Foods that are anti-inflammatory
Foods That Are Anti-Inflammatory: A Complete Evidence-Based Guide

- What Is Inflammation, and Why Does Diet Matter?
- Which Foods Are the Most Effective Anti-Inflammatories?
- What Foods Cause Inflammation and Should Be Reduced?
- How Does an Anti-Inflammatory Diet Differ from a Standard Western Diet?
- Can an Anti-Inflammatory Diet Support Weight Management?
- What Lifestyle Factors Amplify or Undercut an Anti-Inflammatory Diet?
- How Quickly Can Diet Change Inflammatory Markers?
- Foods that are anti-inflammatory – Links
Last updated: April 4, 2026
Quick Answer: The best foods that are anti-inflammatory include fatty fish, berries, leafy greens, extra virgin olive oil, turmeric, avocados, green tea, and dark chocolate. These foods work by supplying antioxidants, omega-3 fatty acids, and polyphenols that interrupt the body’s inflammatory signaling pathways. Eating them consistently — as part of a diet similar to the Mediterranean pattern — is one of the most effective non-pharmaceutical strategies for reducing chronic inflammation.
Key Takeaways
- Chronic inflammation is a root driver of heart disease, type 2 diabetes, arthritis, and certain cancers — and diet directly influences it
- Omega-3 fatty acids (found in salmon, sardines, mackerel) are among the most studied and effective dietary anti-inflammatories
- Curcumin in turmeric and EGCG in green tea both inhibit inflammatory enzyme activity at the cellular level
- Berries, grapes, and cherries contain polyphenols that reduce the production of inflammatory cytokines
- Extra virgin olive oil contains oleocanthal, a compound with mechanisms similar to ibuprofen
- Foods that cause inflammation — refined sugar, processed grains, trans fats, and excess red meat — should be reduced alongside increasing anti-inflammatory foods
- No single food reverses inflammation; the overall dietary pattern matters most
- Lifestyle factors like sleep, stress, and exercise amplify or undercut the effects of an anti-inflammatory diet
What Is Inflammation, and Why Does Diet Matter?
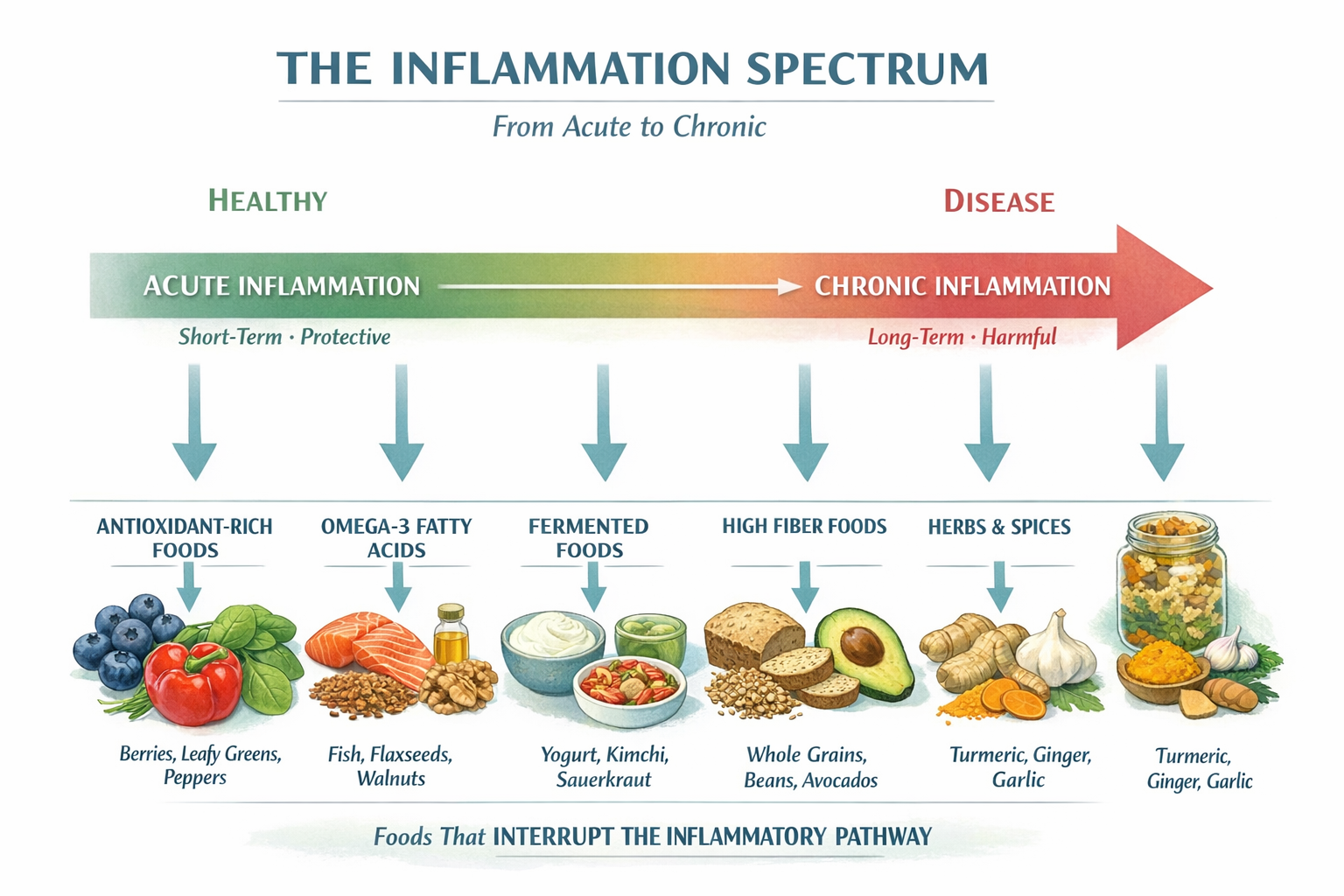
Inflammation is the immune system’s first-line defense against injury, infection, and foreign invaders. When you cut your finger or catch a cold, the body releases chemical signals that increase blood flow, recruit immune cells, and trigger tissue repair. That short-term, acute response is healthy and necessary.
The problem is chronic inflammation — when those same immune signals stay switched on for months or years without a genuine threat. According to the National Institutes of Health, chronic low-grade inflammation is a contributing factor in at least seven of the ten leading causes of death in the United States, including cardiovascular disease, type 2 diabetes, Alzheimer’s disease, and several cancers.
Diet is one of the most direct levers available for managing this. Every meal either adds to or reduces the body’s inflammatory load. Processed foods, refined carbohydrates, and industrial seed oils tend to promote the production of pro-inflammatory compounds like interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-α). Anti-inflammatory foods do the opposite — they supply compounds that suppress these pathways, protect cells from oxidative damage, and support gut health, which is closely tied to systemic inflammation.
For a broader look at how dietary patterns affect the body, the anti-inflammatory foods ultimate guide covers the full picture in detail.
Which Foods Are the Most Effective Anti-Inflammatories?
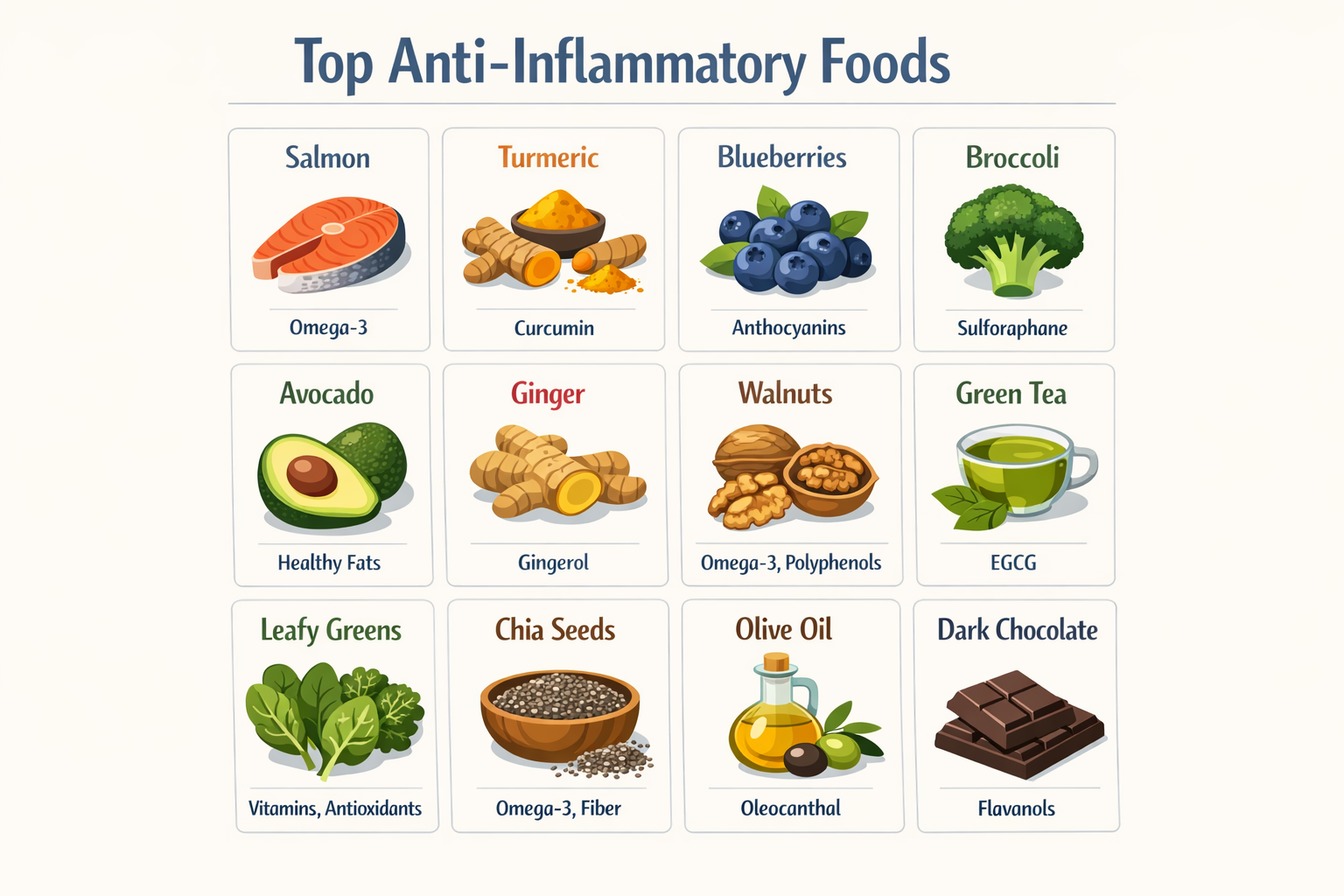
The most effective foods that are anti-inflammatory share a common trait: they are dense in bioactive compounds — polyphenols, omega-3 fatty acids, antioxidants, and specific phytochemicals — that directly interfere with the body’s inflammatory signaling.
Here is a breakdown of the most evidence-supported options:
Fatty Fish (Salmon, Sardines, Mackerel, Tuna)
Fatty fish are the single richest dietary source of long-chain omega-3 fatty acids, specifically EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid). These fatty acids are precursors to compounds called resolvins and protectins, which actively resolve inflammation rather than simply suppressing it.
Research published in journals including Arthritis & Rheumatology has found that regular fatty fish consumption is associated with reduced markers of inflammation, including C-reactive protein (CRP) and IL-6. People with rheumatoid arthritis, Crohn’s disease, and asthma have shown measurable symptom improvement with increased omega-3 intake.
Practical guidance:
- Aim for at least two servings of fatty fish per week, as recommended by the American Heart Association
- Wild-caught salmon and sardines tend to have higher omega-3 concentrations than farmed varieties
- If fish isn’t accessible, algae-based omega-3 supplements provide EPA and DHA from the original plant source
Berries (Blueberries, Strawberries, Raspberries, Blackberries)
Berries are among the most antioxidant-dense foods available. Their color comes from anthocyanins — a class of polyphenols that have been shown in multiple studies to reduce inflammatory cytokine production and protect against oxidative stress.
A study published in the Journal of Nutrition found that participants who consumed blueberries daily showed reduced levels of NF-κB, a key protein complex that controls the transcription of inflammatory genes. Berries also support gut microbiome diversity, which has downstream effects on systemic inflammation.
Choose berries if: You want a low-calorie, high-impact anti-inflammatory food that also supports brain health and blood sugar regulation.
Turmeric and Curcumin
Turmeric has been used in Ayurvedic and Traditional Chinese Medicine for over 2,000 years. Its active compound, curcumin, is one of the most studied natural anti-inflammatory agents in the scientific literature.
Curcumin works by inhibiting NF-κB and COX-2 enzymes — two of the primary drivers of the inflammatory cascade. It also upregulates antioxidant enzymes including superoxide dismutase and catalase. Research from institutions including the University of California, Los Angeles has found curcumin comparable to some pharmaceutical anti-inflammatories in certain markers, though bioavailability is a limiting factor.
Common mistake: Eating turmeric alone provides limited benefit because curcumin is poorly absorbed. Combining it with black pepper (which contains piperine) increases curcumin absorption by up to 2,000%, according to research published in Planta Medica (1998). Cooking turmeric in fat also improves uptake.
Extra Virgin Olive Oil
Extra virgin olive oil (EVOO) deserves its own category. Beyond its well-documented monounsaturated fat content, EVOO contains a phenolic compound called oleocanthal. Research from the Monell Chemical Senses Center identified oleocanthal as a natural COX inhibitor — the same mechanism used by ibuprofen. The researchers noted that the throat-irritating sensation from high-quality EVOO is actually the oleocanthal activating the same receptors as anti-inflammatory drugs.
EVOO is also rich in oleuropein and hydroxytyrosol, two polyphenols associated with reduced CRP levels and improved endothelial function.
Edge case: Heat degrades polyphenol content. For maximum anti-inflammatory benefit, use EVOO as a finishing oil or in cold dressings. For high-heat cooking, refined olive oil or avocado oil is more stable. You can read more about the health benefits of olive oil and how to use it effectively.
Avocados
Avocados provide a combination of anti-inflammatory nutrients that is difficult to find in a single food: monounsaturated fats, vitamin E, vitamin C, carotenoids (lutein and zeaxanthin), and phytosterols. The carotenoids in avocados are fat-soluble, meaning the healthy fat in the fruit itself enhances their absorption.
A 2019 study published in the Journal of Nutrition found that eating one avocado per day for 12 weeks reduced several inflammatory markers in overweight adults, including IL-1β. Avocados also support gut health by acting as a prebiotic, feeding beneficial bacteria that produce short-chain fatty acids — compounds that reduce intestinal inflammation.
For a detailed breakdown of what avocados do for the body, see this guide on avocado health benefits.
Green Tea
Green tea contains epigallocatechin gallate (EGCG), a catechin polyphenol that is one of the most potent plant-based anti-inflammatory compounds identified to date. EGCG inhibits the production of pro-inflammatory cytokines and has shown protective effects against inflammation-driven neurodegeneration in animal models.
Green tea also supports gut microbiome health and has been associated in population studies with reduced rates of cardiovascular disease and type 2 diabetes — both conditions with chronic inflammation as a central mechanism.
Practical note: Matcha (powdered whole green tea leaf) contains significantly more EGCG than brewed green tea. Three to four cups of brewed green tea daily is the amount most commonly associated with measurable health benefits in research.
Broccoli and Cruciferous Vegetables
Broccoli, Brussels sprouts, kale, and cauliflower contain sulforaphane, a sulfur compound produced when the vegetable is chopped or chewed. Sulforaphane activates Nrf2, a transcription factor that switches on the body’s endogenous antioxidant and anti-inflammatory defenses.
Research from Johns Hopkins University, where sulforaphane was first identified, has shown it reduces oxidative stress markers and supports detoxification pathways in the liver. Broccoli is also a significant source of vitamins C and K, both of which play roles in immune regulation.
Decision rule: Lightly steam or eat cruciferous vegetables raw for maximum sulforaphane content. Boiling significantly reduces the enzyme (myrosinase) needed to convert glucosinolates into sulforaphane.
Mushrooms
Edible mushrooms — particularly shiitake, maitake, reishi, and lion’s mane — contain beta-glucans, polysaccharides that modulate immune function and reduce inflammatory cytokine production. They are also one of the few non-animal dietary sources of ergothioneine, an antioxidant amino acid that accumulates in tissues under oxidative stress.
Research published in the Journal of Nutritional Biochemistry found that shiitake mushroom consumption over four weeks significantly reduced CRP levels and improved gut immune function in healthy adults.
Dark Chocolate and Cocoa
Dark chocolate (70% cacao or higher) and raw cocoa contain flavanols — particularly epicatechin and catechin — that reduce inflammation by inhibiting platelet aggregation, lowering blood pressure, and suppressing the expression of inflammatory genes.
A meta-analysis published in Nutrients (2022) found that cocoa flavanol supplementation was associated with significant reductions in CRP and TNF-α. The key is cacao percentage: milk chocolate contains too much sugar and too little flavanol to provide meaningful benefit. For a full breakdown of what the research says, see this article on the benefits of dark chocolate for health.
Practical limit: One to two squares (about 20–30g) of high-quality dark chocolate daily is enough to get the benefit without excess calories or sugar.
Grapes and Cherries
Both grapes and cherries are high in polyphenols with specific anti-inflammatory properties. Grapes contain resveratrol (concentrated in the skin) and quercetin, both of which inhibit inflammatory enzyme activity. Tart cherries are particularly notable: they contain anthocyanins and melatonin, and research from Oregon Health & Science University found that tart cherry juice reduced muscle inflammation and soreness after exercise more effectively than placebo.
Cherries have also been studied in the context of gout, where their anthocyanin content appears to reduce uric acid levels and the frequency of flare-ups.
Peppers
Bell peppers and chili peppers both contribute to an anti-inflammatory diet, though through different mechanisms. Bell peppers are exceptionally high in vitamin C — a medium red bell pepper provides more vitamin C than an orange — which supports immune regulation and reduces oxidative stress.
Chili peppers contain capsaicin, which initially activates pain receptors but then desensitizes them over time, reducing the transmission of pain signals. Capsaicin also inhibits substance P, a neuropeptide involved in inflammatory signaling. Topical capsaicin is already used clinically for arthritis pain; dietary capsaicin offers milder systemic effects.
Nuts (Walnuts, Almonds, Pistachios)
Nuts provide a combination of anti-inflammatory nutrients: vitamin E (a fat-soluble antioxidant), magnesium (which plays a role in regulating inflammatory responses), plant-based omega-3s (ALA, especially in walnuts), and polyphenols in the skin.
A large analysis of dietary data from the PREDIMED trial — one of the most comprehensive Mediterranean diet studies conducted — found that regular nut consumption was associated with significantly lower levels of inflammatory markers including CRP, IL-6, and TNF-α.
Choose walnuts if you want the highest omega-3 content among nuts. Choose almonds if vitamin E is the priority. All unsalted, unroasted nuts provide benefit; heavily processed or salted varieties reduce the net nutritional value.
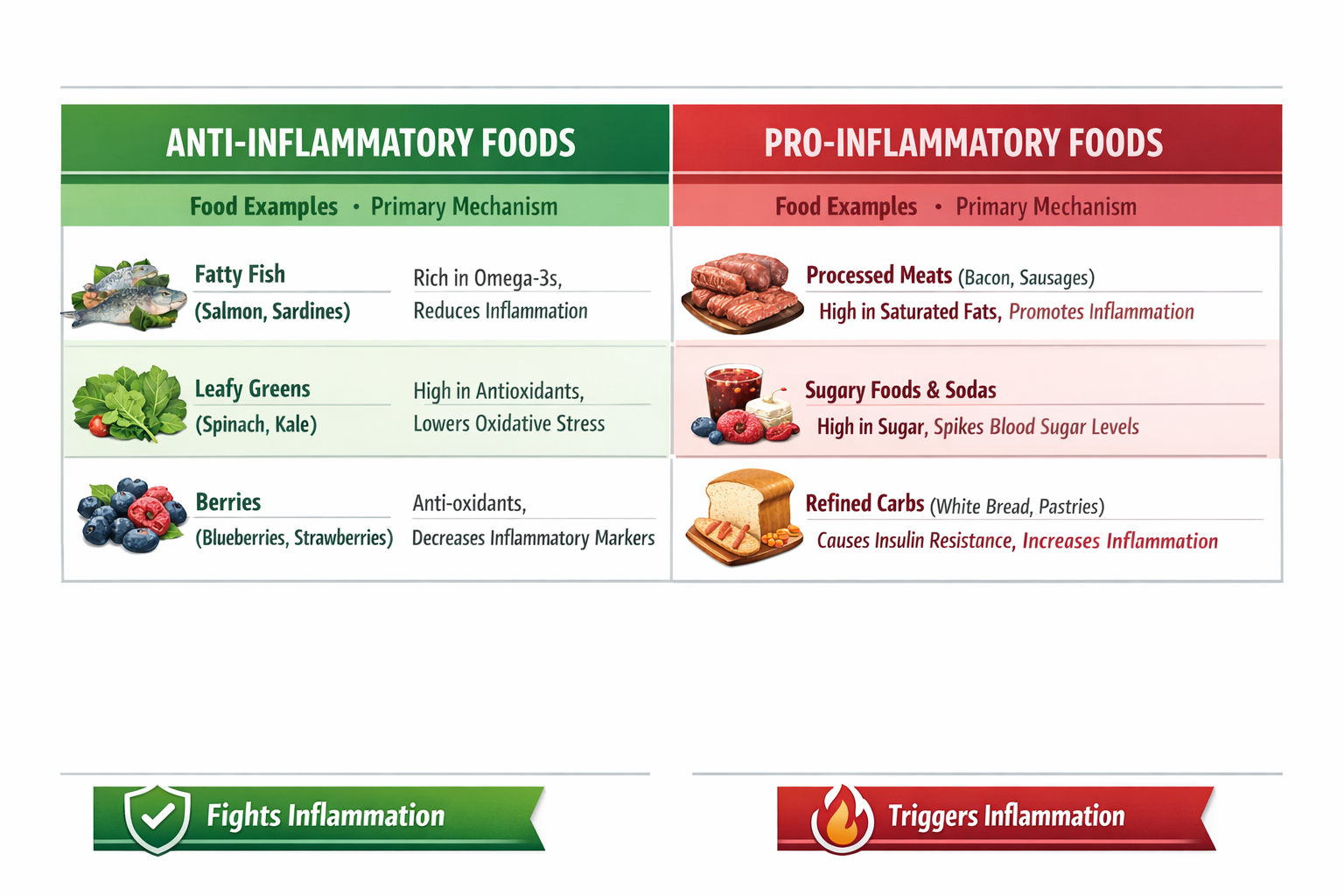
What Foods Cause Inflammation and Should Be Reduced?
Reducing pro-inflammatory foods is just as important as adding anti-inflammatory ones. The following food categories consistently show up in research as drivers of chronic inflammation:
| Food Category | Primary Mechanism | Common Sources |
|---|---|---|
| Refined sugars | Spike blood glucose, feed harmful gut bacteria, increase AGEs | Soda, candy, pastries, sweetened cereals |
| Refined carbohydrates | Rapid glucose spikes, low fiber, disrupt gut microbiome | White bread, white rice, crackers, chips |
| Trans fats (partially hydrogenated oils) | Directly increase LDL and inflammatory markers | Some margarines, packaged snack foods |
| Excess omega-6 vegetable oils | Shift omega-6:omega-3 ratio toward inflammation | Corn oil, soybean oil, sunflower oil in excess |
| Processed meats | High in saturated fat, nitrates, and advanced glycation end products | Hot dogs, deli meats, bacon |
| Alcohol (excess) | Disrupts gut barrier, increases endotoxin exposure | Beer, spirits, wine in excess |
The goal is not perfect elimination but a meaningful shift in ratio — more anti-inflammatory foods, fewer pro-inflammatory ones, consistently over time.
How Does an Anti-Inflammatory Diet Differ from a Standard Western Diet?
The standard Western diet is high in refined carbohydrates, processed foods, industrial seed oils, and red meat, and low in fiber, omega-3 fatty acids, and polyphenols. This pattern consistently produces higher circulating levels of inflammatory markers in population studies.
An anti-inflammatory diet — most closely approximated by the Mediterranean diet — flips this ratio. It emphasizes:
- Vegetables and fruits as the dietary foundation
- Whole grains over refined grains
- Legumes as a primary protein source
- Fatty fish two or more times per week
- Extra virgin olive oil as the primary fat
- Nuts and seeds as snacks
- Minimal processed foods, added sugars, and red meat
The Mediterranean diet is the most studied dietary pattern for inflammation reduction and has the strongest evidence base for cardiovascular protection, cognitive health, and longevity.
Can an Anti-Inflammatory Diet Support Weight Management?
Yes, and the relationship between inflammation and body weight runs in both directions. Excess adipose tissue — particularly visceral fat around the organs — is itself an active source of inflammatory cytokines. Losing even 5–10% of body weight in people with obesity has been shown to meaningfully reduce CRP and IL-6 levels.
Anti-inflammatory foods also tend to be high in fiber and protein, which promote satiety and help regulate blood sugar. This makes them naturally supportive of healthy weight loss without the need for extreme restriction.
Common mistake: Treating anti-inflammatory eating as a short-term diet rather than a long-term pattern. The research benefits accumulate over months and years, not days.
What Lifestyle Factors Amplify or Undercut an Anti-Inflammatory Diet?
Food is one piece of the inflammation puzzle. These lifestyle factors interact directly with dietary choices:
Factors that worsen inflammation:
- Chronic sleep deprivation (less than 6 hours per night is associated with elevated CRP)
- Psychological stress (activates the HPA axis and increases cortisol, which eventually promotes inflammatory signaling)
- Sedentary behavior (physical inactivity is independently associated with higher inflammatory markers)
- Smoking (introduces oxidative stress and directly activates inflammatory pathways)
- Gut dysbiosis (an imbalanced microbiome increases intestinal permeability, allowing bacterial endotoxins into circulation)
Factors that support anti-inflammatory effects:
- Regular moderate exercise (30–45 minutes most days reduces systemic inflammation over time)
- Adequate sleep (7–9 hours for most adults)
- Stress management practices (meditation, breathwork, and social connection all show measurable effects on inflammatory markers)
- Supporting gut health through fiber-rich foods and fermented foods
How Quickly Can Diet Change Inflammatory Markers?
This depends on the individual’s baseline inflammation level, the degree of dietary change, and other lifestyle factors. In clinical studies:
- CRP levels have shown measurable reductions within 4–8 weeks of adopting a Mediterranean-style diet
- Omega-3 supplementation studies show changes in inflammatory markers within 6–12 weeks at therapeutic doses
- Gut microbiome composition begins shifting within 72 hours of significant dietary change, though meaningful diversity improvements take longer
The takeaway: you’re unlikely to feel dramatically different in a week, but consistent dietary change over 6–12 weeks produces measurable, clinically meaningful reductions in inflammatory markers for most people.
Frequently Asked Questions
What are the top three foods that are anti-inflammatory?
Fatty fish (for omega-3s), extra virgin olive oil (for oleocanthal and polyphenols), and berries (for anthocyanins) consistently rank highest in the research for reducing chronic inflammation. Turmeric with black pepper is a close fourth.
Can I reduce inflammation with food alone, without medication?
For mild to moderate chronic inflammation driven by diet and lifestyle, dietary changes can produce significant improvements without medication. For conditions like rheumatoid arthritis or inflammatory bowel disease, diet works best as a complement to medical treatment, not a replacement. Always consult your doctor before changing your approach to managing a diagnosed condition.
How much turmeric do I need to eat to reduce inflammation?
Most research on curcumin uses supplemental doses of 500–2,000mg of curcumin per day — far more than typical cooking amounts. Cooking with turmeric daily provides some benefit, but for therapeutic effects, a standardized curcumin supplement with piperine is more reliable.
Is dairy inflammatory or anti-inflammatory?
The evidence is mixed. Fermented dairy (yogurt, kefir) appears neutral to mildly anti-inflammatory due to its probiotic content. Full-fat dairy in people who tolerate it well does not consistently raise inflammatory markers. However, some individuals with lactose intolerance or dairy sensitivity do experience increased inflammation. Individual response varies.
Are eggs anti-inflammatory?
Eggs are not strongly pro-inflammatory for most people. They contain choline and lutein, which have some anti-inflammatory properties. The concern about egg yolks and cholesterol has been substantially revised in recent years. For most healthy adults, one to two eggs daily fits within an anti-inflammatory dietary pattern.
Is coffee anti-inflammatory?
Yes, moderate coffee consumption is associated with lower levels of inflammatory markers in multiple population studies. Coffee contains chlorogenic acids and other polyphenols with antioxidant properties. The health benefits of coffee extend beyond caffeine to its phytochemical content.
What is the fastest way to reduce inflammation in the body?
No single food or supplement eliminates inflammation overnight. The fastest measurable improvements come from simultaneously removing major pro-inflammatory foods (sugar, refined carbs, processed oils) and adding omega-3-rich foods, while also improving sleep and reducing stress. Some people notice reduced joint stiffness or improved energy within 2–3 weeks of consistent changes.
Can children benefit from anti-inflammatory foods?
Yes. The same foods that reduce inflammation in adults support healthy immune development in children. Berries, vegetables, fatty fish, nuts (where age-appropriate), and whole grains are all beneficial for children. Reducing ultra-processed food consumption is particularly important during childhood, as early dietary patterns influence long-term inflammatory baseline.
Does alcohol cause inflammation?
Excess alcohol consumption does promote inflammation by increasing intestinal permeability and liver stress. Moderate red wine consumption (one glass per day for women, up to two for men) has been associated with neutral to slightly anti-inflammatory effects in some studies, attributed to resveratrol — but the benefit is modest and does not justify drinking if you don’t already.
Are supplements a good substitute for anti-inflammatory foods?
Supplements can be useful when specific nutrients are difficult to obtain from food alone (omega-3s for people who don’t eat fish, curcumin at therapeutic doses). But they don’t replicate the synergistic effect of whole foods, which provide multiple compounds working together. Food-first is the right approach; supplements fill specific gaps.
Sources
- National Institutes of Health, National Institute of Environmental Health Sciences — Inflammation overview
- Calder PC. “Omega-3 fatty acids and inflammatory processes.” Nutrients, 2010
- Aggarwal BB, Harikumar KB. “Potential therapeutic effects of curcumin.” International Journal of Biochemistry & Cell Biology, 2009
- Beauchamp GK et al. “Ibuprofen-like activity in extra-virgin olive oil.” Nature, 2005
- Guasch-Ferré M et al. “Frequency of nut consumption and mortality risk.” BMC Medicine, 2013 (PREDIMED data)
- Shukitt-Hale B et al. “Blueberries and neurological aging.” Journal of Nutrition, 2010
- Ferretti G et al. “Cherry antioxidant activity.” Food Chemistry, 2010
- Bhupathiraju SN, Tucker KL. “Greater variety in fruit and vegetable intake is associated with lower inflammation.” Journal of Nutrition, 2011
Foods that are anti-inflammatory – Links
Health Benefits of Olive Oil
Anti-inflammatory-diet-foods-to-avoid
Dave James has spent 30+ years reading health and longevity research, and has run All Perfect Health for the past five. His background is in Australian mining and industrial engineering — disciplines built on questioning claims, measuring outcomes, and respecting evidence. He writes about what the research actually says, including where the experts disagree.
More about Dave & this site →
References & Research Sources
This article draws on peer-reviewed research, clinical guidelines, and authoritative health organizations. The following sources were consulted during preparation. This is not an exhaustive bibliography, and readers are encouraged to consult primary literature for full study details.
- Calder PC. Omega-3 fatty acids and inflammatory processes: from molecules to man. Biochem Soc Trans. 2017;45(5):1105-1115. https://pubmed.ncbi.nlm.nih.gov/28916517/
- Schwingshackl L, Hoffmann G. Mediterranean dietary pattern, inflammation and endothelial function: a systematic review and meta-analysis of intervention trials. Nutr Metab Cardiovasc Dis. 2014;24(9):929-939. https://pubmed.ncbi.nlm.nih.gov/24931693/
- Estruch R, et al. Primary Prevention of Cardiovascular Disease with a Mediterranean Diet Supplemented with Extra-Virgin Olive Oil or Nuts. N Engl J Med. 2018;378(25):e34. https://pubmed.ncbi.nlm.nih.gov/29211688/
- Joseph SV, Edirisinghe I, Burton-Freeman BM. Berries: anti-inflammatory effects in humans. J Agric Food Chem. 2014;62(18):3886-3903. https://pubmed.ncbi.nlm.nih.gov/24582583/
- Ferguson JFA, et al. Dairy and Cardiometabolic Health: A Review of the Evidence. Nutrients. 2021;13(10):3450. https://pubmed.ncbi.nlm.nih.gov/34684348/
- Holt EM, et al. Fruit and vegetable consumption and its relation to markers of inflammation and oxidative stress in adolescents. J Am Diet Assoc. 2009;109(3):414-421. https://pubmed.ncbi.nlm.nih.gov/19248865/
- Liu S, et al. A prospective study of dietary glycemic load, carbohydrate intake, and risk of coronary heart disease in US women. Am J Clin Nutr. 2000;71(6):1455-1461. https://pubmed.ncbi.nlm.nih.gov/10837285/
- Nieman DC, et al. Chronic consumption of flavanols and related procyanidins does not affect C-reactive protein, body weight, or blood pressure in overweight and moderately obese adults. J Nutr. 2015;145(12):2649-2655. https://pubmed.ncbi.nlm.nih.gov/26581686/
- Kiecolt-Glaser JK. Stress, food, and inflammation: psychoneuroimmunology and nutrition at the cutting edge. Psychosom Med. 2010;72(4):365-369. https://pubmed.ncbi.nlm.nih.gov/20410323/
- Harvard T.H. Chan School of Public Health. The Nutrition Source: Inflammation. https://www.hsph.harvard.edu/nutritionsource/anti-inflammatory-diet/

