Gingivitis Gums: What it is, Symptoms, Causes, treatment, and prevention
- What Is Gingivitis, and How Is It Different from Periodontal Disease?
- How Common Is Gingivitis?
- What Are the Symptoms of Gingivitis?
- What Causes Gingivitis?
- How Is Gingivitis Diagnosed?
- What Are the Treatment Options for Gingivitis?
- How Does Gingivitis Affect Your Overall Health?
- How Can You Prevent Gingivitis?
- Gingivitis vs. Periodontitis: What’s the Difference?
Last updated: April 5, 2026
Quick Answer: Gingivitis gums is the earliest, most reversible stage of gum disease, caused by bacterial plaque accumulating along the gumline. It produces red, swollen, bleeding gums — but causes no bone or tooth loss at this stage. With consistent brushing, flossing, and professional dental cleanings, gingivitis gums can be fully reversed in most people within two to four weeks.
Key Takeaways
- Gingivitis is inflammation of the gums caused by plaque and tartar buildup; it is the precursor to more serious periodontal disease
- The most common symptoms are red or swollen gums, bleeding when brushing or flossing, and persistent bad breath
- Poor oral hygiene is the leading cause, but hormonal changes, certain medications, smoking, diabetes, and genetic factors all raise your risk
- Mild gingivitis often resolves with improved brushing and flossing alone; moderate to severe cases require professional dental treatment
- Untreated gingivitis can progress to periodontitis, which causes irreversible bone loss and eventual tooth loss
- Research links chronic gum disease to increased risk of heart disease, stroke, type 2 diabetes, and respiratory conditions
- A soft-bristled toothbrush, fluoride toothpaste, daily flossing, and dental visits every six months are the foundation of prevention
- Antiseptic mouthwashes containing chlorhexidine can help reduce bacterial load during active treatment
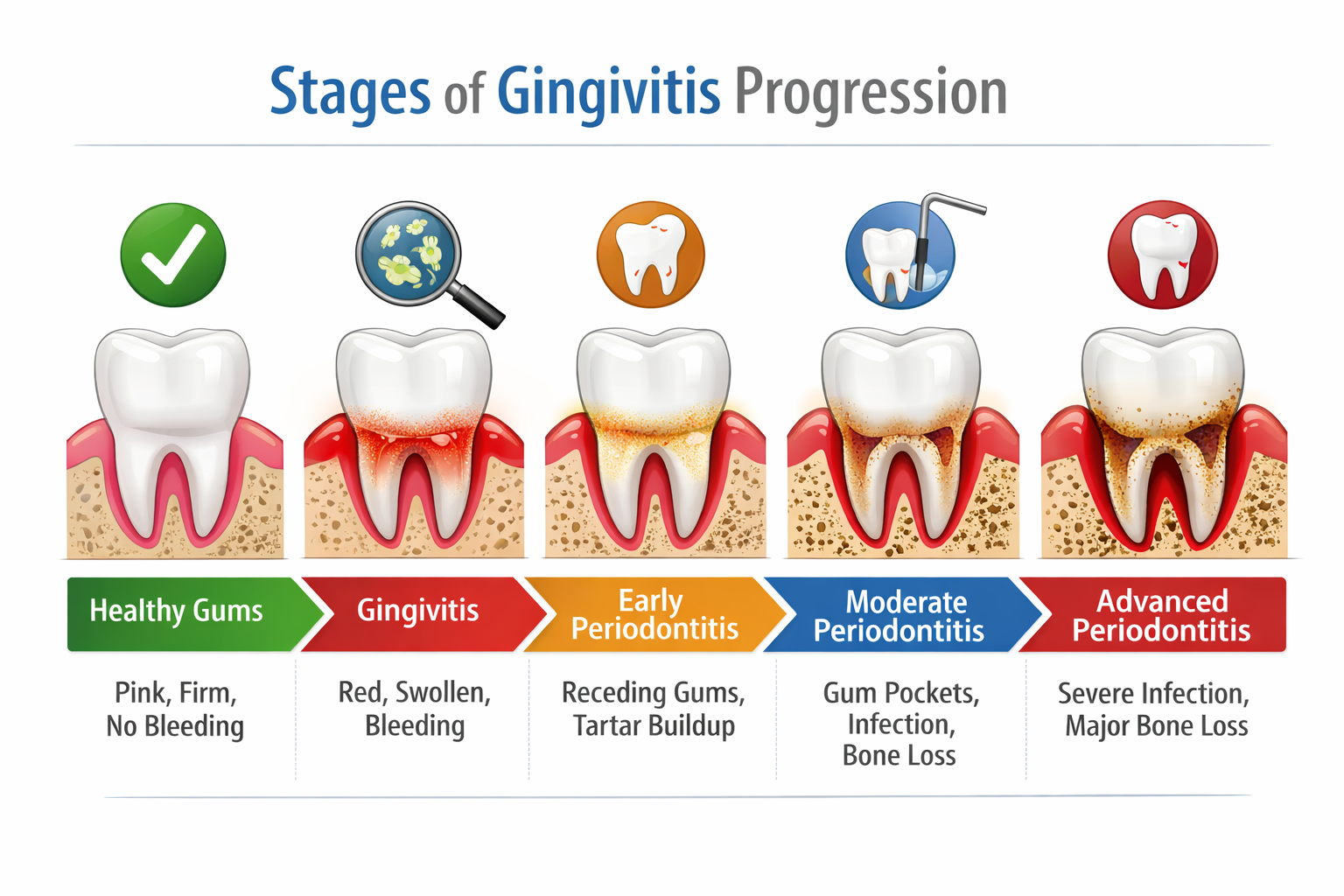
What Is Gingivitis, and How Is It Different from Periodontal Disease?

Gingivitis is gum inflammation caused by the buildup of bacterial plaque along and just below the gumline. It is the earliest form of gum disease and, critically, it has not yet damaged the bone or connective tissue holding your teeth in place.
That distinction matters. Gingivitis is fully reversible. Periodontal disease — the stage that follows when gingivitis is left untreated — causes permanent structural damage to the jawbone and gum tissue. Once bone is lost, it does not grow back without surgical intervention.
The word “gingivitis” breaks down simply: gingiva means gum tissue in Latin, and -itis means inflammation. So gingivitis is, at its core, inflamed gums. What drives that inflammation is a thin, sticky film of bacteria called plaque. When plaque is not removed through daily brushing and flossing, it hardens into tartar (also called calculus) within 24 to 72 hours. Tartar cannot be removed at home — it requires a professional dental cleaning.
How Common Is Gingivitis?
Gingivitis is extremely common, affecting a large proportion of adults at some point in their lives. According to the CDC’s National Health and Nutrition Examination Survey, nearly half of American adults aged 30 and older have some form of periodontal disease, with the prevalence rising sharply with age. Among adults 65 and older, that figure climbs to over 70%, according to CDC data published in the Journal of Dental Research (Eke et al., 2015).
Gingivitis, being the earliest stage, is even more widespread. Many people have it without knowing, because early gingivitis is painless and easy to overlook.
This matters because gingivitis does not stay mild on its own. Without treatment, it progresses — and the longer it progresses, the more complex and expensive the treatment becomes.
What Are the Symptoms of Gingivitis?
Gingivitis often develops quietly. The most reliable early warning sign is bleeding gums during brushing or flossing — something many people dismiss as normal. It is not normal. Healthy gums do not bleed.
Common symptoms include:
- Gums that bleed when you brush or floss
- Red, dark red, or purplish gum color (healthy gums are pale pink)
- Swollen or puffy gum tissue
- Gums that feel tender when touched
- Persistent bad breath (halitosis) that doesn’t resolve after brushing
- Gums that are beginning to pull away from the teeth (early recession)
- A visible buildup of yellowish or brown tartar at the gumline
What gingivitis does not cause (at this stage):
- Loose teeth
- Significant gum recession
- Pain when chewing
- Visible gaps between teeth and gums deeper than 3mm
If you’re experiencing loose teeth, deep gum pockets, or significant recession, the disease has likely progressed beyond gingivitis into periodontitis, and you need to see a periodontist promptly.
What Causes Gingivitis?
The root cause of most gingivitis is inadequate plaque removal. But several factors make some people significantly more vulnerable than others.
Poor Oral Hygiene
When plaque is not disrupted daily through brushing and flossing, it accumulates at the gumline and triggers an immune response in the surrounding tissue. That immune response is what causes the redness, swelling, and bleeding. The bacteria in plaque release toxins that irritate the gum tissue directly, compounding the inflammation.
Tobacco Use
Smoking and chewing tobacco are among the strongest risk factors for gum disease. Tobacco reduces blood flow to the gum tissue, impairs immune function, and slows healing. Smokers are significantly more likely to develop gingivitis and periodontitis than non-smokers — and their symptoms may be masked because reduced circulation can suppress visible bleeding even when disease is active.
Hormonal Changes
Fluctuating estrogen and progesterone levels during puberty, pregnancy, and menopause increase gum sensitivity and blood flow to gum tissue, making it more reactive to plaque. Pregnancy gingivitis is a well-documented phenomenon affecting many pregnant women, typically peaking in the second trimester.
Certain Medications
Several drug classes reduce saliva flow or cause gum tissue changes that raise gingivitis risk:
- Calcium channel blockers (used for high blood pressure, e.g., amlodipine) can cause gum overgrowth
- Anticonvulsants (e.g., phenytoin) are associated with gingival hyperplasia
- Immunosuppressants (e.g., cyclosporine) impair the body’s ability to fight oral bacteria
- Antihistamines and antidepressants reduce saliva, which is a natural antibacterial defense
If you’re on long-term medication and noticing gum changes, mention it to both your prescribing physician and your dentist.
Systemic Health Conditions
Diabetes is particularly significant: high blood glucose impairs white blood cell function, reducing the body’s ability to fight the bacteria causing gum disease. The relationship is bidirectional — gum disease also makes blood sugar harder to control. Conditions like HIV/AIDS, leukemia, and certain autoimmune disorders similarly compromise the immune response in gum tissue.
Genetic Predisposition
Some people are genetically more susceptible to gum disease regardless of how well they brush. If gum disease runs in your family, more frequent professional cleanings (every three to four months rather than every six) may be warranted.
How Is Gingivitis Diagnosed?
A dentist diagnoses gingivitis through a clinical examination combined with a review of your medical and dental history. The process is straightforward and typically takes only a few minutes within a routine checkup.
The diagnostic process includes:
- Medical history review — medications, systemic conditions, smoking status, and family history
- Visual examination — checking gum color, texture, contour, and any visible plaque or tartar
- Periodontal probing — a small calibrated probe is gently inserted between the tooth and gum to measure pocket depth. Healthy pockets measure 1–3mm. Readings of 4mm or more suggest disease progression
- Bleeding on probing — if the gum bleeds when probed, it confirms active inflammation
- Dental X-rays — used to check for bone loss below the gumline, which would indicate periodontitis rather than gingivitis
Gingivitis is confirmed when there is gum inflammation and bleeding but no bone loss on X-ray and no pockets deeper than 3–4mm.
What Are the Treatment Options for Gingivitis?
Treatment depends on severity. Mild gingivitis often resolves with improved home care alone. More established cases require professional intervention.
Professional Dental Cleaning (Prophylaxis)
For most people with early gingivitis, a professional cleaning is the primary treatment. The hygienist removes tartar above and just below the gumline using ultrasonic scalers and hand instruments, then polishes the teeth. Most patients see significant improvement within one to two weeks of improved home care following a cleaning.
Scaling and Root Planing
When gingivitis has progressed toward the early stages of periodontitis, scaling and root planing (sometimes called a “deep cleaning”) is the standard treatment. Scaling removes tartar from below the gumline; root planing smooths the root surface to discourage bacteria from reattaching. This is typically done under local anesthetic over one or two appointments.
Antimicrobial Treatments
Several medications can support treatment:
- Chlorhexidine mouthwash — a prescription-strength antiseptic rinse used twice daily for short-term bacterial reduction
- Antibiotic microspheres — tiny particles containing minocycline placed directly into gum pockets after scaling
- Antiseptic chips — small chlorhexidine chips inserted into pockets to release medication slowly over about a week
- Oral antibiotics — doxycycline or amoxicillin may be prescribed for short courses in cases involving systemic infection
Antibiotics are not a standalone treatment for gingivitis; they work alongside mechanical cleaning, not instead of it.
Laser Therapy
Some dental practices use laser treatment to remove inflamed gum tissue and kill bacteria in pockets. Laser therapy causes less bleeding and discomfort than traditional surgery for some patients, though it is not universally available and tends to cost more.
Surgical Options (for Advanced Disease)
If gingivitis has progressed to periodontitis, surgical procedures may be necessary:
- Flap surgery (pocket reduction surgery) — the gum is folded back to allow deep cleaning of the root surface, then sutured back into a tighter position
- Bone grafting — replaces bone destroyed by infection using synthetic, donor, or the patient’s own bone
- Soft tissue grafts — addresses significant gum recession by transplanting tissue from the palate or using donor tissue
- Crown lengthening — removes excess gum tissue to expose more of the tooth, often done before restorative work
Surgery is not a treatment for gingivitis itself — it becomes relevant only when the disease has advanced beyond the gum tissue into the supporting bone.
How Does Gingivitis Affect Your Overall Health?
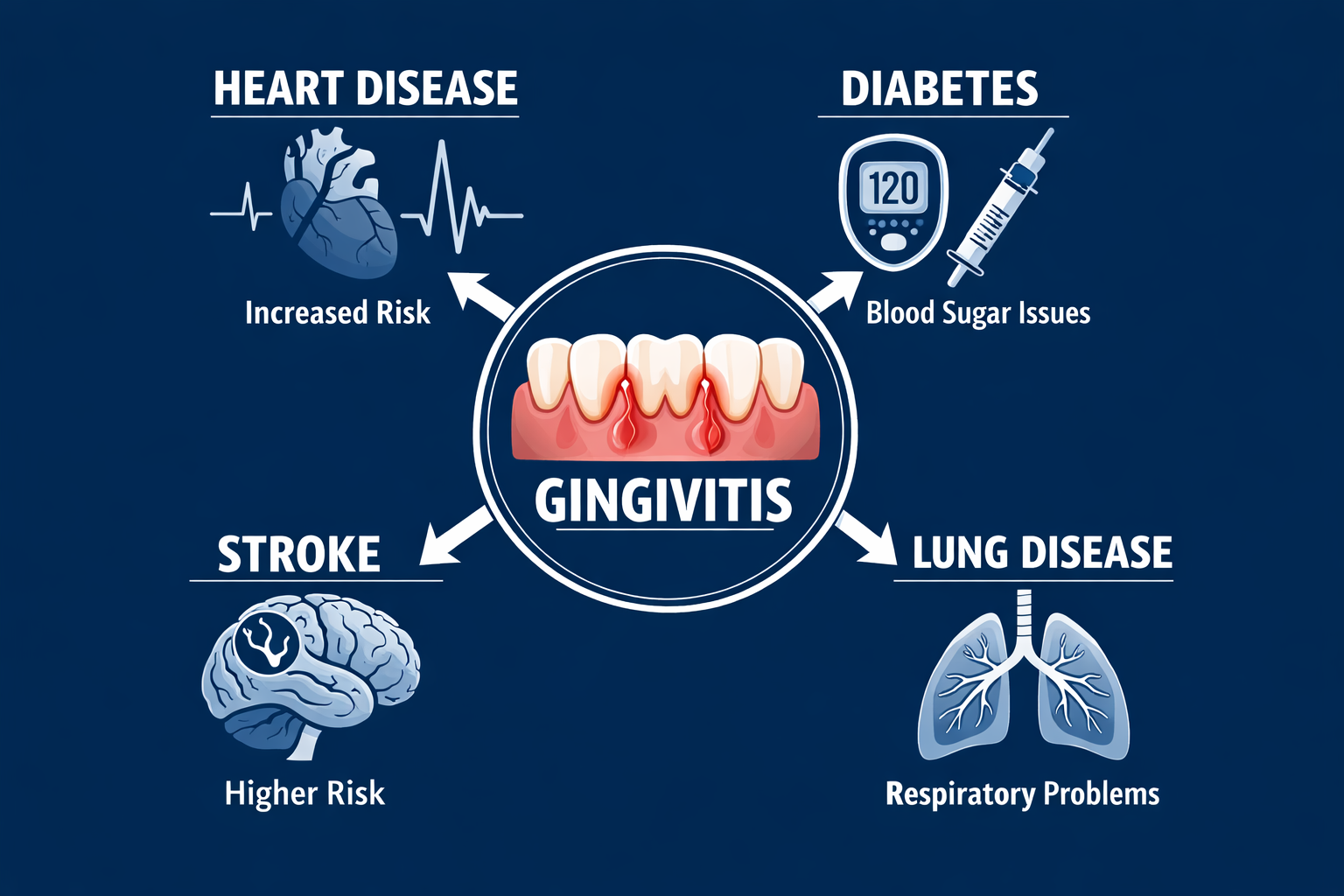
Gingivitis is not just a dental problem. Chronic gum inflammation creates a persistent source of bacteria and inflammatory compounds that can enter the bloodstream and affect distant organs.
The systemic connections are well-documented:
Heart disease and stroke: People with periodontal disease have a higher incidence of cardiovascular events. Oral bacteria, particularly Porphyromonas gingivalis, have been found in arterial plaques. The American Heart Association has acknowledged an association between periodontal disease and cardiovascular disease, though causality is still being studied.
Type 2 diabetes: The relationship between gum disease and diabetes is bidirectional. Gum disease makes blood sugar harder to control, and high blood sugar worsens gum disease. Treating periodontal disease has been shown in some studies to modestly improve HbA1c levels in people with type 2 diabetes.
Respiratory conditions: Oral bacteria can be aspirated into the lungs, contributing to pneumonia and worsening chronic obstructive pulmonary disease (COPD), particularly in older adults and those already immunocompromised.
Pregnancy complications: Periodontal disease during pregnancy has been associated with preterm birth and low birth weight, though research is ongoing. Treating gingivitis during pregnancy is safe and recommended.
Maintaining good gum health is genuinely part of maintaining overall health. If you’re interested in how anti-inflammatory foods can support your body’s inflammatory response more broadly, that’s a useful complement to good oral hygiene. Similarly, gut health and oral health share more overlap than most people realize, as the mouth is the entry point to the entire digestive system.
How Can You Prevent Gingivitis?
Prevention is straightforward in principle, though it requires consistency. The following habits, maintained regularly, prevent gingivitis in the vast majority of people.
Daily Oral Hygiene Routine
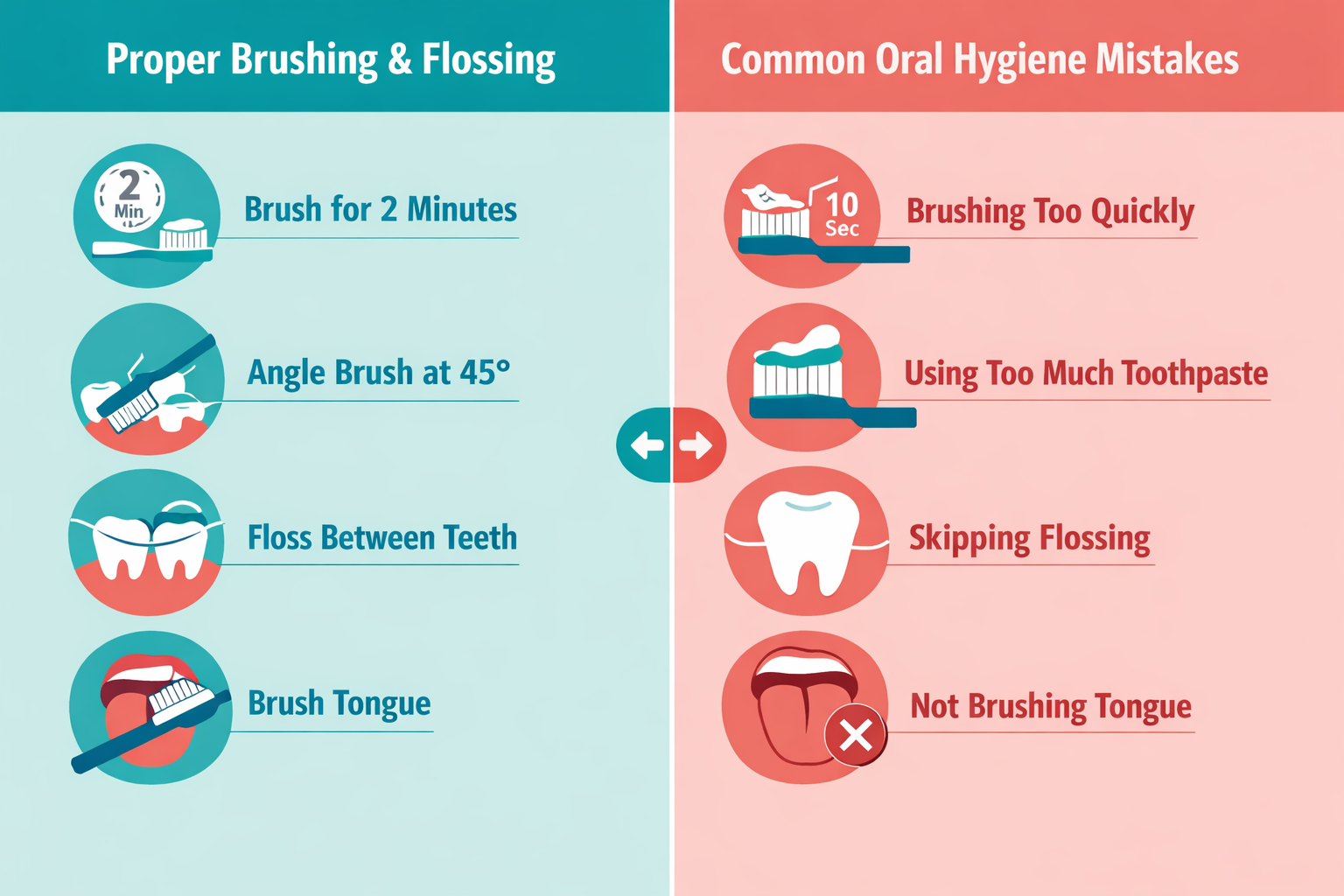
- Brush twice daily for two minutes using a soft-bristled toothbrush and fluoride toothpaste. Use gentle, circular strokes — scrubbing hard damages gum tissue rather than cleaning it better
- Floss once daily, ideally before bed, to remove plaque from between teeth where a toothbrush cannot reach. Floss picks and water flossers are acceptable alternatives for people who struggle with traditional floss
- Use an antiseptic mouthwash if recommended by your dentist — it reduces bacterial load but does not replace brushing or flossing
- Replace your toothbrush every three to four months, or sooner if the bristles are frayed
Regular Dental Visits
Professional cleanings every six months remove tartar that home care cannot address. People with a history of gum disease, smokers, or those with diabetes may benefit from cleanings every three to four months. Don’t skip these appointments — tartar buildup is silent and accumulates even in people who brush well.
Diet and Lifestyle
- Reduce sugary and starchy foods, which fuel the bacteria that produce plaque
- Drink water throughout the day to support saliva production, which naturally neutralizes acids and washes away bacteria
- Quit smoking — this is one of the most impactful changes you can make for gum health
- Manage systemic conditions like diabetes carefully, as blood sugar control directly affects gum tissue health
Eating foods rich in calcium supports the bone structure underlying your teeth, and reducing chronic stress — which impairs immune function — can also lower your susceptibility to gum inflammation. Stress management practices like regular exercise and adequate sleep are genuinely relevant to oral health, not just general wellness advice.
Gingivitis vs. Periodontitis: What’s the Difference?
| Feature | Gingivitis | Periodontitis |
|---|---|---|
| Bone loss | None | Present |
| Reversible | Yes, fully | No (bone loss is permanent) |
| Pocket depth | 1–3mm | 4mm or deeper |
| Tooth mobility | None | Possible in advanced cases |
| Bleeding on probing | Common | Common |
| Treatment | Cleaning + home care | Deep cleaning, possibly surgery |
| Pain | Usually none | Sometimes present |
The clearest takeaway: catch it at gingivitis, and you can reverse it completely. Wait until periodontitis, and you’re managing permanent damage.
Frequently Asked Questions About Gingivitis
Can gingivitis go away on its own?
Mild gingivitis can improve significantly with better brushing and flossing, but it rarely resolves without addressing the tartar that’s already formed. Professional cleaning combined with improved home care is the most reliable path to resolution.
How long does it take to reverse gingivitis?
Most people with mild gingivitis see clear improvement within two to four weeks of consistent brushing, flossing, and a professional cleaning. More established cases may take longer.
Is gingivitis contagious?
The bacteria that cause gingivitis can be transmitted through saliva — for example, through kissing or sharing utensils. However, developing gingivitis also depends on your own oral hygiene and immune response, so transmission doesn’t guarantee infection.
Can children get gingivitis?
Yes. Gingivitis is common in children and adolescents, particularly during puberty when hormonal changes increase gum sensitivity. The same prevention principles apply: twice-daily brushing, daily flossing, and regular dental visits.
Does gingivitis cause tooth loss?
Gingivitis itself does not cause tooth loss because it hasn’t yet damaged the bone. However, if it progresses to periodontitis, bone loss occurs and teeth can eventually loosen and fall out or require extraction.
Is bleeding gums always gingivitis?
Bleeding gums are the most common sign of gingivitis, but they can also result from brushing too hard, certain medications (especially blood thinners), vitamin C deficiency, or blood disorders. If bleeding persists after improving your oral hygiene, see a dentist.
Can I treat gingivitis at home without seeing a dentist?
You can significantly improve mild gingivitis at home through better brushing and flossing. But if tartar has formed, you cannot remove it at home — a professional cleaning is required. Attempting to self-treat moderate or severe gingivitis without professional help risks allowing it to progress silently.
What toothpaste is best for gingivitis?
Toothpastes containing stannous fluoride (such as Crest Pro-Health) have clinical evidence supporting their effectiveness against gingivitis. Triclosan-containing toothpastes were previously recommended but are now less commonly available. Ask your dentist for a specific recommendation based on your situation.
Does mouthwash cure gingivitis?
No. Mouthwash reduces bacterial load and can support treatment, but it does not remove plaque or tartar. It works as an adjunct to brushing and flossing, not a replacement.
Can stress cause gingivitis?
Stress doesn’t directly cause gingivitis, but it suppresses immune function, making it harder for your body to fight off the bacteria responsible for gum inflammation. People under chronic stress also tend to neglect oral hygiene habits, compounding the risk.
Sources
- Eke PI, Dye BA, Wei L, et al. “Prevalence of Periodontitis in Adults in the United States: 2009 and 2010.” Journal of Dental Research, 2012. CDC Periodontal Disease Data
- American Academy of Periodontology. “Gum Disease Information.” AAP
- American Heart Association. “Periodontal Disease and Cardiovascular Disease.” 2012 Scientific Statement.
- National Institute of Dental and Craniofacial Research (NIDCR). “Periodontal (Gum) Disease.” NIDCR
Foods that are anti-inflammatory

