Modern Food Processing and Gut Health: How Processed Food Affects Gut Chemistry

Last updated: May 16, 2026
Quick Answer: Modern food processing changes the chemistry, structure, and speed of what reaches your gut — not just the calorie count. Ultra-processed foods tend to be low in fermentable fiber, high in refined ingredients, and may contain additives that interact with gut microbes. The evidence suggests this pattern is associated with reduced microbial diversity and gut health concerns, though not every processed food carries the same risk. The goal is not to fear every packaged item, but to understand which foods give your gut more useful chemistry — and which ones crowd that chemistry out.
Key Takeaways
- Your gut responds to food chemistry, not nutrition labels. Fiber, food structure, digestion speed, and microbial fuel matter as much as calories.
- Not all processed food is harmful. Yogurt, canned beans, frozen vegetables, and oats are processed — and they can support gut health.
- Ultra-processed foods (UPFs) are a specific concern. They are industrially formulated with refined ingredients, additives, and little intact fiber.
- Recent CDC/NCHS data suggests adults in the U.S. get roughly 53% of their daily calories from ultra-processed foods — making this a food environment issue, not just a personal choice.
- Fiber is your gut microbiome’s main fuel. When processing removes fiber, it reduces the raw material for short-chain fatty acid production.
- Short-chain fatty acids (SCFAs) — particularly butyrate — are associated with gut barrier support, immune signaling, and inflammation regulation.
- Some emulsifiers and artificial sweeteners may influence gut microbiota, but much of the evidence is preclinical or early-stage human research. Caution is warranted, not panic.
- The strongest practical move is adding fiber-rich, whole-food ingredients to your regular diet — not eliminating every packaged food.
- Persistent digestive symptoms — blood in stool, unexplained weight loss, severe pain, or new symptoms after 50 — should be discussed with a clinician.
- Context matters. The issue is repeated dietary patterns, not a single ingredient or occasional meal.
In this guide
- What Does "Modern Food Processing" Actually Mean?
- Gut Chemistry 101: What Happens After You Eat?
- How Processing Changes the Food Before It Reaches Your Gut
- How Processed Food Affects Gut Health: What the Evidence Suggests
- Food Additives, Emulsifiers, and Sweeteners: What Should Readers Know?
- The Fiber Problem: Modern Processing Often Removes Your Gut's Main Fuel
- Satiety, Eating Speed, and Metabolism: Why Food Texture Matters
- The Gut Barrier, Mucus Layer, and Inflammation: What to Explain Carefully
- The Modern Food Environment: It Is Not Just Individual Willpower
- How to Build a Gut-Friendlier Diet Without Going Extreme
- What to Eat More Often for Better Gut Chemistry
- Who Should Be More Careful With Gut Health Advice?
- Conclusion: What to Do With This Information
- Frequently Asked Questions
What Does “Modern Food Processing” Actually Mean?
Modern food processing covers a wide range of techniques — from simple preservation to complex industrial formulation. The distinction that matters most for gut health is not whether food is processed, but how extensively it has been altered and what that alteration removes or adds.
Processing is not automatically bad
Let’s keep this practical. Many foods we eat regularly are processed in some way, and that is not a problem. Consider:
- Yogurt — fermented milk, often beneficial for gut bacteria
- Canned beans — heat-processed for safety, still fiber-rich
- Frozen vegetables — blanched and frozen, largely nutritious
- Oats — rolled or steel-cut, still intact whole grain
- Pasteurized milk — heat-treated for safety
- Olive oil — pressed and filtered, rich in polyphenols
- Sourdough bread — fermented, with altered starch structure
These foods have been processed. They are also, in most cases, reasonable choices for gut health. The idea that “natural” automatically means safer or healthier does not hold up. Raw milk carries pathogens. Wild mushrooms can be toxic. Processing, at its core, exists to make food safer, more digestible, more affordable, and more shelf-stable.
The real concern is ultra-processing
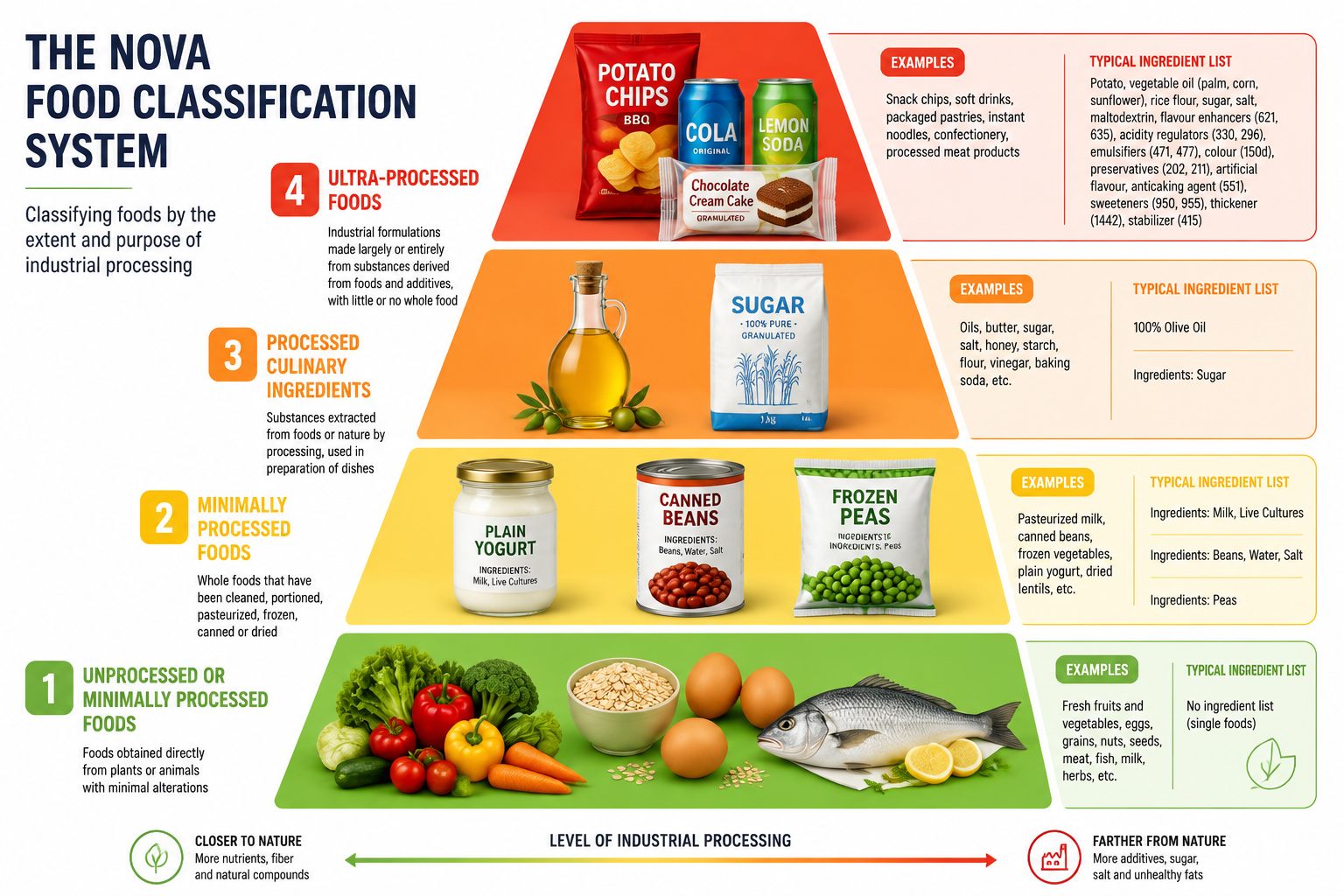
Here is the real issue. Ultra-processed foods are a different category. The NOVA classification system — developed by researchers at the University of São Paulo — defines them as industrial formulations made largely from refined or extracted food substances, combined with additives not typically used in home cooking. These include:
- Hydrogenated oils and interesterified fats
- High-fructose corn syrup and other refined sweeteners
- Protein isolates and hydrolysates
- Emulsifiers, stabilizers, and thickeners
- Artificial and “nature-identical” flavorings
- Colorings, humectants, and preservatives
Common examples most readers will recognize:
| Category | Examples |
|---|---|
| Soft drinks | Cola, sweetened fruit drinks, energy drinks |
| Packaged snacks | Chips, crackers, flavored popcorn |
| Sweetened cereals | Many breakfast cereals marketed to adults and children |
| Packaged pastries | Muffins, cookies, cakes with extended shelf life |
| Instant noodles | Ramen packets, cup noodles |
| Fast food items | Chicken nuggets, processed burger patties |
| Shelf-stable snack bars | Many flavored protein or granola bars |
| Sweetened dairy desserts | Flavored yogurt cups, pudding snacks |
The NOVA system is a useful framework, not a perfect one. Some foods land in ambiguous territory. But as a starting point, it helps readers see the difference between a food that has been minimally altered and one that has been industrially reformulated.
A practical way to tell the difference
Ask yourself three questions:
- Could you make something similar in a home kitchen with recognizable ingredients?
- Does it contain intact food components, or mostly refined fractions of food?
- Is it designed to be shelf-stable, hyper-palatable, and easy to overeat?
If the answer to questions 2 and 3 is yes, you are likely looking at an ultra-processed product. That does not mean you can never eat it. It means it is worth knowing what it is.
Gut Chemistry 101: What Happens After You Eat?
Your gut is not a passive tube. It is a chemically active environment where food structure, microbial populations, and metabolic signals interact continuously. Understanding the basics makes the rest of this article much easier to apply.
Digestion starts before food reaches your gut microbes
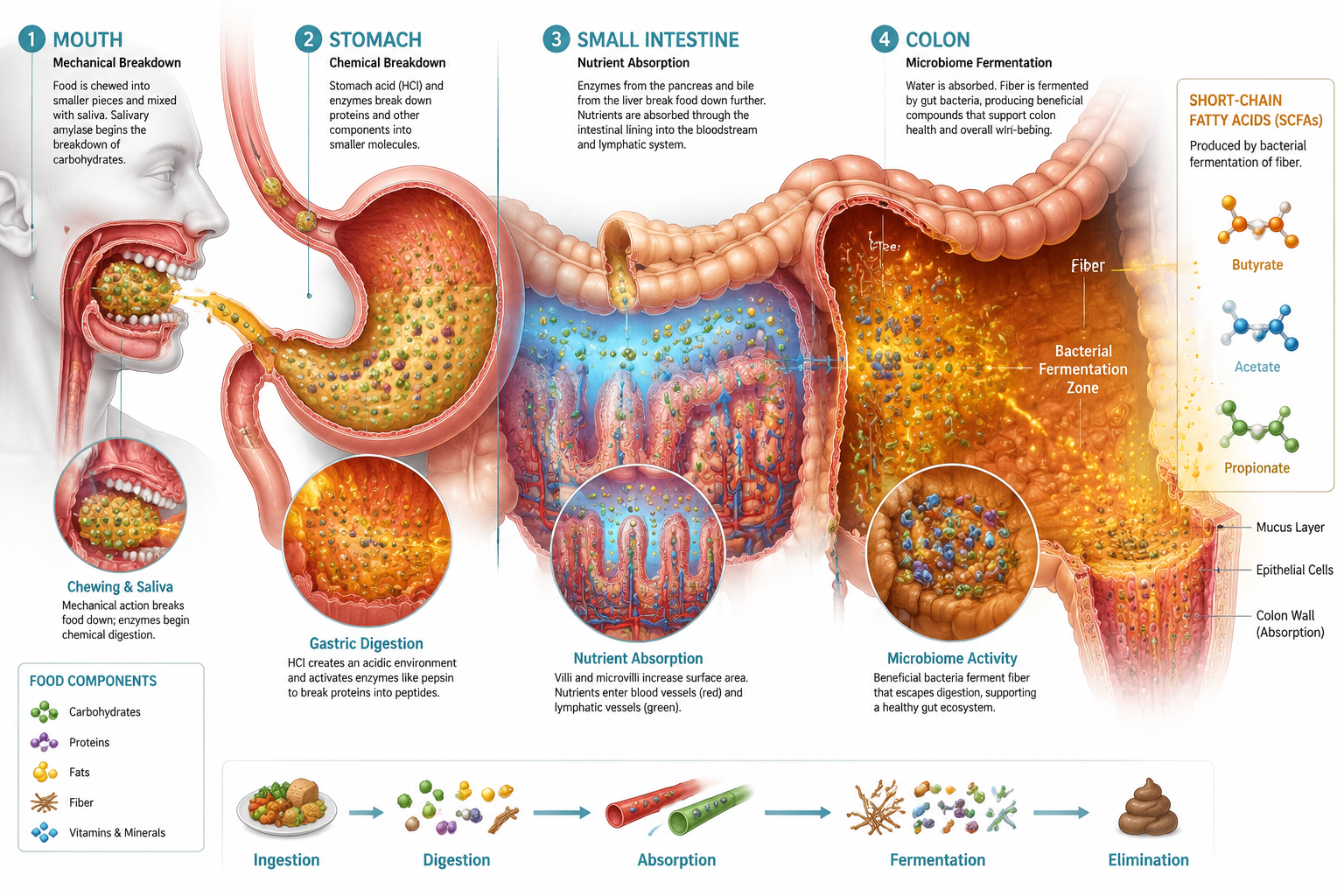
The process begins in the mouth. Chewing breaks food into smaller particles and mixes it with saliva, which contains enzymes that start breaking down starches. From there:
- The stomach uses acid and enzymes to break down proteins and continue starch digestion.
- The small intestine is where most sugars, amino acids, fats, vitamins, and minerals are absorbed into the bloodstream.
- Bile from the liver helps emulsify and absorb dietary fats.
- The colon is where the story gets interesting for gut health.
Your microbiome feeds on what you do not fully digest
By the time food reaches the colon, most easily digestible components have already been absorbed. What arrives in the colon are the materials that escaped earlier digestion: dietary fibers, resistant starches, some polyphenols, and certain proteins.
This is where your gut microbiome — the trillions of bacteria, fungi, and other microorganisms living in your digestive tract — gets to work. They ferment these materials and produce compounds called short-chain fatty acids (SCFAs), primarily:
- Butyrate — the main energy source for colonocytes (the cells lining your colon), and commonly discussed in relation to gut barrier function
- Propionate — transported to the liver and involved in metabolic signaling
- Acetate — the most abundant SCFA, used by peripheral tissues and involved in appetite signaling
In plain English: fiber is not just roughage. It is raw material for gut chemistry. The microbiome uses it to produce compounds that influence the gut lining, immune function, and metabolic signaling throughout the body.
“Fiber is not just roughage. It is raw material for gut chemistry.”
Why the colon matters
Here is the part that connects directly to modern food processing. Many highly refined foods — white bread, sugary drinks, refined crackers, sweetened cereals — are absorbed rapidly in the small intestine. They arrive in the colon with very little fermentable material left.
The microbiome, starved of its preferred fuel, may shift its composition over time. The issue is not one meal. It is the repeated pattern of a diet that consistently delivers little to the colon. That pattern, sustained over weeks and months, is what the research on ultra-processed foods and gut health is really examining.
How Processing Changes the Food Before It Reaches Your Gut
Processing can alter food in ways that go well beyond changing its calorie count. The physical structure, fiber content, digestion speed, and additive load all change — and your gut responds to all of them.
Processing can break the food matrix
The “food matrix” refers to the physical structure of food: its cell walls, fiber networks, water distribution, fat arrangement, and particle size. This structure matters because it affects how quickly food is digested and what reaches the colon.
Consider almonds as a straightforward example:
- Whole almonds — cell walls slow digestion; some fat and protein pass to the colon
- Almond flour — cell walls broken down; faster digestion, less material reaches the colon
- Almond oil — essentially pure fat; no fiber, no fermentable material
The same food, processed three different ways, behaves very differently in the digestive tract. The same principle applies to oats. Whole rolled oats and sweetened instant oat cereal may both contain oats, but they can differ substantially in texture, sugar content, fiber integrity, and digestion speed.
Processing can remove or dilute fiber
Refining grains removes the bran and germ — the fiber-rich parts — leaving primarily the starchy endosperm. Juicing removes much of the intact fiber structure of fruit, delivering sugar and some micronutrients but little of the fermentable material that would have reached the colon. Many packaged foods are energy-dense but fiber-poor.
The practical consequence: less fermentable material arriving in the colon means less fuel for beneficial microbial activity. This is one of the clearest and most consistent mechanisms linking processed food patterns to gut microbiome changes.
Processing can make food easier to eat quickly
Soft textures, refined starches, liquid calories, and engineered flavor combinations reduce chewing time and can accelerate eating speed. This matters because:
- Satiety signals from the gut take time to reach the brain (roughly 15–20 minutes after eating begins)
- Faster eating may mean more food consumed before those signals register
- Highly palatable foods — engineered to hit precise combinations of salt, fat, and sweetness — can make portion awareness harder
This is not about willpower. It is about how food engineering interacts with human biology.
Processing can introduce additives that change texture, stability, or sweetness
Emulsifiers keep oil and water mixed. Stabilizers improve texture and mouthfeel. Preservatives extend shelf life. Non-nutritive sweeteners provide sweetness without sugar calories. These ingredients are not automatically harmful, but they are relevant to gut chemistry research — and that research is still developing.
The FDA defines a food additive as any substance whose intended use may reasonably be expected to become a component of food or otherwise affect its characteristics. Direct additives are generally identified on ingredient labels, which is why reading labels matters.
How Processed Food Affects Gut Health: What the Evidence Suggests
The evidence linking ultra-processed food patterns to gut health concerns is growing, but it is largely observational. Associations are real and worth taking seriously. Definitive causal proof in humans is still limited.
What research links UPFs with
A 2024 review in Nature Reviews Gastroenterology & Hepatology reported increasing evidence of an association between UPF-rich diets and gut diseases, including inflammatory bowel disease (IBD), colorectal cancer, and irritable bowel syndrome (IBS). The review also emphasized that causal evidence is challenging to establish and that human intervention studies remain limited.
The associations researchers have identified include:
- Changes in gut microbiome composition — reduced diversity, shifts in bacterial populations
- Lower overall diet quality — less fiber, more refined carbohydrates, more added sugars
- Possible links with intestinal permeability — the integrity of the gut barrier
- Inflammatory markers — some studies suggest associations with low-grade systemic inflammation
- Colorectal cancer risk — observational associations, not proven causation
The numbers matter here. When more than half of U.S. adult calories come from ultra-processed foods — as recent CDC/NCHS data suggests — even modest per-person effects translate into a significant population-level concern.
Why the microbiome may respond differently to ultra-processed foods
The mechanisms being studied include:
- Less fermentable fiber reaching the colon — reducing SCFA production
- More refined ingredients absorbed early — leaving little for microbial fermentation
- Additives potentially interacting with microbes or the mucus layer — still being studied
- Altered eating patterns — faster eating, larger portions, reduced meal variety
None of these mechanisms work in isolation. The gut microbiome is shaped by the cumulative pattern of what you eat over time, not by any single food or ingredient.
Why “all processed food is bad” is the wrong takeaway
We need to separate fact from hype here. Frozen vegetables, canned beans, plain yogurt, and minimally processed grains can all support a healthy diet. The issue is the overall pattern — specifically, whether ultra-processed foods are displacing fiber-rich, whole-food options as the dietary default.
A useful question to ask is not “Is this food processed?” but “What is this food replacing in my diet?”
Food Additives, Emulsifiers, and Sweeteners: What Should Readers Know?
Additives are a legitimate area of scientific interest, but the evidence is more nuanced than most popular coverage suggests. Let’s call it what it is: interesting, early-stage, and not yet grounds for panic.
Why additives are used
Additives serve real functions in food manufacturing:
- Emulsifiers — keep oil and water mixed (mayonnaise, salad dressings, ice cream)
- Stabilizers — maintain texture and prevent separation
- Preservatives — extend shelf life and reduce spoilage
- Humectants — retain moisture in baked goods
- Colorings — maintain or add visual appeal
- Flavorings — enhance or standardize taste
- Thickeners and gums — improve mouthfeel in low-fat products
These are not arbitrary additions. They solve real manufacturing problems. The question is whether some of them — at the doses and frequencies found in modern diets — may have unintended effects on gut biology.
Emulsifiers and gut barrier questions
Emulsifiers are among the most studied additives in gut health research. Common examples include polysorbate 80, carboxymethylcellulose (CMC), lecithins (from soy or sunflower), mono- and diglycerides, and various gums (xanthan, guar, carrageenan).
The 2024 Nature Reviews Gastroenterology & Hepatology review notes that some additives commonly found in UPFs — including emulsifiers, sweeteners, colors, and microparticles — have been shown to affect outcomes such as the gut microbiome, intestinal permeability, and intestinal inflammation. Importantly, the review also emphasizes that much of this additive-specific evidence comes from preclinical studies (cell cultures and animal models), and human relevance is still being established.
I would be careful with that — meaning: take the preclinical findings seriously enough to stay informed, but do not conclude that a product containing lecithin is equivalent to consuming a gut irritant. The dose, the specific additive, the individual’s microbiome, and the overall dietary context all matter.
Artificial sweeteners and microbiome uncertainty
Non-nutritive sweeteners — including saccharin, sucralose, aspartame, acesulfame-K, and stevia — are used widely in diet beverages, sugar-free products, and reduced-calorie foods. They were developed to provide sweetness without the caloric and blood sugar impact of sugar.
A study published in Nature Medicine reported that non-nutritive sweeteners were shown to disrupt the gut microbiome of healthy people and impair glucose tolerance in some individuals, though effects varied by sweetener type and by person. This is worth noting — but it is also a single study in a specific population, and the field is still developing.
The practical takeaway is not “never use sweeteners.” It is:
- Effects appear to vary by sweetener type and individual microbiome
- Personalized response is real — what affects one person may not affect another
- Replacing sugar with sweeteners does not automatically improve gut health
- The overall dietary pattern still matters more than any single ingredient
The practical reader takeaway
Do not panic over one ingredient. Look at the whole pattern: how often, how much, and what foods are being displaced? A product that contains a small amount of xanthan gum alongside high fiber and whole-food ingredients is a different situation from a daily diet built around multiple ultra-processed foods combining low fiber, high sweetness, refined starches, added fats, and a long list of additives.
The basics still do the heavy lifting. A diet rich in fermentable fiber, diverse plants, and minimally processed staples gives the gut microbiome what it needs — and that foundation matters far more than avoiding any single additive.
The Fiber Problem: Modern Processing Often Removes Your Gut’s Main Fuel
Fiber is the single most important dietary factor for gut microbiome health, and modern food processing frequently removes it. This is not a secondary concern — it is the central mechanism connecting processed food patterns to gut health outcomes.
Fiber is chemistry, not just bowel regularity
Most people think of fiber as something that keeps digestion moving. That is true, but it undersells what fiber actually does:
- Fermentable fibers (fructooligosaccharides, inulin, pectin, beta-glucan) feed specific beneficial bacterial populations
- Resistant starch (found in cooked and cooled potatoes, rice, and legumes) ferments slowly in the colon, producing butyrate
- Diverse plant fibers support a more diverse microbiome — and diversity is generally associated with better gut health outcomes
- Soluble fiber (oats, beans, apples) forms a gel that slows digestion and feeds microbes
- Insoluble fiber (wheat bran, vegetables) adds bulk and supports transit time
The evidence base here is stronger than for most other dietary interventions. Systematic reviews consistently show that fiber interventions increase SCFA production and can shift gut microbiota composition in measurable ways.
Why fiber loss matters in processed diets
Many refined foods are low in fiber by design. Refining wheat removes the bran. Juicing removes pulp. Puffing and extruding grains changes their structure. The result is a food environment where energy is abundant but fermentable material is scarce.
A low-fiber diet gives the microbiome less material to ferment. Over time, this may reduce beneficial microbial metabolites, allow less beneficial bacterial populations to expand, and shift the gut environment in ways that are associated — in observational research — with increased risk of gut-related diseases.
Practical fiber upgrades
The good news: you do not need exotic supplements or expensive products. The strongest evidence points to whole food sources of fiber. Here are realistic swaps:
| Instead of this | Try this | Why it helps |
|---|---|---|
| Sweetened breakfast cereal | Rolled oats with berries | More beta-glucan, less added sugar |
| Fruit juice | Whole fruit | Intact fiber, slower sugar release |
| White rice as a side | Cooked and cooled rice or lentils | Resistant starch forms on cooling |
| Flavored crackers | Hummus with raw vegetables | Fiber plus prebiotic compounds |
| Fruit snacks or gummies | Fresh or frozen berries | Real fermentable fiber and polyphenols |
| Refined pasta | Beans or lentils added to pasta dishes | Significant fiber increase |
| Sweetened yogurt cup | Plain yogurt with seeds and fruit | Fiber added, sugar reduced |
A sensible starting point is simply adding one fiber-rich food to each main meal. That alone can meaningfully shift what arrives in your colon.
Satiety, Eating Speed, and Metabolism: Why Food Texture Matters
Ultra-processed foods are not just nutritionally different — they are physically engineered in ways that can alter how much you eat and how quickly. This is relevant to gut chemistry because eating speed, portion size, and food structure all affect digestion.
The NIH ultra-processed diet study
One of the most cited studies in this area was a small randomized controlled trial conducted by researchers at the NIH. Twenty adults were admitted to a clinical research facility and given access to ultra-processed and minimally processed diets in alternating two-week periods. Meals were matched for total calories, sugar, fiber, fat, and carbohydrates — participants could eat as much or as little as they wanted.
The result: on the ultra-processed diet, participants ate approximately 500 more calories per day and gained weight. On the minimally processed diet, they ate less and lost weight — without being told to restrict intake.
That is a strong finding and worth taking seriously. It is also a small study in a controlled setting, so I would be careful about overgeneralizing. But the direction of the evidence is consistent with what we know about food texture, eating speed, and satiety signaling.
Why this matters for gut chemistry
The connection to gut health goes beyond calorie intake:
- Faster eating and softer textures may change how satiety hormones are released
- Refined ingredients absorbed quickly in the small intestine deliver less to the colon
- Less intact food structure means less physical work for the digestive system — and potentially less mechanical stimulation of gut motility
- The gut-brain axis — the communication network between gut microbes, the enteric nervous system, and the brain — may respond differently to liquid, soft, and engineered foods than to intact meals
Practical examples
The simplest way to look at it is through direct comparisons:
- Apple vs apple juice — whole fruit delivers fiber, slower sugar release, more colonic material
- Rolled oats vs sweetened instant oat packets — similar origin, different texture, sugar load, and digestion speed
- Beans and rice vs refined snack crackers — similar carbohydrate content, very different fiber and satiety profiles
- Plain yogurt with berries vs sweetened yogurt dessert — similar dairy base, very different sugar and additive load
- Whole nuts vs nut-flavored snack bars — whole nuts slow digestion; bars often contain refined starches and sweeteners
The food matrix — the physical structure of what you eat — is not a minor detail. It is part of the chemistry your gut responds to.
The Gut Barrier, Mucus Layer, and Inflammation: What to Explain Carefully
The gut barrier is a legitimate area of research, and diet does appear to influence it. But this topic also attracts considerable hype. Here is what the evidence actually supports.
What the gut barrier does
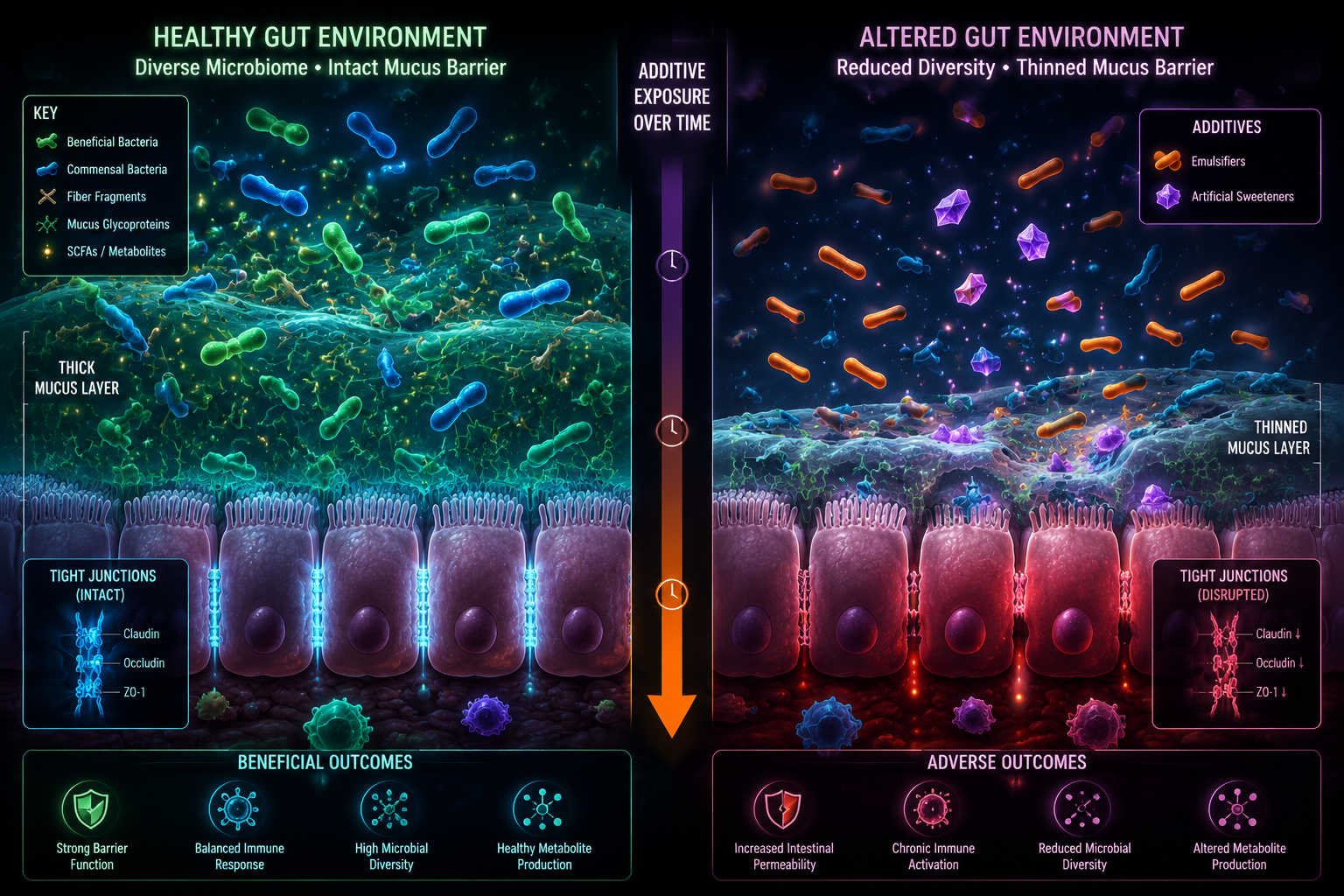
The gut lining is not just a passive wall. It is a dynamic system that includes:
- Epithelial cells — the physical lining of the intestine
- Tight junctions — protein structures that control what passes between cells
- The mucus layer — a protective coating produced by goblet cells that separates gut contents from the epithelium
- Immune cells — concentrated in the gut-associated lymphoid tissue (GALT)
- The microbiome itself — which interacts with and helps maintain barrier function
The barrier’s job is to allow selective absorption of nutrients while keeping bacteria, toxins, and undigested food particles from entering the bloodstream inappropriately.
How diet may influence barrier function
Fiber-derived metabolites — particularly butyrate — are commonly discussed in relation to colonocyte energy and barrier support. Colonocytes (the cells lining the colon) use butyrate as their primary fuel source. A diet that consistently delivers little butyrate-producing fiber may, over time, affect how well these cells function.
Diet patterns high in UPFs and low in fiber may be less supportive of the mucus layer and tight junction integrity. Some additives — particularly certain emulsifiers — are being studied for potential effects on mucus thickness and permeability. The evidence is not conclusive in humans, but it is a reasonable area of ongoing scientific interest.
What not to overclaim
It is not that simple. “Leaky gut” has become a catch-all explanation for everything from fatigue to autoimmune conditions in popular health media. The science is more nuanced:
- Intestinal permeability exists on a spectrum and is measured in specific ways
- Increased permeability is associated with certain conditions (IBD, celiac disease) but is not a diagnosis in itself
- You cannot “heal the gut lining in 30 days” with a specific protocol
- Eliminating broad food groups without medical need is rarely supported by evidence
When to see a doctor: Persistent digestive symptoms — blood in stool, unexplained weight loss, severe abdominal pain, ongoing diarrhea, or new symptoms after age 50 — should be discussed with a qualified healthcare professional. These symptoms require proper clinical evaluation, not dietary self-management.
The Modern Food Environment: It Is Not Just Individual Willpower
Ultra-processed foods are convenient, affordable, heavily marketed, and designed to be satisfying. Understanding how processed food affects gut health at a population level means acknowledging that food environment shapes behavior as much as individual choice does.
Recent CDC/NCHS data reported that people in the United States got approximately 55% of daily calories from ultra-processed foods during August 2021–August 2023, with adults averaging around 53%. That is not a personal discipline failure. That is a food environment issue.
Many people rely on ultra-processed foods because of:
- Cost — whole foods are often more expensive per calorie
- Time — work schedules, caregiving, and commuting leave little time for cooking
- Availability — in many communities, ultra-processed options are more accessible than fresh produce
- Marketing — UPFs are promoted heavily, especially to families with children
- Palatability — they are engineered to taste good and be easy to eat
The goal of this article is not to shame anyone for eating a bag of chips or buying packaged meals. The goal is to help readers understand what is happening in their gut when certain foods dominate the diet — and to offer practical, realistic options that work within real life.
A practical framing: do not aim for a perfect pantry. Aim for a gut-friendlier default.
How to Build a Gut-Friendlier Diet Without Going Extreme
The evidence suggests that adding fiber-rich, diverse, minimally processed foods to your regular diet is more effective — and more sustainable — than trying to eliminate every ultra-processed item.

Add before you subtract
Start with what gives the biggest return. Before worrying about what to remove, focus on adding:
- Fiber-rich foods to every main meal (beans, oats, vegetables, fruit, whole grains)
- Protein and fiber to breakfast — this combination supports satiety and reduces mid-morning snacking
- Plants to meals you already eat — add spinach to scrambled eggs, beans to soup, seeds to yogurt
- Fermented foods if tolerated — plain yogurt, kefir, kimchi, sauerkraut, miso
- Water when increasing fiber — fiber needs fluid to function properly
Use the “ingredient displacement” test
Ask yourself: what is this food replacing? If a packaged product is replacing beans, vegetables, whole grains, fish, eggs, or home-cooked meals — that is worth noticing. If it is a convenient addition to an otherwise fiber-rich diet, the concern is lower.
Choose better convenience foods
Convenience is not the enemy. These options are processed, practical, and still support gut health:
- Frozen vegetables — nutritionally comparable to fresh, no prep required
- Canned beans — high fiber, affordable, versatile (rinse to reduce sodium)
- Plain Greek yogurt — protein, live cultures, low added sugar
- Rotisserie chicken — minimal processing, easy protein base for meals
- Unsweetened oatmeal — beta-glucan fiber, easy to prepare
- Canned fish (sardines, tuna, salmon) — protein and omega-3 fatty acids
- Pre-washed salad greens — convenience without ultra-processing
- Microwave brown rice or quinoa packets — whole grain, fast
- Nuts and seeds — fiber, healthy fats, portable
- Hummus — legume-based, fiber-rich, pairs with vegetables
Use a label-reading shortcut
You do not need to memorize every additive. A practical approach:
- Check fiber per serving — aim for at least 3g per serving for a meaningful contribution
- Check added sugars — the lower the better for most packaged foods
- Look for whole-food ingredients near the top of the list — ingredients are listed by weight
- Be cautious with long lists of sweeteners, emulsifiers, gums, colorings, flavorings, and refined starches combined
- Judge the whole pattern — one additive in an otherwise fiber-rich food is different from a product built entirely from refined and additive-heavy ingredients
Keep it simple and consistent. You do not need to read every label every time. Build familiarity with the foods you buy regularly, and apply the shortcut when evaluating something new.
What to Eat More Often for Better Gut Chemistry
The positive case for gut health is stronger than the negative one. Rather than focusing only on what to avoid, here is what the evidence supports eating more of.
Fermentable fibers
These are the foods that most directly fuel SCFA production in the colon:
- Oats (especially rolled or steel-cut)
- Beans, lentils, and chickpeas
- Barley
- Apples and pears (with skin)
- Berries (blueberries, raspberries, blackberries)
- Onions and garlic
- Asparagus and leeks
- Slightly underripe bananas
- Cooked and cooled potatoes or rice (for resistant starch)
Polyphenol-rich foods
Polyphenols are plant compounds that reach the colon largely intact and are fermented by gut microbes. They are associated with microbiome diversity and anti-inflammatory effects:
- Berries of all kinds
- Dark cocoa (unsweetened or minimally sweetened)
- Green tea and coffee
- Herbs and spices (turmeric, oregano, rosemary)
- Extra-virgin olive oil
- Colorful vegetables (red cabbage, purple carrots, beets)
Fermented foods
Foods with live cultures can contribute beneficial microorganisms and may support microbial diversity:
- Yogurt with live active cultures (plain, unsweetened preferred)
- Kefir — fermented milk with diverse bacterial strains
- Sauerkraut — fermented cabbage (note: can be high in sodium)
- Kimchi — fermented vegetables (also high in sodium; may not suit everyone with IBS)
- Miso — fermented soybean paste
- Tempeh — fermented soybeans, also a good protein source
A note on tolerance: fermented foods with high histamine content may not suit everyone, particularly those with histamine sensitivity or certain IBS patterns. Start with small amounts and observe your response.
Minimally processed staples
The foundation of a gut-friendly diet does not need to be complicated:
- Eggs
- Fish and seafood
- Beans and legumes
- Whole grains (oats, barley, brown rice, quinoa)
- Nuts and seeds
- Vegetables (fresh, frozen, or canned without heavy additives)
- Fruit
- Plain dairy or fortified plant alternatives
- Extra-virgin olive oil
Who Should Be More Careful With Gut Health Advice?
General dietary guidance is a starting point, not a prescription. Some people need individualized advice before making significant changes.
The following groups should consult a healthcare provider or registered dietitian before making major dietary shifts based on general gut health guidance:
- IBS (irritable bowel syndrome) — high-fiber foods can worsen symptoms for some IBS subtypes; a low-FODMAP approach may be more appropriate
- IBD (Crohn’s disease or ulcerative colitis) — fiber needs vary by disease activity and location
- Celiac disease — gluten-containing whole grains are not appropriate; safe whole-grain alternatives exist
- Diverticular disease — fiber recommendations have evolved; individualized advice is important
- Diabetes — fiber and carbohydrate choices interact with blood sugar management
- Kidney disease — high-potassium plant foods and certain fibers may need to be limited
- People taking GLP-1 medications — slower gastric emptying may require personalized guidance on fiber, meal size, and digestion speed
- Food allergies or intolerances — some high-fiber foods (legumes, wheat, nuts) are common allergens
When to seek medical attention: Do not manage the following with dietary changes alone. See a clinician promptly if you experience:
- Blood in stool or black, tarry stools
- Unexplained weight loss
- Severe or persistent abdominal pain
- Ongoing diarrhea or constipation that is new or worsening
- New digestive symptoms after age 50
- Symptoms that interfere with daily life
Key Takeaway: Think Less About “Good vs Bad Foods” and More About Gut Inputs
Your gut chemistry is shaped by what repeatedly arrives in your digestive tract — not by any single meal, ingredient, or packaged food.
The most important pattern is not perfection. It is the balance between:
- Fiber vs refined starch — does your diet deliver enough fermentable material to the colon?
- Whole-food structure vs broken-down food matrix — are you eating foods that still have their original physical architecture?
- Microbial fuel vs empty convenience calories — are your gut bacteria getting what they need to produce beneficial metabolites?
- Diverse plants vs repetitive packaged foods — does your diet support microbial diversity?
- Occasional additives vs additive-heavy daily staples — is the overall additive load reasonable?
The goal is to shift the default toward foods that feed the microbiome and support stable digestion. That does not require a perfect pantry, expensive supplements, or eliminating every packaged food. It requires consistent, practical choices that give your gut more of what it works best with.
I prefer to look at what actually works. And what works, based on current evidence, is a diet with enough diverse, fermentable fiber; enough whole-food structure; and enough variety to support a healthy microbial community. Everything else — the specific additives, the occasional ultra-processed meal, the convenience shortcuts — matters less than that foundation.
Conclusion: What to Do With This Information
Understanding how processed food affects gut health is not about becoming anxious every time you open a package. It is about building a clearer picture of what your gut actually responds to — and using that picture to make better everyday decisions.
Here are the most actionable next steps:
- Add one fiber-rich food to each main meal this week. Beans, oats, vegetables, or whole fruit. Start there.
- Identify your top three ultra-processed staples — the foods you eat most often that fit the UPF profile. Ask what you could swap them for, even partially.
- Stock two or three gut-friendly convenience foods — frozen vegetables, canned beans, plain yogurt, or canned fish. These give you a fast option that still supports gut chemistry.
- Read labels with the shortcut in mind — fiber content, added sugars, and ingredient list length are your three quick signals.
- Do not aim for perfection. Aim for a gut-friendlier default that you can maintain without stress.
The evidence suggests that consistent dietary patterns — not single foods or ingredients — are what shape gut health over time. A diet that regularly delivers diverse, fermentable fiber and minimally processed whole foods gives your gut microbiome the raw material it needs. That is the main takeaway.
For readers who want to go deeper, consider exploring how to read food labels for gut health, which high-fiber foods have the strongest evidence, and how fermented foods compare to probiotic supplements. Each of those topics builds on what this article has covered.
Frequently Asked Questions
What is modern food processing?
Modern food processing includes any technique used to alter food from its raw state — from simple preservation (freezing, canning) to complex industrial formulation (ultra-processed foods made with refined ingredients, additives, and flavorings). Not all processing is harmful; the concern centers on ultra-processed products that are low in fiber and high in additives.
Are all processed foods bad for gut health?
No. Yogurt, canned beans, frozen vegetables, oats, and plain dairy are all processed — and they can support gut health. The concern is with ultra-processed foods that displace fiber-rich options and deliver little fermentable material to the colon.
What is the difference between processed and ultra-processed food?
Processed foods are minimally altered from their whole-food state (canned tomatoes, pasteurized milk, rolled oats). Ultra-processed foods are industrially formulated with refined ingredients, additives, and flavorings not typically used in home cooking — think packaged pastries, soft drinks, instant noodles, and many flavored snack foods.
How do ultra-processed foods affect the gut microbiome?
UPF-heavy diets tend to deliver less fermentable fiber to the colon, which reduces short-chain fatty acid production. Some additives may also interact with gut microbes or the mucus layer. Research associates UPF-heavy diets with reduced microbial diversity and links to gut diseases, though causal evidence in humans is still developing.
What is gut chemistry?
Gut chemistry refers to the biological and chemical processes occurring in the digestive tract — including microbial fermentation, short-chain fatty acid production, gut barrier function, immune signaling, and the metabolites produced when gut bacteria process what you eat.
What are short-chain fatty acids, and why do they matter?
Short-chain fatty acids (SCFAs) — primarily butyrate, propionate, and acetate — are produced when gut bacteria ferment dietary fiber and resistant starch. Butyrate is the main energy source for colon cells and is associated with gut barrier support. SCFAs are also involved in immune signaling and metabolic regulation.
Do emulsifiers affect gut health?
Some research — mostly preclinical — suggests certain emulsifiers (such as polysorbate 80 and carboxymethylcellulose) may affect gut microbiota, intestinal permeability, and inflammation. Human evidence is limited. The concern is not about any single product containing lecithin, but about frequent exposure to multiple additives in a low-fiber dietary pattern.
Are artificial sweeteners bad for the microbiome?
Some human studies suggest certain non-nutritive sweeteners can alter gut microbiome composition and glucose tolerance in some individuals. Effects vary by sweetener type and person. Replacing sugar with sweeteners does not automatically improve gut health — the overall dietary pattern still matters most.
How does fiber support gut bacteria?
Dietary fiber — particularly fermentable types like fructooligosaccharides, inulin, pectin, beta-glucan, and resistant starch — is the primary fuel for gut microbes. Bacteria ferment these fibers in the colon, producing short-chain fatty acids that support the gut lining, immune function, and metabolic health.
What are simple ways to eat fewer ultra-processed foods?
Add fiber-rich foods before worrying about restriction. Stock gut-friendly convenience foods (frozen vegetables, canned beans, plain yogurt). Use the label-reading shortcut: check fiber content, added sugars, and ingredient list complexity. Identify your top two or three UPF staples and find one realistic swap for each.
What processed foods can still be healthy?
Frozen vegetables, canned beans, plain Greek yogurt, rolled oats, canned fish, pre-washed salad greens, microwave brown rice, nuts, seeds, and hummus are all processed — and all reasonable choices for gut health. The key is whether they deliver fiber, intact food structure, and minimal added sugars or additives.
When should digestive symptoms be discussed with a doctor?
Seek medical advice for blood in stool, unexplained weight loss, severe or persistent abdominal pain, ongoing diarrhea or constipation, or any new digestive symptoms after age 50. These require clinical evaluation and should not be managed with dietary changes alone.
Evidence and further reading
Modern Food Processing & Gut Chemistry reading path
- Start here: Modern Food Processing and Gut Health (you are here)
- Deep dive: Ultra-Processed Foods, Emulsifiers and Microplastics
- Deep dive: Fermented Foods vs Probiotics vs Postbiotics
- Deep dive: Resistant Starch and Prebiotic Fiber

