The Best Anti-Inflammatory Foods for Gut Health: A Complete Guide

Last updated: May 4, 2026
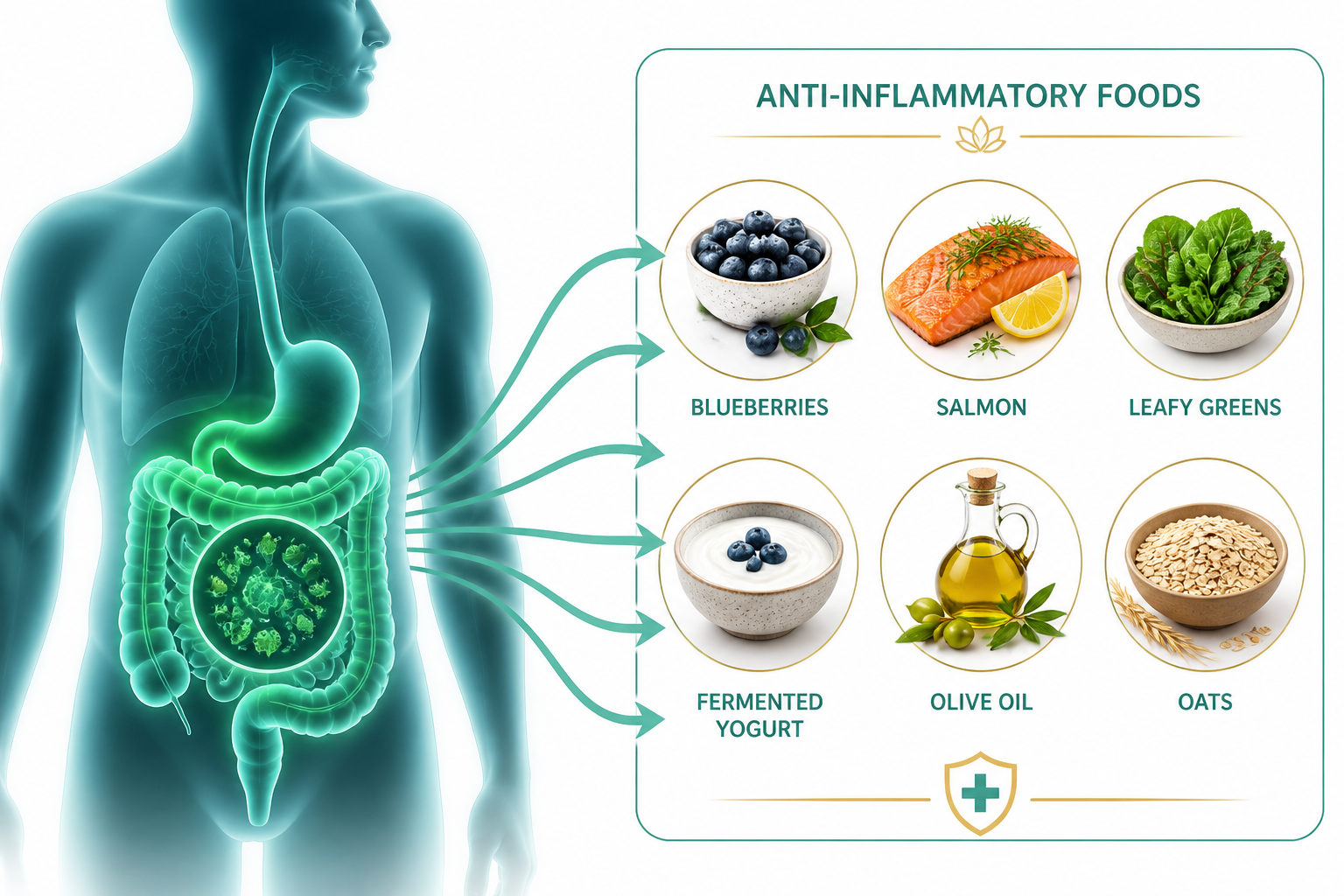
Quick Answer: The best anti-inflammatory foods for gut health include fermented foods (kefir, yogurt, kimchi), high-fiber vegetables, leafy greens, fatty fish, berries, olive oil, and prebiotic-rich allium vegetables like garlic and onions. These foods work by feeding beneficial gut bacteria, reducing inflammatory signalling in the gut lining, and supporting a diverse microbiome. No single food does the job alone — the pattern matters more than any individual item.
Key Takeaways
- Gut inflammation and systemic inflammation are connected. What happens in your digestive tract influences immune responses throughout the body.
- Fermented foods with live cultures (kefir, sauerkraut, kimchi, yogurt) directly support microbiome diversity and may reduce gut inflammation markers. [1][3]
- Prebiotic foods — garlic, onions, leeks — feed the beneficial bacteria already in your gut. [2]
- Omega-3 fatty acids from fatty fish and plant sources (walnuts, chia, flaxseed) are among the most consistently supported anti-inflammatory nutrients in the research. [1]
- Leafy greens provide vitamins A, C, and K alongside antioxidants that support immune regulation and tissue repair. [1]
- Whole grains like oats and barley contain beta-glucan, a soluble fiber with well-documented gut health benefits. [1]
- Polyphenol-rich foods — berries, olive oil, dark chocolate, green tea — reduce oxidative stress in gut tissue. [2]
- Dietary pattern beats individual foods. The Mediterranean-style eating approach consistently outperforms single-food interventions in the evidence.
- Processed foods, refined sugars, and seed oils work against everything on this list. You cannot out-eat a poor baseline diet.
- A sensible starting point is adding two or three foods from this guide consistently, rather than overhauling everything at once.
Table of Contents
- Why Does Gut Inflammation Matter in the First Place?
- What Makes a Food Anti-Inflammatory for the Gut Specifically?
- The Best Anti-Inflammatory Foods for Gut Health: Core Categories
- How Do These Foods Work Together? The Pattern Matters
- A Practical Anti-Inflammatory Gut Health Food Reference
- What About Supplements? Can They Replace These Foods?
- Common Mistakes When Eating for Gut Anti-Inflammation
- The Best Anti-Inflammatory Foods for Gut Health: A Simple Starting Framework
- FAQ: The Best Anti-Inflammatory Foods for Gut Health
- Conclusion: What Actually Matters

Why Does Gut Inflammation Matter in the First Place?
Gut inflammation is not just a digestive problem. The gut lining hosts roughly 70% of the body’s immune cells, and when that lining is chronically irritated, the immune system stays in a low-level alert state that affects the whole body. [4]
In plain English: a chronically inflamed gut does not just cause bloating or discomfort. Over time, it is associated with fatigue, mood disruption, joint pain, and a higher risk of metabolic disease. The gut-brain axis is a real and well-studied communication network — what happens in the gut genuinely affects how you think and feel.
Here’s the real issue: most people treat gut symptoms without addressing the food environment that drives them. Anti-inflammatory eating is not a cure for diagnosed conditions, but it is one of the most practical and evidence-supported levers available.
What drives gut inflammation?
- Low dietary fiber intake (starves beneficial bacteria)
- High intake of ultra-processed foods and refined sugar
- Chronic stress and poor sleep (yes, these affect the gut directly)
- Overuse of certain medications, including NSAIDs
- Low microbiome diversity — fewer bacterial species, weaker gut defence
The foods covered in this guide address several of these drivers simultaneously.
What Makes a Food Anti-Inflammatory for the Gut Specifically?
Not every anti-inflammatory food is equally useful for gut health. A food qualifies on both counts when it does at least one of the following:
- Feeds beneficial gut bacteria (prebiotic effect)
- Introduces live bacteria directly (probiotic effect)
- Reduces oxidative stress in gut tissue (antioxidant polyphenols)
- Supports the integrity of the gut lining (specific vitamins, short-chain fatty acids)
- Modulates inflammatory signalling pathways (omega-3s, certain plant compounds)
The evidence suggests that foods doing more than one of these things simultaneously offer the most practical benefit. [2][4] That is why fermented vegetables, fatty fish, and leafy greens appear on nearly every credible list — they are multi-mechanism foods, not single-trick items.
“There is no magic in it. The strongest evidence points to dietary patterns, not superfoods.”
The Best Anti-Inflammatory Foods for Gut Health: Core Categories
This is where the guide earns its place. Let’s keep this practical and work through the food categories that have the clearest evidence behind them.
🥬 1. Leafy Greens
Spinach, kale, Swiss chard, and collard greens are among the most nutrient-dense foods available. They provide vitamins A, C, and K, alongside a range of antioxidants that support immune regulation and tissue repair in the gut lining. [1]
- Vitamin K plays a role in gut barrier function and has anti-inflammatory properties at the cellular level
- Vitamin C supports collagen synthesis in gut tissue
- Magnesium (found in dark leafy greens) supports hundreds of enzymatic reactions, including those involved in inflammation control
Practical point: Raw spinach and cooked kale are both useful — cooking breaks down some oxalates in spinach, which can improve mineral absorption. Aim for at least one serving of dark leafy greens daily.
🫐 2. Berries and Polyphenol-Rich Fruits
Blueberries, raspberries, blackberries, and cherries are high in anthocyanins — a class of polyphenol with documented antioxidant and anti-inflammatory activity. [2]
The stronger evidence points to polyphenols reducing oxidative stress in gut tissue and selectively feeding beneficial bacterial strains. For more on how polyphenols work, see what polyphenols are and why they matter.
Choose berries if: You want a high-impact, low-effort addition. A handful of frozen blueberries in oatmeal or yogurt is one of the simplest and most consistent anti-inflammatory habits available.
🐟 3. Fatty Fish
Salmon, mackerel, sardines, and trout are the most direct dietary sources of EPA and DHA — the long-chain omega-3 fatty acids with the most consistent anti-inflammatory evidence. [2][4]
The mechanism is well-established: EPA and DHA compete with arachidonic acid in inflammatory pathways, reducing the production of pro-inflammatory compounds called prostaglandins and leukotrienes.
Hopkins Medicine identifies omega-3-rich fish as a cornerstone of anti-inflammatory eating, and the evidence for this is considerably stronger than for most other individual foods. [4]
Practical guidance:
- Two to three servings of fatty fish per week is the commonly recommended target
- Canned sardines and mackerel are cost-effective and nutritionally comparable to fresh options
- If fish is not an option, walnuts, chia seeds, and flaxseeds provide ALA (alpha-linolenic acid), though the conversion to EPA and DHA is inefficient [1]
🧄 4. Prebiotic Allium Vegetables
Garlic, onions, leeks, and shallots contain inulin and fructooligosaccharides (FOS) — prebiotic fibers that feed Bifidobacterium and Lactobacillus species in the colon. [2][3]
This matters because these bacterial species produce short-chain fatty acids (SCFAs), particularly butyrate, which is the primary fuel source for colonocytes (gut lining cells) and has direct anti-inflammatory effects on the gut mucosa.
Context matters: Raw garlic and onions deliver more prebiotic fiber than cooked versions, though lightly cooked still provides benefit. For people with IBS or FODMAP sensitivity, high doses of these foods can worsen symptoms — this is one case where more is not always better.
For a broader look at how prebiotics and probiotics work together, the complete guide to probiotics vs prebiotics covers the mechanisms clearly.
🫙 5. Fermented Foods with Live Cultures
This category has gained significant research attention over the past five years, and for good reason. Yogurt, kefir, sauerkraut, kimchi, and miso introduce live bacterial strains directly into the gut environment. [1][3]
A 2021 Stanford study (published in Cell) found that a high-fermented-food diet increased microbiome diversity and reduced markers of immune activation more effectively than a high-fiber diet alone — a finding that challenged some prior assumptions about fiber being the primary lever.
What to look for:
- Refrigerated products, not shelf-stable pasteurized versions (heat kills the cultures)
- Labels that say “contains live and active cultures”
- Plain, unsweetened yogurt and kefir — added sugar works against the anti-inflammatory goal
Common mistake: Buying yogurt marketed as probiotic but loaded with added sugar. The sugar content partially offsets the benefit.
🫒 6. Extra Virgin Olive Oil
Extra virgin olive oil (EVOO) contains oleocanthal, a polyphenol compound that inhibits the same inflammatory enzymes (COX-1 and COX-2) targeted by ibuprofen — at much lower potency, but with consistent dietary exposure. [2][4]
The evidence on olive oil’s health benefits is among the most robust of any single food, largely because of the Mediterranean diet research base. EVOO also supports the absorption of fat-soluble vitamins (A, D, E, K) from vegetables eaten alongside it.
Practical point: Use EVOO as a primary cooking fat and dressing base. The anti-inflammatory polyphenols are heat-sensitive, so low-to-medium heat cooking and raw applications preserve more of the benefit.
🌾 7. Whole Grains (Especially Oats and Barley)
Oats and barley contain beta-glucan, a soluble fiber with well-documented effects on gut microbiome composition, cholesterol management, and blood sugar regulation. [1]
Beta-glucan is fermented by gut bacteria into SCFAs, particularly butyrate and propionate, which reduce gut inflammation and support barrier integrity. This is a different mechanism from the direct antioxidant effect of polyphenols — it works through the microbiome.
For a deeper look at fiber types and daily targets, see the complete guide to high fiber foods.
Choose oats if: You want a practical, affordable, and evidence-backed breakfast option. Steel-cut and rolled oats retain more beta-glucan than instant varieties.
🫘 8. Legumes
Lentils, black beans, chickpeas, and kidney beans deliver plant protein, soluble fiber, and polyphenols in a single package. Their slow-digesting carbohydrates avoid the blood sugar spikes that drive systemic inflammation. [1]
Legumes are foundational in the Mediterranean and DASH dietary patterns — both of which have strong anti-inflammatory evidence behind them. They are also among the most cost-effective foods on this list.
Edge case: Some people experience significant gas and bloating from legumes, particularly if they are not regular consumers. Starting with smaller portions (two to three tablespoons) and increasing gradually allows the gut microbiome to adapt.

How Do These Foods Work Together? The Pattern Matters
The simplest way to look at it is this: individual foods create conditions. Dietary patterns create outcomes.
No single food on this list will meaningfully change gut inflammation on its own. But a consistent eating pattern that includes several of these categories — leafy greens, fermented foods, prebiotic vegetables, omega-3 sources, and polyphenol-rich fruits — creates a gut environment that is structurally different from one built on ultra-processed food. [4][5]
The Mediterranean dietary pattern is the most studied example of this approach, and the evidence for its anti-inflammatory effects is substantially stronger than for any individual supplement or superfood. [4] For practical meal ideas that follow this pattern, the Mediterranean food guide is worth exploring.
What to reduce alongside adding these foods:
- Ultra-processed foods (emulsifiers and additives disrupt gut barrier function)
- Refined sugar and high-fructose corn syrup (feed pro-inflammatory bacterial species)
- Excessive alcohol (damages gut lining and reduces microbiome diversity)
- Trans fats and highly refined seed oils in large quantities
A Practical Anti-Inflammatory Gut Health Food Reference
| Food Category | Key Compounds | Primary Gut Benefit | Ease of Use |
|---|---|---|---|
| Leafy greens | Vitamins A, C, K; antioxidants | Gut lining support, immune regulation | ⭐⭐⭐⭐⭐ |
| Berries | Anthocyanins, polyphenols | Reduces oxidative stress, feeds beneficial bacteria | ⭐⭐⭐⭐⭐ |
| Fatty fish | EPA, DHA (omega-3s) | Reduces inflammatory signalling | ⭐⭐⭐⭐ |
| Garlic/onions/leeks | Inulin, FOS | Feeds beneficial bacteria, boosts SCFA production | ⭐⭐⭐⭐ |
| Fermented foods | Live bacterial cultures | Increases microbiome diversity | ⭐⭐⭐⭐ |
| Extra virgin olive oil | Oleocanthal, polyphenols | COX enzyme inhibition, fat-soluble vitamin absorption | ⭐⭐⭐⭐⭐ |
| Oats/barley | Beta-glucan | SCFA production, microbiome support | ⭐⭐⭐⭐⭐ |
| Legumes | Fiber, polyphenols, plant protein | Microbiome diversity, blood sugar stability | ⭐⭐⭐⭐ |
| Walnuts/chia/flaxseed | ALA (plant omega-3) | Anti-inflammatory support for plant-based diets | ⭐⭐⭐⭐ |
| Ginger | Gingerols, shogaols | Digestive comfort, inflammation pathway influence | ⭐⭐⭐⭐ |
What About Supplements? Can They Replace These Foods?
Here’s where hype gets in the way of sensible decision-making. The supplement industry has built an enormous market around gut health and anti-inflammation — probiotics, fish oil capsules, curcumin extracts, and prebiotic powders are all heavily marketed.
That is a strong claim and needs strong proof. The honest answer is that food-based sources consistently outperform isolated supplements in the research, for several reasons:
- Food provides co-factors. Olive oil delivers oleocanthal alongside vitamin E, polyphenols, and healthy fats that work together. A capsule delivers one isolated compound.
- Bioavailability is often better from food. The matrix of a whole food affects how compounds are absorbed and metabolised.
- Supplements do not replace a poor dietary pattern. A fish oil capsule does not undo the inflammatory effect of a diet high in ultra-processed food.
Where supplements have a reasonable role:
- Omega-3 fish oil for people who genuinely cannot or will not eat fatty fish two to three times per week
- Probiotic supplements during or after antibiotic use
- Specific therapeutic situations under medical guidance
I would be careful with broad supplement stacks marketed for “gut repair” or “inflammation reduction” without specific clinical indication. Start with what gives the biggest return, and that is almost always the food.
For people dealing with specific digestive conditions, the science-backed 4-week gut reset guide provides a structured approach grounded in evidence rather than marketing claims.
Common Mistakes When Eating for Gut Anti-Inflammation
1. Adding anti-inflammatory foods without removing inflammatory ones
Eating blueberries with breakfast is not meaningful if the rest of the day is built around ultra-processed food. The basics still do the heavy lifting.
2. Expecting fast results
Microbiome changes take weeks to months of consistent dietary shifts. [6] This is not a two-week programme.
3. Over-relying on a single food
Turmeric is a good example. The research on curcumin is interesting but largely based on high-dose supplementation, not culinary use. Turmeric in food is valuable as part of a broader pattern — not as a standalone intervention.
4. Ignoring fermented foods because they seem unfamiliar
Plain yogurt and kefir are the most accessible entry points. Sauerkraut and kimchi are acquired tastes for some, but a tablespoon alongside a meal is all that is needed.
5. Buying the wrong versions
Pasteurised shelf-stable sauerkraut has no live cultures. Flavoured yogurt with 20g of sugar per serving is not the same as plain Greek yogurt. Read labels.

The Best Anti-Inflammatory Foods for Gut Health: A Simple Starting Framework
Based on current evidence, here is a practical weekly framework that does not require overhauling your entire diet:
Daily non-negotiables (start here):
- One serving of dark leafy greens
- One serving of berries or polyphenol-rich fruit
- Extra virgin olive oil as your primary fat
- One serving of whole grains (oats, barley, or whole wheat)
Three to four times per week:
- Fatty fish (salmon, sardines, mackerel)
- Fermented food with live cultures (plain yogurt, kefir, or a tablespoon of sauerkraut)
- Legumes (lentils, chickpeas, black beans)
Regular use in cooking:
- Garlic and onions as a base for most savoury dishes
- Ginger (fresh or ground) in cooking or tea
- Walnuts or chia seeds added to oatmeal, salads, or yogurt
Keep it simple and consistent. That combination covers fermented foods, prebiotics, omega-3s, polyphenols, and fiber — the main mechanisms — without requiring exotic ingredients or expensive products.
For those looking to understand how digestive wellness fits into a broader health picture, the complete guide to gut health and digestive wellness covers the full context.
FAQ: The Best Anti-Inflammatory Foods for Gut Health
Q: How long does it take for anti-inflammatory foods to make a difference to gut health?
Most people notice digestive changes within two to four weeks of consistent dietary shifts. Measurable microbiome diversity changes typically take six to twelve weeks. Systemic inflammatory markers take longer — months of sustained dietary change. [6]
Q: Is there one single best anti-inflammatory food for gut health?
No. The evidence does not support a single food as decisive. If forced to choose one category, fermented foods with live cultures have the most direct gut-specific evidence in recent research. But they work best as part of a broader dietary pattern.
Q: Can anti-inflammatory eating help with IBS or IBD?
It depends on the condition. Anti-inflammatory dietary patterns are associated with reduced symptom burden in some IBS presentations, and dietary modification is a recognised component of IBD management. However, these are medical conditions that require professional oversight. Food is supportive, not curative, in this context.
Q: Are raw vegetables better than cooked for gut anti-inflammation?
Not always. Cooking increases the bioavailability of some compounds (lycopene in tomatoes, beta-carotene in carrots) while reducing others. A mix of raw and lightly cooked vegetables is the practical answer.
Q: Is coffee anti-inflammatory for the gut?
The evidence on coffee is actually quite positive. Coffee contains polyphenols that feed beneficial gut bacteria and has been associated with reduced inflammatory markers in several large observational studies. The evidence on coffee’s health benefits is more robust than most people expect.
Q: Does dark chocolate count as an anti-inflammatory food for gut health?
High-cocoa dark chocolate (70% or above) contains flavanols that have prebiotic effects and antioxidant activity. The evidence is real but modest. A small daily portion is reasonable — it is not a health food in large quantities.
Q: What foods should I avoid to reduce gut inflammation?
Ultra-processed foods, refined sugar, excessive alcohol, and artificial emulsifiers (found in many packaged foods) are the most consistently identified dietary drivers of gut inflammation. Reducing these has as much impact as adding anti-inflammatory foods. [5]
Q: Do I need to follow a specific diet like Mediterranean or DASH?
Not strictly. These dietary patterns are useful frameworks because they naturally incorporate most of the foods on this list. But you do not need to follow a named diet — you need to eat the right foods consistently.
Q: Is ginger genuinely anti-inflammatory for the gut?
The evidence is promising. Ginger’s active compounds (gingerols and shogaols) have demonstrated effects on inflammatory pathways in laboratory and some clinical research, and it has a long track record for digestive comfort. [1] It is a useful addition but not a primary intervention on its own.
Q: Can children and older adults follow the same anti-inflammatory eating approach?
The core principles apply across age groups. Older adults may benefit particularly from omega-3s and fermented foods given age-related changes in gut microbiome diversity. Children’s portion sizes differ, and any significant dietary changes for children should involve a healthcare provider.
Conclusion: What Actually Matters
The main takeaway is this: gut inflammation is largely diet-driven, and diet is one of the most modifiable factors available to most people.
The best anti-inflammatory foods for gut health are not exotic or expensive. Leafy greens, berries, fatty fish, garlic, fermented foods, olive oil, oats, and legumes are ordinary foods with extraordinary consistency in the evidence. None of them is a magic solution. All of them, used consistently as part of a sensible dietary pattern, create a gut environment that is more resilient, less inflamed, and better equipped to support whole-body health.
The basics still do the heavy lifting. Start with what gives the biggest return — add fermented foods, increase fiber from whole plants, use olive oil as your primary fat, and eat fatty fish two to three times per week. Then build from there.
Truth over hype. Evidence first. Keep it simple and consistent.
For a broader understanding of how natural foods support health across multiple systems, the evidence-based guide to health benefits of natural foods and herbs is a useful next read.
