Fermented Foods vs Probiotics vs Postbiotics: What Actually Survives Digestion?

Last updated: May 16, 2026
Quick Answer
Fermented foods, probiotics, and postbiotics are not the same thing, and they do not behave the same way in your digestive system. Some live microbes from fermented foods and probiotic supplements may survive the journey through stomach acid and bile to reach the colon, but survival depends heavily on the strain, the food, the formulation, and your individual digestive conditions. Postbiotics are a different category entirely: they are intentionally non-living, so the survival question does not apply to them in the same way.
Key Takeaways
- Fermented foods are made through microbial growth and enzymatic conversion, but not all of them contain live microbes by the time you eat them. Pasteurization, baking, and shelf-stable processing can eliminate living organisms.
- Probiotics are defined as live microorganisms that, when consumed in adequate amounts, confer a health benefit. The effect is strain-specific, not category-wide.
- Postbiotics are inanimate microbial preparations or components with demonstrated health benefit. They do not need to survive digestion as living organisms.
- Survival through stomach acid is real but inconsistent. It depends on strain, dose, food matrix, timing, and formulation.
- Fermented foods are not automatically probiotics. Very few fermented foods meet the formal scientific definition.
- For everyday gut health, food pattern and fiber intake matter more than chasing a high-CFU supplement.
- Probiotics may be most useful for specific, strain-supported goals under appropriate guidance, not as a general wellness shortcut.
- Postbiotic research is promising but still developing. Be cautious with broad marketing claims.
- The strongest everyday strategy combines fiber-rich plants, minimally processed foods, and fermented foods you tolerate well.
- Persistent digestive symptoms should be discussed with a clinician, not managed with supplements alone.
In this guide
- Quick Answer
- What Is the Difference Between Fermented Foods, Probiotics, and Postbiotics?
- Why Digestion Survival Is More Complicated Than "Dead or Alive"
- Do Fermented Foods Survive Digestion?
- Do Probiotic Supplements Survive Digestion?
- Do Postbiotics Survive Digestion?
- Fermented Foods vs Probiotics vs Postbiotics: Which Is Better for Gut Health?
- What Matters More Than Survival Alone?
- Common Mistakes People Make With Fermented Foods and Probiotics
- Practical Food Examples: What to Eat If You Want More Fermented Foods
- So, What Actually Survives Digestion?
- FAQs
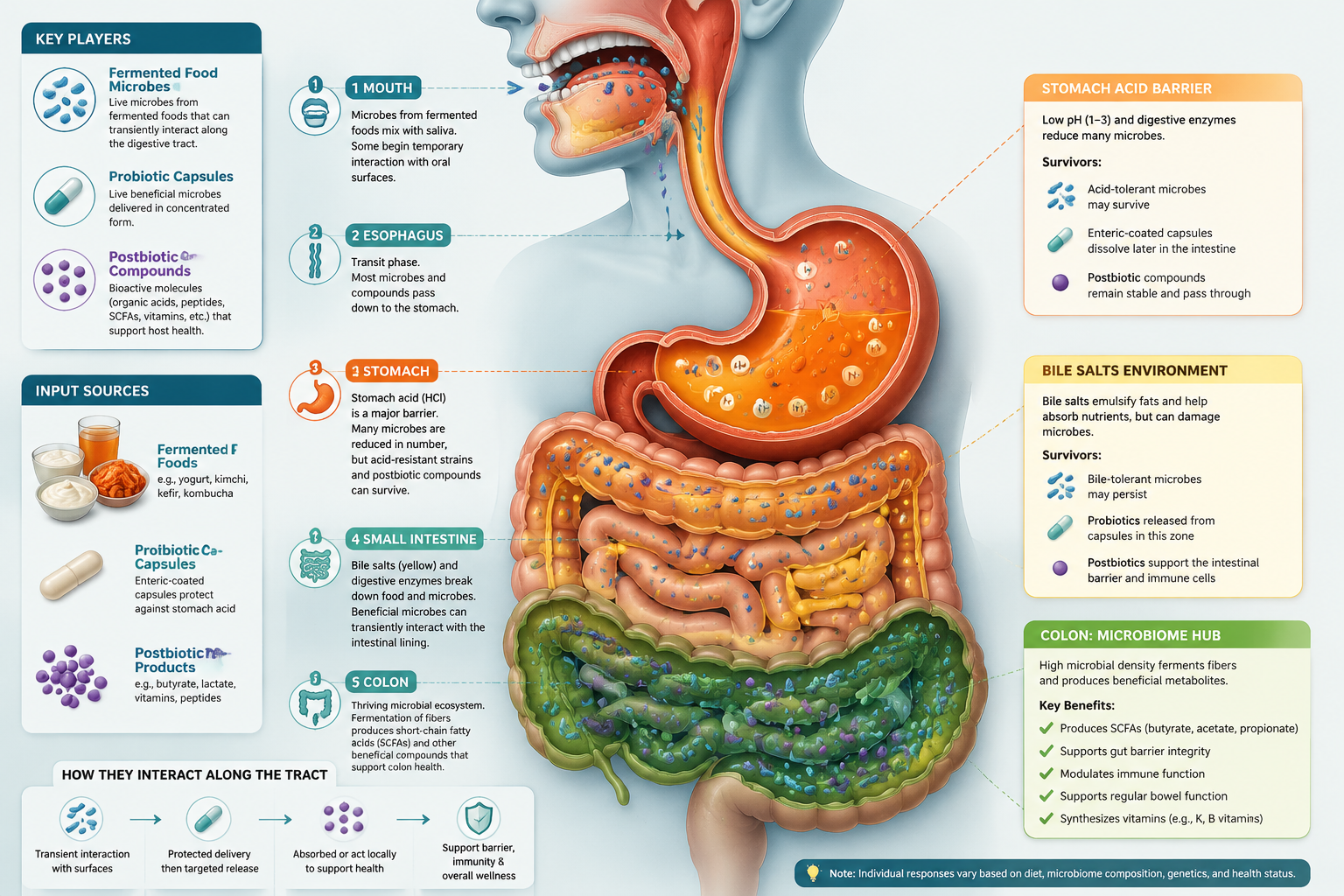
What Is the Difference Between Fermented Foods, Probiotics, and Postbiotics?
Before we get into what survives digestion, let’s define the terms properly. These three categories are frequently used interchangeably in health content, and that is where most of the confusion starts. They are related, but they are not the same thing.
What Counts as a Fermented Food?
A fermented food is any food made through the desired growth of microorganisms and the enzymatic conversion of food components. That is the working definition used by the International Scientific Association for Probiotics and Prebiotics (ISAPP), and it is a useful one because it focuses on the process, not the outcome.
Common fermented foods include yogurt, kefir, kimchi, sauerkraut, miso, tempeh, natto, kombucha, and sourdough bread. Fermentation can improve taste, preservation, digestibility, texture, and nutrient availability. These are real and meaningful benefits.
Here is the key distinction: fermented food is a food process, not automatically a probiotic claim. The fact that a food was fermented does not mean it currently contains live microbes, and it certainly does not mean those microbes have been identified, tested, and proven to deliver a specific health benefit.
What Counts as a Probiotic?
A probiotic is not just any “good bacteria.” The formal definition requires three things:
- The microorganism must be live
- It must be consumed in adequate amounts
- It must confer a health benefit on the host
Beyond that, a true probiotic should be identified at the genus, species, and strain level. This matters because probiotic effects are strain-specific. Saying “Lactobacillus” is enough to call something a probiotic is like saying “medication” is enough to describe a treatment. The strain is the tool. The genus is just the category.
In plain English: a probiotic is a named, tested, live microorganism with a documented job to do. Most products on the market do not meet that bar in full.
What Counts as a Postbiotic?
This is where the terminology gets most muddled online. A postbiotic is not simply “whatever probiotics produce” or “dead bacteria.” The stricter consensus definition, developed by ISAPP, describes postbiotics as inanimate microorganisms and/or their components that confer a health benefit on the host.
That distinction matters. A killed bacterial cell is not automatically a postbiotic. A purified short-chain fatty acid (SCFA) extracted from a fermentation process is not automatically a postbiotic under the strict definition. To qualify, the preparation must be characterized and must have demonstrated a health benefit.
Marketers often blur this term because “postbiotic” sounds credible and scientific. I would be careful with that. The evidence for postbiotics is developing, but the category is real and the science behind it is serious. It just needs to be separated from the hype.
The simplest way to look at it is this: Fermented foods are the broad food category. Probiotics are the tested live microbes. Postbiotics are non-living microbial preparations or components with demonstrated benefit.
Why Digestion Survival Is More Complicated Than “Dead or Alive”
The survival question sounds simple, but it is not. Whether a microbe survives digestion is not a binary outcome. It depends on multiple overlapping conditions, and even microbes that do not survive in large numbers can still interact with the gut environment in ways that matter.
The Mouth and Stomach Start Breaking Things Down
Digestion begins before food reaches the stomach. Chewing breaks food into smaller particles, and salivary enzymes start chemical breakdown. By the time food reaches the stomach, it encounters hydrochloric acid at a pH that can drop below 2 in a fasted state. That is a genuinely hostile environment for most microorganisms.
Here is where the food matrix becomes important. A microbe consumed inside a yogurt or kefir matrix is not entering the stomach in isolation. The food itself, its proteins, fats, and buffering capacity, may partially protect microbes from immediate acid exposure. This is one reason why eating fermented foods with a meal, rather than on an empty stomach, may influence how many live microbes reach further down the tract.
The Small Intestine Adds Bile, Enzymes, and Absorption Pressure
Surviving the stomach is only part of the challenge. In the small intestine, bile acids are released to help digest fats, and they create a stressful chemical environment for many microbes. Pancreatic enzymes add further pressure. Some microbial strains are more bile-tolerant than others, and this is one of the traits researchers look for when selecting probiotic strains.
It is also worth noting that even transient microbes, ones that do not permanently colonize the gut, can still interact with the intestinal lining, immune cells, and the existing microbial community as they pass through. Survival to the colon is not the only way a microbe can have an effect.
The Colon Is Where Microbial Fermentation Becomes Most Relevant
The large intestine is where the most complex microbial activity happens. This is where resident gut bacteria ferment fiber and resistant starch into short-chain fatty acids like butyrate, acetate, and propionate. These compounds feed the colon lining, influence immune signaling, and support gut barrier function.
What reaches the colon shapes what happens there. Fermented foods and fiber-rich foods can complement each other because microbes need substrate. A diet high in fermented foods but low in fiber is a bit like stocking a kitchen with skilled chefs and no ingredients. The microbes, whether resident or transient, have less to work with.
For a deeper look at how fiber, SCFAs, and colon chemistry connect, read the full guide to how modern food processing affects gut chemistry.
Do Fermented Foods Survive Digestion?
Some live microbes from fermented foods may survive digestion, but it depends significantly on the food itself, how it was processed, and how it was stored.

Some Live Microbes May Survive, but It Depends on the Food
Raw or unpasteurized fermented foods are more likely to contain live microbes than heat-treated or shelf-stable versions. Refrigerated sauerkraut, kimchi, kefir, and yogurt labeled with “live and active cultures” are stronger candidates for delivering live microorganisms. These products have not been subjected to the heat that kills microbes.
Sourdough bread is a good example of the other side. It is genuinely fermented, and the fermentation process improves its digestibility and flavor. But baking kills the live organisms. What remains is a fermented food with real nutritional benefits, including modified gluten structure, organic acids, and improved mineral availability, but without live microbes.
Pasteurized kombucha, shelf-stable pickles made with vinegar rather than lacto-fermentation, and many commercial miso products that have been heat-treated fall into a similar category. Fermented, yes. Probiotic, no.
Fermented Foods Are Not Automatically Probiotics
This is one of the most important points in the fermented foods vs probiotics conversation, and it is worth being direct about it.
A fermented food can be genuinely beneficial without meeting the formal probiotic definition. The microbes in most fermented foods have not been identified at the strain level. They have not been tested in controlled trials for a specific health outcome. That does not make the food worthless; it just means it is a dietary pattern tool rather than a targeted therapeutic product.
ISAPP has been clear on this: very few fermented foods meet all the criteria required to carry a probiotic claim. That is not a criticism of fermented foods. It is a clarification of what the word “probiotic” actually means.
What Fermented Foods May Offer Besides Live Microbes
Even when live microbes do not survive in large numbers, fermented foods can still offer meaningful nutritional value:
- Organic acids (lactic acid, acetic acid) that may support gut pH and inhibit certain pathogens
- Bioactive peptides formed during fermentation that may have anti-inflammatory or antihypertensive properties
- Improved digestibility, particularly for proteins and starches
- Reduced lactose in fermented dairy like yogurt and kefir, making them better tolerated by many people
- Transformed micronutrients, including increased B vitamin availability in some fermented foods
- Greater microbial diversity in the diet, even if individual strains are not formally tested
Kefir is a useful example here. It is not just a delivery vehicle for microbes. It is a fermented food matrix containing protein, minerals, organic acids, and fermentation-derived compounds. The whole product has value beyond the question of which microbes survive to the colon.
Do Probiotic Supplements Survive Digestion?
Some probiotic strains are specifically selected or formulated to survive stomach acid and bile exposure better than others. But the honest answer is that survival varies considerably, and survival alone does not guarantee benefit.
Some Probiotic Strains Are Built to Survive Better Than Others
Strain selection matters. Spore-forming bacteria like certain Bacillus species are inherently more resistant to heat, acid, and bile. Specific Lactobacillus and Bifidobacterium strains have been selected for clinical research partly because of their demonstrated ability to reach the gut in viable form. Saccharomyces boulardii, a yeast-based probiotic, has different survival characteristics from bacterial strains.
Formulation also matters. Enteric-coated capsules are designed to resist stomach acid and release contents further along the digestive tract. Microencapsulation is another approach. These are real engineering solutions to a real problem, and they can make a difference.
The National Center for Complementary and Integrative Health (NCCIH) notes that different probiotics can have different effects, and evidence for one type does not automatically apply to another. That is a point worth repeating: probiotic benefits are strain-specific, not category-wide.
CFU Count Is Not the Whole Story
CFU stands for colony-forming units, and it is the standard way to measure the number of live microorganisms in a probiotic product. A higher CFU count sounds better, but more is not always better.
A product with 50 billion CFUs of a poorly researched strain is less useful than a product with 5 billion CFUs of a well-studied strain matched to a specific outcome. The number is only meaningful in context.
Storage conditions also affect viability. Heat, moisture, and time can significantly reduce the number of live organisms in a product before you even open the bottle. Some products guarantee CFU counts at manufacture but not at the point of use. That is a meaningful difference.
NCCIH has also noted that some probiotic products have been reported to contain microorganisms other than those listed on the label, which is a quality-control concern worth keeping in mind when choosing products.
Probiotics May Be Useful, but They Are Not a Shortcut Around Diet
For specific, well-defined goals, such as reducing the risk of antibiotic-associated diarrhea or supporting recovery from certain digestive disruptions, there is reasonable evidence behind specific probiotic strains. This is where probiotic supplements can make genuine sense, particularly under the guidance of a clinician who knows the relevant evidence.
For generally healthy adults, the evidence does not strongly support taking high-CFU supplements as a daily default. Food pattern, fiber intake, and fermented food variety likely matter more for long-term gut health than chasing a supplement.
⚠️ Safety note: People with serious illness, compromised immune systems, premature infants, or complex medical conditions should consult a clinician before using probiotic supplements. NCCIH highlights greater risk in people with severe illness or compromised immune function. This is not a category where “natural” automatically means safe for everyone.
Do Postbiotics Survive Digestion?
Postbiotics do not need to survive digestion as living organisms, because they are not alive to begin with. That is the simplest and most important thing to understand about this category.
Postbiotics Do Not Need to Be Alive
The question “do postbiotics survive digestion?” is a different question from the one we ask about probiotics. With postbiotics, the relevant question is whether their active components remain biologically relevant after passing through the digestive system.
Think of postbiotics as microbial signals, structures, or preparations rather than living passengers. A heat-killed bacterial cell wall fragment, for example, may still interact with immune receptors in the gut lining. A characterized cell-free preparation from a fermentation process may still influence gut barrier function. The mechanism does not require the organism to be alive.
Why Stability Is the Big Postbiotic Advantage
Because postbiotics are not live microbes, they offer a stability advantage that probiotics cannot match. They do not require refrigeration in the same way. They are not vulnerable to heat-induced die-off during manufacturing or storage. They can potentially be incorporated into foods, beverages, and supplements more easily than live cultures.
This stability makes postbiotics an interesting area for food science and clinical research. But I would be careful with the enthusiasm here. The research is developing, and the category is newer than the marketing suggests. Product-specific evidence matters more than category-wide claims.
Why the Term Gets Misused
Many online articles loosely describe SCFAs, lactic acid, or any microbial byproduct as postbiotics. This is not accurate under the stricter consensus definition. Purified metabolites alone, like isolated butyrate or lactic acid, are not automatically postbiotics. The preparation must be characterized, and a health benefit must be demonstrated.
Fermented foods can contain postbiotic-like compounds and microbial metabolites. But that does not automatically make a fermented food a validated postbiotic product. The terms describe different things, and conflating them does not help anyone make better decisions.
Fermented Foods vs Probiotics vs Postbiotics: Which Is Better for Gut Health?
There is no single winner in the fermented foods vs probiotics vs postbiotics comparison. They serve different purposes, work through different mechanisms, and suit different contexts. The better question is: which one fits your situation?

Choose Fermented Foods for a Food-First Gut Health Pattern
For most healthy adults, fermented foods are the most practical daily tool. They fit into meals, they bring nutritional value beyond live microbes, and they support a broader dietary pattern that is associated with gut health.
A small but carefully conducted clinical trial of 36 healthy adults, published in Cell in 2021 by researchers at Stanford, found that a 10-week high-fermented-food diet increased microbiome diversity and reduced several markers of immune activation, compared to a high-fiber diet in the same study. This is promising and worth noting, but it should not be read as proof that fermented foods treat disease. It is one study, and the field needs more replication.
What it does support is fermented foods as a meaningful dietary strategy, not just a wellness trend.
Choose Probiotics for Strain-Specific Goals
Probiotic supplements make the most sense when there is a specific, researched reason to use a particular strain. Antibiotic-associated diarrhea is one of the better-supported use cases. Certain digestive conditions, traveler’s diarrhea prevention, and some immune-related applications have reasonable evidence behind specific strains.
The key word is “specific.” Do not assume that a probiotic supplement labeled for “digestive health” or “immune support” has the evidence to back those claims. Look for strain identification and published research on that strain for that outcome.
Choose Postbiotics for Stability and Emerging Use Cases
Postbiotics are best framed as an emerging category with genuine scientific interest behind it. If you are looking at a product making postbiotic claims, the evidence should be product-specific. What preparation? What health benefit? What study? If those questions cannot be answered clearly, treat the claim with appropriate skepticism.
Best Everyday Strategy: Do Not Pick Just One
For general gut health, the foundation remains what it has always been:
- Fiber-rich plants as the primary substrate for your gut microbiome
- Minimally processed foods that preserve food structure and nutrient density
- Fermented foods where tolerated, as a regular part of the diet
- Lower reliance on ultra-processed foods that displace fiber-rich options and may disrupt gut ecology
Probiotics and postbiotics are tools, not replacements for diet quality. The basics still do the heavy lifting.
For the other side of this conversation, see the guide to ultra-processed foods, emulsifiers, and microplastics, which explains what modern food processing may remove from or add to what reaches your gut.
What Matters More Than Survival Alone?
Survival through stomach acid is a real and relevant question, but it is not the only thing that determines whether fermented foods, probiotics, or postbiotics have any effect. Several other factors matter just as much, sometimes more.
The Food Matrix Matters
Microbes inside yogurt, kefir, kimchi, or sauerkraut are not entering your digestive system in isolation. They are embedded in a food matrix of proteins, fats, carbohydrates, acids, and other compounds. That matrix may buffer stomach acid exposure, slow gastric emptying, and influence how microbes interact with the gut environment.
This is one reason why the fermented foods vs probiotics comparison is not simply about which delivers more live microbes. The food matrix itself is part of the benefit, and it is something a capsule cannot replicate.
The Strain Matters
Probiotic benefits cannot be generalized across all strains, and this point cannot be overstated. Saying all probiotics work the same is like saying all medicines work the same because they come in capsules. The strain is the active ingredient. The genus is just the family name.
When evaluating any fermented food or probiotic product, the question to ask is: which specific strain, and what is the evidence for that strain doing what is claimed?
The Dose and Frequency Matter
Occasional fermented foods are likely beneficial, but consistency matters more than any single serving. The gut microbiome responds to patterns over time, not to one-off interventions.
Start small and build tolerance, particularly if you are new to fermented foods. Some people experience gas, bloating, or digestive discomfort when introducing them too quickly. That is normal and usually temporary, but it is worth managing gradually.
Avoid exact dosing claims unless tied to a specific study or product. Context matters, and individual responses vary.
The Rest of the Diet Matters Most
Fermented foods and probiotics have less to work with if the overall diet is low in fiber and high in ultra-processed foods. Gut microbes need substrate. Without fermentable fiber, even the most carefully chosen probiotic strain has limited material to work with.
This is the connection to the broader cluster of content on this site: ultra-processed foods often displace the fiber-rich foods that gut microbes depend on. Fermented foods can be part of a gut-friendlier default, but they work best alongside a diet that gives the microbiome something to do.
Common Mistakes People Make With Fermented Foods and Probiotics
Mistake 1: Assuming All Fermented Foods Contain Live Cultures
Pasteurization, baking, filtering, and shelf-stable processing can reduce or eliminate live microbes. The label matters. Look for “live and active cultures,” refrigerated storage requirements, and “raw” or “unpasteurized” where relevant and safe. Vinegar-based pickles, for example, are not lacto-fermented and typically contain no live cultures.
Mistake 2: Thinking More CFUs Always Means Better Results
Strain and evidence matter more than a large number on the label. High CFU counts can be a marketing strategy rather than a meaningful quality indicator. A well-researched strain at a moderate dose will generally outperform a poorly researched strain at a high dose.
Mistake 3: Using Probiotics to Ignore a Low-Fiber Diet
Probiotics do not replace the substrates gut microbes need to function. If the diet is low in vegetables, legumes, whole grains, and other fiber sources, no supplement is going to compensate for that gap. Fiber is the foundation. Probiotics are an addition, not a substitute.
Mistake 4: Going Too Fast With Fermented Foods
Some people experience gas, bloating, histamine reactions, or digestive discomfort when introducing fermented foods too quickly. A gradual approach, starting with small servings and building over several weeks, is sensible for most people. For those with diagnosed digestive conditions, significant symptoms, or a history of histamine intolerance, speaking with a clinician or registered dietitian before making major dietary changes is the right call.
Mistake 5: Treating Gut Health Content Like Medical Treatment
This is the most important mistake to name clearly. Fermented foods, probiotics, and postbiotics are dietary and supplemental tools. They are not treatments for medical conditions.
⚠️ When to see a clinician: Persistent diarrhea, blood in stool, unexplained weight loss, severe abdominal pain, fever, or new digestive symptoms after age 50 should be discussed with a doctor, not managed with supplements or dietary changes alone. These symptoms need proper evaluation.
Practical Food Examples: What to Eat If You Want More Fermented Foods

Good Starting Options
These are practical, widely available fermented foods that are most likely to contain live microbes and offer meaningful nutritional value:
- Plain yogurt with live and active cultures (lower sugar, higher protein)
- Kefir (dairy or non-dairy), which typically contains a broader range of microorganisms than yogurt
- Kimchi (refrigerated, not pasteurized)
- Refrigerated sauerkraut (not the shelf-stable canned version)
- Miso added after cooking, not boiled heavily, to preserve live cultures
- Tempeh, which is fermented soy with a firm texture and good protein content
- Natto, if you are willing to acquire the taste
- Kombucha in moderation, watching for high sugar content in commercial versions
What to Check on the Label
| Label Element | What to Look For |
|---|---|
| Live cultures | “Live and active cultures” stated clearly |
| Storage | Refrigerated, not shelf-stable |
| Sugar content | Lower is generally better |
| Processing | “Pasteurized after fermentation” is a red flag for live microbes |
| Sodium | Check pickled vegetables; sodium can be high |
| Ingredients | Simpler is usually better |
How to Add Fermented Foods Without Overdoing It
- Start with small servings, around 1–2 tablespoons of kimchi or sauerkraut, or a small glass of kefir
- Pair fermented foods with fiber-rich meals to give gut microbes substrate to work with
- Use fermented foods as condiments or sides rather than the main event
- If you are choosing kombucha or sweetened yogurt as your primary strategy, check the sugar content first. A high-sugar fermented food is a trade-off, not a straightforward win
So, What Actually Survives Digestion?
Let’s return to the question the title asks, because it deserves a direct answer.
Fermented foods: Some live microbes may survive digestion, but it depends on the food, how it was processed, how it was stored, and individual digestive conditions. Heat-treated and shelf-stable fermented foods are unlikely to deliver significant numbers of live microbes. Refrigerated, unpasteurized versions are better candidates. Even when live microbes do not survive in large numbers, fermented foods still deliver organic acids, bioactive compounds, and a food matrix with real nutritional value.
Probiotics: Some strains are specifically selected or formulated to survive stomach acid and bile. Survival is strain-specific and formulation-specific. A well-chosen probiotic at an adequate dose may reach the colon in viable form, but this is not guaranteed across all products. Survival is necessary but not sufficient; the strain still needs to be matched to a specific, researched outcome.
Postbiotics: They do not survive as living organisms because they are not alive. The relevant question is whether their active components remain biologically relevant after digestion. Because they are inanimate and stable, they sidestep the survival problem entirely.
The main takeaway is this: For everyday gut health, do not obsess over survival alone. Focus on what consistently reaches your gut over time: dietary fiber, diverse plants, minimally processed foods, and fermented foods you tolerate well. That is the foundation. Probiotics and postbiotics can be considered as additions for specific purposes, not as replacements for diet quality.
For the bigger picture on what modern food processing removes from what reaches your gut, read the guide to how processed food affects gut chemistry. For the opposite side of the food-processing conversation, see the guide to ultra-processed foods, emulsifiers, and microplastics.
FAQs
Are fermented foods better than probiotic supplements?
Not automatically. Fermented foods are a better fit as a daily food-first habit because they bring nutritional value beyond live microbes and fit naturally into meals. Probiotic supplements may be more appropriate for specific, strain-supported goals, such as antibiotic-associated diarrhea support, where the evidence is clearer and the strain is matched to the outcome.
Do probiotics survive stomach acid?
Some do, some do not. Survival depends on the specific strain, the dose, the formulation (enteric-coated capsules help), whether the probiotic is taken with food, and individual stomach acidity. Spore-forming strains and certain Lactobacillus and Bifidobacterium strains tend to have better survival profiles, but this varies by product.
Are all fermented foods probiotic?
No. Fermented foods are not automatically probiotics. A formal probiotic must contain live, identified microorganisms at an adequate dose with demonstrated health benefits. Most fermented foods have not been tested at the strain level for specific health outcomes, and many have been heat-treated, which eliminates live microbes entirely.
Are postbiotics dead probiotics?
Not exactly. A killed probiotic is not automatically a postbiotic. Under the stricter scientific definition, a postbiotic must be a characterized inanimate microbial preparation or component with a demonstrated health benefit. The preparation, the characterization, and the evidence are all required. Simply killing a probiotic does not create a postbiotic.
Is yogurt a fermented food or a probiotic?
Yogurt is a fermented food. It may also contain probiotic strains if it is made with live cultures that have been identified at the strain level and shown to confer a specific health benefit. Many commercial yogurts contain live cultures but have not been formally tested as probiotics. Look for “live and active cultures” on the label, and prefer plain varieties with lower added sugar.
Does cooking fermented food kill probiotics?
Yes, heat can kill live microbes. Boiling miso, baking sourdough, or cooking kimchi will reduce or eliminate live organisms. The food may still contain fermentation-derived compounds, organic acids, and nutrients, but it will no longer deliver live microbes in meaningful numbers. Add miso to dishes after cooking rather than during, if preserving live cultures is the goal.
Should people with IBS eat fermented foods?
It depends. Some people with IBS tolerate fermented foods well and find them beneficial. Others react to FODMAPs (fermentable carbohydrates found in some fermented foods), histamine, carbonation in kombucha, acidity, or spice in kimchi. Starting with small amounts and monitoring response is a sensible approach. Anyone with significant or persistent IBS symptoms should work with a clinician or registered dietitian rather than self-managing with dietary changes alone.
What is the difference between live cultures and probiotics?
“Live cultures” describes microorganisms that are alive in a food product. “Probiotics” is a more specific term requiring identified strains, adequate amounts, and demonstrated health benefits. All probiotics are live cultures, but not all live cultures qualify as probiotics. The distinction matters when evaluating product claims.
Can postbiotics be found in fermented foods?
Fermented foods contain microbial metabolites, organic acids, cell fragments, and other compounds that resemble postbiotic-like substances. However, a fermented food is not automatically a validated postbiotic product. The formal postbiotic definition requires characterization of the inanimate preparation and demonstrated health benefit. Most fermented foods have not been evaluated through that lens.
Is the fermented foods vs probiotics debate settled?
No, and it should not be framed as a competition. Fermented foods and probiotics serve different purposes and suit different contexts. The evidence for fermented foods as a dietary pattern tool is growing. The evidence for specific probiotic strains in specific situations is solid in some areas. These are complementary approaches, not competing ones.
This article is for informational purposes only and does not constitute medical advice. If you are experiencing persistent or concerning digestive symptoms, please consult a qualified healthcare professional.
Evidence and further reading
Modern Food Processing & Gut Chemistry reading path
- Start here: Modern Food Processing and Gut Health
- Deep dive: Ultra-Processed Foods, Emulsifiers and Microplastics
- Deep dive: Fermented Foods vs Probiotics vs Postbiotics (you are here)
- Deep dive: Resistant Starch and Prebiotic Fiber

