Gut Health and Digestive Wellness: The Complete Evidence-Based Guide

Last updated: April 8, 2026
In this guide
- What Exactly Is the Gut Microbiome and Why Does It Matter?
- What Are the Signs That Your Gut Health Is Off?
- Which Foods Most Effectively Support Gut Health and Digestive Wellness?
- How Do Lifestyle Habits Affect Gut Health?
- What Is the Gut-Brain Axis and How Does It Affect Mental Health?
- How Do Probiotics and Prebiotics Actually Work?
- What Role Does Gut Health Play in Immunity and Skin Health?
- How Do Antibiotics Affect the Gut Microbiome and What Can You Do About It?
- How Does the Environment Affect Gut Health?
- Step-by-Step: A Practical 4-Week Gut Health Reset
Quick Answer
Your gut is far more than a digestion machine. It houses trillions of microorganisms that regulate your immune system, influence your mood, and affect your sleep quality. Maintaining gut health and digestive wellness comes down to a consistent combination of dietary choices — particularly complete fiber playbook (soluble vs insoluble, daily targets, ramp-up), fermented foods, and diverse plant intake — alongside lifestyle habits like regular movement, quality sleep, and stress management. When those factors fall out of balance, the effects show up across your entire body, not just your stomach.
Key Takeaways
- The human gut contains an estimated 38 trillion microbial cells, roughly equal to the number of human cells in the body (Sender et al., Cell, 2016)
- The gut produces approximately 90% of the body’s serotonin, directly linking digestive health to mood and the gut-brain axis and how your gut shapes mood, anxiety, and mental clarity well-being
- Common signs of gut imbalance include bloating, irregular bowel movements, persistent fatigue, skin flare-ups, anxiety, and disrupted sleep
- Dietary diversity is the single most evidence-supported strategy for building a resilient gut microbiome
- Fermented foods (yogurt, kefir, kimchi, sauerkraut) introduce beneficial live bacteria that can shift microbiome composition within days
- Chronic stress measurably disrupts gut motility and microbial balance via the gut-brain axis
- Antibiotics, while sometimes necessary, can deplete gut bacterial diversity for months — targeted probiotic support during and after a course can help mitigate this
- Environmental factors including water quality, air pollution, and pesticide exposure affect gut microbial health
- Most people can meaningfully improve their digestive wellness within four to eight weeks through dietary and lifestyle changes alone
- Persistent symptoms that don’t respond to dietary changes warrant medical evaluation — conditions like IBS, SIBO, and IBD require clinical diagnosis
What Exactly Is the Gut Microbiome and Why Does It Matter?
The gut microbiome is the collective community of bacteria, viruses, fungi, and other microorganisms living in your gastrointestinal tract, primarily in the large intestine. This isn’t a passive passenger system — it’s an active biological network that shapes your health from the inside out.
Research published in Cell (Sender et al., 2016) estimated that the average adult carries roughly 38 trillion microbial cells. These organisms collectively perform functions your body cannot do alone:
- Fermenting dietary fiber into short-chain fatty acids (SCFAs) like butyrate, which fuel colon cells and reduce inflammation
- Synthesizing vitamins, including B12, K2, and folate
- Training the immune system — approximately 70% of immune tissue is located in the gut wall
- Producing neurotransmitters — the gut synthesizes around 90% of the body’s serotonin and significant amounts of dopamine precursors
- Regulating the gut-brain axis, the bidirectional communication highway between your enteric nervous system and your central nervous system via the vagus nerve
The term “second brain” isn’t metaphorical. The enteric nervous system contains over 500 million neurons — more than the spinal cord. It operates semi-independently and communicates constantly with the brain, which is why anxiety can cause stomach cramps and why gut inflammation can contribute to depression.
Why this matters for you: A disrupted microbiome — called dysbiosis — doesn’t just cause digestive discomfort. It has been associated with conditions ranging from autoimmune disease and obesity to anxiety disorders and cardiovascular risk. Taking care of your gut is, in practical terms, one of the highest-leverage health investments you can make.
What Are the Signs That Your Gut Health Is Off?
Gut imbalance rarely announces itself with a single obvious symptom. More often, it shows up as a cluster of seemingly unrelated issues that persist over weeks or months.
Digestive symptoms
- Bloating, especially after meals
- Constipation (fewer than three bowel movements per week) or loose stools
- Excessive gas or abdominal cramping
- Acid reflux or heartburn that recurs regularly
- Feeling uncomfortably full after small meals
Systemic symptoms
- Chronic fatigue that doesn’t improve with rest — gut dysbiosis impairs nutrient absorption, meaning your body may be running on less fuel even when you eat well
- Skin conditions including acne, eczema, rosacea, and psoriasis — all have documented links to gut inflammation and increased what the science actually says about leaky gut and intestinal permeability (sometimes called “leaky gut”)
- Mood changes — persistent low mood, irritability, or heightened anxiety can reflect disrupted serotonin production in the gut
- Sleep disturbances — the gut produces melatonin precursors, and dysbiosis can interfere with sleep onset and quality
- Frequent illness — if you’re catching every cold that circulates, a compromised gut immune barrier may be a contributing factor
- Food intolerances that seem to be multiplying — a sign the gut lining may be more permeable than it should be
Common mistake: Many people treat these symptoms in isolation — taking antihistamines for skin issues, sleep aids for insomnia, or antacids for reflux — without addressing the gut as a potential root cause. If you have three or more of these symptoms simultaneously, a gut-focused approach is worth exploring before reaching for symptom-specific medications.
When to see a doctor: If you notice blood in your stool, unintentional weight loss, severe abdominal pain, or symptoms that persist beyond four to six weeks despite dietary changes, get a clinical evaluation. These can signal conditions like inflammatory bowel disease (IBD), celiac disease, or colorectal issues that need medical diagnosis.
Which Foods Most Effectively Support Gut Health and Digestive Wellness?
The most gut-supportive diet is one built around variety, fiber, and fermentation. No single superfood repairs the microbiome — diversity is the mechanism.
Fiber: the foundation
Dietary fiber is the primary fuel source for beneficial gut bacteria. When bacteria ferment fiber, they produce short-chain fatty acids that reduce gut inflammation, strengthen the intestinal lining, and support immune function. Most adults in Western countries consume well under the recommended 25–38 grams of fiber per day.
The best fiber sources for gut health:
- Legumes (lentils, black beans, chickpeas) — among the highest fiber-per-serving foods available
- Vegetables — particularly artichokes, leeks, garlic, onions, asparagus, and broccoli, which contain prebiotic fibers that selectively feed beneficial bacteria
- Fruits — apples, pears, berries, and bananas (especially slightly underripe ones, which are high in resistant starch)
- Whole grains — oats, barley, and rye contain beta-glucan, a soluble fiber with strong evidence for gut and cardiovascular benefit
- Nuts and seeds — flaxseed, chia seeds, and almonds provide both fiber and anti-inflammatory fats
For a detailed breakdown of high-fiber options, the complete list of high-fiber foods is a practical starting point.
Fermented foods: live microbial support
Fermented foods introduce live bacteria directly into the gut. A 2021 Stanford study published in Cell found that a high-fermented-food diet increased microbiome diversity and reduced markers of immune activation — effects that a high-fiber diet alone did not produce as quickly.
Effective fermented foods to include regularly:
- Plain yogurt with live cultures — look for “live and active cultures” on the label
- Kefir — a fermented milk drink with a broader range of bacterial strains than yogurt
- Kimchi and sauerkraut — fermented vegetables that also provide fiber and anti-inflammatory compounds
- Miso and tempeh — fermented soy products common in Japanese and Indonesian cuisine
- Kombucha — fermented tea; useful but lower in bacterial diversity than dairy-based ferments
Anti-inflammatory foods
Chronic gut inflammation is a driver of dysbiosis. Foods with documented anti-inflammatory properties help reduce this baseline inflammation. Anti-inflammatory foods worth incorporating regularly include fatty fish (salmon, sardines, mackerel), extra-virgin olive oil, turmeric, ginger, and dark leafy greens.
The health benefits of olive oil extend specifically to the gut — its polyphenols act as prebiotics, feeding beneficial Lactobacillus and Bifidobacterium species.
Foods to limit
- Ultra-processed foods — emulsifiers like carboxymethylcellulose and polysorbate-80, found in many packaged foods, have been shown in animal studies to disrupt the gut mucus layer
- Excess added sugar — feeds opportunistic bacteria and yeast like Candida, which can crowd out beneficial species
- Alcohol — even moderate intake increases intestinal permeability and alters microbial composition
- Artificial sweeteners — some research suggests saccharin and sucralose may negatively affect microbial diversity, though evidence in humans is still developing
Decision rule: If you’re starting from scratch, prioritize adding before subtracting. Add one serving of fermented food and two additional servings of vegetables per day for two weeks before worrying about elimination. Most people see noticeable digestive improvement from addition alone.
How Do Lifestyle Habits Affect Gut Health?

Diet is the biggest lever, but it doesn’t operate in isolation. Several lifestyle factors have direct, measurable effects on gut microbial composition and digestive function.
Exercise
Regular physical activity increases microbial diversity and promotes the production of butyrate-producing bacteria. A 2019 study in the British Journal of Sports Medicine found that athletes had significantly more diverse gut microbiomes than sedentary controls, even when diet was accounted for. You don’t need elite fitness levels — consistent moderate activity (brisk walking, cycling, swimming) appears sufficient to produce microbiome benefits.
For practical guidance, the exercise guide for better health covers how to build sustainable movement habits from any starting point.
Sleep
The gut microbiome follows circadian rhythms. Disrupted sleep — whether from shift work, chronic late nights, or poor sleep quality — alters microbial composition and reduces the diversity of beneficial species. Conversely, gut dysbiosis disrupts melatonin precursor production, creating a feedback loop that makes sleep worse. Aim for seven to nine hours of consistent sleep, with a regular sleep and wake time, to support both gut and systemic health.
Stress management
The gut-brain axis means that psychological stress has direct physiological effects on the gut. Acute stress accelerates gut motility (causing diarrhea in some people). Chronic stress slows motility, reduces mucus production, and increases intestinal permeability. Cortisol, the primary stress hormone, directly suppresses the growth of beneficial Lactobacillus species.
Practical stress-reduction approaches with documented gut benefits:
- Diaphragmatic breathing — activates the parasympathetic nervous system, which governs “rest and digest” function
- Mindfulness meditation — even 10 minutes daily has been shown to reduce cortisol and improve IBS symptoms in clinical trials
- Yoga — combines movement, breathwork, and stress reduction; several small trials show improvement in gut motility and symptom scores for IBS patients
Hydration
Water is essential for gut motility. Dehydration is one of the most common and easily corrected causes of constipation. The gut lining also requires adequate hydration to maintain its mucus layer, which protects against pathogens and supports microbial balance. Aim for consistent fluid intake throughout the day — the specific target varies by body size, activity, and climate, but pale yellow urine is a reliable practical indicator of adequate hydration.
If you’re looking for natural approaches to digestive discomfort, 10 ways to soothe your stomach naturally covers evidence-supported remedies including ginger, peppermint, and warm fluids.
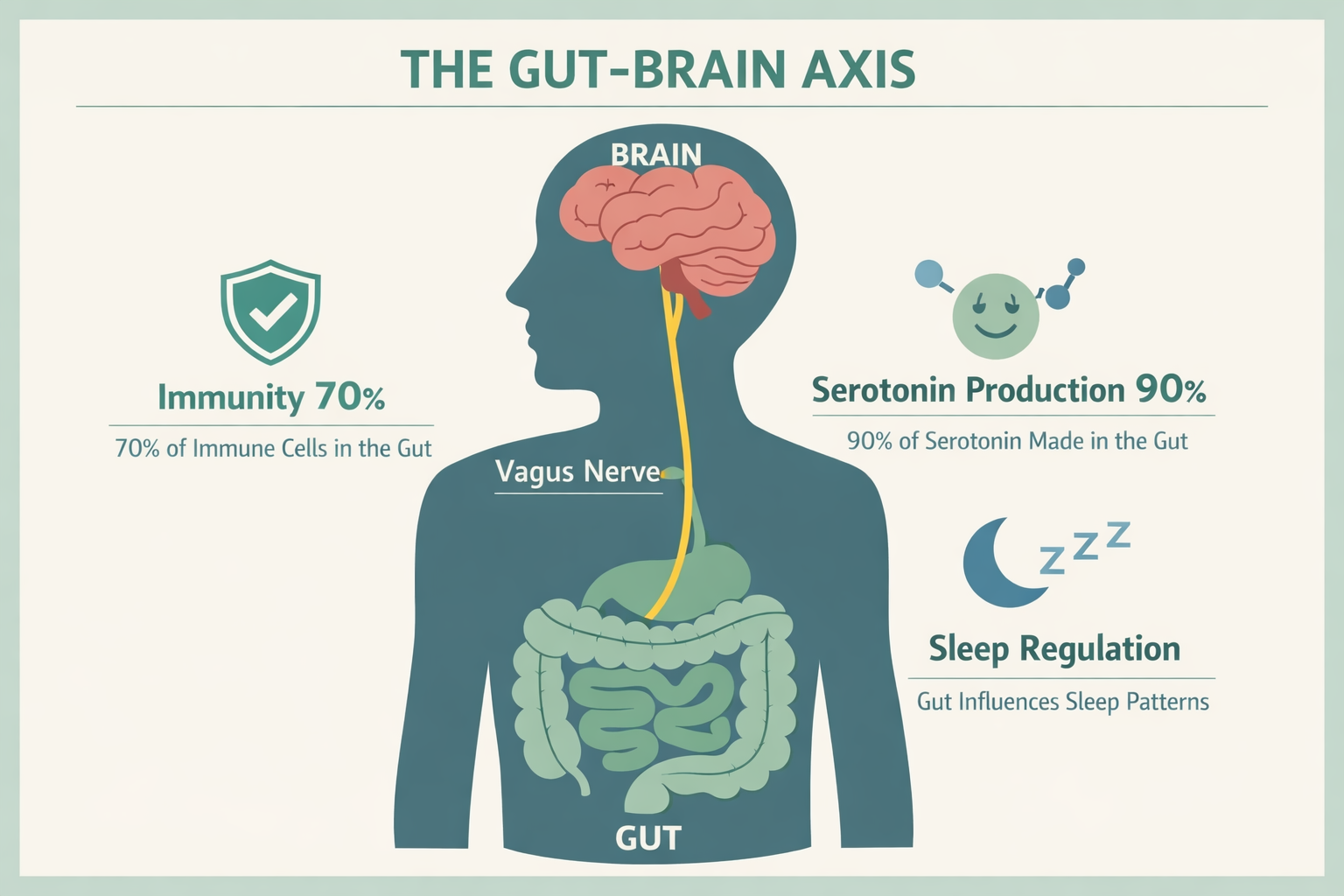
What Is the Gut-Brain Axis and How Does It Affect Mental Health?
The gut-brain axis is the two-way communication system connecting the central nervous system (brain and spinal cord) with the enteric nervous system (the gut’s own neural network). This connection runs primarily through the vagus nerve, and it carries signals in both directions — meaning the gut influences the brain just as much as the brain influences the gut.
How gut health affects mood
- The gut produces roughly 90% of the body’s serotonin. Low serotonin is associated with depression and anxiety. Gut dysbiosis can impair serotonin synthesis, contributing to mood disorders through a pathway that has nothing to do with brain chemistry directly.
- Gut bacteria produce gamma-aminobutyric acid (GABA), a neurotransmitter that reduces anxiety. Certain Lactobacillus and Bifidobacterium strains are particularly active GABA producers.
- Gut inflammation generates pro-inflammatory cytokines that cross the blood-brain barrier and contribute to neuroinflammation — a mechanism increasingly studied in depression research.
The microbiome-mental health connection in practice
Several clinical trials have tested probiotic supplementation in people with depression and anxiety. A 2019 meta-analysis in General Psychiatry found that both probiotic and prebiotic interventions produced statistically significant reductions in depression and anxiety scores compared to placebo. The effect sizes were modest but consistent.
This doesn’t mean probiotics replace therapy or medication. But it does mean that gut health is a legitimate, underutilized component of mental wellness — one that dietary changes can influence within weeks.
Edge case: The gut-brain connection also runs in reverse. People with anxiety disorders frequently experience IBS-like symptoms even without underlying gut pathology. In these cases, treating the anxiety (through therapy, medication, or stress reduction) often resolves the gut symptoms. The direction of causation matters for treatment planning, which is why persistent symptoms warrant professional evaluation.
How Do Probiotics and Prebiotics Actually Work?
Probiotics and prebiotics are frequently mentioned together but serve different functions. Understanding the distinction helps you use both more effectively.
Probiotics
Probiotics are live microorganisms that, when consumed in adequate amounts, confer a health benefit. They work by:
- Temporarily colonizing the gut and competing with pathogenic bacteria for space and nutrients
- Producing antimicrobial compounds (bacteriocins) that suppress harmful bacteria
- Modulating immune responses in the gut lining
- Producing short-chain fatty acids and neurotransmitter precursors
Important caveat: Most probiotic strains are transient — they don’t permanently colonize the gut. This is why consistent intake matters more than occasional supplementation. Food-based probiotics (yogurt, kefir, kimchi) tend to be more effective than supplements for most healthy adults because they come packaged with other nutrients that support bacterial survival.
Strain specificity matters. Lactobacillus rhamnosus GG has strong evidence for antibiotic-associated diarrhea. Bifidobacterium longum has evidence for anxiety reduction. A generic “probiotic blend” may not deliver the specific strain you need for a specific condition.
Prebiotics
Prebiotics are non-digestible food components — primarily specific types of fiber — that selectively stimulate the growth of beneficial gut bacteria. They’re the food that probiotics eat.
Key prebiotic compounds and their sources:
| Prebiotic Type | Food Sources | Primary Bacterial Benefit |
|---|---|---|
| Inulin / FOS | Garlic, onion, leeks, chicory root | Feeds Bifidobacterium |
| Resistant starch | Unripe bananas, cooked-and-cooled rice/potatoes | Feeds butyrate producers |
| Beta-glucan | Oats, barley, rye | Broad microbial diversity |
| Pectin | Apples, citrus peel, carrots | Feeds Akkermansia muciniphila |
| Arabinoxylan | Wheat bran, psyllium husk | Increases Bifidobacterium and Lactobacillus |
Practical note: Increasing prebiotic intake too quickly causes gas and bloating as bacteria ferment the new substrate. Introduce high-prebiotic foods gradually over two to three weeks to allow the microbiome to adapt. For a deep dive into this, see our full guide on bloating: causes, types, and how to fix it.
What Role Does Gut Health Play in Immunity and Skin Health?
Approximately 70% of the body’s immune tissue — called gut-associated lymphoid tissue (GALT) — lines the gastrointestinal tract. This makes the gut the largest immune organ in the body, not a secondary one.
Gut health and immunity
The gut microbiome trains immune cells to distinguish between harmless substances and genuine threats. When microbial diversity is low, this calibration breaks down, contributing to:
- Increased susceptibility to infections — beneficial bacteria compete with pathogens and produce antimicrobial compounds
- Autoimmune conditions — dysbiosis is associated with conditions including rheumatoid arthritis, type 1 diabetes, and multiple sclerosis, though causality is still being established
- Allergies and food sensitivities — a poorly calibrated immune system may overreact to harmless food proteins
The gut-skin connection
The gut-skin axis is a well-documented but underappreciated relationship. Skin conditions including acne, eczema (atopic dermatitis), rosacea, and psoriasis all show associations with gut dysbiosis and increased intestinal permeability.
The mechanism works like this: when the gut lining becomes more permeable than it should be, bacterial fragments and metabolic byproducts enter the bloodstream. The immune system responds with systemic inflammation, which can manifest in the skin as flare-ups, redness, and breakouts.
A 2022 review in the Journal of Clinical Medicine found that patients with moderate-to-severe acne had significantly lower gut microbial diversity and higher levels of inflammatory markers than clear-skinned controls. Probiotic supplementation reduced acne severity in several small trials, though larger studies are needed.
Practical takeaway: If you’re dealing with persistent skin issues that don’t respond fully to topical treatments, addressing gut health is a logical next step — not an alternative to dermatological care, but a complementary approach worth exploring.
How Do Antibiotics Affect the Gut Microbiome and What Can You Do About It?

Antibiotics are sometimes necessary and genuinely life-saving. But their effect on the gut microbiome is significant and often underestimated.
A single course of broad-spectrum antibiotics can reduce gut microbial diversity by 25–50%, with some studies showing that full recovery takes six months to two years — and in some individuals, certain species never fully return (Dethlefsen & Relman, Science, 2011).
This matters because antibiotic-associated disruption increases susceptibility to:
- Clostridioides difficile (C. diff) infection — a serious gut infection that can occur when protective bacteria are depleted
- Antibiotic-associated diarrhea, which affects an estimated 5–35% of antibiotic users depending on the drug class
- Post-antibiotic gut symptoms including bloating, altered motility, and increased food sensitivities
What to do during and after a course of antibiotics
- Take probiotics — specifically Lactobacillus rhamnosus GG or Saccharomyces boulardii, both of which have strong evidence for reducing antibiotic-associated diarrhea. Take them two hours apart from the antibiotic dose so the antibiotic doesn’t kill the probiotic before it reaches the gut.
- Eat fermented foods consistently throughout the course and for at least four weeks after
- Increase prebiotic intake — feed the surviving bacteria to help them repopulate faster
- Avoid unnecessary antibiotics — if your doctor says a viral infection doesn’t require antibiotics, trust that assessment; unnecessary courses cause microbiome damage without benefit
- Be patient — microbiome recovery is real but takes time; don’t expect full restoration in two weeks
How Does the Environment Affect Gut Health?
The gut microbiome doesn’t exist in isolation from the external world. Environmental factors including air quality, water purity, chemical exposures, and even where you live all influence microbial composition.
Key environmental influences
- Pesticide exposure — glyphosate, one of the most widely used herbicides globally, has been shown in animal studies to disrupt gut bacterial balance by inhibiting the shikimate pathway used by many beneficial bacteria. Human evidence is still developing, but choosing organic produce for the highest-pesticide crops (the “dirty dozen” list) is a reasonable precaution.
- Air pollution — particulate matter inhaled from polluted air can be swallowed and reach the gut, where it may alter microbial composition. Urban residents consistently show lower gut microbial diversity than rural populations in comparative studies.
- Chlorinated water — chlorine in tap water is designed to kill bacteria, and it doesn’t fully discriminate between pathogens and beneficial microbes. Filtered water is a simple mitigation strategy.
- Antibiotic residues in food — trace antibiotics in conventionally raised meat and poultry may contribute to cumulative microbiome disruption over time. Choosing antibiotic-free or organic animal products where budget allows reduces this exposure.
- Nature exposure — contact with natural environments introduces microbial diversity through soil, plants, and outdoor air. Research on the “old friends hypothesis” suggests that reduced exposure to environmental microbes in modern urban life contributes to immune dysregulation and reduced gut diversity.
The relationship between environment and gut health reinforces a broader point: digestive wellness isn’t achieved through diet alone. It’s shaped by the totality of your daily exposures and choices.
Step-by-Step: A Practical 4-Week Gut Health Reset
If you want a structured starting point rather than a list of general advice, this four-week framework builds habits progressively without overwhelming your system.
Week 1: Add fiber and water
- Increase vegetable intake by two servings per day (any vegetables you enjoy)
- Add one serving of legumes (lentils, chickpeas, or beans) three times per week
- Drink an additional two glasses of water per day
- Don’t change anything else yet
Week 2: Introduce fermented foods
- Add one serving of plain yogurt or kefir daily
- Introduce one other fermented food (kimchi, sauerkraut, or miso) two to three times per week
- Note any digestive changes — some initial gas is normal and typically resolves within a week
Week 3: Address lifestyle factors
- Commit to 20–30 minutes of moderate physical activity at least four days per week
- Establish a consistent sleep schedule (same bedtime and wake time, including weekends)
- Practice five to ten minutes of diaphragmatic breathing or mindfulness daily
Week 4: Reduce gut disruptors
- Cut ultra-processed snack foods to no more than once per day
- Reduce alcohol to no more than one drink per day if you currently drink more
- Swap refined grains for whole grain alternatives in at least two meals per day
By the end of four weeks, most people report improvements in bloating, energy, bowel regularity, and sleep quality. These aren’t dramatic overnight changes — they’re the compound effect of consistent, small adjustments.
Frequently Asked Questions About Gut Health and Digestive Wellness
How long does it take to improve gut health?
Measurable changes in microbial composition can occur within three to five days of dietary changes, according to research from Stanford. Symptom improvements typically take two to four weeks of consistent effort. Significant microbiome restructuring takes three to six months.
Can stress alone cause gut problems, even with a good diet?
Yes. Chronic psychological stress elevates cortisol, which suppresses beneficial bacteria, increases intestinal permeability, and alters gut motility. Diet helps, but stress management is a non-negotiable component of gut health — not optional.
Are probiotic supplements worth taking?
For healthy adults without specific conditions, food-based probiotics (fermented foods) are generally more effective and less expensive than supplements. Supplements are worth considering during and after antibiotic use, for IBS management, or when fermented foods aren’t accessible. Strain specificity matters — choose products with documented clinical evidence for your specific concern.
What is leaky gut and is it a real medical condition?
Increased intestinal permeability — colloquially called “leaky gut” — is a real and measurable phenomenon. The gut lining becomes more permeable than normal, allowing bacterial fragments and food particles to enter the bloodstream and trigger immune responses. It’s associated with IBD, celiac disease, and chronic stress. However, “leaky gut syndrome” as a broad diagnosis for vague symptoms is not a recognized clinical diagnosis, and some practitioners overuse the term.
Does coffee affect gut health?
Coffee has a complex relationship with the gut. It stimulates gut motility (which is why many people need the bathroom after their morning cup) and contains polyphenols that act as prebiotics. Moderate consumption (two to three cups per day) appears neutral to beneficial for most people. Excessive intake or coffee on an empty stomach can worsen acid reflux and gut sensitivity in some individuals.
Can children’s gut health be supported the same way as adults?
The principles are similar — dietary diversity, fermented foods, fiber, and reduced ultra-processed food intake — but children’s microbiomes are still developing and more responsive to intervention. Unnecessary antibiotic use in childhood has particularly significant long-term effects on microbiome development. Consult a pediatrician before giving children probiotic supplements.
Is intermittent fasting good for gut health?
There’s emerging evidence that time-restricted eating supports the gut microbiome’s circadian rhythms and may increase microbial diversity. However, the evidence is still preliminary. For people with existing gut conditions, extended fasting windows can sometimes worsen symptoms. It’s worth exploring if you’re interested, but it’s not a required component of gut health.
What’s the difference between IBS and IBD?
IBS (irritable bowel syndrome) is a functional disorder — the gut works abnormally but shows no structural damage on imaging or biopsy. IBD (inflammatory bowel disease, including Crohn’s disease and ulcerative colitis) involves actual inflammation and tissue damage in the gut wall. Both require medical diagnosis and management, but their treatments differ significantly.
How does aging affect gut health?
Gut microbial diversity typically declines with age, partly due to reduced dietary variety, decreased physical activity, and more frequent medication use. Older adults benefit particularly from consistent prebiotic and probiotic food intake, adequate hydration, and regular movement to maintain gut motility.
Can gut health affect weight management?
Yes. Gut bacteria influence how efficiently calories are extracted from food, how hunger hormones (ghrelin and leptin) are regulated, and how fat is stored. People with higher gut microbial diversity tend to have healthier body weight profiles. However, gut health is one factor among many — it doesn’t override caloric balance, but it does influence it.
Related Reading
- Anti-inflammatory foods: the ultimate guide
- High-fiber foods: the complete list, benefits, and how much you need
- 10 ways to soothe your stomach naturally
- Healthy choice meals
Sources
Sender, R., Fuchs, S., & Milo, R. (2016). Revised Estimates for the Number of Human and Bacteria Cells in the Body. PLOS Biology, 14(8), e1002533.
https://pubmed.ncbi.nlm.nih.gov/27541692/
Sonnenburg, J. et al. Gut-microbiota-targeted diets modulate human immune status. Cell, 184(16), 4137–4153.e14, 2021.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9020749/
Dethlefsen, L., & Relman, D.A. (2011). Incomplete recovery and individualized responses of the human distal gut microbiota to repeated antibiotic perturbation. PNAS, 108(Suppl 1), 4554–4561.
https://pubmed.ncbi.nlm.nih.gov/20847294/
Related Reading
- How to Soothe Your Stomach Naturally: 10 Evidence-Based Remedies That Work
- Foods that are anti-inflammatory
- Explore how to Revamp your Digestion: Complete guide to bland food diets for optimal health.
- Bland Diet Breakfast: 15 Satisfying Recipes That Won’t Upset Your Stomach
- 6 Best Bland Diet Recipes for Digestive Recovery (2026)
- Anti-Inflammatory Foods and Diets: Ultimate Guide
- The Comprehensive Guide to Modern Diets: What Actually Works in 2026
- Health Benefits of Natural Foods and Herbs






