Fiber Decoded: Soluble vs. Insoluble, Daily Targets, and Why Most People Get It Wrong

- What Fiber Actually Is (And Why Your Body Can't Digest It)
- Soluble vs. Insoluble — The Critical Difference
- The Daily Target — By Age and Sex
- The Fiber Paradox (Why More Can Make Things Worse)
- The 5g-Per-Week Ramp-Up Plan
- Best Foods for Each Type
- Fiber and Your Gut Microbiome
- Fiber and Specific Goals
- Fiber Supplements — Worth It or Marketing?
- Common Fiber Mistakes
Last updated: April 23, 2026
Quick Answer
Soluble fiber dissolves in water and forms a gel that slows digestion, feeds gut bacteria, and helps manage blood sugar and cholesterol. Insoluble fiber does not dissolve — it adds bulk, speeds up transit time, and keeps you regular. Most adults need 25–38 grams of fiber per day depending on age and sex, but only about 7% of Americans actually hit that target [8]. The most common mistake isn’t eating too little fiber — it’s adding too much, too fast, without enough water.
Key Takeaways
- Soluble vs. insoluble fiber serve different functions — you need both, in roughly a 1:3 ratio (one part soluble to two parts insoluble) [1]
- Daily targets range from 22g to 38g depending on your age and sex [5]
- A useful rule of thumb: 14g of fiber per 1,000 calories consumed [1]
- Ramping up by no more than 5g per week prevents the what causes bloating and how to match the fix to your type and gas that makes most people quit
- Add 30ml of water for every extra gram of fiber you introduce — hydration is non-negotiable
- Short-chain fatty acids (SCFAs) are the reason fiber matters so much for 4-week gut healing reset that pairs perfectly with a fiber ramp-up — and most people have never heard of them
- Fiber above 50–60g per day can actually cause constipation and reduce mineral absorption [4]
- IBS-C and IBS-D respond differently to fiber types — one size does not fit all
- Whole food sources beat supplements in most situations, but supplements have a legitimate role
- The “fiber paradox” is real: eating more fiber can make symptoms worse before it makes them better
What Fiber Actually Is (And Why Your Body Can’t Digest It)
Fiber is a type of carbohydrate found in plant foods that your digestive enzymes cannot break down. Unlike sugars and starches, it passes through your small intestine largely intact and arrives in your large intestine still in one piece — or close to it [6].
That might sound like a design flaw. It isn’t. The fact that fiber resists digestion is exactly what makes it useful. It adds bulk to stool, slows the absorption of glucose, feeds the bacteria that live in your colon, and helps keep your bowel movements predictable.
The Dietary Guidelines Advisory Committee classifies fiber as a shortfall nutrient — meaning most people don’t get nearly enough of it [7]. In 2026, estimates suggest only 7% of American adults meet their daily fiber targets [8]. That’s not a rounding error. That’s a genuine public health gap.
There are two main categories: soluble fiber and insoluble fiber. They behave differently, do different jobs, and come from different foods. Understanding the distinction between soluble vs. insoluble fiber is where most people’s fiber knowledge stops being vague and starts being useful.
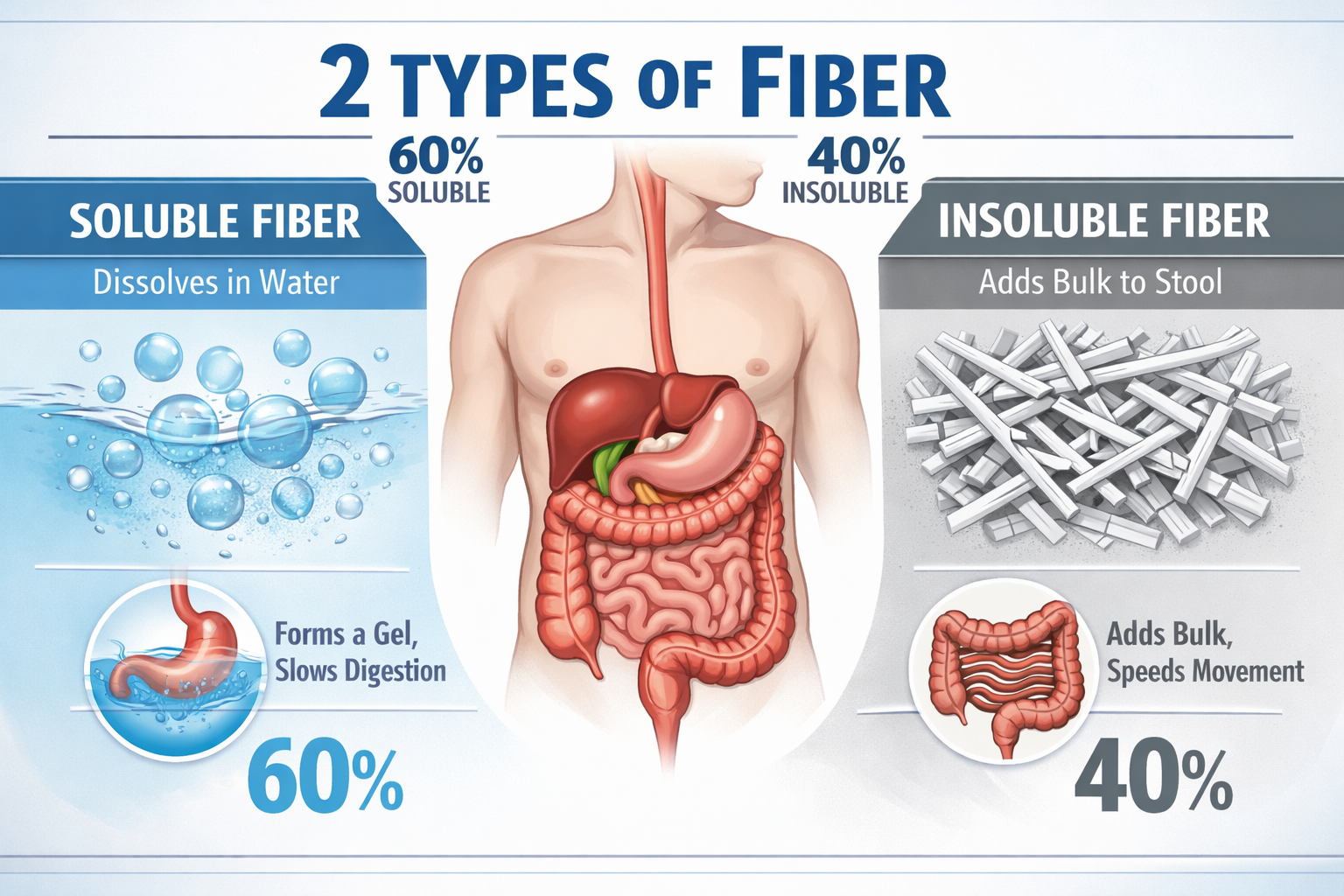
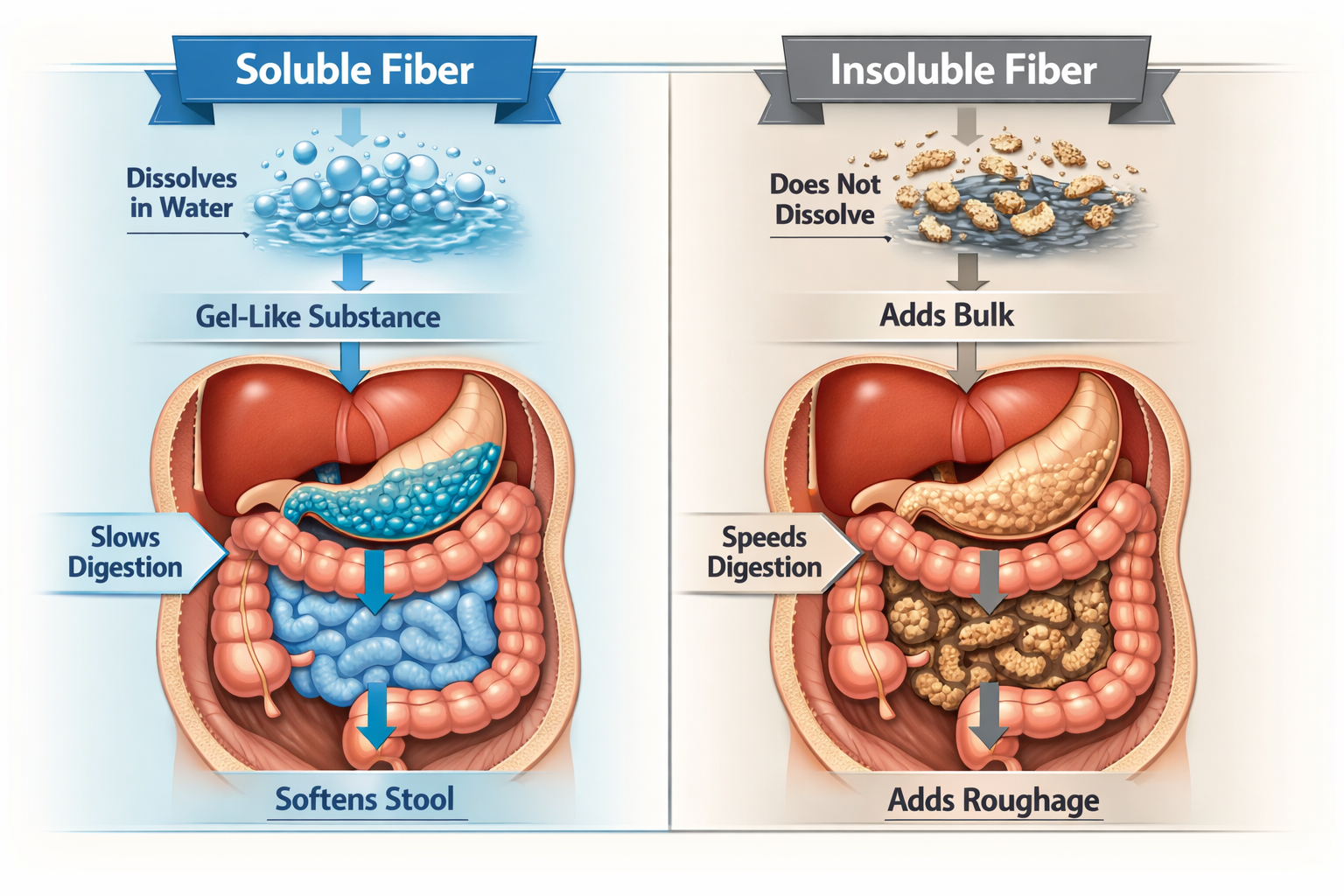
Soluble vs. Insoluble — The Critical Difference
The simplest way to look at it is this: soluble fiber dissolves in water; insoluble fiber does not. But what happens after that is where the real story begins.
Soluble Fiber: The Gel Former
When soluble fiber meets water in your gut, it forms a thick, gel-like substance [1]. That gel does several things at once:
- Slows digestion, which means glucose enters your bloodstream more gradually — useful for blood sugar management
- Attracts water into your gut, which keeps stool soft and easier to pass
- Acts as a how probiotics and prebiotics work together, feeding the beneficial bacteria in your colon [1]
- Binds to bile acids in your small intestine, which prompts your liver to pull cholesterol from your blood to make more bile — effectively lowering LDL cholesterol [7]
Soluble fiber is found in oats, barley, rye, apples, bananas, avocados, citrus fruits, full list of high-fiber foods with grams per serving, peas, lentils, carrots, potatoes, and psyllium [1][3][7].
A practical example: the beta-glucan in oats is one of the most studied soluble fibers. It’s the reason oatmeal has a legitimate claim to supporting heart health — not marketing, actual mechanism [6].
Insoluble Fiber: The Bulk Builder
Insoluble fiber doesn’t dissolve. It passes through your digestive tract largely unchanged, absorbing water along the way and adding physical bulk to your stool [1][3].
The result is faster gut transit — food moves through more quickly, which reduces the time waste material sits in your colon. That’s why insoluble fiber is the primary tool for preventing and relieving constipation [3].
It also contributes zero calories to your diet, because your body can’t extract energy from it [1].
Good sources of insoluble fiber include whole-wheat flour, wheat bran, brown rice, quinoa, nuts, broccoli, cauliflower, green beans, celery, popcorn, berries, edible fruit and vegetable skins, and ground flaxseed [3][4].
The 1:3 Ratio — What It Means in Practice
To maintain a healthy gut balance, the evidence suggests aiming for roughly twice as much insoluble fiber as soluble fiber [1]. In practical terms, that’s a 1:2 soluble-to-insoluble ratio — sometimes rounded to “1:3” in general guidance.
If your daily target is 30g total, aim for approximately:
- 10g soluble fiber
- 20g insoluble fiber
Most whole plant foods contain a mix of both types, so you don’t need to track them separately with obsessive precision. Eating a variety of vegetables, legumes, whole grains, and fruit will naturally land you in the right range.
The Daily Target — By Age and Sex
Here’s the real issue with most fiber advice: the generic “eat more fiber” instruction tells you nothing useful. The actual targets vary by age and sex, and they’re more specific than most people realize [5].
| Group | Age 19–30 | Age 31–50 | Age 51+ |
|---|---|---|---|
| Women | 28g/day | 25g/day | 22g/day |
| Men | 34g/day | 31g/day | 28g/day |
Source: Cleveland Clinic [5]
Targets decrease slightly with age, partly because calorie needs tend to drop. The alternative guideline — 14g of fiber per 1,000 calories consumed — is a useful cross-check [1]. If you eat around 2,000 calories a day, that puts your target at 28g, which aligns well with the table above for most adults.
A note on context: These are population-level recommendations. If you have a digestive condition like IBS, Crohn’s disease, or diverticulitis, your individual target may be different. A registered dietitian is the right person to help you calibrate.
The Fiber Paradox (Why More Can Make Things Worse)
Here’s something worth saying plainly: eating more fiber can make your symptoms worse before it makes them better — and for some people, it makes them worse full stop.
This is the fiber paradox, and it’s why so many health-aware adults have a complicated relationship with fiber. They’ve been told to eat more. They tried. They ended up bloated, gassy, and uncomfortable. So they stopped.
The problem usually isn’t the fiber itself. It’s the speed of introduction and the lack of water.
When you add fiber faster than your gut bacteria can adapt, the bacteria ferment it rapidly, producing gas as a byproduct. That gas causes bloating, cramping, and flatulence. Consuming more than 50–60g of fiber per day can also cause constipation — the very thing most people are trying to fix — and reduce your absorption of minerals like calcium, zinc, iron, and magnesium [4].
The IBS complication is real. People with IBS-C (constipation-predominant) often benefit from gradually increasing soluble fiber, particularly psyllium, which softens stool without dramatically speeding transit. People with IBS-D (diarrhea-predominant) may find that soluble fiber helps slow things down, but insoluble fiber can make symptoms significantly worse. These are genuinely different situations that need different approaches. The evidence here is nuanced, and I’d be careful about applying blanket fiber advice to either group without professional input.
The main takeaway is this: more is not always better, and the rate of increase matters as much as the total amount.
The 5g-Per-Week Ramp-Up Plan
A sensible starting point is to increase your fiber intake by no more than 5g per week, giving your how your digestive system actually works time to adjust [4]. Most sources suggest adding 2–3g per day as a daily increment, but thinking in weekly blocks is easier to manage practically.
Equally important: for every extra gram of fiber you add, drink an additional 30ml of water. If you add 10g of fiber to your daily intake, that’s 300ml (about 1.25 cups) more water per day on top of your baseline.
General hydration targets are 9 cups (72 oz) per day for women and 11 cups (88 oz) per day for men [4]. Fiber without water is a recipe for the exact constipation you’re trying to avoid.
Here’s a practical week-by-week framework, assuming a starting intake of around 10–12g per day (which is close to the average American’s actual intake):
| Week | Target Daily Fiber | What to Add |
|---|---|---|
| Week 1 | 15g | Add one serving of oats or lentils at one meal |
| Week 2 | 20g | Add a piece of fruit with skin + a vegetable at lunch |
| Week 3 | 25g | Add a second legume serving or swap white rice for brown |
| Week 4 | 28–30g | Add a handful of nuts or seeds; introduce whole grain bread |
| Week 5+ | Maintain target | Distribute fiber across all meals; monitor tolerance |
Start with what gives the biggest return. Legumes (beans, lentils, chickpeas) are the single most fiber-dense food group you can add. One cup of cooked lentils delivers around 15g of fiber. That’s half a day’s target in one serving.

Best Foods for Each Type
Let’s keep this practical. Rather than a comprehensive list of every fiber-containing food, here are the highest-impact options for each type.
Top Soluble Fiber Sources
| Food | Serving | Approx. Soluble Fiber |
|---|---|---|
| Psyllium husk | 1 tbsp | 5–6g |
| Black beans | ½ cup cooked | 2–3g |
| Oats (rolled) | ½ cup dry | 2g |
| Avocado | ½ fruit | 2g |
| Apple (with skin) | 1 medium | 1g |
| Barley | ½ cup cooked | 1g |
Top Insoluble Fiber Sources
| Food | Serving | Approx. Insoluble Fiber |
|---|---|---|
| Wheat bran | 2 tbsp | 3–4g |
| Lentils | ½ cup cooked | 4g |
| Broccoli | 1 cup | 2g |
| Brown rice | ½ cup cooked | 1.5g |
| Ground flaxseed | 1 tbsp | 1.5g |
| Almonds | 1 oz (23 nuts) | 2g |
Most whole plant foods contain both types. Beans and lentils, for example, are genuinely good sources of both soluble and insoluble fiber — which is one reason they show up consistently in the research on fiber and health outcomes [6].
Fiber and Your Gut Microbiome
This is where the science gets genuinely interesting, and where I think the public conversation about fiber still undersells the real story.
When soluble fiber reaches your large intestine, your gut bacteria ferment it. The byproducts of that fermentation are short-chain fatty acids (SCFAs) — primarily acetate, propionate, and butyrate [6].
In plain English: SCFAs are the fuel your colon cells run on. Butyrate, in particular, is the preferred energy source for colonocytes (the cells lining your colon). It also plays a role in maintaining the integrity of the gut lining, regulating anti-inflammatory foods that lower chronic inflammation, and may influence immune function [6].
The evidence suggests that a diet consistently high in fermentable fiber supports a more diverse gut microbiome, and microbial diversity is generally associated with better metabolic and immune health [6]. That’s not a guarantee — the research is still developing — but the direction of the evidence is consistent enough to take seriously.
What this means practically: the fiber you eat isn’t just moving things along mechanically. It’s actively feeding a community of microorganisms that affect your health in ways we’re still mapping. That’s a stronger argument for getting your fiber from whole foods than from isolated supplements, because whole foods bring a broader range of fermentable substrates.
Fiber and Specific Goals
Weight Management
Soluble fiber slows gastric emptying — the rate at which your stomach empties into the small intestine. That translates to a longer feeling of fullness after meals [1][7]. From a practical standpoint, this can reduce overall calorie intake without requiring willpower, because you’re simply less hungry.
Insoluble fiber adds bulk with zero caloric contribution, which means you can eat a larger volume of food for the same calorie count. Both effects are real, and both are useful for weight management.
Blood Sugar Control
The gel formed by soluble fiber slows the absorption of glucose from your small intestine into your bloodstream [1][7]. This blunts post-meal blood sugar spikes — relevant for anyone managing type 2 diabetes, insulin resistance, or simply trying to avoid the energy crashes that follow high-glycaemic meals.
The evidence here is reasonably strong. The stronger evidence points to viscous soluble fibers — like psyllium and beta-glucan from oats — as the most effective for glycaemic control [6].
Cholesterol
Soluble fiber binds to bile acids in the small intestine. Your body uses cholesterol to make bile acids, so when they’re bound and excreted, your liver pulls LDL cholesterol from your blood to produce more [7]. The net effect is a modest but measurable reduction in LDL cholesterol.
This is not a dramatic effect — we’re not talking about replacing medication — but it’s a real, mechanistic benefit that holds up across multiple studies [6].
Gut Transit and Constipation
Insoluble fiber is the primary lever here [3]. It adds bulk to stool and speeds transit time. If constipation is your main concern, increasing insoluble fiber (with adequate water) is the most direct approach.
For people with slow-transit constipation, adding insoluble fiber without enough water can make things worse. The 30ml-per-gram rule applies here more than anywhere else.
Fiber Supplements — Worth It or Marketing?
The honest answer is: it depends on the conditions.
Fiber supplements — psyllium husk, inulin, methylcellulose, wheat dextrin — can be genuinely useful in specific situations. They’re not inherently inferior to food fiber, but they’re also not a replacement for a varied, plant-rich diet.
When supplements make sense:
- You have a medically confirmed need for a specific fiber type (e.g., psyllium for IBS-C)
- You’re traveling or in circumstances where whole food fiber is genuinely hard to access
- You’re using them as a short-term bridge while building better food habits
- Your clinician has recommended them for a specific therapeutic purpose
Where whole food wins:
- Whole foods deliver a mix of soluble and insoluble fiber, plus vitamins, minerals, phytonutrients, and fermentable substrates that isolated supplements don’t replicate [6]
- The SCFA production from whole food fiber fermentation is broader and more varied than from isolated supplements
- There’s no supplement equivalent of eating a bowl of lentils, a handful of berries, and a side of broccoli
This is where hype gets in the way. Some supplement marketing implies that a daily psyllium capsule covers your fiber needs. It doesn’t. It addresses one specific aspect of fiber intake, and it does so reasonably well — but it’s not a substitute for dietary diversity.
The FDA has a defined list of dietary fibers that must demonstrate a physiological benefit to be labeled as fiber on a nutrition facts panel [9]. That’s a useful baseline for evaluating supplement claims — if the fiber type isn’t on that list, the evidence for it is thinner.
There is no magic in it. Supplements are a tool, not a solution.
Common Fiber Mistakes
Based on the evidence and real-world patterns, here are the mistakes worth avoiding:
1. Adding too much, too fast
The most common reason people quit. Stick to the 5g-per-week ramp. Your gut bacteria need time to adapt [4].
2. Not drinking enough water
Fiber without water is a constipation risk. The 30ml-per-gram rule is a practical minimum. Most people adding fiber are also under-hydrated to begin with [4].
3. Relying on one source
Eating only wheat bran or only psyllium gives you a narrow fiber profile. Variety matters for microbiome diversity.
4. Ignoring the soluble vs. insoluble distinction
If you’re constipated, you need more insoluble fiber and water — not just more fiber in general. If you have IBS-D, more insoluble fiber may make things worse. The distinction between soluble vs. insoluble fiber matters clinically.
5. Expecting immediate results
Gut microbiome changes take weeks, not days. Give any dietary change at least 4–6 weeks before drawing conclusions.
6. Assuming supplements are equivalent to food
They’re not. They’re useful in specific contexts. They don’t replicate the full nutritional matrix of whole plant foods [6].
7. Exceeding 50–60g per day
More is not always better. Above this threshold, you risk impaired mineral absorption and paradoxical constipation [4].
Frequently Asked Questions
Q1: What’s the easiest way to remember the difference between soluble and insoluble fiber?
Soluble fiber dissolves in water and forms a gel — think oats and beans going soft when cooked. Insoluble fiber doesn’t dissolve — think wheat bran and vegetable skins staying firm. Soluble slows things down; insoluble speeds things up.
Q2: Can I get enough fiber from supplements alone?
Technically you can hit a gram target, but you’ll miss the broader nutritional benefits of whole food fiber — including the variety of fermentable substrates that support microbial diversity. Supplements work best as a targeted addition, not a replacement for dietary fiber from whole foods [6].
Q3: Why does fiber cause bloating, and how do I stop it?
Bloating happens when gut bacteria ferment fiber rapidly, producing gas. The fix is to increase fiber slowly (no more than 5g per week), drink enough water, and spread fiber intake across meals rather than front-loading it. Starting with soluble fiber tends to cause less gas than starting with large amounts of insoluble fiber.
Q4: Is psyllium husk soluble or insoluble fiber?
Psyllium is predominantly soluble fiber. It forms a viscous gel in water, which is why it’s effective for both constipation (softens stool) and diarrhea (slows transit). It’s one of the most evidence-backed fiber supplements available [3].
Q5: Do fiber needs change after menopause or andropause?
Daily targets decrease slightly with age — women over 51 need around 22g per day, men over 51 around 28g [5]. However, the type of fiber that matters most doesn’t change. The bigger concern with age is that calorie intake often drops, so hitting fiber targets requires more deliberate food choices.
Q6: How do I know if I’m getting the right balance of soluble vs. insoluble fiber?
A practical check: if your stool is consistently soft and well-formed, transit is regular (once or twice daily), and you’re not experiencing chronic bloating, your fiber intake is probably working. If you’re constipated, increase insoluble fiber and water. If you’re loose or have urgency, focus on soluble fiber and reduce insoluble. These are starting points — persistent symptoms warrant a conversation with a clinician.
Conclusion
The gap between “eat more fiber” and actually doing it well is wider than most nutrition advice acknowledges. The distinction between soluble vs. insoluble fiber isn’t a technicality — it determines which foods you prioritize, how your gut responds, and whether fiber helps or hurts depending on your specific situation.
The basics still do the heavy lifting here. Eat a variety of whole plant foods. Ramp up slowly. Drink more water than you think you need. Aim for the right daily target for your age and sex. And if you have a digestive condition, don’t apply generic fiber advice without professional input.
Actionable next steps:
- Calculate your current intake — use a free food diary app for three days to see where you actually stand
- Identify your gap — compare your average to the targets in the table above
- Pick one high-impact addition — lentils, oats, or an apple with skin at one meal per day
- Add 5g per week maximum — and increase water intake alongside it
- Give it six weeks — before judging whether it’s working
Context matters. The numbers matter. And getting this right is less about discipline than it is about understanding what you’re actually doing and why.






