How to Heal Your Gut: A Science-Backed 4-Week Reset

Last updated: April 19, 2026
- What “Healing Your Gut” Actually Means
- How Do You Know If Your Gut Needs Healing?
- The Myth of the “Gut Cleanse”
- The 4R Framework — A Useful Structure
- The 4-Week Reset Plan: Overview
- Week 1: Remove and Reduce Inflammation
- Week 2: Soothe and Rest the Gut
- Week 3: Reinoculate and Rebuild the Microbiome
- Week 4: Rebuild, Diversify, and Maintain
- Beyond Food: The 3 Non-Dietary Factors That Matter Most
- What to Expect: An Honest Timeline
- Common Pitfalls to Avoid
- When to See a Doctor, Not Just Try a Reset
Quick Answer: Healing your gut means reducing intestinal inflammation, restoring microbial diversity, and supporting your honest evidence-based take on leaky gut and gut lining health — and a structured 4-week plan built around food changes, adequate sleep, and stress management can produce measurable improvements. No expensive supplements required. The process is not fast, but it is straightforward if you follow a consistent, phased approach.
Key Takeaways
- “Leaky gut” is not a recognized clinical diagnosis, but increased intestinal permeability and gut dysbiosis are real, measurable conditions that respond to dietary and lifestyle changes.
- A 4-week reset is enough to establish new habits and see meaningful improvements, but deeper gut repair — especially for serious imbalances — takes 60–90 days of consistency.
- The 4R framework (Remove, Replace, Reinoculate, Repair) gives the reset its structure and is grounded in functional medicine principles that align with mainstream nutritional science.
- Most people notice reduced bloating and better energy within the first 7–14 days. Brain fog and skin improvements tend to follow in weeks 3–4.
- Food is the primary tool. Fermented foods, prebiotic full fiber decoded guide with daily targets by age and sex, and diverse plant intake do more than any supplement stack.
- Sleep and stress are not optional add-ons. Chronic stress and poor sleep measurably reshape the microbiome within days.
- If you have persistent pain, blood in stool, unexplained weight loss, or symptoms worsening over two weeks — see a doctor, not a wellness blog.
- Consistency beats perfection. The microbiome adapts to what you do most of the time, not what you do perfectly once.
What “Healing Your Gut” Actually Means
Healing your gut is not a single event — it is a process of reducing inflammation, restoring microbial balance, and supporting the physical barrier between your digestive tract and your bloodstream.
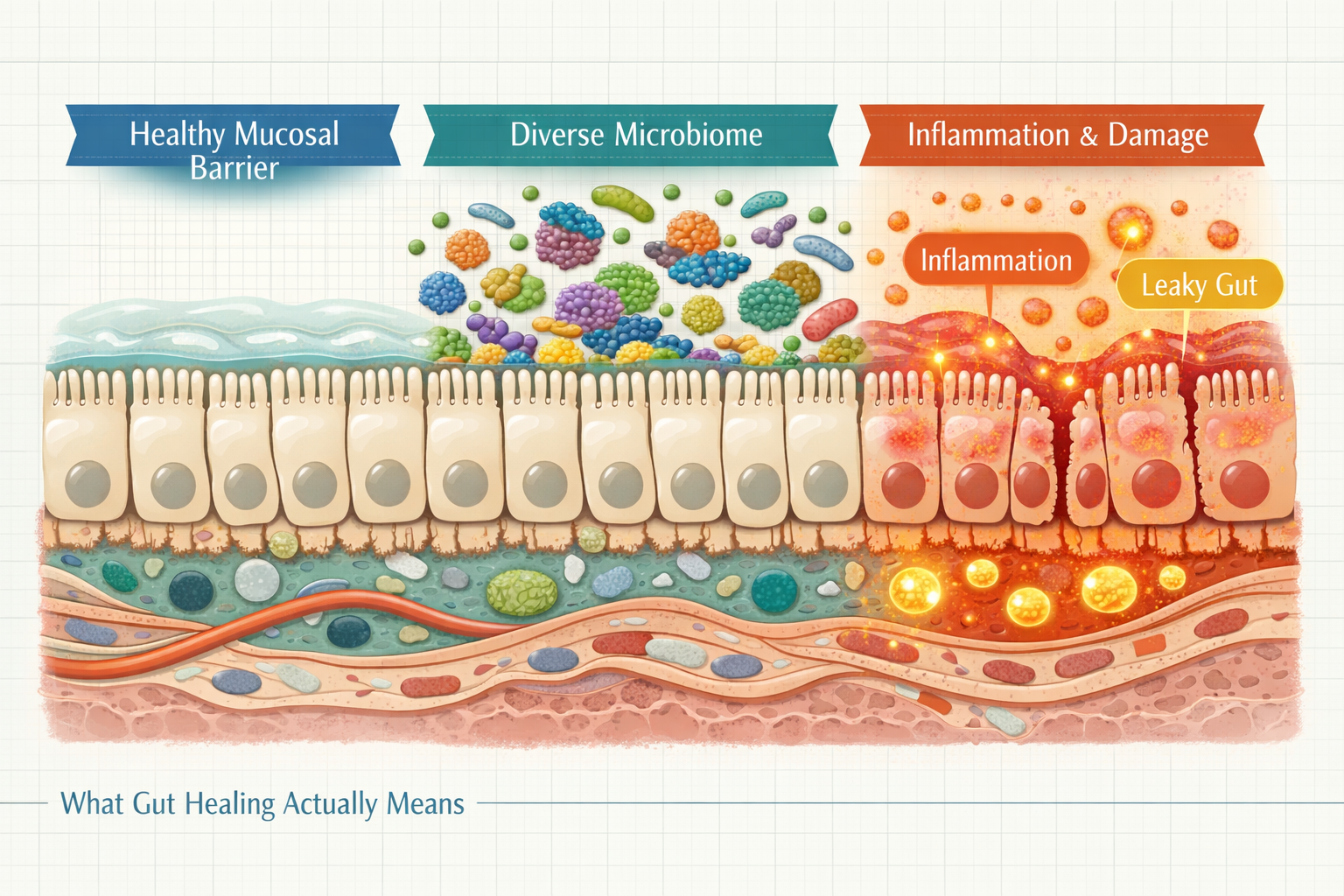
Your gut is home to roughly 38 trillion microorganisms — bacteria, fungi, and viruses — that collectively influence digestion, immunity, mood, and metabolism. When this ecosystem is balanced, things run quietly in the background. When it is not, you feel it.
In plain English, when people say their gut is “off,” three things are usually happening in some combination:
1. Dysbiosis — The microbial community has shifted. There are fewer beneficial species, less diversity overall, and often an overgrowth of bacteria or yeast that produce gas, drive cravings, and create low-level inflammation.
2. Intestinal inflammation — The lining of the gut becomes irritated. Common triggers include alcohol, ultra-processed foods, chronic stress, certain medications (particularly NSAIDs and antibiotics), and food sensitivities. Inflamed gut tissue does not absorb nutrients efficiently and sends distress signals throughout the body.
3. Increased intestinal permeability — This is the scientific term for what wellness circles call “leaky gut.” The tight junctions between cells in the gut lining become less selective, allowing bacterial fragments and undigested particles to pass into the bloodstream and trigger immune responses. This is a real, documented phenomenon. It is also contested as a standalone diagnosis — most mainstream medical bodies do not recognize “leaky gut syndrome” as a formal condition, and the evidence connecting it to the wide range of symptoms claimed online is still developing. I would be careful with any source that presents it as a settled diagnosis with a definitive cure.
What healing actually means, then, is reducing inflammation, restoring microbial diversity, and supporting the mucosal barrier. All three are achievable. None of them happen in three days.
How Do You Know If Your Gut Needs Healing?
The honest answer is that most of the symptoms associated with poor gut health are also symptoms of a dozen other things. That said, a pattern of several of these signals together — especially if they appeared gradually or worsened after a stressful period or course of antibiotics — is worth taking seriously.
Common signals that your gut may need support:
- Frequent bloating, gas, or abdominal discomfort after meals
- Irregular bowel movements (constipation, loose stools, or alternating between both)
- Fatigue that does not match your sleep quality
- Brain fog or difficulty concentrating, particularly after eating
- Strong and frequent cravings for sugar or refined carbohydrates
- Skin issues such as acne, eczema, or unexplained rashes
- Food sensitivities that appeared or worsened in adulthood
- Mood shifts, low-grade anxiety, or irritability without clear cause
The gut-brain axis is real — the vagus nerve connects the gut and brain bidirectionally, and gut bacteria produce neurotransmitters including serotonin and GABA. So mood and cognition symptoms alongside digestive ones are not coincidental.
⚠️ See a doctor — not a blog — if you have: persistent abdominal pain, blood in your stool, unexplained weight loss, or any severe symptoms lasting more than three weeks. These are not “gut reset” territory. They require proper investigation.
The Myth of the “Gut Cleanse”
Let’s call it what it is: most products and protocols marketed as gut cleanses are built on hype, not evidence.
Here is what the evidence does not support:
- ❌ 3-day juice cleanses — These produce a laxative effect and caloric restriction. They do not “reset” the microbiome. Bacterial populations take weeks to shift meaningfully, not days.
- ❌ Expensive “leaky gut” supplement stacks — Most lack robust clinical evidence. That is a strong claim and needs strong proof, and that proof is largely absent for the majority of products in this category.
- ❌ Colon hydrotherapy (colonics) — Not supported by evidence for gut health improvement and carries real risks including electrolyte imbalance and bowel perforation in rare cases.
- ❌ Eliminating all “inflammatory foods” permanently — Unsustainable, often unnecessary, and can create new nutritional gaps and disordered eating patterns.
We need to separate fact from hype here. What actually works is less exciting: consistent, modest food changes sustained over four or more weeks, combined with better sleep and lower stress. There is no magic in it. But it works.
The 4R Framework — A Useful Structure
The 4R protocol comes from functional medicine, a field with a mixed evidence base. But the framework itself — Remove, Replace, Reinoculate, Repair — maps reasonably well onto what mainstream nutritional science supports. It is a sensible starting point.
Remove — Eliminate the main drivers of gut inflammation for the reset period: alcohol, added sugar, ultra-processed foods, and any personal triggers you have identified (often gluten or dairy for some people).
Replace — Support digestion with what it needs: adequate fiber, hydration, and foods that stimulate stomach acid and bile production naturally (bitter greens, apple cider vinegar in small amounts, lemon water).
Reinoculate — Introduce beneficial bacteria through fermented foods and feed existing beneficial bacteria with prebiotic fiber. This is where the microbiome rebuilding happens.
Repair — Provide the raw materials the gut lining needs: glutamine-rich foods (meat, fish, eggs, cabbage), zinc (pumpkin seeds, meat, legumes), omega-3 fatty acids (oily fish, flaxseed), and polyphenols (berries, olive oil, green tea).
The evidence suggests that all four components matter and that skipping any one of them slows progress. Most people focus on reinoculation (probiotics) and skip removal entirely — which is like trying to fill a bucket that still has holes in it.
The 4-Week Reset Plan: Overview
Here is the phased structure. Each week has a clear focus, and the phases build on each other deliberately.

| Week | Focus | Key Actions |
|---|---|---|
| Week 1 | Remove — reduce inflammation | Cut alcohol, added sugar, ultra-processed foods; limit caffeine |
| Week 2 | Soothe — rest the gut | Bland, easily-digested foods; bone broth; avoid raw cruciferous vegetables |
| Week 3 | Reinoculate — rebuild microbiome | Add fermented foods and prebiotic fiber daily |
| Week 4 | Rebuild and maintain | Diverse plant foods, sustainable routine, reintroduce any removed foods methodically |
Research shows that improvements become visible by week two, with more significant changes by weeks three and four [2]. The four-week window is enough to establish new habits and see real change — but it is a foundation, not a finish line [2].
Week 1: Remove and Reduce Inflammation
Goal: Lower the inflammatory load so healing can begin.
This is the week most people find hardest, because it requires cutting things they rely on daily. Keep it simple and consistent.
Cut completely for 28 days:
- Alcohol (all forms)
- Added sugar — read labels carefully; it appears in bread, sauces, yogurt, and almost everything packaged
- Ultra-processed foods — a practical rule: if it has more than five ingredients you cannot picture in their natural form, put it back
- Excess caffeine — one coffee per day maximum; switch to green tea for additional cups if needed
- Gluten and dairy — only if you have already suspected these as personal triggers; do not eliminate them without reason
Keep or add:
- Water — a practical baseline is roughly half your body weight in ounces daily
- Anti-inflammatory foods: fatty fish (salmon, mackerel, sardines), leafy greens, berries, turmeric, ginger
- Sleep — 7–8 hours is non-negotiable here; sleep deprivation directly disrupts gut bacteria within days [1]
What to expect in Week 1:
- Days 2–4: possible headache, irritability, and increased cravings — this is sugar and caffeine withdrawal and it is normal
- Days 5–7: energy begins to stabilize; bloating often reduces noticeably
A practical elimination protocol removes grains, legumes, dairy, nuts, seeds, and eggs for the first week, basing meals on protein (fish, poultry, meat) plus cooked vegetables and healthy fats, with 1–2 litres of water daily [3]. After the elimination phase, food groups are reintroduced one at a time to identify individual triggers [3].
If symptoms flare during this adjustment period, digestive enzymes with meals, bitters taken 5–10 minutes before eating, and peppermint or ginger tea after meals can help ease the transition [3].
Week 2: Soothe and Rest the Gut
Goal: Reduce the digestive workload while the gut lining calms down.
This is the quietest week of the reset. The aim is not to add anything dramatic — it is to give the gut a lower-effort environment to begin recovering.
A practical daily template:
- Morning: Warm lemon water or a cup of bone broth
- Breakfast: Cooked oats with banana, or soft scrambled eggs
- Lunch: White rice or quinoa with well-cooked vegetables and lean protein
- Snack: Banana, applesauce, or chamomile tea
- Dinner: Soup or stew with tender meat or fish and soft-cooked vegetables
- Evening: Chamomile or ginger tea
Avoid this week:
- Raw salads — harder to digest than most people realise when the gut is irritated
- Raw cruciferous vegetables (broccoli, cauliflower, cabbage) — cook them thoroughly instead
- Beans and legumes — can worsen bloating before the gut has settled
- Spicy food
- Very cold drinks — room temperature or warm is easier on the gut
Why bone broth? It provides gelatin and glycine, which support the mucosal lining. The evidence for bone broth specifically is limited but plausible, and it is a practical, low-irritation food that fits the week’s goal well.
A 12–14 hour overnight fast — finishing dinner by 7pm and eating breakfast at 8am — supports the migrating motor complex, the gut’s overnight cleaning cycle, and may enhance microbial diversity when used consistently [1]. This is gentle intermittent fasting in practice, not a dramatic protocol.
Week 3: Reinoculate and Rebuild the Microbiome
Goal: Restore microbial diversity through food, not supplements.
This is where the reset starts to feel different. Most people notice clearer energy and quieter digestion by the end of this week.

Add daily:
- One serving of fermented food: kefir, natural yogurt with live cultures, kimchi, sauerkraut, or miso. Start small — one tablespoon of sauerkraut, then two, then three — to avoid the temporary gas and bloating that can come from introducing fermented foods too quickly.
- One serving of prebiotic fiber: oats, garlic, onions, leeks, asparagus, or a slightly green banana. These feed the beneficial bacteria you are trying to grow.
- One serving of polyphenol-rich food: berries, dark chocolate (70% or higher), extra-virgin olive oil, or green tea. Polyphenols act as fuel for beneficial bacteria and have anti-inflammatory properties.
Resistant starch foods — cooked and cooled potatoes or rice, green bananas, lentils, beans, and oats — are particularly useful in this phase because they fuel beneficial bacteria in the colon and support butyrate production [1]. Butyrate is a short-chain fatty acid that plays a key role in gut lining integrity and inflammation control.
On probiotic supplements: Skip the pressure to buy an expensive probiotic capsule. Food sources do the heavy lifting here. Supplements are optional and may be useful in specific circumstances (post-antibiotic recovery, for example), but they are not a substitute for dietary change.
The stronger evidence points to dietary diversity — not supplementation — as the primary driver of microbiome recovery.
Week 4: Rebuild, Diversify, and Maintain
Goal: Build a sustainable long-term eating pattern you can actually keep.
The main takeaway from the research on gut microbiome diversity is this: people who eat 30 or more different plant foods per week consistently show greater microbial diversity than those eating fewer. That 30-plant target counts everything — herbs, spices, nuts, seeds, grains, legumes, fruits, and vegetables all contribute.
Weekly habits to lock in:
- 1–2 servings of fermented foods daily
- Hit your fiber target (roughly 25g for women, 38g for men)
- Two servings of oily fish per week
- Limit ultra-processed foods to occasional, not regular
- Reintroduce alcohol thoughtfully, or not at all — this is a good moment to reassess your baseline
Reintroduction testing (if you removed gluten or dairy in Week 1):
Reintroduce one food group at a time, three days apart, and note any symptoms. This is the only reliable way to identify personal triggers without expensive testing. Keep a simple food and symptom journal for this phase.
From a practical point of view, Week 4 is less about adding new things and more about making the previous three weeks feel normal. Consistency over perfection is the operating principle. The microbiome adapts to what you do most consistently — small daily habits including hydration, fiber, movement, and rest compound into lasting results [1].
Beyond Food: The 3 Non-Dietary Factors That Matter Most
Many gut reset guides focus entirely on food and skip the factors that can undo all of it. Here is what the evidence says actually matters alongside diet.

Sleep
Gut bacteria follow a circadian rhythm. Poor sleep measurably reduces microbial diversity within days — not weeks. Aim for 7–8 hours with a consistent bedtime. A screen-free wind-down ritual in the hour before bed supports both melatonin production and microbial repair [1].
Stress
Chronic cortisol elevation reduces beneficial microbes and weakens digestion directly [1]. The gut and brain communicate via the vagus nerve, and this connection runs both ways — stress reshapes the microbiome, and a disrupted microbiome amplifies stress responses.
The practical intervention does not need to be complicated. Five minutes of slow breathing before meals, a 20-minute walk, or a consistent wind-down routine before sleep are enough to move the needle. You do not need a meditation app or a yoga retreat.
Movement
Moderate daily activity — and walking counts — increases microbial diversity independently of diet. This effect is well-documented and does not require intense exercise. In real-world terms, 30 minutes of walking most days is a meaningful gut health intervention.
What to Expect: An Honest Timeline
Let’s keep this practical. Here is what most people experience, based on available evidence and reported outcomes [2]:
| Timeframe | What Typically Happens |
|---|---|
| Days 1–7 | Possible headache, irritability, increased bloating before it reduces |
| Week 2 | Digestion feels quieter; cravings reduce; energy begins to stabilise |
| Weeks 3–4 | Energy more consistent; brain fog lifts for most people; skin often improves |
| Months 2–3 | Deeper changes — microbial diversity and gut lining repair take 60–90 days of consistency |
One documented account describes significant energy improvements by week three after adding fiber-rich and fermented foods, with better sleep quality than in years [2]. That kind of result is realistic — but it requires getting through the first two weeks, which is where most people quit.
Caveat: If symptoms worsen and stay worse for more than 7–10 days, that is a signal to see a doctor, not to push through.
Common Pitfalls to Avoid
Based on what typically derails people, here are the mistakes worth knowing in advance:
- Trying to do everything in Week 1 — adding supplements, cutting ten food groups, starting a new exercise routine simultaneously. Pick one change per category and build.
- Confusing initial gas and bloating for failure — when you add fermented foods and prebiotic fiber, temporary gas is normal. It usually settles within a week.
- Supplementing instead of eating real food — a probiotic capsule does not compensate for a diet of ultra-processed food.
- Quitting at Day 22 — progress often feels slow around Day 18. This is normal. The changes are happening; they are just not visible yet.
- Using the reset as a weight-loss plan — different goal, different rules. Conflating the two creates confusion and sets up the wrong success metrics.
- Ignoring sleep and stress entirely — you can eat perfectly and still plateau if cortisol is chronically elevated and sleep is poor.
When to See a Doctor, Not Just Try a Reset
A 4-week gut reset is appropriate for generally healthy adults who suspect their gut is imbalanced and want to make structured improvements. It is not appropriate as a substitute for medical care in the following situations:
- Persistent abdominal pain that does not resolve
- Blood in stool (any amount)
- Unexplained weight loss
- Symptoms that worsen over two or more weeks despite dietary changes
- Existing diagnosis of IBD, Crohn’s disease, or celiac disease — work with your gastroenterologist, not a reset plan
- Starting a new medication with known gut side effects (antibiotics, NSAIDs, PPIs)
I would be careful with any approach — including this one — that encourages pushing through worsening symptoms. That is not resilience. That is ignoring information your body is sending you.
Frequently Asked Questions
How long does it actually take to heal the gut?
For most people, meaningful improvements in digestion, energy, and bloating appear within 2–4 weeks of consistent dietary changes. Deeper repair — including microbial diversity and gut lining integrity — takes 60–90 days of sustained effort [2]. The 4-week reset is a foundation, not a finish line. For a deep dive into this, see our full guide on identify your bloating type and match the right fix.
Do I need supplements to heal my gut?
No. Food-based interventions — fermented foods, prebiotic fiber, diverse plant intake, and anti-inflammatory foods — are the primary tools. Supplements may be useful in specific cases (post-antibiotic recovery, confirmed deficiencies), but they are not required and should not replace dietary change.
Is “leaky gut” real?
Increased intestinal permeability is a real, measurable phenomenon documented in peer-reviewed research. “Leaky gut syndrome” as a standalone clinical diagnosis is not formally recognised by most mainstream medical bodies. The evidence connecting it to the broad range of symptoms claimed in wellness circles is still developing. Be sceptical of any source presenting it as a settled diagnosis with a definitive cure.
Can I drink coffee during the reset?
One coffee per day is a reasonable limit, particularly during Weeks 1 and 2. Coffee is mildly acidic and can irritate an inflamed gut lining in some people. Green tea is a useful alternative — it provides caffeine at lower levels and contains polyphenols that support beneficial bacteria.
What if I have IBS?
IBS is a clinical diagnosis that often requires a more tailored approach, potentially including a low-FODMAP protocol. Some elements of this reset — particularly the prebiotic fiber additions in Week 3 — may worsen IBS symptoms initially. Work with a registered dietitian if you have a confirmed IBS diagnosis.
Do I need to eliminate gluten and dairy?
Only if you have reason to suspect they are personal triggers. Blanket elimination without evidence is unnecessary and can create nutritional gaps. If you do eliminate them, reintroduce them methodically in Week 4 to assess your individual response.
What about intermittent fasting during the reset?
A gentle 12–14 hour overnight fast (finishing dinner by 7pm, eating breakfast at 8am) is compatible with this reset and may support the gut’s overnight repair process [1]. More aggressive fasting protocols are not necessary and can add unnecessary stress during the adjustment period.
Can symptoms get worse before they get better?
Yes, and this is normal in the first week. Cutting sugar and caffeine causes temporary withdrawal symptoms. Adding fermented foods can cause temporary gas. Both typically resolve within 5–7 days. If symptoms worsen and stay worse beyond 10 days, see a doctor.
Conclusion
If there is a three-word version of how to heal your gut, it is this: food, sleep, stress. Get those three consistently right over four weeks, and most people feel meaningfully better. Not perfect — better.
The 4-week reset gives you a structured way to do that. Remove the main irritants, soothe the system, rebuild microbial diversity with fermented foods and prebiotic fiber, and then lock in a sustainable routine built around diverse plant foods and consistent habits.
What matters most is this: healing is not a 28-day event. It is a rhythm you return to. The reset is how you establish that rhythm. After four weeks, the goal is not to go back to how things were — it is to have built a baseline that feels better than where you started.
Start with what gives the biggest return: cut alcohol and added sugar, add one fermented food daily, sleep 7–8 hours, and take a 20-minute walk most days. Everything else builds from there.
For the complete evidence-based overview of how your gut works, see our Gut Health and Digestive Wellness guide.
References
[1] Gut Reboot 2026 A Science Based Approach To Start The Year Right – https://newvitality.ie/gut-reboot-2026-a-science-based-approach-to-start-the-year-right/
[2] 30 Day Gut Reset Challenge – https://nutriscan.app/blog/posts/30-day-gut-reset-challenge-7f22bb3615
[3] Gut Health Resolutions – https://bellalindemann.com/blog/gut-health-resolutions

