What Are the Early Signs of Diabetes? A Complete Guide (2026)
In this guide
- What Is Diabetes and Why Do Early Signs Matter?
- What Are the 7 Most Common Early Signs of Diabetes?
- Are There Early Signs of Diabetes That Are Specific to Women?
- What’s the Difference Between Type 1 and Type 2 Diabetes Early Signs?
- What Risk Factors Increase Your Chances of Developing Diabetes?
- How Is Diabetes Diagnosed? Tests and What the Numbers Mean
- What Should You Do If You Notice Early Signs of Diabetes?
- How Can You Manage or Prevent Diabetes Through Lifestyle Changes?
Last updated: April 8, 2026
Quick Answer: The early signs of diabetes include frequent urination, excessive thirst, unexplained weight loss, persistent fatigue, blurred vision, slow-healing wounds, and tingling in the hands or feet. These symptoms occur because the body either cannot produce enough insulin or cannot use it effectively, causing blood sugar to rise to damaging levels. If you notice several of these symptoms together — especially over days or weeks — see a doctor promptly. Early detection dramatically improves long-term outcomes. Understanding these Diabetes early signs can save lives.
Key Takeaways
- Frequent urination and extreme thirst are often the first noticeable signs of high blood sugar
- Type 2 diabetes can develop silently — many people have no obvious symptoms in the early stages
- According to the CDC, approximately 38.4 million Americans had diabetes as of 2024, with roughly 90–95% having Type 2
- An estimated 97.6 million U.S. adults have prediabetes, and most don’t know it (CDC, 2024)
- Blurred vision linked to diabetes is caused by fluid shifts in the eye’s lens — it can be reversed with early treatment
- Slow wound healing is a red flag that blood sugar has been elevated long enough to affect circulation and immune function
- Women may experience unique early symptoms, including recurrent yeast infections and urinary tract infections
- Type 1 diabetes symptoms tend to appear suddenly; Type 2 symptoms develop gradually over months or years
- A simple fasting blood glucose test or A1C test can confirm or rule out diabetes
- Lifestyle changes — diet, exercise, and weight management — can prevent or delay Type 2 diabetes in high-risk individuals
What Is Diabetes and Why Do Early Signs Matter?
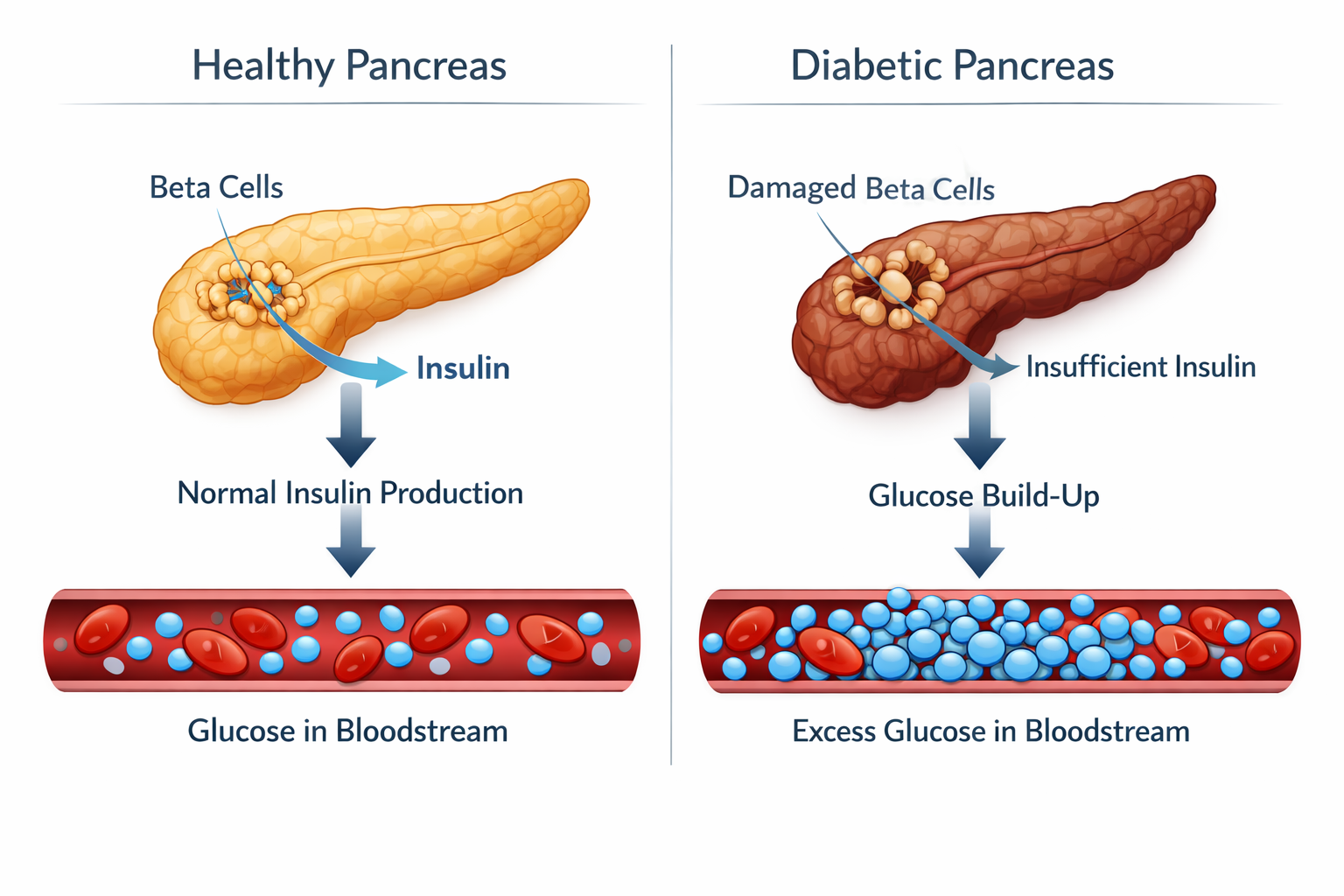
Diabetes is a chronic metabolic condition in which the body cannot properly regulate blood sugar (glucose) levels. This happens either because the pancreas produces little or no insulin (Type 1), or because the body’s cells become resistant to insulin’s effects and the pancreas can’t compensate (Type 2). A third form, gestational diabetes, develops during pregnancy and usually resolves after delivery but raises the mother’s lifetime risk of Type 2.
Glucose is the body’s primary fuel source. When insulin is absent or ineffective, glucose builds up in the bloodstream instead of entering cells. Over time, this elevated blood sugar damages blood vessels, nerves, and organs throughout the body.
Why early detection matters: Catching diabetes before it progresses protects against serious complications including kidney disease, cardiovascular disease, vision loss, and nerve damage. For prediabetes — the stage before Type 2 diabetes — lifestyle changes alone can reduce the risk of progression by up to 58%, according to the landmark Diabetes Prevention Program study (National Institutes of Health, 2002, with follow-up data confirming long-term benefit).
The challenge is that early symptoms are easy to dismiss. Fatigue feels like stress. Thirst seems like dehydration. That’s why knowing the specific pattern of symptoms matters.
What Are the 7 Most Common Early Signs of Diabetes?
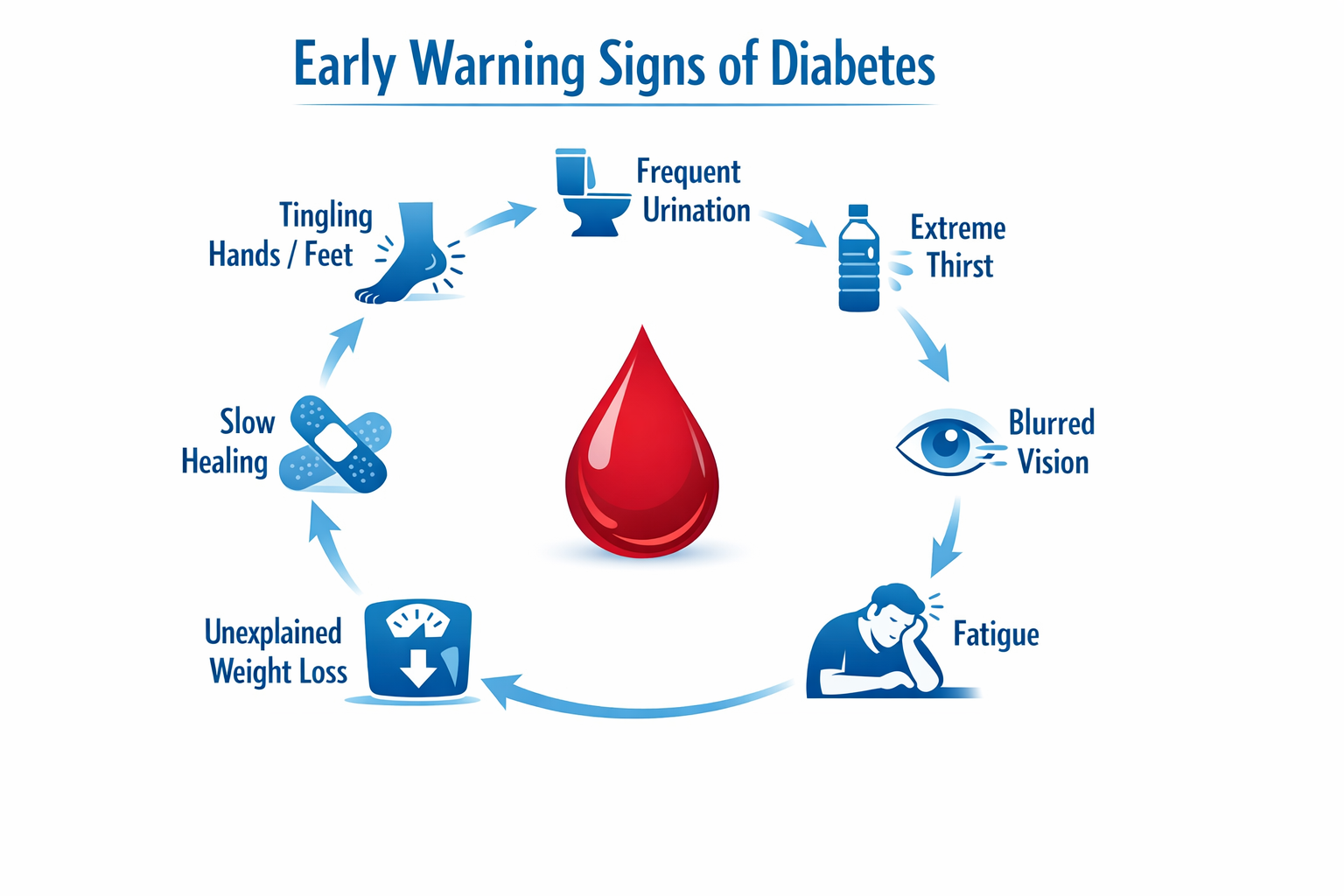
The seven most recognized early warning signs of diabetes are frequent urination, excessive thirst, unexplained weight loss, persistent fatigue, blurred vision, slow-healing cuts or sores, and tingling or numbness in the extremities. These signs often appear together, and their combination is more telling than any single symptom alone.
1. Frequent Urination (Polyuria)
When blood sugar rises above a certain threshold — roughly 180 mg/dL — the kidneys can no longer reabsorb all the glucose filtering through them. The excess glucose spills into urine, pulling water with it. The result is significantly increased urine output, often eight or more times per day and frequently at night (a pattern called nocturia).
What makes this a red flag: Occasional frequent urination has many causes — a large fluid intake, a urinary tract infection, or certain medications. But if you’re urinating more than usual without drinking significantly more water, and especially if it’s waking you at night, that pattern warrants a blood sugar check.
Common mistake: Many people attribute nighttime urination to aging or a small bladder and delay getting tested for years.
2. Excessive Thirst (Polydipsia)
Excessive thirst follows directly from frequent urination. As the body loses more water through increased urination, it triggers a strong thirst response to compensate. People with undiagnosed diabetes often describe drinking large amounts of water or juice throughout the day and still feeling thirsty.
This cycle — drink more, urinate more, feel thirsty again — is one of the clearest early indicators of elevated blood sugar. If you’re consuming well over 2–3 liters of fluid daily and still feel parched, that’s worth discussing with a doctor.
3. Unexplained Weight Loss
Unexplained weight loss is more common in Type 1 diabetes but can also appear in Type 2. When cells can’t access glucose for energy, the body breaks down fat and muscle tissue instead. This can cause noticeable weight loss — sometimes 10 to 20 pounds over weeks — even when appetite is normal or increased.
If you haven’t changed your diet or exercise habits and you’re losing weight without trying, that’s a symptom that needs investigation. It’s especially significant if it accompanies other signs on this list.
For people managing their weight, it’s worth noting that intentional weight loss through healthy strategies is very different from the involuntary muscle and fat loss driven by uncontrolled blood sugar.
4. Persistent Fatigue
Fatigue is one of the most common — and most overlooked — early signs of diabetes. When cells are starved of glucose despite high blood sugar levels, the body simply doesn’t have enough usable energy. The result is a bone-deep tiredness that sleep doesn’t fully resolve.
People with early-stage diabetes often describe feeling exhausted after normal activities, struggling to concentrate, or needing to rest far more than usual. This fatigue can also be compounded by dehydration from frequent urination.
Choose this as a prompt to act if: The fatigue is persistent (lasting more than two weeks), doesn’t improve with rest, and occurs alongside any other symptom on this list.
5. Blurred Vision
Blurred vision is an early sign of diabetes that many people attribute to needing new glasses. In reality, high blood sugar causes fluid to shift in and out of the lens of the eye, temporarily changing its shape and affecting its ability to focus. This produces blurry, fluctuating vision that may come and go.
The good news: in the early stages, this vision change is often reversible once blood sugar is brought under control. The concern is that if high blood sugar persists long-term, it can cause diabetic retinopathy — damage to the blood vessels in the retina — which is a leading cause of blindness in adults.
Supporting your eye health proactively matters, and understanding herbs and nutrients that support eye health can be a useful complement to medical care.
Edge case: If blurred vision is sudden, severe, or accompanied by eye pain, seek emergency care — this may indicate a different, acute condition.
6. Slow-Healing Cuts, Sores, or Bruises
When blood sugar is chronically elevated, it impairs circulation and weakens the immune response. White blood cells — the body’s infection fighters — function less effectively in a high-glucose environment. Combined with reduced blood flow to small vessels, this means wounds take longer to heal and are more prone to infection.
A cut that would normally close in a few days might linger for weeks. Foot sores are particularly concerning because peripheral neuropathy (nerve damage in the feet) can make them hard to detect until they’ve progressed significantly.
Practical example: If you notice a blister or small cut on your foot that isn’t healing after 7–10 days, don’t wait — see a doctor. Diabetic foot complications are a leading cause of non-traumatic lower-limb amputations, but they’re largely preventable with early intervention.
7. Tingling, Numbness, or Burning in Hands and Feet
Tingling or numbness — particularly in the feet — can be an early sign that elevated blood sugar is beginning to affect nerve function. This condition, called peripheral neuropathy, develops when high glucose damages the small blood vessels that supply nerves.
Early neuropathy often presents as:
- A pins-and-needles sensation in the feet or hands
- Burning or sharp pain, especially at night
- Reduced sensitivity to touch or temperature
- A feeling of wearing invisible socks or gloves
This symptom is more commonly associated with Type 2 diabetes that has been undiagnosed for some time, but it can appear earlier than expected in people with consistently high blood sugar.
Are There Early Signs of Diabetes That Are Specific to Women?
Yes. Women with diabetes — or prediabetes — may experience several symptoms that men typically don’t, or that present differently.
Recurrent yeast infections: High blood sugar creates an environment where the Candida fungus thrives. Women with uncontrolled or undiagnosed diabetes often experience frequent vaginal yeast infections that don’t respond well to standard treatment. Itching, unusual discharge, and irritation in the vaginal area that keeps returning is worth discussing with a doctor, especially alongside other diabetes symptoms.
Recurrent urinary tract infections (UTIs): Elevated glucose in urine promotes bacterial growth, making women with diabetes more susceptible to UTIs. Frequent or hard-to-treat UTIs can be an early indicator.
Polycystic ovary syndrome (PCOS) connection: Women with PCOS have a significantly higher risk of developing insulin resistance and Type 2 diabetes. If you have PCOS, regular blood sugar screening is especially important.
Gestational diabetes: During pregnancy, hormonal changes can cause insulin resistance. Gestational diabetes often has no obvious symptoms, which is why routine glucose screening during pregnancy (typically at 24–28 weeks) is standard practice. Left unmanaged, it raises risks for both mother and baby.
What’s the Difference Between Type 1 and Type 2 Diabetes Early Signs?
The core early symptoms — thirst, urination, fatigue, blurred vision — overlap between Type 1 and Type 2, but the pattern and speed of onset differ significantly.
| Feature | Type 1 Diabetes | Type 2 Diabetes |
|---|---|---|
| Onset of symptoms | Sudden (days to weeks) | Gradual (months to years) |
| Age of typical onset | Often childhood/young adulthood | Typically over 40, but rising in younger adults |
| Weight changes | Often significant weight loss | May be overweight or no weight change |
| Symptom severity | Usually dramatic and urgent | Often mild or absent early on |
| Cause | Autoimmune destruction of beta cells | Insulin resistance + declining beta cell function |
| Emergency risk | High (diabetic ketoacidosis) | Lower initially, but serious if untreated |
Key distinction: Type 1 diabetes can escalate to a medical emergency — diabetic ketoacidosis (DKA) — within days of symptom onset. Symptoms of DKA include nausea, vomiting, abdominal pain, fruity-smelling breath, and rapid breathing. This requires immediate emergency care.
Type 2 diabetes, by contrast, often develops so gradually that people live with it for years before diagnosis. The CDC estimates that 1 in 5 people with diabetes don’t know they have it.
What Risk Factors Increase Your Chances of Developing Diabetes?
Understanding your personal risk helps determine how urgently you should seek screening, even without obvious symptoms.
Risk factors for Type 2 diabetes include:
- Being overweight or obese (especially with excess abdominal fat)
- Physical inactivity
- Family history of Type 2 diabetes (parent or sibling)
- Age 45 or older
- History of prediabetes or gestational diabetes
- Polycystic ovary syndrome (PCOS)
- Certain ethnicities: African American, Hispanic/Latino, Native American, Asian American, and Pacific Islander populations have higher risk
- High blood pressure (130/80 mmHg or above)
- Abnormal cholesterol or triglyceride levels
- History of cardiovascular disease
Choose to get screened now if: You’re over 35 with any of the above risk factors, or if you have two or more risk factors at any age. The U.S. Preventive Services Task Force recommends screening for prediabetes and Type 2 diabetes in adults aged 35–70 who are overweight or obese.
Diet plays a central role in both risk and management. Eating patterns high in processed foods and refined carbohydrates drive insulin resistance over time. Incorporating anti-inflammatory foods and reducing ultra-processed food intake are evidence-based strategies for lowering risk.
How Is Diabetes Diagnosed? Tests and What the Numbers Mean
Diabetes is confirmed through blood tests, not symptoms alone. Here are the four standard diagnostic tests:
1. A1C Test (Glycated Hemoglobin)
- Measures average blood sugar over the past 2–3 months
- Normal: below 5.7%
- Prediabetes: 5.7%–6.4%
- Diabetes: 6.5% or higher (confirmed with a repeat test)
2. Fasting Plasma Glucose (FPG)
- Taken after an 8-hour fast
- Normal: below 100 mg/dL
- Prediabetes: 100–125 mg/dL
- Diabetes: 126 mg/dL or higher (on two separate occasions)
3. Oral Glucose Tolerance Test (OGTT)
- Blood sugar measured 2 hours after drinking a glucose solution
- Normal: below 140 mg/dL
- Prediabetes: 140–199 mg/dL
- Diabetes: 200 mg/dL or higher
4. Random Plasma Glucose Test
- Can be taken at any time, regardless of when you last ate
- Diabetes is indicated at 200 mg/dL or higher, especially with symptoms present
A single abnormal result is usually confirmed with a second test before a diabetes diagnosis is made, unless symptoms are severe or a random glucose test shows 200 mg/dL or higher with clear symptoms.
What Should You Do If You Notice Early Signs of Diabetes?

If you recognize several of the symptoms described above, the right move is straightforward: schedule an appointment with your doctor for a blood glucose test. Don’t try to self-diagnose based on symptoms alone, and don’t wait to see if symptoms resolve on their own.
Steps to take:
- Document your symptoms — note when they started, how frequent they are, and whether they’re worsening. This helps your doctor assess the timeline.
- Request a blood sugar test — ask specifically for a fasting glucose test and/or an A1C. These are routine, low-cost, and widely available.
- Review your risk factors — share your family history, weight changes, and lifestyle habits with your doctor.
- Don’t self-treat with dietary changes alone before being tested — while healthy eating is always beneficial, masking symptoms without a diagnosis can delay necessary treatment.
- If symptoms are severe — particularly rapid weight loss, vomiting, confusion, or difficulty breathing — seek emergency care, as these may indicate diabetic ketoacidosis.
While awaiting your appointment, focusing on your overall health is sensible. Regular physical activity, even moderate walking, improves insulin sensitivity. A structured exercise guide can help you build sustainable habits that support blood sugar regulation.
How Can You Manage or Prevent Diabetes Through Lifestyle Changes?
For prediabetes and Type 2 diabetes, lifestyle changes are the most powerful tool available — and in many cases, they’re more effective than medication alone in the early stages.
Diet:
- Prioritize whole foods: vegetables, legumes, whole grains, lean proteins, and healthy fats
- Reduce refined carbohydrates and added sugars, which spike blood sugar rapidly
- Increase dietary fiber — fiber slows glucose absorption and improves insulin sensitivity. High-fiber foods are among the most accessible tools for blood sugar management
- Avoid sugary beverages, including fruit juice — liquid sugar raises blood glucose faster than almost any other food source
- Eating healthy, balanced meals consistently throughout the day helps prevent blood sugar spikes and crashes
Exercise:
- Aim for at least 150 minutes of moderate-intensity aerobic activity per week (e.g., brisk walking, cycling, swimming)
- Resistance training two or more days per week improves muscle glucose uptake
- Even short walks after meals (10–15 minutes) measurably reduce post-meal blood sugar spikes
- Home workouts without equipment are a practical starting point for people who are new to regular exercise
Weight management:
- Losing 5–10% of body weight in people with prediabetes or early Type 2 diabetes can significantly improve blood sugar control
- Weight loss doesn’t need to be dramatic to be effective — even modest reductions improve insulin sensitivity
Monitoring:
- If diagnosed, monitor blood sugar at home as directed by your doctor
- Keep a log of readings, meals, and activity to identify patterns
- Attend regular check-ups to assess kidney function, eye health, blood pressure, and cholesterol
Medications:
- Metformin is the most commonly prescribed first-line medication for Type 2 diabetes and is also used in some prediabetes cases
- Type 1 diabetes always requires insulin therapy
- Never adjust or stop diabetes medications without consulting your doctor
Frequently Asked Questions About Diabetes Early Signs
Q: Can you have diabetes with no symptoms at all?
Yes. Type 2 diabetes frequently develops without noticeable symptoms, especially in the early stages. This is why routine screening is recommended for adults with risk factors, even if they feel completely healthy.
Q: How quickly do early diabetes symptoms appear?
In Type 1 diabetes, symptoms can appear suddenly over days to weeks. In Type 2 diabetes, symptoms typically develop gradually over months or years — and may go unnoticed until a routine blood test reveals elevated glucose.
Q: Is frequent urination always a sign of diabetes?
Not necessarily. Frequent urination can also be caused by a urinary tract infection, overactive bladder, excessive fluid intake, certain medications, or prostate issues in men. However, when it occurs alongside excessive thirst and fatigue, diabetes becomes a more likely explanation and warrants testing.
Q: Can stress cause blood sugar to rise and mimic diabetes symptoms?
Yes. Stress hormones like cortisol and adrenaline raise blood sugar levels temporarily. Chronic stress can contribute to insulin resistance over time. However, stress-induced blood sugar changes are generally transient — if symptoms persist, a blood test is the only way to know for certain.
Q: What is the difference between prediabetes and diabetes?
Prediabetes means blood sugar levels are higher than normal but not yet high enough for a diabetes diagnosis. It’s a warning stage. Without intervention, prediabetes often progresses to Type 2 diabetes within 5–10 years — but with lifestyle changes, that progression can be stopped or reversed.
Q: Can children develop Type 2 diabetes?
Yes, and rates have been rising. While Type 2 diabetes was historically considered an adult condition, increasing rates of childhood obesity and sedentary behavior have made it more common in adolescents. Type 1 diabetes remains the more common form in children and young adults.
Q: Are tingling feet always a sign of diabetes?
Tingling feet have multiple causes, including vitamin B12 deficiency, poor circulation, and nerve compression. However, persistent tingling or numbness in both feet — especially with other diabetes symptoms — warrants a blood sugar test.
Q: What’s the fastest way to get tested for diabetes?
A fasting blood glucose test or A1C test ordered by a doctor is the most reliable approach. Many pharmacies and community health clinics also offer walk-in glucose screening. At-home glucose meters can provide a quick snapshot, but they don’t replace a formal diagnostic test.
Q: Can diabetes be reversed?
Type 2 diabetes can go into remission — meaning blood sugar returns to normal levels without medication — through significant weight loss, dietary changes, and exercise. This is most achievable in the early stages of the disease. Type 1 diabetes cannot currently be reversed, as it involves permanent loss of insulin-producing cells.
Q: How does gut health relate to diabetes risk?
Research increasingly links gut microbiome composition to insulin sensitivity and metabolic health. A diet rich in fiber and fermented foods supports a healthier gut environment. For more on this connection, see our guide on gut health and digestive wellness.
Conclusion
The early signs of diabetes — frequent urination, excessive thirst, unexplained weight loss, persistent fatigue, blurred vision, slow-healing wounds, and tingling in the extremities — are the body’s way of signaling that blood sugar regulation is breaking down. Recognizing these signs early and acting on them is the single most important step you can take to protect your long-term health.
Diabetes is manageable. With the right combination of medical care, dietary adjustments, regular physical activity, and consistent monitoring, millions of people live full, healthy lives with this condition. The key is not waiting until symptoms become severe or complications develop.
If you recognize several of these signs in yourself or someone you care about, make an appointment with a healthcare provider this week. A simple blood test can provide clarity — and early clarity changes outcomes.
Sources
- Centers for Disease Control and Prevention. National Diabetes Statistics Report, 2024. cdc.gov/diabetes
- National Institutes of Health. Diabetes Prevention Program Outcomes Study. niddk.nih.gov
- CDC. Diabetic Neuropathy. cdc.gov/diabetes/library
- American Diabetes Association. Standards of Medical Care in Diabetes — 2024. diabetes.org
- U.S. Preventive Services Task Force. Screening for Prediabetes and Type 2 Diabetes, 2021. uspreventiveservicestaskforce.org

