Environmental factors that affect human health


Last updated: March 28, 2026
Quick Answer

Environmental factors that affect human health include air pollution, chemical exposure, contaminated water, climate change, poor indoor air quality, and microbial threats. These factors operate at every scale — from the air inside your home to industrial emissions released miles away — and collectively contribute to millions of preventable deaths each year. Understanding which environmental hazards pose the greatest risk, and what you can do about them, is the first step toward protecting your long-term health.
Key Takeaways
- The World Health Organization (WHO) estimates that environmental risk factors contribute to roughly 24% of all global deaths, with air pollution alone responsible for approximately 7 million premature deaths annually (WHO, 2024).
- Indoor air pollution is often more dangerous than outdoor air pollution because most people spend 80–90% of their time indoors.
- Chemical exposure — from food packaging, household cleaners, and industrial sources — is linked to cancer, hormonal disruption, and developmental problems in children.
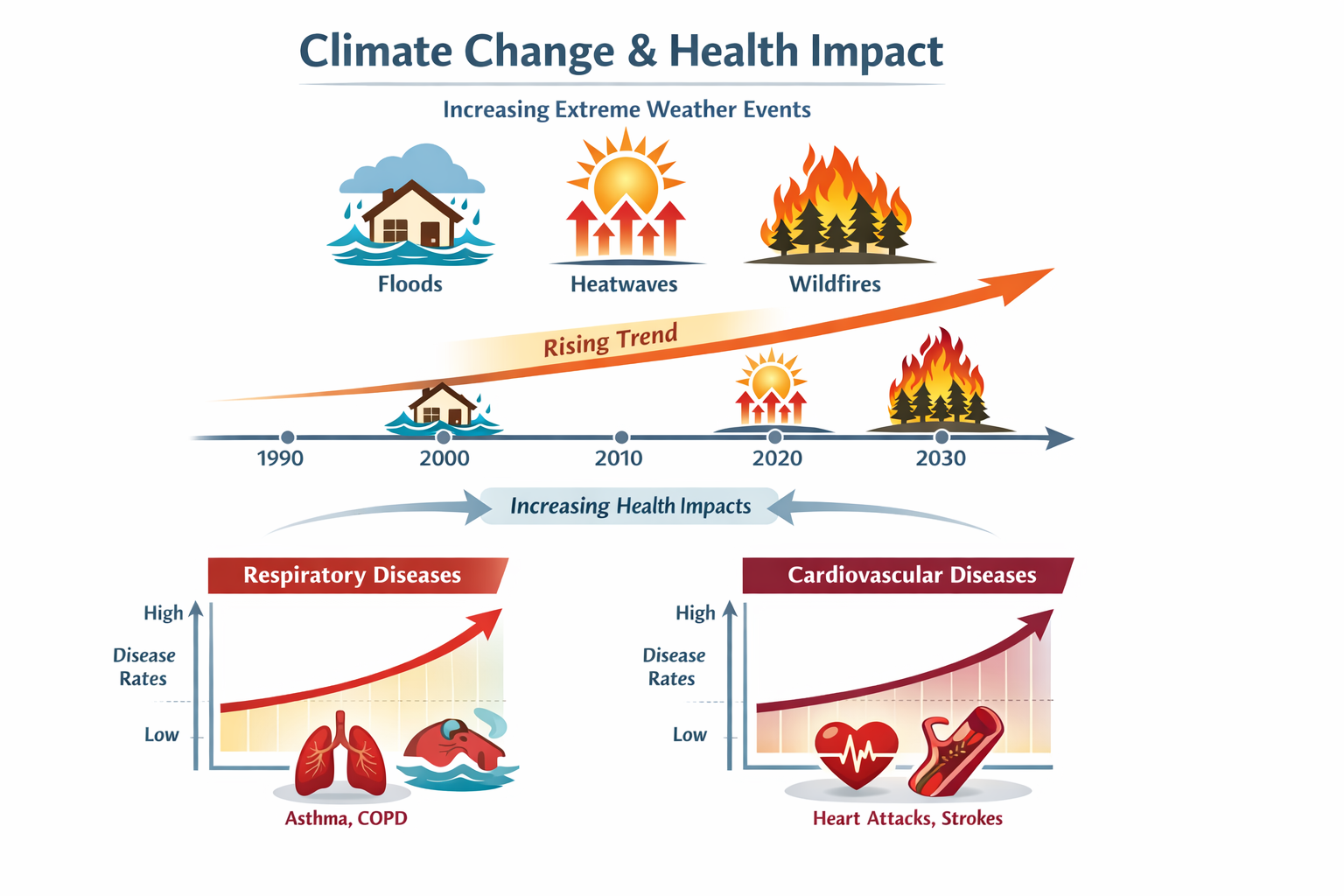
- Climate change is amplifying existing environmental health risks by increasing the frequency of heatwaves, floods, wildfires, and disease outbreaks.
- Microbial threats (bacteria, viruses, fungi) in water, food, and air remain a leading cause of illness globally, particularly in lower-income communities.
- Children, the elderly, and people with pre-existing conditions are disproportionately affected by environmental health hazards.
- Many environmental health risks can be reduced through practical, low-cost changes at home and through community-level action.
- Diet and nutrition play a supporting role in building resilience against environmental stressors — anti-inflammatory foods can help reduce the body’s inflammatory response to pollutants.
What Are Environmental Factors That Affect Human Health?
Environmental factors that affect human health are any external physical, chemical, or biological conditions in a person’s surroundings that influence their wellbeing. This includes the air they breathe, the water they drink, the chemicals in the products they use, the climate they live in, and the microorganisms present in their environment.
These factors don’t affect everyone equally. Where you live, what you do for work, your age, and your existing health status all determine your level of exposure and vulnerability. A child growing up near a petrochemical plant faces a very different environmental risk profile than an adult living in a rural area with clean air and access to fresh food.
The key environmental factors covered in this guide are:
- Air pollution (outdoor and indoor)
- Chemical safety and toxic exposure
- Water quality and contamination
- Climate change and extreme weather
- Microbial threats (bacteria, viruses, mould)
- Noise and light pollution (emerging area of concern)
Why Is Environmental Health Important for Communities?
Environmental health matters because no individual can fully protect themselves from risks that exist at a community or systemic level. You can eat well and exercise regularly, but if the air in your neighbourhood is heavily polluted or your tap water contains lead, your health outcomes are compromised regardless of your personal choices.
Healthy environments support healthy communities in concrete ways:
- Clean air reduces rates of asthma, cardiovascular disease, and lung cancer.
- Safe drinking water prevents gastrointestinal illness, developmental delays in children, and chronic kidney disease.
- Access to green spaces improves mental health, encourages physical activity, and reduces urban heat island effects.
- Reduced chemical exposure lowers cancer risk and protects hormonal health across all age groups.
The WHO’s 2024 environmental burden of disease data confirms that low- and middle-income countries bear a disproportionate share of environment-related illness, largely due to greater exposure to indoor cooking smoke, unsafe water, and industrial pollution with less regulatory oversight.
Common mistake: Treating environmental health as a concern only for environmentalists or policymakers. In reality, it directly shapes individual chronic disease risk, child development, and life expectancy.
How Does Air Pollution Affect Human Health?
Air pollution is the single largest environmental cause of premature death worldwide. Both outdoor (ambient) and indoor air pollution damage the respiratory and cardiovascular systems, and long-term exposure is linked to several cancers.
Outdoor Air Pollution
Outdoor air pollution comes primarily from vehicle exhaust, industrial emissions, power generation, and agricultural burning. The main pollutants of concern include:
- Particulate matter (PM2.5 and PM10): Tiny particles that penetrate deep into lung tissue. PM2.5 — particles smaller than 2.5 micrometres — can enter the bloodstream directly.
- Nitrogen dioxide (NO₂): Produced by vehicles and power plants. Linked to asthma and reduced lung function.
- Sulphur dioxide (SO₂): Released by coal burning and industrial processes. Causes airway inflammation.
- Ground-level ozone: Formed when sunlight reacts with vehicle emissions. Triggers asthma attacks and reduces lung capacity.
- Carbon monoxide (CO): Reduces the blood’s ability to carry oxygen. Dangerous at high concentrations.
- Heavy metals: Arsenic, cadmium, lead, and mercury from industrial sites accumulate in the body over time.
According to the WHO (2024), approximately 4.2 million deaths per year are attributable to outdoor air pollution, with cardiovascular disease and stroke accounting for the majority of those deaths.
Indoor Air Pollution
Indoor air pollution is frequently worse than outdoor air pollution, yet it receives far less attention. The main indoor pollutants include:
- Combustion products from gas stoves, wood-burning fires, and candles (carbon monoxide, nitrogen oxides, fine particles)
- Volatile organic compounds (VOCs) from paints, varnishes, cleaning products, and synthetic furniture
- Formaldehyde from pressed wood products, carpets, and adhesives
- Radon gas seeping from the ground into basements and lower floors
- Mould spores from damp surfaces
- Tobacco smoke — one of the most well-documented indoor air pollutants
Children are especially vulnerable to indoor air pollution. Their lungs are still developing, they breathe faster than adults relative to their body size, and they spend more time at floor level where some pollutants concentrate.
Practical steps to improve indoor air quality:
- Open windows regularly to increase ventilation, even for 10–15 minutes a day.
- Use exhaust fans when cooking, especially on gas stoves.
- Test your home for radon — test kits are widely available and inexpensive.
- Choose low-VOC paints and cleaning products.
- Keep indoor humidity below 60% to prevent mould growth.
- Add air-purifying houseplants — certain species have been shown to absorb some VOCs.
- Replace HVAC filters every 60–90 days and consider a HEPA air purifier for bedrooms.
If you’re working on building overall resilience alongside cleaner air, living a healthy lifestyle in a city covers practical strategies for urban environments where pollution exposure is highest.
What Chemical Exposures Pose the Greatest Health Risks?

Chemical exposure is a broad category that includes industrial pollutants, pesticides, heavy metals, endocrine-disrupting compounds, and synthetic additives in everyday consumer products. Many of these chemicals accumulate in body tissue over years, making their health effects difficult to trace to a single source.
The Most Concerning Chemical Hazards
Endocrine disruptors are chemicals that interfere with the body’s hormonal system. They include:
- Bisphenol A (BPA): Found in some plastic food containers and the lining of canned goods. Linked to hormonal disruption, obesity, early puberty in children, and certain cancers. Banned in food packaging in the EU and Canada, but still permitted in some products in the United States.
- Phthalates: Used to soften plastics and found in personal care products. Associated with reduced fertility and developmental issues in children.
- PFAS (per- and polyfluoroalkyl substances): Known as “forever chemicals” because they don’t break down in the environment. Found in non-stick cookware, food packaging, and water supplies near industrial sites. Linked to thyroid disease, kidney cancer, and immune suppression.
Pesticides used in agriculture can contaminate groundwater, persist in soil, and appear as residues on food. Organophosphate pesticides, in particular, are associated with neurological damage and are especially harmful to children during developmental stages.
Heavy metals — including lead, mercury, arsenic, and cadmium — enter the body through contaminated water, food, and air. Lead exposure in children causes irreversible cognitive impairment. Mercury, often found in certain fish species, affects neurological development in foetuses and young children.
How to Reduce Chemical Exposure at Home
- Check product ingredient lists before buying. Databases like the Environmental Working Group (EWG) provide safety ratings for thousands of consumer products.
- Choose glass or stainless steel containers over plastic, particularly for hot foods and beverages.
- Buy organic produce for the “Dirty Dozen” — the fruits and vegetables with the highest pesticide residue loads (updated annually by the EWG).
- Avoid non-stick cookware with damaged coatings. Ceramic or cast iron are safer alternatives.
- Use fragrance-free or naturally scented cleaning and personal care products.
- Run cold water for 30 seconds before drinking from the tap if your home has older plumbing.
Edge case: People who work in manufacturing, agriculture, construction, or healthcare face occupational chemical exposures that far exceed typical household risks. In these settings, following OSHA guidelines, using appropriate personal protective equipment, and requesting material safety data sheets (MSDS) for all chemicals in the workplace is essential.
How Does Water Contamination Affect Health?
Contaminated water is one of the most direct environmental pathways to illness. Water can carry biological contaminants (bacteria, viruses, parasites), chemical pollutants (heavy metals, pesticides, industrial chemicals), and radiological hazards (radon, uranium).
Common Water Contaminants and Their Health Effects
| Contaminant | Source | Health Effects |
|---|---|---|
| Lead | Old pipes and plumbing | Cognitive impairment, especially in children |
| Nitrates | Agricultural runoff | Dangerous for infants (“blue baby syndrome”) |
| Arsenic | Natural deposits, industrial discharge | Skin lesions, cancer, cardiovascular disease |
| PFAS | Industrial sites, firefighting foam | Thyroid disease, immune suppression, kidney cancer |
| E. coli | Sewage contamination | Severe gastrointestinal illness |
| Chlorine byproducts | Water treatment | Long-term cancer risk at high levels |
Access to safe drinking water remains a global challenge. According to WHO and UNICEF’s 2023 Joint Monitoring Programme report, approximately 2 billion people still lack access to safely managed drinking water at home.
What you can do:
- Request a water quality report from your local utility (required annually in most countries).
- Use a certified water filter — look for NSF/ANSI certification for the specific contaminants you want to remove.
- If you’re on a private well, test your water annually for bacteria, nitrates, and pH, and every 3–5 years for heavy metals and other contaminants.
Poor gut health can amplify the effects of waterborne contaminants. Supporting gut health and digestive wellness through diet and lifestyle can help the body process and recover from low-level environmental exposures more effectively.
How Does Climate Change Worsen Environmental Health Risks?
Climate change amplifies nearly every existing environmental health threat. It doesn’t create entirely new risks so much as it makes existing ones more frequent, more severe, and harder to manage.
The Main Climate-Health Pathways
Extreme heat: Rising average temperatures increase the frequency and intensity of heatwaves. Heat stress causes dehydration, heat exhaustion, and heat stroke. Older adults, outdoor workers, and people without access to air conditioning are most at risk. The European heatwave of 2022 was associated with over 60,000 excess deaths, according to a study published in Nature Medicine (2023).
Flooding and storms: More intense rainfall events increase flood risk, which contaminates drinking water supplies, damages sewage infrastructure, and creates conditions for mould growth in homes. Flooding also displaces communities, disrupting healthcare access and increasing mental health burdens.
Wildfires: Longer fire seasons driven by drought and heat produce smoke that travels hundreds of miles. Wildfire smoke contains fine particulate matter, carbon monoxide, and toxic compounds from burning buildings and vegetation. Communities far from the fire itself can experience dangerous air quality for days or weeks.
Infectious disease spread: Warmer temperatures expand the geographic range of disease-carrying vectors like mosquitoes and ticks. Diseases like dengue fever, Lyme disease, and West Nile virus are appearing in regions where they were previously rare. The WHO projects that climate change could cause an additional 250,000 deaths per year between 2030 and 2050 from malaria, malnutrition, diarrhoea, and heat stress.
Food and water security: Droughts and unpredictable growing seasons threaten agricultural output. This affects food availability, nutritional quality, and price — with the greatest impact on lower-income populations who already face food insecurity.
Choose this framing if: You’re assessing climate-health risk for a specific region. Coastal communities face flooding and storm surge risks. Inland and arid regions face greater wildfire and drought exposure. Urban areas face compounded heat island effects on top of rising baseline temperatures.
What Microbial Threats in the Environment Affect Human Health?
Microbes — including bacteria, viruses, fungi, and parasites — are present everywhere in the environment. Most are harmless or beneficial, but some cause serious illness, particularly when environmental conditions allow them to proliferate or when they enter the body through contaminated food, water, or air.
Key Microbial Environmental Health Threats
Waterborne pathogens: Bacteria like E. coli, Salmonella, Campylobacter, and parasites like Cryptosporidium and Giardia enter water supplies through agricultural runoff, sewage overflow, and inadequate treatment. They cause gastrointestinal illness ranging from mild discomfort to life-threatening dehydration.
Airborne pathogens: Viruses like influenza, SARS-CoV-2, and respiratory syncytial virus (RSV) spread through airborne droplets. Poor ventilation in indoor spaces dramatically increases transmission risk. Legionella bacteria, which causes Legionnaires’ disease, can grow in poorly maintained water systems and air conditioning units.
Foodborne pathogens: Contamination during food production, processing, or preparation introduces pathogens including Listeria, Salmonella, and Staphylococcus aureus. The WHO estimates that foodborne diseases cause approximately 600 million illnesses and 420,000 deaths globally each year (WHO, 2022).
Mould and mycotoxins: Mould thrives in damp, poorly ventilated environments. Certain mould species produce mycotoxins — toxic compounds that can cause respiratory illness, neurological symptoms, and immune suppression with prolonged exposure. Stachybotrys chartarum (commonly called “black mould”) is among the most studied, though many mould species pose health risks.
Soil-borne pathogens: Clostridium tetani (tetanus), Clostridium botulinum (botulism), and Histoplasma (a fungal infection) live in soil and can enter the body through wounds or inhalation of disturbed soil.
Reducing Microbial Risk in Your Environment
- Maintain indoor humidity between 30–50% to inhibit mould growth.
- Ensure HVAC and cooling tower systems are regularly cleaned and maintained.
- Practice proper food safety: cook to safe temperatures, refrigerate promptly, and avoid cross-contamination.
- Wash hands thoroughly and frequently, particularly after outdoor activities and before eating.
- Ensure vaccinations are current — vaccines protect against several environmentally transmitted pathogens including tetanus, hepatitis A, and influenza.
If gastrointestinal symptoms follow suspected exposure to contaminated food or water, natural ways to soothe your stomach can provide supportive relief while recovery progresses.
Who Is Most Vulnerable to Environmental Health Hazards?
Not everyone is equally affected by environmental factors. Vulnerability depends on biology, age, socioeconomic status, and geographic location.
High-Risk Groups
Children (especially under 5):
- Breathe more air relative to body weight than adults
- Have developing organ systems that are more sensitive to toxins
- Spend more time on the floor where some pollutants settle
- Are less able to metabolise and excrete certain chemicals
Older adults:
- Have reduced lung and cardiovascular reserve
- Are more susceptible to heat stress and dehydration
- Often have pre-existing conditions that are worsened by pollution
Pregnant women:
- Pollutant exposure can cross the placenta and affect foetal development
- Air pollution exposure during pregnancy is linked to preterm birth and low birth weight
People with pre-existing conditions:
- Asthma, COPD, heart disease, and diabetes all increase sensitivity to environmental stressors
Low-income communities:
- More likely to live near industrial sites, highways, or waste facilities
- Less likely to have access to air conditioning, clean water filtration, or healthcare
- This pattern — sometimes called “environmental injustice” — is well-documented in public health literature
Outdoor and industrial workers:
- Face elevated occupational exposure to heat, chemicals, particulate matter, and biological hazards
What Practical Steps Can You Take to Protect Your Health From Environmental Risks?
Protecting yourself from environmental health risks doesn’t require a complete lifestyle overhaul. Many of the most effective steps are low-cost and can be implemented immediately.
At Home
- Test your air and water. Radon test kits cost under $30. Annual water testing for a private well typically costs $100–$300 depending on the panel.
- Improve ventilation. Open windows daily, use exhaust fans, and consider a HEPA air purifier for bedrooms.
- Switch to safer products. Replace conventional cleaning products with fragrance-free or naturally derived alternatives. Check the EWG’s Skin Deep database for personal care products.
- Reduce plastic use. Store food in glass or stainless steel. Avoid heating food in plastic containers.
- Control moisture. Fix leaks promptly, use bathroom exhaust fans, and monitor indoor humidity.
Through Diet
Diet is one of the most accessible tools for building resilience against environmental stressors. Certain nutrients and food compounds support the body’s detoxification pathways and reduce inflammation caused by pollutant exposure.
- Antioxidant-rich foods — berries, leafy greens, and cruciferous vegetables — help neutralise oxidative stress caused by air pollution and chemical exposure.
- Omega-3 fatty acids from oily fish, walnuts, and flaxseed have anti-inflammatory properties that may partially offset the cardiovascular effects of air pollution.
- Fibre supports gut health and helps the body eliminate certain toxins through the digestive system.
- Foods with anti-inflammatory properties are particularly relevant for people with high pollution exposure.
At the Community Level
- Advocate for local air quality monitoring and public reporting.
- Support policies that reduce industrial emissions and improve public transport.
- Participate in community clean-up initiatives and tree-planting programmes, which reduce urban heat and improve air quality.
- Know your rights: in most countries, residents have the right to access environmental monitoring data for their area.
Frequently Asked Questions
Q: What is the biggest environmental factor affecting human health?
Air pollution is consistently identified as the largest single environmental contributor to premature death globally, responsible for an estimated 7 million deaths per year according to the WHO (2024). Indoor air pollution accounts for roughly 3.2 million of those deaths.
Q: How do environmental factors cause chronic disease?
Environmental factors cause chronic disease through repeated, low-level exposure to pollutants that damage cells, trigger inflammation, disrupt hormonal signalling, and impair organ function over time. Air pollution, for example, promotes arterial inflammation that contributes to heart disease. Chemical exposure can alter gene expression in ways that increase cancer risk.
Q: Can diet help protect against environmental pollution?
Yes, to a meaningful degree. Antioxidants, omega-3 fatty acids, and fibre support the body’s ability to manage oxidative stress and inflammation caused by pollutant exposure. Diet alone cannot eliminate the health effects of heavy pollution, but it’s a practical supporting measure.
Q: Is indoor or outdoor air pollution more dangerous?
For most people, indoor air pollution poses a greater cumulative risk because people spend significantly more time indoors. However, outdoor air pollution contributes heavily to cardiovascular and respiratory disease at the population level, particularly in urban and industrial areas.
Q: How does climate change affect infectious disease?
Climate change expands the geographic range of disease vectors like mosquitoes and ticks, which carry malaria, dengue, Lyme disease, and other infections. Warmer temperatures also allow some pathogens to survive in environments where they previously could not.
Q: What chemicals should I be most concerned about in my home?
The most common household chemical concerns are VOCs from paints and cleaning products, PFAS from non-stick cookware and food packaging, BPA and phthalates from plastics, formaldehyde from pressed wood furniture, and radon from the ground. Testing and product substitution address most of these.
Q: How can I find out about pollution levels in my area?
In the United States, AirNow.gov provides real-time air quality data. The EPA’s Envirofacts database shows nearby industrial emission sources. In the UK, the DEFRA air quality monitoring network provides similar data. Most developed countries have publicly accessible environmental monitoring portals.
Q: Are children more affected by environmental hazards than adults?
Yes. Children breathe more air relative to their body weight, have developing organ systems that are more sensitive to toxins, and spend more time in environments where some pollutants concentrate (floor level, schools). The health effects of early environmental exposures can persist throughout life.
Q: What is environmental injustice?
Environmental injustice refers to the disproportionate burden of environmental hazards borne by low-income communities and communities of colour. These populations are more likely to live near industrial facilities, highways, and waste sites, and less likely to have resources to mitigate exposure.
Q: How does noise pollution affect health?
Chronic noise exposure — from traffic, airports, and industrial sources — is linked to sleep disruption, elevated stress hormones, cardiovascular disease, and cognitive impairment in children. The WHO identifies noise pollution as a significant but under-recognised environmental health threat in Europe and other urbanised regions.
Q: What is the link between environmental factors and mental health?
Growing evidence links environmental exposures to mental health outcomes. Air pollution is associated with increased rates of depression and anxiety. Extreme weather events cause trauma and displacement. Green space exposure, conversely, is linked to reduced stress, better mood, and lower rates of mental illness.
Q: How do I know if my tap water is safe to drink?
Request your utility’s annual Consumer Confidence Report (required in the US and many other countries). For private wells, test annually for bacteria and nitrates, and every few years for heavy metals and other contaminants. If you have older plumbing, test specifically for lead.
Related Reading
- How to Live a Healthy Lifestyle — practical foundations for health that complement environmental protection
- Anti-Inflammatory Foods: Ultimate Guide — dietary strategies that support resilience against environmental stressors
- Gut Health and Digestive Wellness — how digestive health affects your body’s ability to handle environmental toxins
- Foods That Are Anti-Inflammatory — specific foods that reduce inflammation linked to pollution exposure
Sources
- World Health Organization. Ambient (outdoor) air quality and health. WHO, 2024. who.int
- WHO & UNICEF Joint Monitoring Programme. Progress on Household Drinking Water, Sanitation and Hygiene 2000–2022. 2023.
- WHO. Food safety: Key facts. 2022. who.int
- Ballester, J. et al. Heat-related mortality in Europe during the summer of 2022. Nature Medicine, 2023.
- WHO. Climate change and health. 2023. who.int
- Environmental Working Group. EWG’s Dirty Dozen. 2024. ewg.org
*** More great articles that may be of interest to you 🙂




