions. Managing stress for better long-term health means addressing it consistently through sleep, movement, nutrition, social connection, and, where needed, professional support. Manage stress, there is no single fix, but the evidence is clear: small, sustained habits produce real, measurable health benefits over time.
Key Takeaways
- Chronic stress disrupts nearly every body system, raising cortisol and adrenaline levels in ways that damage the heart, gut, immune system, and brain over time [1]
- Regular exercise is one of the most effective stress-reduction tools available — the American Heart Association recommends at least 150 minutes of moderate-intensity activity per week [6]
- Sleep is not optional — adults need 7–9 hours per night; poor sleep raises cortisol and worsens every stress-related health outcome [6]
- Diet matters more than most people realise — whole foods, lean proteins, and vegetables support stress recovery; ultra-processed foods and excess sugar worsen it [4]
- Social connection is a genuine buffer against stress, not just a lifestyle preference [3]
- Mindfulness, deep breathing, and journaling have real evidence behind them — they are not fringe practices [1]
- Professional help is appropriate when self-management is not enough — this is not a sign of failure [5]
- The basics still do the heavy lifting — sleep, movement, food, and connection consistently outperform supplements and quick fixes
Table of Contents
- What Does Chronic Stress Actually Do to the Body?
- Why Most People Underestimate Stress as a Health Risk
- How to Manage Stress for Better Long-Term Health: The Core Strategies
- The Role of Social Connection in Long-Term Stress Management
- How Mindful Eating Connects to Stress Management
- When to Seek Professional Help for Stress
- Building a Practical Stress Management Plan That Actually Sticks
- What Effective Stress Management Actually Delivers
- FAQ: How to Manage Stress for Better Long-Term Health
- Conclusion: What Actually Works Over Time
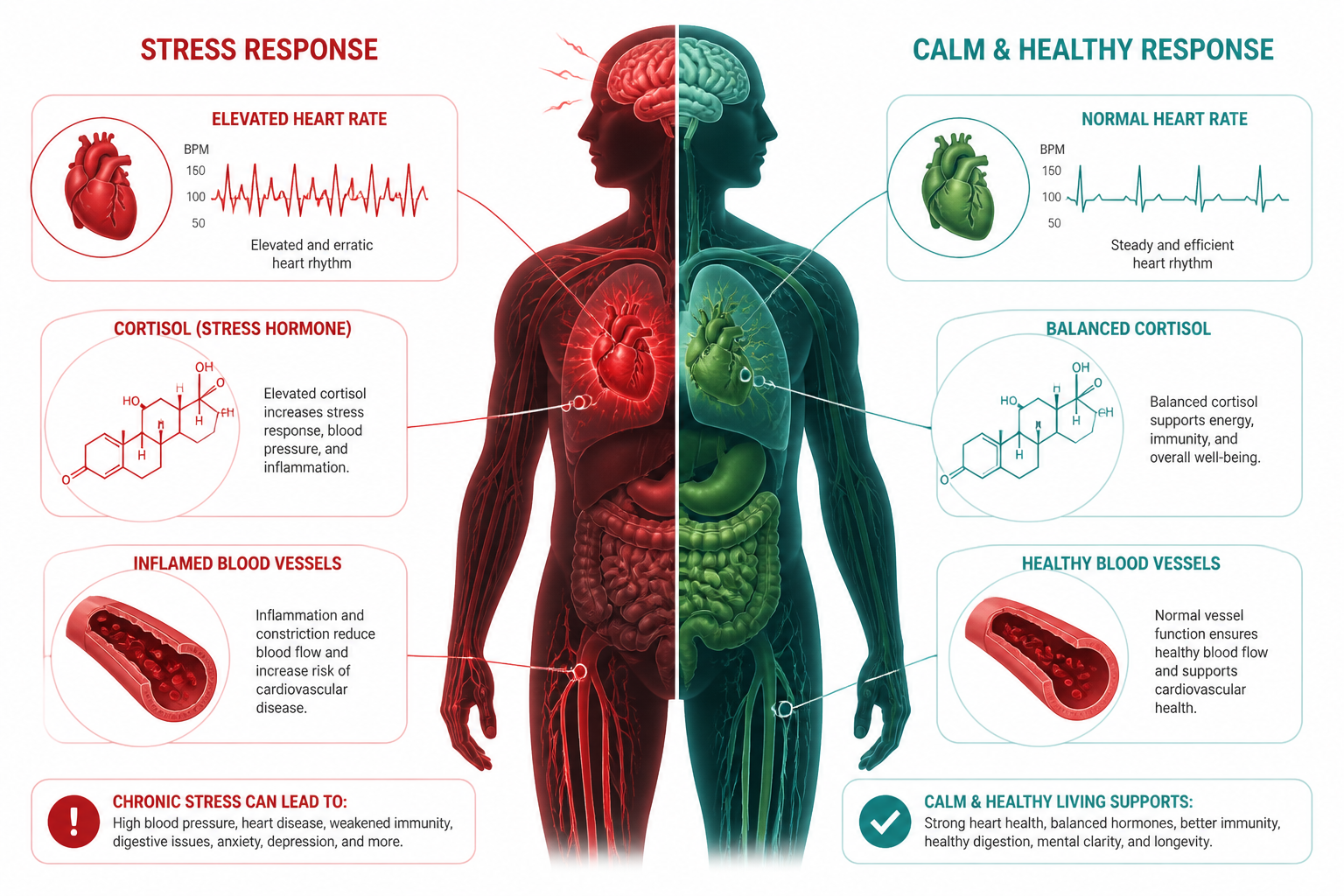
What Does Chronic Stress Actually Do to the Body?
Chronic stress is not the same as feeling pressured before a deadline. It is a sustained physiological state where the body’s stress response system stays partially activated for weeks, months, or years. That distinction matters because the health consequences are very different.
In the short term, stress hormones — primarily cortisol and adrenaline — are useful. They sharpen focus, increase heart rate, and prepare the body to respond to a threat. The problem starts when that response never fully switches off.
Here’s the real issue: long-term cortisol exposure disrupts nearly all body systems. According to the Mayo Clinic, chronic stress is directly linked to anxiety, depression, digestive problems, heart disease, high blood pressure, stroke, sleep problems, weight gain, and cognitive difficulties [1]. The NIH adds that chronic stress cannot be resolved through normal body functioning alone — it requires deliberate intervention [7].
What the body experiences under chronic stress:
| Body System | Effect of Chronic Stress |
|---|---|
| Cardiovascular | Raised blood pressure, increased heart disease risk |
| Immune | Weakened immune response, slower recovery |
| Digestive | Gut inflammation, IBS symptoms, appetite changes |
| Endocrine | Elevated cortisol, disrupted blood sugar regulation |
| Mental health | Anxiety, depression, reduced concentration |
| Reproductive | Reduced sex drive, hormonal disruption |
| Sleep | Difficulty falling and staying asleep |
The American Heart Association notes that negative psychological health is associated with increased cardiovascular risk, while positive psychological health is linked to lower risk of heart disease and death [3]. That is a strong claim, but it is backed by consistent evidence across multiple large studies.
The main takeaway is this: chronic stress is a physical health problem, not just a mental one. Treating it seriously is not optional if long-term health matters to you.
Why Most People Underestimate Stress as a Health Risk
Most adults recognise that stress feels unpleasant. Far fewer connect it directly to their blood pressure reading, their digestive problems, or their weight. That gap between perception and reality is where a lot of preventable damage happens.
In plain English: stress does not just make you feel worse. It makes you biologically worse off. Weill Cornell Medicine points out that long-term stress leads to measurable physical outcomes including high blood pressure and loss of sex drive, alongside mental health consequences like anxiety and depression [2]. These are not vague quality-of-life complaints — they are clinical findings.
This is where hype gets in the way. A lot of wellness content frames stress management as self-care or lifestyle optimisation. That framing undersells the problem. Learning how to manage stress for better long-term health is closer to managing a chronic risk factor — like diet or physical activity — than it is to booking a spa day.
“Stress is not a weakness. It is a physiological process that, when left unmanaged, creates measurable harm. Treating it like a background inconvenience is a mistake.”
The people most at risk of underestimating stress tend to be those who are highly functional under pressure — they cope well enough day-to-day that the cumulative damage goes unnoticed until something breaks. Context matters here: if you are sleeping poorly, gaining weight, getting sick more often, or feeling persistently flat, stress may be the underlying driver rather than any single lifestyle factor.
How to Manage Stress for Better Long-Term Health: The Core Strategies
The evidence on stress management is not particularly mysterious. The strongest interventions are also the most accessible. Let’s keep this practical and start with what gives the biggest return.
1. Prioritise Sleep Above Almost Everything Else
Sleep is where the body processes stress hormones and resets. Adults need 7–9 hours per night. When sleep is consistently short or poor, cortisol levels rise and the stress response becomes harder to regulate — creating a feedback loop that compounds over time [6].
A sensible starting point: fix sleep before adding any other stress management tool. Consistent sleep and wake times, a dark and cool room, and limiting screens in the hour before bed are the basics. For a deeper look at building good sleep habits, the complete guide to sleep hygiene for health and longevity covers the evidence in detail.
2. Move Regularly — Especially When You Don’t Feel Like It
Exercise is one of the most well-documented stress interventions available. It increases endorphins while reducing cortisol and adrenaline [6]. The American Heart Association recommends at least 150 minutes of moderate-intensity exercise weekly, plus strength training two to three times per week [2].
The CDC suggests starting smaller if needed — even 20 to 30 minutes of daily activity makes a measurable difference, and short walks provide immediate mood improvement [4].
Choose the format that fits your life. Walking, swimming, cycling, and resistance training all work. Consistency matters far more than intensity. If you are not sure where to start, the exercise guide for better health is a practical starting point, and walking vs. running for weight loss is worth reading if you prefer lower-impact options.
3. Eat in a Way That Supports Recovery
Food does not cure stress, but it does affect the body’s ability to manage it. The CDC recommends a diet built around fruits, vegetables, whole grains, and lean proteins, while limiting foods high in unhealthy fats, salt, and added sugars [4].
Chronic stress tends to increase cravings for calorie-dense, low-nutrient foods — partly because cortisol affects appetite regulation. That is a real biological pull, not just a lack of willpower. Eating to support stress management means building a baseline diet that reduces inflammation and supports stable blood sugar. The best anti-inflammatory foods for gut health is a useful companion read here.
There is also a meaningful connection between gut health and stress response — the gut-brain axis is a real and well-studied pathway. If stress is affecting your digestion, the gut brain axis guide explains the mechanism clearly.
4. Use Mindfulness and Relaxation Practices — But Keep Expectations Realistic
The Mayo Clinic lists yoga, deep breathing, meditation, massage, journaling, and maintaining hobbies as evidence-supported stress management tools [1]. These are not fringe recommendations — they appear consistently across major health organisations.
That said, there is no magic in it. A 10-minute breathing exercise will not undo six months of poor sleep and overwork. These practices work best as part of a consistent routine, not as occasional emergency measures.
The simplest way to look at it is: if a practice reliably lowers your heart rate, improves your mood, or helps you sleep, it is worth keeping. If it does not, try something else. Journaling works well for some people; others find a walk or a conversation with a friend more effective. The evidence supports the category, not one specific technique.

The Role of Social Connection in Long-Term Stress Management
Social connection is one of the most underrated tools in stress management. The American Heart Association and Cornell Mental Health both identify a strong social support network as a genuine buffer against chronic stress [3][8].
This is not just about feeling supported. Social interaction affects cortisol regulation, immune function, and cardiovascular health through measurable biological pathways. Isolation, by contrast, is associated with elevated stress hormones and worse health outcomes across multiple studies.
In real-world terms: this means maintaining relationships actively, not just when things are difficult. Regular contact with people you trust — whether that is family, friends, or a community group — functions as a form of stress inoculation. It does not need to be deep or time-consuming. Consistent, low-key connection tends to be more protective than occasional intense social contact.
Common mistake: treating social connection as a reward for getting through a busy period, rather than as a scheduled, non-negotiable part of the week. People who are most stressed often withdraw socially at exactly the point when connection would help most.
How Mindful Eating Connects to Stress Management
Stress and eating are closely linked in ways that go beyond comfort food cravings. Elevated cortisol changes how the body stores fat (particularly around the abdomen), affects appetite-regulating hormones, and can drive a cycle of stress eating that worsens both physical and mental health over time.
The practice of mindful eating — paying deliberate attention to what, when, and why you eat — directly addresses this cycle. It is not a diet. It is a way of breaking the automatic, stress-driven eating patterns that build up over time. For a practical breakdown of how this works, the guide to mindful eating and breaking the stress-eating cycle is worth reading alongside this article.
The evidence suggests that people who eat more mindfully report lower stress levels, better food choices, and improved weight management — though the research is still developing and individual results vary. What is clearer is that stress eating is a well-documented pattern, and awareness is the first step to changing it.

When to Seek Professional Help for Stress
Self-management works well for everyday and moderate stress. It is not always sufficient for chronic, severe, or clinically significant stress — and recognising that distinction is important.
The U.S. Office of Disease Prevention and Health Promotion recommends seeking help from a doctor or mental health professional when managing stress independently becomes difficult [5]. That is sound advice, not a last resort.
Signs that professional support is appropriate:
- Stress has persisted for several months without improvement
- Sleep is consistently disrupted despite making changes
- Physical symptoms (headaches, chest tightness, digestive problems) are worsening
- Mood is significantly and persistently low
- Stress is affecting work, relationships, or daily function
- You are using alcohol, food, or other substances to cope
I would be careful with the tendency to treat professional help as a sign that self-management has failed. It is not. A GP can rule out underlying medical causes, and a psychologist or therapist can provide cognitive-behavioural tools that are significantly more effective than general lifestyle advice for clinical anxiety or depression.
If physical symptoms are part of the picture, the common health symptoms guide can help you assess when to seek medical input.
Building a Practical Stress Management Plan That Actually Sticks
Knowing what to do and doing it consistently are different problems. Most people have a reasonable idea of what helps with stress. The gap is usually in building habits that hold up under pressure — which is, of course, exactly when stress management is most needed.
A sensible starting point is to choose two or three changes and build them in before adding more. Trying to overhaul sleep, diet, exercise, and mindfulness simultaneously tends to produce short-term effort and long-term abandonment.
A realistic starting framework:
Week 1–2: Anchor sleep
- Set a consistent wake time, even on weekends
- Remove screens from the bedroom
- Aim for 7–8 hours
Week 3–4: Add movement
- Start with 20–30 minutes of walking daily
- Build toward 150 minutes per week over time
Week 5–6: Address nutrition
- Add one serving of vegetables to two meals per day
- Reduce ultra-processed snacks to one occasion per day
Week 7 onward: Layer in mindfulness and connection
- Five minutes of deep breathing or journaling in the morning
- Schedule one social activity per week that is non-negotiable
Keep it simple and consistent. The goal is not perfection — it is a baseline that holds up over months and years. That is what actually produces long-term health benefits.
For broader lifestyle context, the guide to living a healthy lifestyle covers how stress management fits into the wider picture of long-term wellbeing.

What Effective Stress Management Actually Delivers
Let’s be specific about outcomes, because this is where motivation either holds or fades.
According to the Mayo Clinic and the U.S. Office of Disease Prevention and Health Promotion, effective stress management is associated with [1][5]:
- Better sleep quality and duration
- Increased energy levels
- Improved weight control
- Reduced muscle tension and headaches
- Better mood and emotional regulation
- Improved relationships
- Lower blood pressure
- Better focus and self-control
- Potentially longer, healthier life
The numbers matter, but so does the timeline. Most of these benefits are not immediate. Sleep improvements can come within days. Blood pressure changes may take weeks to months. Cardiovascular risk reduction is a years-long process. Managing expectations around timeline is part of what makes a stress management plan sustainable.
More is not always better. Adding every possible stress reduction technique at once tends to create its own pressure. The stronger evidence points to consistency with a small number of well-chosen habits, rather than an elaborate multi-intervention programme.
FAQ: How to Manage Stress for Better Long-Term Health
Q: What is the fastest way to reduce stress right now?
Deep, slow breathing — specifically extending the exhale — activates the parasympathetic nervous system and reduces cortisol within minutes. It is not a long-term solution, but it is a reliable immediate tool [1].
Q: Does exercise help with stress even if you don’t enjoy it?
Yes. The physiological benefits — reduced cortisol, increased endorphins — occur regardless of whether exercise feels enjoyable. That said, choosing an activity you tolerate or enjoy improves consistency, which is what matters for long-term outcomes [6].
Q: How much sleep do adults actually need for stress management?
The consistent recommendation across major health organisations is 7–9 hours per night for adults. Consistently sleeping less than 6 hours significantly worsens cortisol regulation and stress resilience [6].
Q: Can diet alone manage chronic stress?
No. Diet supports the body’s stress response and reduces inflammation, but it cannot substitute for sleep, movement, and psychological tools. It is one component of a broader approach [4].
Q: Is meditation necessary for stress management?
No. Meditation is one evidence-supported option among several. Deep breathing, journaling, physical activity, and social connection all have comparable evidence. Choose what you will actually do consistently [1][8].
Q: When does stress become a medical issue?
When it persists for months, significantly disrupts sleep or daily function, or is accompanied by physical symptoms like chest pain or persistent headaches, it warrants medical assessment. A GP is the appropriate first contact [5].
Q: Does alcohol reduce stress?
In the short term, alcohol may reduce the subjective experience of stress. In the medium and long term, it disrupts sleep, raises cortisol, and worsens anxiety — making it counterproductive as a stress management tool [10].
Q: How does gut health relate to stress?
The gut-brain axis is a well-documented bidirectional communication system. Chronic stress disrupts gut microbiome balance and gut barrier function; conversely, poor gut health can amplify stress and anxiety responses [7].
Q: Are supplements useful for stress management?
Some supplements — magnesium, for example — have modest evidence for supporting stress-related outcomes, particularly sleep. However, the evidence is not strong enough to recommend supplements over lifestyle changes. Start with the basics first [9].
Q: Can you manage stress without making big lifestyle changes?
Small, consistent changes produce real benefits. You do not need to overhaul your life. Adding 20 minutes of walking, improving sleep by 45 minutes, and scheduling one social activity per week are all meaningful steps with documented effects [4].
Conclusion: What Actually Works Over Time
Learning how to manage stress for better long-term health is not complicated, but it does require consistency. The basics — sleep, movement, food quality, social connection, and occasional mindfulness practice — are not glamorous. They are also the interventions with the strongest and most consistent evidence behind them [1][3][6].
Start with what gives the biggest return. For most people, that is sleep. Fix that first, then add movement. Build from there. Do not try to do everything at once.
The basics still do the heavy lifting. Supplements, apps, and stress-reduction programmes all have their place, but none of them substitute for a consistent sleep schedule and regular physical activity. Evidence first, common sense backed by evidence.
If self-management is not working after a genuine effort, seek professional support. That is not a failure — it is the appropriate next step [5].
Stress is a real health risk. Managing it is a real health strategy. Treat it accordingly.
