The Gut Brain Axis: How Your Belly Talks to Your Brain (And What to Do About It)

In this guide
- What the Gut-Brain Axis Actually Is
- The Vagus Nerve — Your Body’s Internet Cable
- Your Microbiome’s Secret Pharmacy
- The Stress Loop — How Your Brain Wrecks Your Gut
- The Conditions Where the Gut-Brain Axis Plays a Real Role
- Signs Your Gut-Brain Axis Might Be Off
- The Boring Stuff That Actually Works
- Specific Practices That Improve Vagal Tone
- Psychobiotics — Hype vs. Reality
- Diet Patterns That Support the Gut-Brain Axis
- When Gut-Brain Issues Need a Doctor (Red Flags)
Last updated: April 25, 2026
Roughly 90% of your body’s serotonin is made in your gut — not your brain. If that surprises you, you’re not alone. For most of medical history, the gut and brain were treated as separate systems that occasionally sent each other polite memos. We now know they’re in constant, 24/7 conversation through nerves, hormones, and immune signals. This biological highway is known as the gut brain axis, a living microbial ecosystem that influences your mood, your focus, and your stress response in ways that are only starting to be fully mapped. Let’s keep this practical and start with what the evidence actually says.
Quick Answer
The gut-brain axis is a bidirectional communication system linking your gut and brain through the vagus nerve, neurotransmitters, immune signals, and hormones. Disruption to this system is associated with anxiety, depression, brain fog, IBS, and poor sleep. The strongest evidence for improving it points to soluble vs insoluble fiber and daily targets that feed the right bacteria, fermented foods, quality sleep, regular exercise, and stress management — not expensive supplement bundles. Specific probiotic strains show modest, real effects for mood and anxiety, but they work best as part of a broader lifestyle approach, not as standalone fixes.
Key Takeaways
- The gut contains over 500 million neurons — more than the spinal cord — forming what researchers call the “enteric nervous system” or second brain [1]
- Around 90% of the body’s serotonin is produced in the gut, not the brain [2]
- The vagus nerve is the main communication highway, and roughly 80% of its fibers carry signals upward — from gut to brain — not the other way around [1]
- Chronic stress disrupts the gut microbiome within hours, creating a feedback loop that worsens both gut and mental health [2]
- The strongest evidence for gut-brain support comes from diet quality, sleep, and stress management — not supplements
- Specific probiotic strains (Lactobacillus rhamnosus, Bifidobacterium longum) have real but modest evidence for mood and anxiety effects
- The Mediterranean diet has the strongest dietary evidence for supporting both complete gut health and digestive wellness guide and mental wellbeing
- Persistent depression, suicidal thoughts, or sudden cognitive changes need professional assessment — not a probiotic
What the Gut Brain Axis Actually Is
The gut-brain axis is the two-way communication network between your gastrointestinal tract and your central nervous system. It’s not a metaphor. It’s a physical, chemical, and electrical system that operates continuously, whether you’re aware of it or not [1].
Think of it like a bidirectional control loop in an industrial system — the kind an engineer would recognise immediately. You have two processing units (gut and brain), multiple communication channels running between them, and feedback mechanisms that constantly adjust the system’s output based on incoming data. When the loop is working well, the system self-regulates. When one end gets disrupted, the whole loop can start producing bad outputs.
The four main communication channels are:
- The vagus nerve — the primary physical cable, running from brainstem to gut
- Neurotransmitters — chemical messengers produced in the gut that influence brain function
- Immune signaling — cytokines and inflammatory molecules that cross the gut-brain barrier
- Hormonal pathways — including cortisol and other stress hormones that affect both ends
The enteric nervous system — the network of neurons embedded in your gut wall — contains over 500 million neurons [1]. That’s more than your spinal cord. It can operate independently of the brain, which is why it earned the “second brain” label. But it’s also in constant dialogue with your central nervous system, and that dialogue shapes how you feel, think, and respond to stress [2].
Here’s the real issue with how most people think about this: they assume the brain is in charge and the gut just follows orders. The evidence says otherwise. The gut is sending far more information upward than it receives going down.
The Vagus Nerve — Your Body’s Internet Cable
The vagus nerve is the longest cranial nerve in the body. It runs from your brainstem down through your neck, chest, and abdomen, connecting directly to your heart, lungs, and gut. It is the primary physical pathway of the gut-brain axis [1].
Here’s the fact that changes how you think about this system: approximately 80% of vagal nerve fibers carry signals from the gut up to the brain. Only about 20% carry signals downward [1]. In plain English, your gut is doing most of the talking. Your brain is mostly listening.
This explains something that a lot of people experience but can’t quite articulate — why physical gut states so reliably affect mental states. When your gut is inflamed, dysbiotic, or under stress, it is actively broadcasting that information to your brain via the vagus nerve. The brain then responds with changes in mood, alertness, anxiety levels, and cognitive clarity.
Vagal tone is the term used to describe how well this system functions. Higher vagal tone is associated with better emotional regulation, lower inflammation, and more resilient stress responses. The good news is that vagal tone is trainable.
Practices that improve vagal tone:
- Slow nasal breathing — techniques like box breathing (4 seconds in, hold 4, out 4, hold 4) or the 4-7-8 method directly stimulate the vagus nerve
- Cold exposure — cold showers or face immersion in cold water activates the vagal response; the evidence here is real, not just biohacker folklore
- Humming, singing, and gargling — the vagus nerve innervates the throat muscles; these activities create vibrations that stimulate it directly
- Gentle movement — yoga, tai chi, and slow walking all show measurable effects on vagal tone
- Social connection — genuine face-to-face interaction has a documented effect on vagal activity through the polyvagal system (Stephen Porges’ work)
Recent research has also explored transcutaneous auricular vagus nerve stimulation (taVNS) — a non-invasive technique that stimulates the vagus nerve through the ear. A 2025 study found that taVNS demonstrated antidepressant properties in animal models, partly by altering gut microbiota composition and increasing beneficial Akkermansia muciniphila bacteria [3]. This is early-stage research, but it points to the same conclusion: the vagus nerve and the microbiome are deeply connected, and supporting one tends to support the other.
Your Microbiome’s Secret Pharmacy
Your gut microbiome — the roughly 38 trillion bacteria, fungi, and other microorganisms living in your digestive tract — is not just processing food. It’s running what amounts to a small pharmaceutical operation, producing or influencing compounds that directly affect brain function [2].
Key compounds your gut microbiome produces or influences:
| Compound | Role | Gut contribution |
|---|---|---|
| Serotonin | Mood, sleep, appetite regulation | ~90% produced in gut [2] |
| Dopamine precursors | Motivation, reward, focus | Significant gut involvement |
| GABA | Calm, anxiety regulation | Produced by specific gut bacteria [2] |
| Short-chain fatty acids (SCFAs) | Brain fuel, anti-inflammatory | Produced from dietary fiber fermentation |
| Tryptophan metabolites | Mood, immune regulation | Gut-bacteria dependent |
The 90% serotonin figure deserves a moment of attention. Most people associate serotonin with antidepressants and brain chemistry. The fact that the overwhelming majority of it is manufactured in the gut — primarily by enterochromaffin cells that are directly influenced by gut bacteria — is not a minor footnote. It’s a central fact about how mood regulation actually works [2].
Different bacteria produce different neurotransmitter profiles. This is why microbiome diversity matters more than any single strain. A diverse, well-fed microbiome produces a broader and more stable range of these compounds. A depleted or imbalanced microbiome — what researchers call dysbiosis — produces a narrower, less stable profile, which can contribute to mood instability, anxiety, and cognitive difficulties [2] [6].
The simplest way to look at it is this: your gut bacteria are not passive passengers. They are active participants in your neurochemistry.
The Stress Loop — How Your Brain Wrecks Your Gut
The gut-brain axis runs in both directions, and this is where chronic stress becomes a serious problem. When your brain perceives a threat — real or imagined — it activates the hypothalamic-pituitary-adrenal (HPA) axis, releasing cortisol and other stress hormones. Those hormones travel to the gut and start causing problems [2].
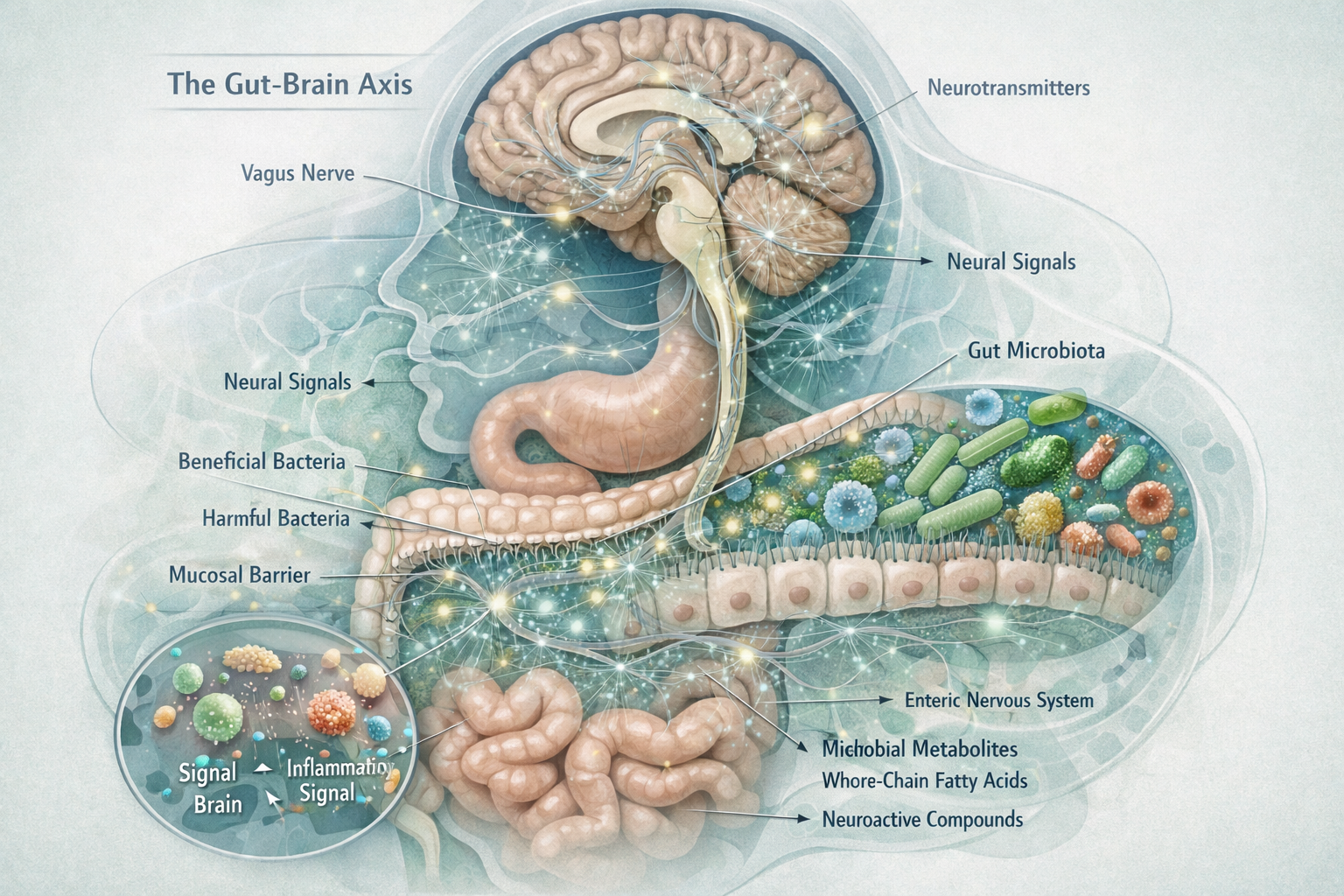
What chronic stress does to your gut:
- Loosens what the science actually says about leaky gut and intestinal permeability in the gut lining, increasing intestinal permeability (sometimes called “leaky gut”)
- Shifts microbiome composition within hours — stress-induced changes in gut bacteria have been documented in research settings
- Reduces production of serotonin and dopamine precursors in the gut [6]
- Dysregulates the HPA axis itself — gut dysbiosis feeds back into cortisol regulation, making stress responses harder to control [2]
- Increases systemic inflammation via immune signaling, which is strongly associated with depressive symptoms [2]
This is the loop that many people are stuck in without realising it: chronic stress disrupts the gut, the disrupted gut sends distress signals back to the brain via the vagus nerve, the brain interprets those signals as more threat, and the stress response continues. It’s a self-reinforcing cycle.
Here’s the real issue: stress management isn’t optional if you’re trying to support your gut health. You can eat all the fermented foods you want, but if you’re running on chronic cortisol, you’re fighting the loop from only one end.
The Conditions Where the Gut Brain Axis Plays a Real Role
We need to separate fact from hype here, because the range of claims made about the gut-brain axis runs from “genuinely well-supported” to “barely plausible.” Here’s where the evidence actually sits.
Strong evidence
Irritable Bowel Syndrome (IBS) is the most thoroughly studied gut-brain axis condition. The bidirectional relationship between gut dysfunction and psychological distress in IBS is well-established. Gut-directed hypnotherapy, cognitive behavioural therapy, and specific dietary interventions all show measurable effects [1].
Depression has a documented association with microbiome differences. People with depression consistently show altered gut microbiota profiles compared to healthy controls, with reduced diversity and lower levels of specific beneficial bacteria [6]. The causal direction is still being worked out — does the microbiome change cause depression, or does depression change the microbiome? Probably both, which is consistent with the bidirectional loop model.
Growing evidence
Anxiety disorders, sleep disturbances, brain fog, and chronic fatigue all show associations with gut microbiome composition and gut-brain signaling in current research [2] [4]. The evidence is real but not yet at the level where clinicians can prescribe specific microbiome interventions. The stronger evidence points to general gut health support — diet, sleep, stress management — rather than targeted probiotic therapy.
Emerging research
ADHD, autism spectrum conditions, Parkinson’s disease, and Alzheimer’s disease are all areas where gut-brain axis research is active and producing interesting early findings [5]. The Parkinson’s-gut connection is particularly intriguing — some researchers have proposed that the disease may originate in the gut and travel to the brain via the vagus nerve. This is compelling but not yet confirmed.
I would be careful with that level of extrapolation at this stage. The research is worth watching, but it’s not yet a basis for clinical recommendations.
Overhyped online
Direct cures for chronic mental illness through gut interventions. This is where hype gets in the way of genuinely useful science. The gut-brain axis is real and clinically relevant, but it is not a back door around psychiatry. Serious mental illness requires professional assessment and evidence-based treatment. how probiotics and prebiotics actually differ — and which strains matter and fiber are not replacements for antidepressants, therapy, or psychiatric care.
That’s a strong claim and it needs to be said clearly: supporting your gut health may be a useful complement to mental health treatment, but it is not a substitute.
Signs Your Gut-Brain Axis Might Be Off
These are patterns worth paying attention to — not a diagnostic checklist, but a set of signals that suggest the gut-brain conversation may be disrupted.
Common patterns:
- 🔵 Frequent what really causes bloating — and the four bloater types combined with low mood — not just digestive discomfort, but a consistent pairing of the two
- 🔵 Anxiety that reliably worsens after eating — particularly after high-sugar or ultra-processed meals
- 🔵 Brain fog after meals — a heavy, unfocused feeling that follows eating, especially larger meals
- 🔵 “Butterflies” before stressful events that linger as digestive trouble — the classic stress-gut response that doesn’t resolve quickly
- 🔵 Sleep problems alongside digestive issues — both the gut microbiome and sleep are regulated by circadian rhythms; disruption to one often disrupts the other
- 🔵 New mood or energy issues following a course of antibiotics — antibiotics can significantly alter microbiome composition, and some people notice mood changes in the weeks following treatment
None of these patterns are diagnostic on their own. But if several of them apply to you consistently, it’s reasonable to consider gut-brain axis support as part of your overall health approach — and to mention the pattern to your doctor.
The Boring Stuff That Actually Works
There is no magic in it. The interventions with the strongest evidence for supporting the gut-brain axis are the same ones that support general health. This is either reassuring or frustrating, depending on your perspective.
The basics still do the heavy lifting:
- Dietary fiber — feeds the bacteria that produce SCFAs and GABA. Aim for 25–35g per day from whole food sources. Most people in Western countries get roughly half that. This is the single highest-return dietary change for microbiome health.
- Fermented foods — yogurt, kefir, kimchi, sauerkraut, miso. The evidence for modest but real microbiome benefits is solid. You don’t need large quantities — a serving or two daily is a sensible starting point.
- Sleep quality and duration — the gut microbiome follows a circadian rhythm. Disrupted sleep disrupts microbial composition, and vice versa. Seven or more hours of quality sleep is not optional for gut-brain health.
- Regular moderate exercise — consistent moderate exercise increases microbiome diversity. More is not always better here — very high-intensity training without adequate recovery can have the opposite effect.
- Time in nature — exposure to diverse natural environments appears to increase microbial diversity, both through direct contact and through stress reduction. The evidence is modest but real.
- Reducing ultra-processed food — ultra-processed foods disrupt microbiome composition, reduce diversity, and are associated with higher rates of depression and anxiety [6]. This is one of the cleaner associations in the diet-mental health literature.
- Chronic stress reduction — I keep returning to this because it’s the lever most people underestimate. Stress management is gut health management.
Keep it simple and consistent. None of these require a supplement budget or a special protocol. They require sustained, ordinary effort — which is harder than buying something, but considerably more effective.
Specific Practices That Improve Vagal Tone
Vagal tone is trainable. These practices have actual evidence behind them, not just wellness community enthusiasm.
Breathing techniques:
Slow, diaphragmatic breathing is the most accessible vagal tone intervention. The evidence for slow nasal breathing (around 5–6 breath cycles per minute) on heart rate variability — a proxy for vagal tone — is well-established. Box breathing and the 4-7-8 technique both work. The key is consistency: a few minutes daily produces measurable effects over weeks.
Cold exposure:
Cold water immersion and cold showers activate the diving reflex, which strongly stimulates the vagus nerve. Even 30–60 seconds of cold water at the end of a shower is enough to produce a vagal response. Start with what you can manage and build from there. I prefer to look at what actually works rather than what sounds dramatic — and cold exposure, used sensibly, works.
Humming, singing, and gargling:
This sounds trivial, but the mechanism is real. The vagus nerve innervates the muscles of the larynx and pharynx. Humming, singing, and gargling create vibrations that directly stimulate vagal activity. Choir singers and regular singers show higher vagal tone in some studies. Gargling with water for 30 seconds a few times a day is a genuinely low-effort, evidence-supported practice.
Gentle movement:
Yoga, tai chi, and slow walking all show measurable effects on vagal tone. The mechanism involves both the breathing patterns these practices encourage and the parasympathetic activation that comes with slow, intentional movement.
Social connection:
Stephen Porges’ polyvagal theory describes how the social engagement system — eye contact, facial expression, prosodic voice — is directly linked to vagal regulation. Genuine face-to-face social interaction is not just good for mental health in a vague sense; it has a measurable effect on vagal tone. This is worth taking seriously in an era when screen-mediated communication has largely replaced in-person contact for many people.
Psychobiotics — Hype vs. Reality
Psychobiotics are probiotic strains studied specifically for their effects on mental health and brain function. The term was coined by researchers John Cryan and Ted Dinan at APC Microbiome Ireland, who have been among the most rigorous investigators in this field. Their work deserves credit for bringing scientific discipline to an area that is otherwise saturated with marketing claims.
What the evidence actually shows:
The two strains with the strongest current evidence are:
- Lactobacillus rhamnosus — studied in animal models and some human trials for anxiety and stress response. The effects are real but modest. The mechanism appears to involve GABA receptor modulation via the vagus nerve.
- Bifidobacterium longum — studied for effects on stress, anxiety, and cognitive performance. Again, modest but real effects in human trials, with the strongest results in people with elevated baseline stress or IBS.
What matters most is this: these effects are strain-specific, dose-dependent, and modest in magnitude. A generic “mood probiotic” containing unspecified strains at unspecified doses is mostly marketing. The evidence is for specific strains, at specific doses, in specific populations.
When food beats supplements:
For most people with a reasonably healthy gut, fermented foods provide a broader range of microbial benefit than any single-strain supplement. Kefir, for example, contains dozens of bacterial and yeast strains in a food matrix that supports their survival and colonisation.
When supplements might help:
If you’ve recently completed a course of antibiotics, are dealing with significant stress-related gut symptoms, or have IBS with a mood component, a well-researched probiotic supplement containing L. rhamnosus or B. longum at documented doses may provide a useful short-term boost. The evidence suggests it’s worth trying for 4–8 weeks and assessing the response.
I would be careful with any product making large claims. The numbers matter, and most of the numbers in this space are modest.
Diet Patterns That Support the Gut Brain Axis
Individual foods matter, but diet patterns matter more. The gut-brain axis responds to the overall nutritional environment, not single nutrients in isolation.
The Mediterranean diet has the strongest evidence of any dietary pattern for both gut health and mental wellbeing. It’s high in fiber, anti-inflammatory foods and polyphenols that support gut and brain health, omega-3 fatty acids, and fermented foods, and low in ultra-processed food and refined sugar. Multiple large observational studies and several intervention trials link Mediterranean-style eating to lower rates of depression and better cognitive outcomes [6].
Key dietary elements with gut brain axis support:
- Polyphenol-rich foods — berries, olive oil, dark chocolate (70%+), green tea, and red wine in moderate amounts. Polyphenols are selectively fermented by beneficial gut bacteria, acting as prebiotics.
- Omega-3 fatty acids — fatty fish (salmon, sardines, mackerel), walnuts, and flaxseed. Omega-3s reduce neuroinflammation and support the integrity of the gut lining.
- Diverse plant foods — aim for 30+ different plant foods per week. Each plant species feeds a slightly different bacterial population. Variety is the key driver of microbiome diversity.
- Stable blood sugar — large blood sugar swings affect mood, energy, and gut motility. Whole grains, legumes, and protein at each meal help maintain stability.
- Limiting ultra-processed food — this is not about perfection. It’s about proportion. A diet where ultra-processed food is the exception rather than the norm consistently shows better gut-brain outcomes than one where it’s the baseline.
A sensible starting point is simply asking: does my diet look broadly Mediterranean? More vegetables, legumes, fish, olive oil, and fermented foods; less packaged food, refined sugar, and seed oil-heavy snacks. That single question covers most of the ground.
When Gut-Brain Issues Need a Doctor (Red Flags)
This section matters. The gut-brain axis is a real and useful framework for understanding health, but it is not a reason to self-manage conditions that require professional assessment.
See a doctor or mental health professional if you experience:
- Persistent depression or anxiety that is significantly affecting your daily life — this requires professional assessment, not a probiotic protocol
- Suicidal thoughts or self-harm — contact a mental health professional or crisis service immediately
- Sudden or unexplained personality changes — these can indicate neurological conditions that need investigation
- Cognitive decline — memory loss, confusion, or significant changes in mental function need medical evaluation
- Severe digestive symptoms — blood in stool, unexplained weight loss, persistent pain, or difficulty swallowing
- Mood or cognitive changes following significant gut illness — particularly if they don’t resolve within a few weeks
- Drug or alcohol use affecting both gut and mental health — this requires integrated professional support
The gut-brain axis is a useful lens for understanding the connection between physical and mental health. It is not a substitute for evidence-based psychiatric or medical care. Common sense backed by evidence means knowing which tool to use for which job.
Conclusion
The gut-brain axis is not wellness hype. It is a well-documented, biologically real communication system that influences your mood, cognition, stress response, and sleep in measurable ways. The science is still developing in several areas, but the core mechanisms — the vagus nerve, the microbiome’s neurochemical output, the stress-gut feedback loop — are established enough to inform practical decisions.
Here’s what I’d suggest as a starting point:
- Audit your fiber intake. Most people are significantly under the recommended 25–35g per day. This is the highest-return gut-brain intervention available.
- Add one fermented food daily. Yogurt, kefir, or kimchi — pick what you’ll actually eat consistently.
- Take sleep seriously. Seven or more hours of quality sleep supports both microbiome health and brain function.
- Practice slow breathing daily. Five minutes of slow nasal breathing costs nothing and has measurable effects on vagal tone.
- Reduce ultra-processed food as a proportion of your diet. You don’t need to be perfect — you need to shift the ratio.
- Address chronic stress directly. Exercise, sleep, social connection, and breathing practices are all evidence-supported approaches.
- If you’re considering a probiotic supplement, look for L. rhamnosus or B. longum at documented doses. Give it 4–8 weeks and assess honestly.
- If your symptoms are persistent or severe, see a professional. The gut-brain axis is one piece of a larger picture.
The basics still do the heavy lifting. Start there, stay consistent, and be honest about what’s actually changing. That’s the approach that works.
Frequently Asked Questions
Can probiotics actually improve mood?
Some specific probiotic strains — particularly Lactobacillus rhamnosus and Bifidobacterium longum — have shown modest but real effects on mood and anxiety in clinical trials. The effects are strain-specific and generally modest in magnitude. Generic “mood probiotic” blends with unspecified strains have little supporting evidence. Probiotics work best as part of a broader diet and lifestyle approach, not as standalone mood treatments.
How long does it take to feel a difference?
Microbiome composition can shift within days of dietary changes, but meaningful, stable changes in gut-brain signaling typically take 4–12 weeks of consistent effort. Most probiotic studies showing mood effects run for 4–8 weeks. Vagal tone improvements from breathing practices can be felt within a few weeks of daily practice. There is no quick fix here — but the timeline is not as long as people often assume.
Is the gut really a “second brain”?
In a functional sense, yes. The enteric nervous system contains over 500 million neurons, can operate independently of the central nervous system, and produces the majority of the body’s serotonin [1] [2]. It doesn’t think or reason the way your brain does, but it processes information, responds to its environment, and communicates with your brain continuously. The “second brain” label is a useful shorthand for a genuinely complex system.
Can fixing my gut cure anxiety?
No — and any source telling you otherwise is overstating the evidence. Supporting gut health may reduce anxiety symptoms in some people, particularly where gut dysbiosis is contributing to the anxiety loop. But anxiety disorders have multiple causes and usually require a multi-pronged approach. If your anxiety is significantly affecting your life, a mental health professional is the right starting point, not a gut health protocol.
What about coffee and the gut-brain axis?
Coffee has a complex relationship with the gut-brain axis. It stimulates gut motility (which is why many people need the bathroom shortly after their morning cup), contains polyphenols that feed beneficial gut bacteria, and affects cortisol and adenosine signaling in the brain. Moderate coffee consumption — 2–4 cups per day for most adults — appears broadly neutral to beneficial for gut microbiome diversity in current research. Excessive consumption, or coffee consumed in ways that spike anxiety, may worsen the stress-gut loop for some individuals. Context matters, and individual responses vary considerably.
Do antidepressants affect the microbiome?
Yes — this is an active research area. Several classes of antidepressants, including SSRIs, have been shown to alter gut microbiota composition. Some of these changes may actually contribute to their therapeutic effects, which is consistent with the gut-brain axis model. This does not mean antidepressants are harmful to the gut — it means the gut-brain relationship is relevant to how these medications work. If you are on antidepressants and concerned about gut health, discuss it with your prescribing doctor rather than adjusting your medication based on gut health reasoning alone.






