Sleep Hygiene: The Complete Guide to Better Sleep for Health and Longevity

Last updated: May 4, 2026
Quick Answer
Sleep hygiene refers to a set of consistent habits and environmental conditions that support reliable, restorative sleep. For most adults, the most effective starting points are fixing a consistent wake time, removing screens from the bedroom, and keeping the room cool and dark. These three changes alone address the majority of common sleep problems and are supported by the strongest available evidence.
Key Takeaways
- Most adults need 7–9 hours of sleep per night; consistently getting less is linked to increased risk of cardiovascular disease, metabolic dysfunction, and cognitive decline [8]
- A fixed wake time is the single most powerful tool for regulating your circadian rhythm — more so than a fixed bedtime [1]
- Phone use before bed is now identified as the leading modern sleep disruptor — the content, not just the blue light, is the problem [1]
- Bedroom temperature between 18–22°C (64–72°F) supports the core body temperature drop required for deep sleep [3]
- Morning light exposure within 30–60 minutes of waking calibrates melatonin timing for the entire day [1]
- Caffeine has a half-life of roughly 5–7 hours, meaning an afternoon coffee can still be half-active in your system at midnight
- Chronic deficiencies in Vitamin D or B12 can contribute to fragmented sleep and restless leg syndrome — worth checking if sleep problems persist [3]
- Red light frequencies do not suppress melatonin, making them a practical alternative to standard white or blue lighting in the evening [3]
- Sleep hygiene works best as a system, not a collection of isolated tips — consistency matters more than perfection
Table of Contents
- What Is Sleep Hygiene and Why Does It Matter for Health and Longevity?
- What Are the Biggest Sleep Disruptors in 2026?
- What Does a Practical Sleep Hygiene Routine Actually Look Like?
- How Does Sleep Affect Long-Term Health and Longevity?
- How Should You Set Up Your Bedroom for Better Sleep?
- What Role Does Diet and Nutrition Play in Sleep Quality?
- What Are the Most Common Sleep Hygiene Mistakes?
- When Is Sleep Hygiene Not Enough?
- Sleep Hygiene: The Complete Guide to Better Sleep for Health and Longevity — Practical Checklist
- Frequently Asked Questions
- Conclusion

What Is Sleep Hygiene and Why Does It Matter for Health and Longevity?
Sleep hygiene is the collection of daily habits, routines, and environmental factors that either support or undermine your ability to sleep well. It is not a treatment for serious sleep disorders, but it is the foundation that everything else rests on.
Here’s the real issue: most people treat sleep as whatever is left after everything else gets done. That mindset has a measurable cost. Research consistently links short or poor-quality sleep to higher rates of cardiovascular disease, type 2 diabetes, obesity, depression, and accelerated cognitive aging [8]. The 2026 Sleep Awareness Week theme — “Sleep Better, Live Well” — reflected a growing body of evidence connecting sleep regularity to increased life expectancy [2].
In plain English: you cannot exercise, eat, or supplement your way around chronic poor sleep. It sits at the base of almost every other health outcome.
What counts as “poor sleep”?
Poor sleep is not just about hours. It includes:
- Taking more than 30 minutes to fall asleep regularly
- Waking frequently during the night and struggling to return to sleep
- Waking unrefreshed despite adequate time in bed
- Relying on an alarm to reach minimum sleep duration
- Needing caffeine or stimulants to function through the day
If two or more of those apply consistently, sleep hygiene is the right starting point before considering any other intervention.
What Are the Biggest Sleep Disruptors in 2026?
The evidence points clearly to three dominant disruptors for most adults today: screen use before bed, irregular sleep timing, and poor sleep environment. Of these, phone use at bedtime has moved to the top of the list [1].
This is where hype gets in the way. For years, the conversation focused almost entirely on blue light from screens. Blue light does suppress melatonin, but that is only part of the problem. The content on phones — social media feeds, news, short-form video — triggers dopamine and cortisol responses that keep the brain in an alert, stimulated state. That is a fundamentally different problem from light exposure, and it requires a different solution [1].
The three main disruptors, ranked by impact:
| Disruptor | Mechanism | Common Mistake |
|---|---|---|
| Phone/screen use before bed | Dopamine + cortisol stimulation, blue light | Switching to “night mode” and thinking that’s enough |
| Irregular sleep timing | Disrupts circadian rhythm and melatonin cycle | Sleeping in on weekends to “catch up” |
| Poor sleep environment | Temperature, light, noise cause micro-arousals | Assuming the bedroom is fine without checking |
Caffeine timing is a close fourth. Most people underestimate how long caffeine stays active. With a half-life of 5–7 hours, a 3pm coffee still has roughly half its stimulant effect at 9pm.
What Does a Practical Sleep Hygiene Routine Actually Look Like?
A sensible starting point is what some researchers now call the “Modern Sleep Hygiene Stack” — three foundational changes that address the most common causes of poor sleep in 2026 [1]:
- Block your phone at bedtime. Put it in another room or use a physical alarm clock. This is not about willpower — it is about removing the trigger entirely.
- Fix your wake time. Choose a time and keep it seven days a week. The wake time anchors the entire sleep-wake cycle. Bedtime adjusts naturally over a few weeks.
- Get morning light. Step outside within 30–60 minutes of waking. Even on overcast days, outdoor light is significantly brighter than indoor lighting and sends a clear signal to the brain’s circadian clock.
These three changes are not glamorous. There is no magic in it. But they target the root causes rather than the symptoms, and they work for most people who apply them consistently.
The evening wind-down hour
A relaxing bedtime routine in the hour before sleep helps the nervous system shift from a sympathetic (alert) state to a parasympathetic (rest) state [8]. Turning off mobile phones and tablets 30–60 minutes before bed significantly reduces the time it takes to fall asleep [3].
Practical wind-down activities:
- Reading a physical book or e-reader without a backlit screen
- A warm bath or shower (the subsequent drop in skin temperature signals sleep readiness)
- Gentle stretching or progressive muscle relaxation
- Writing a short to-do list for the next day (offloads mental loops)
- Herbal tea — chamomile or valerian, though the evidence for these is modest
Avoid in the hour before bed:
- News, social media, or anything emotionally activating
- Work emails or problem-solving tasks
- Intense exercise (moderate exercise earlier in the day is beneficial — see our exercise guide for better health)
- Large meals or alcohol
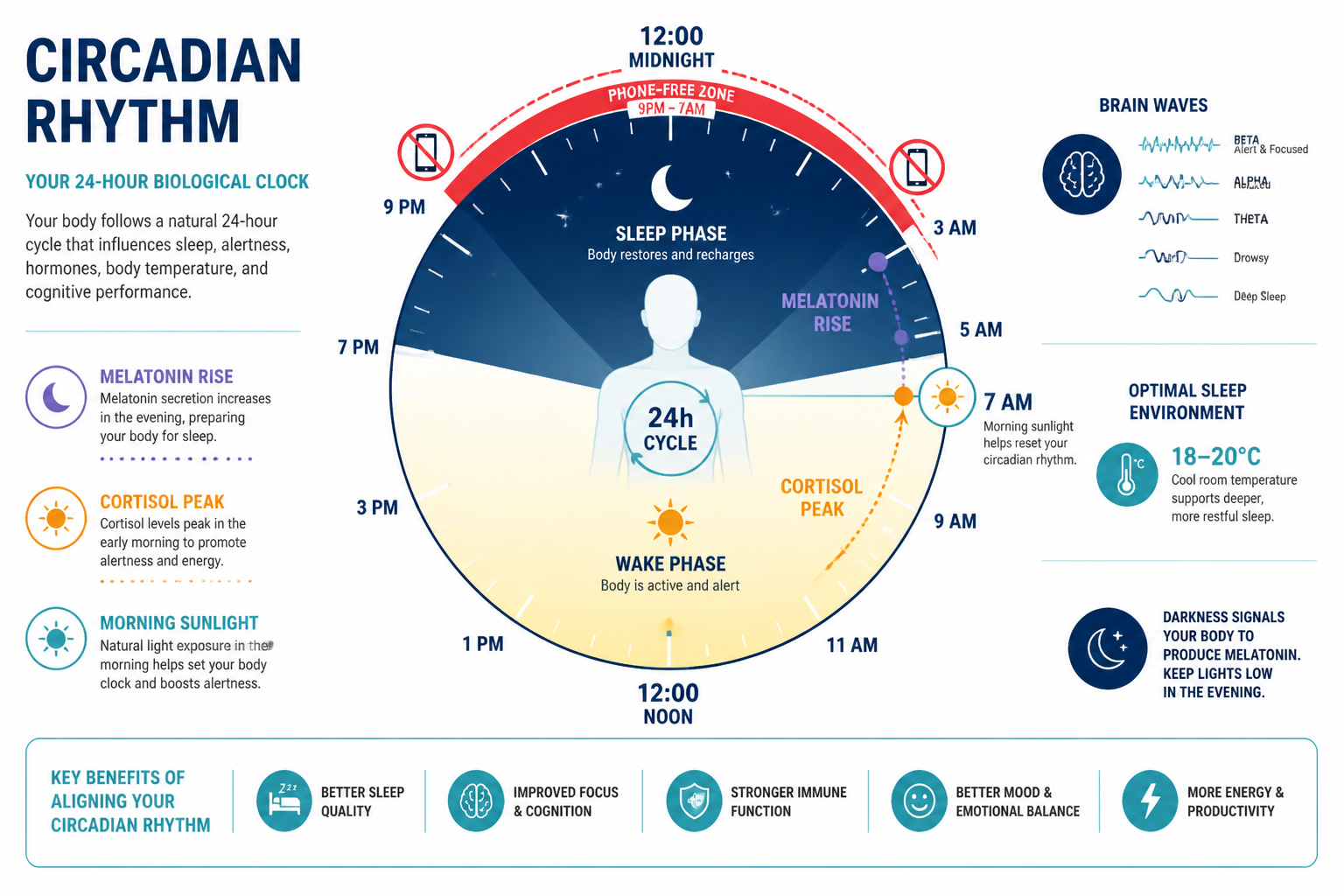
How Does Sleep Affect Long-Term Health and Longevity?
The evidence on sleep and longevity has strengthened considerably over the past decade. The stronger evidence points to sleep quality and regularity — not just duration — as independent predictors of health outcomes [2][8].
What the research shows:
- Cardiovascular health: Short sleep duration (under 6 hours) is associated with higher rates of hypertension, coronary artery disease, and stroke. The mechanism involves elevated cortisol, increased inflammatory markers, and impaired glucose regulation [8]
- Metabolic function: Poor sleep disrupts leptin and ghrelin — the hormones that regulate hunger and satiety. This is one reason sleep deprivation is consistently linked to weight gain and insulin resistance. For context on how diet and metabolic health interact, our guide on intermittent fasting for weight loss covers the overlap in detail
- Brain health: Sleep is when the glymphatic system clears metabolic waste from the brain, including proteins associated with Alzheimer’s disease. Chronic sleep disruption impairs this clearance process
- Immune function: Sleep deprivation reduces natural killer cell activity and antibody response — meaning poor sleepers are more susceptible to infection and may respond less effectively to vaccines
- Inflammation: Chronic poor sleep elevates C-reactive protein and interleukin-6, both markers of systemic inflammation. This connects directly to the role of diet in managing inflammation — see our anti-inflammatory foods guide for the dietary side of that equation
The numbers matter here. A 2026 analysis highlighted in Sleep Awareness Week coverage found that sleep regularity — meaning consistent timing, not just duration — was associated with meaningful reductions in all-cause mortality risk [2]. That is a strong claim, and it does need strong proof, but the direction of evidence across multiple large studies is consistent.
How Should You Set Up Your Bedroom for Better Sleep?
The bedroom environment is one of the most controllable variables in sleep hygiene, and it is frequently underestimated. The goal is to make the room a reliable cue for sleep — and nothing else [7][8].
The four key variables:
1. Temperature
Optimal bedroom temperature sits between 18–22°C (approximately 64–72°F), with some sleep specialists recommending the lower end of that range, around 15–19°C (60–67°F) [3][7]. A cool room supports the drop in core body temperature that triggers deep NREM sleep. If the room is too warm, the body struggles to initiate and maintain deep sleep stages.
2. Light
Total darkness is the most effective environment for melatonin production. Blackout curtains or a sleep mask are practical solutions. If some light is needed — for safety or comfort — red-spectrum light is the right choice. Red light frequencies do not suppress melatonin, unlike white, blue, or green light [3].
3. Sound
Quiet is ideal, but complete silence is not always achievable. White noise machines, fans, or earplugs can mask variable environmental sounds — it is the unpredictability of sound (a car horn, a neighbour’s door) that causes micro-arousals, not steady background noise [3][6].
4. Association
The bedroom should be reserved for sleep and sex only. Working, watching television, scrolling phones, or having stressful conversations in bed weakens the mental association between the bedroom and sleep [8]. This is not a minor point — it is one of the core principles of stimulus control therapy, which is a component of CBT-I (Cognitive Behavioural Therapy for Insomnia), currently the gold-standard clinical treatment for chronic insomnia [6].

What Role Does Diet and Nutrition Play in Sleep Quality?
Diet affects sleep through multiple pathways — blood sugar stability, neurotransmitter production, and micronutrient status all have measurable effects on sleep quality.
What to know:
- Tryptophan is a precursor to serotonin and melatonin. Foods containing tryptophan (turkey, eggs, dairy, nuts, seeds) may support melatonin production, though the effect is modest and context-dependent
- Magnesium plays a role in GABA regulation, the primary inhibitory neurotransmitter involved in sleep. Low magnesium intake is associated with poorer sleep quality, though supplementation evidence is mixed
- Vitamin D and B12 deficiencies are worth checking if sleep problems persist. Chronic deficiency in either can contribute to restless leg syndrome and fragmented sleep [3]. A standard blood panel will identify these gaps
- Alcohol is widely misunderstood as a sleep aid. It does reduce sleep onset time, but it fragments the second half of the night and suppresses REM sleep — leaving people feeling unrefreshed even after adequate hours
- Large meals within 2–3 hours of bed increase the likelihood of acid reflux and raise core body temperature, both of which impair sleep
For a broader look at how food choices affect health outcomes — including inflammation and gut function, both of which interact with sleep — the health benefits of natural foods and herbs guide covers the evidence in detail.
There is also a meaningful gut-sleep connection. The gut microbiome produces a significant proportion of the body’s serotonin, which is a precursor to melatonin. Gut health and sleep quality appear to influence each other bidirectionally. Our gut health and digestive wellness guide covers the gut side of that relationship.
What Are the Most Common Sleep Hygiene Mistakes?
Most sleep hygiene advice is correct in principle but fails in practice because people apply it inconsistently or miss the highest-leverage changes.
Common mistakes, in plain English:
1. Treating weekends differently
Sleeping in on weekends shifts the circadian rhythm — a phenomenon sometimes called “social jet lag.” Even one to two hours of weekend sleep drift can meaningfully disrupt the following week’s sleep. The fix is simple but uncomfortable: keep the wake time consistent, even on days off.
2. Thinking night mode solves the phone problem
Switching a phone to warm-tone display settings reduces blue light but does nothing about the stimulating content. The brain does not care what colour the screen is when it is processing a stressful news story or a dopamine-triggering video feed [1].
3. Staying in bed when awake
Lying in bed awake for extended periods — especially if anxious about sleep — reinforces a negative association between the bed and wakefulness. The standard recommendation is to get up after 20 minutes if sleep has not come, do something calm in low light, and return when sleepy.
4. Using alcohol as a sleep aid
This is one of the most common and counterproductive habits. The sedative effect of alcohol masks poor sleep quality — people fall asleep faster but wake more frequently and miss restorative REM sleep.
5. Expecting immediate results
Sleep hygiene changes take time. Circadian rhythm adjustments typically require 1–2 weeks of consistent behaviour before the full effect is felt. People abandon the approach too early because they expect overnight improvement.
When Is Sleep Hygiene Not Enough?
Sleep hygiene is a strong foundation, but it is not a treatment for clinical sleep disorders. It is not that simple.
If consistent sleep hygiene practice over 4–6 weeks does not produce meaningful improvement, it is worth considering whether an underlying condition is involved. Common conditions that require clinical assessment include:
- Obstructive sleep apnoea (OSA): Characterised by snoring, gasping, and unrefreshed sleep despite adequate hours. Requires a sleep study for diagnosis. Untreated OSA carries significant cardiovascular risk
- Restless leg syndrome (RLS): An urge to move the legs, particularly at night. Can have nutritional components (iron, B12, folate deficiency) but may also require medical management
- Chronic insomnia disorder: Defined as difficulty initiating or maintaining sleep at least three nights per week for three or more months, with daytime impairment. CBT-I is the recommended first-line treatment — more effective than sleep medication in the long term [6]
- Circadian rhythm disorders: Including delayed sleep phase syndrome, which is common in younger adults and shift workers
If any of these seem relevant, the right step is a conversation with a GP or sleep specialist — not more sleep hygiene tips. Our common health symptoms guide covers the broader question of when symptoms warrant professional assessment.

Sleep Hygiene: The Complete Guide to Better Sleep for Health and Longevity — Practical Checklist
Here is a straightforward checklist. Start with the top items — they give the biggest return.
Highest priority (start here):
- ✅ Fix a consistent wake time, 7 days a week
- ✅ Remove phone from the bedroom at night
- ✅ Get outside for natural light within 60 minutes of waking
- ✅ Keep bedroom temperature between 18–22°C
High priority:
- ✅ Avoid caffeine after 2pm
- ✅ No alcohol within 3 hours of bed
- ✅ Use blackout curtains or a sleep mask
- ✅ Begin a wind-down routine 60 minutes before bed
- ✅ Reserve the bed for sleep only — no work, no screens
Worth adding once the basics are in place:
- ✅ Check Vitamin D and B12 levels if sleep problems persist
- ✅ Manage evening light with red-spectrum bulbs or lamps
- ✅ Use white noise or earplugs if environmental sound is an issue
- ✅ Consider magnesium intake through diet (nuts, seeds, leafy greens)
Keep it simple and consistent. The basics still do the heavy lifting.
Frequently Asked Questions
Q: How many hours of sleep do adults actually need?
Most adults need 7–9 hours per night. Individual variation exists, but consistently sleeping under 6 hours carries measurable health risks. Claims about needing only 5–6 hours are almost always rationalisation rather than genuine biology [8].
Q: Is it better to go to bed at the same time or wake up at the same time?
Wake time is more important. A consistent wake time anchors the circadian rhythm and builds sleep pressure predictably. Bedtime tends to self-regulate once wake time is fixed [1].
Q: Does melatonin supplementation help?
Melatonin is most useful for circadian timing issues — jet lag, shift work, or delayed sleep phase. It is not a strong sleep-inducing agent for standard insomnia. Low doses (0.5–1mg) timed 1–2 hours before the desired sleep time are more effective than the high doses commonly sold [6].
Q: Can exercise improve sleep quality?
Yes, consistently. Regular moderate exercise improves sleep onset, deep sleep duration, and overall sleep quality. Timing matters — vigorous exercise within 1–2 hours of bed can delay sleep onset in some people. For practical guidance, see our exercise guide for better health.
Q: Does a warm bath before bed actually help?
Yes, and the mechanism is well-established. A warm bath raises skin temperature, and the subsequent cooling as you exit triggers a drop in core body temperature — the same signal the body uses to initiate sleep. Timing it 1–2 hours before bed appears to be most effective.
Q: What is the best temperature for sleeping?
Between 18–22°C (64–72°F) for most adults, with some evidence supporting the cooler end of that range. The key mechanism is facilitating the drop in core body temperature that triggers deep sleep [3][7].
Q: Is it bad to nap during the day?
Short naps (10–20 minutes) before 3pm are generally fine and can improve alertness. Longer naps or naps taken late in the afternoon reduce sleep pressure and make it harder to fall asleep at night — particularly problematic if you are already dealing with insomnia.
Q: Why do I wake up at 3am?
Early morning waking is often linked to stress and elevated cortisol, alcohol consumption in the evening, or natural sleep cycle transitions. It can also be a symptom of depression or sleep apnoea. If it is consistent and accompanied by other symptoms, it warrants a clinical assessment.
Q: Can CBD oil help with sleep?
Some people report benefit, particularly for anxiety-related sleep difficulties. The evidence is preliminary and inconsistent. For a detailed breakdown of what is known, our guide on how long CBD oil stays in your system covers the pharmacology and current evidence.
Q: How long does it take for sleep hygiene changes to work?
Expect 1–4 weeks before the full effect is apparent. Circadian rhythm adjustment takes time, and sleep pressure needs to build consistently. Most people who abandon sleep hygiene changes do so in the first week — before the changes have had time to work.
Conclusion
Sleep hygiene — the complete guide to better sleep for health and longevity — comes down to a handful of consistent, evidence-backed habits applied over time. There is no shortcut, and there is no supplement that replaces the basics.
The main takeaway is this: start with the three highest-leverage changes — fix your wake time, remove your phone from the bedroom, and get morning light. These address the most common root causes of poor sleep in 2026 and require no equipment, no expense, and no special knowledge.
From there, build the environment: cool, dark, quiet, and reserved for sleep. Then address diet, timing, and the evening wind-down. Check nutritional status if problems persist. Seek clinical help if consistent effort over 4–6 weeks produces no improvement.
Sleep is not a passive state. It is an active biological process that repairs tissue, consolidates memory, regulates hormones, clears metabolic waste from the brain, and calibrates every system in the body. Treating it as a priority — not an afterthought — is one of the highest-return decisions available for long-term health.
The basics still do the heavy lifting. Keep it simple and consistent, and give it time.
