Foods Rich in Calcium: Best Sources, Daily Needs and Absorption Tips

Last updated: April 3, 2026
Quick Answer: The best foods rich in calcium includes dairy products (milk, yogurt, cheese), canned fish with bones (sardines, salmon), leafy greens (kale, bok choy, collard greens), almonds, seeds, and calcium-fortified foods like orange juice and plant-based milks. Most adults need 1,000–1,200 mg of calcium per day, and it’s entirely achievable through diet alone with the right food choices.
Key Takeaways
- Dairy products remain the most concentrated and bioavailable sources of calcium, but they’re far from the only option
- Canned sardines and salmon (eaten with bones) are among the most underrated calcium sources available
- Leafy greens like kale and bok choy provide meaningful calcium, but spinach is less effective due to high oxalate content that blocks absorption
- Calcium absorption depends heavily on vitamin D — without adequate vitamin D, your body cannot properly use the calcium you consume
- The recommended daily intake (RDI) is 1,000 mg for adults aged 19–50, rising to 1,200 mg for women over 50 and adults over 70 (per the National Institutes of Health)
- Calcium deficiency is linked to osteoporosis, muscle cramps, poor dental health, and in severe cases, cardiac complications
- Spreading calcium intake across meals (rather than consuming it all at once) improves absorption
- Fortified foods — including plant milks, cereals, and orange juice — are reliable options for people avoiding dairy
- Seeds, beans, figs, and almonds provide moderate calcium and are easy to add to everyday meals
- Calcium supplements are a backup, not a first choice — food sources come packaged with co-nutrients that aid absorption
What Is Calcium and Why Does Your Body Need It?
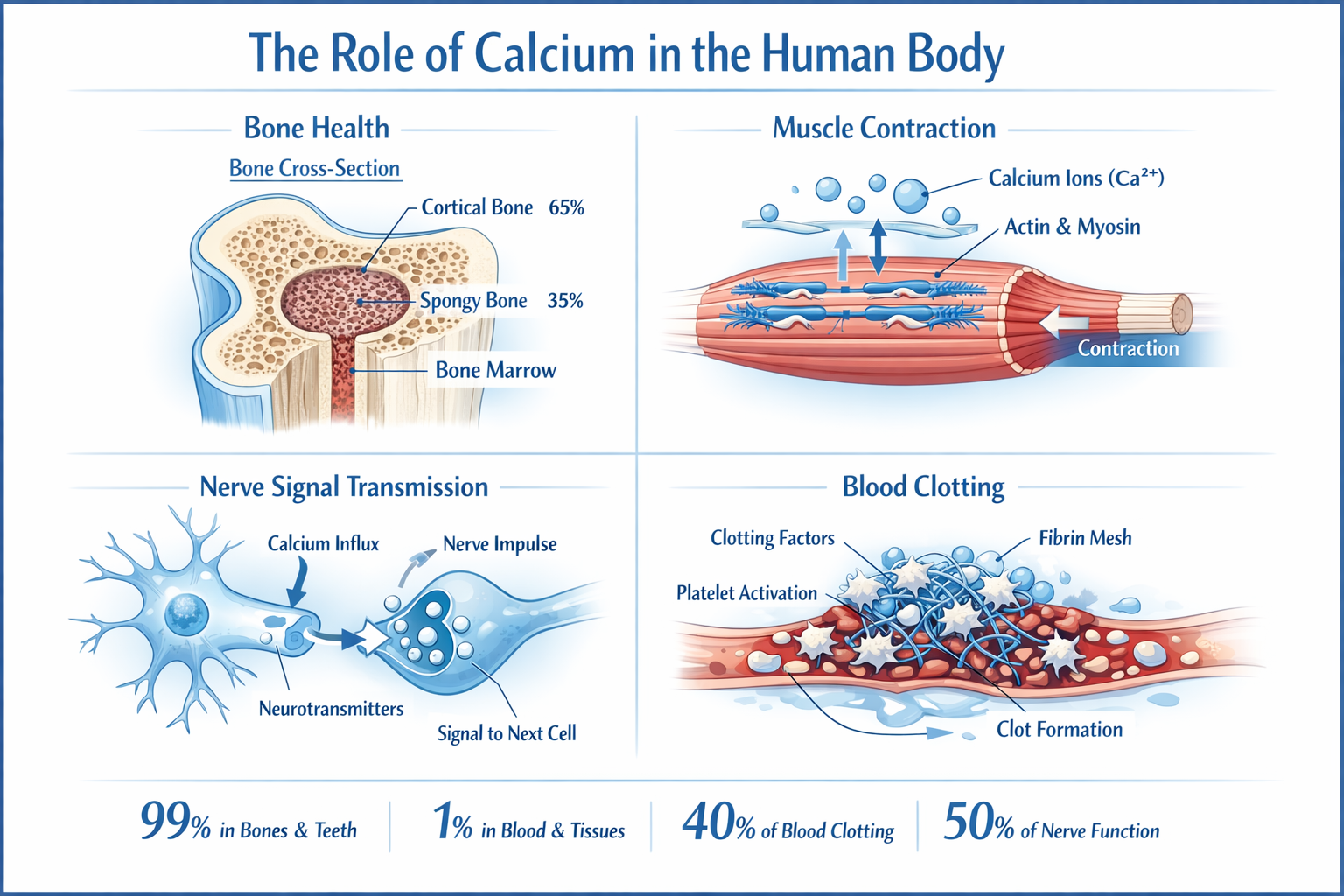
Calcium is the most abundant mineral in the human body, and it does far more than build bones. About 99% of the body’s calcium is stored in bones and teeth, where it provides structural strength. The remaining 1% circulates in the blood, muscles, and soft tissues — and that small fraction is critical. It regulates muscle contraction (including the heartbeat), enables nerve signal transmission, supports blood clotting, and triggers the release of hormones and enzymes.
When your dietary calcium intake falls short, your body doesn’t simply go without. It pulls calcium from your bones to maintain blood calcium levels — a process that, over time, weakens bone density and raises the risk of fractures and osteoporosis.
Calcium’s key roles in the body:
- Bone and tooth formation: Calcium is the primary structural mineral in bone tissue. Adequate intake during childhood, adolescence, and early adulthood builds peak bone mass, which acts as a reserve against age-related bone loss
- Muscle function: Every muscle contraction — from a bicep curl to a heartbeat — requires calcium ions. Low calcium can cause muscle cramps and spasms
- Nerve transmission: Calcium helps neurons fire correctly, enabling everything from reflexes to complex thought
- Blood clotting: Calcium is a co-factor in several steps of the coagulation cascade — the process that stops bleeding after injury
- Hormone secretion: Calcium triggers the release of insulin and other hormones from endocrine glands
- Blood pressure regulation: Research published by the National Institutes of Health notes that adequate calcium intake is associated with modest reductions in blood pressure, particularly in people who are deficient
Who is most at risk of calcium deficiency?
- Postmenopausal women (estrogen decline accelerates bone loss)
- Adults over 70
- People who avoid dairy without replacing it with other calcium sources
- Those with lactose intolerance or milk allergies who don’t use fortified alternatives
- People with vitamin D deficiency (which impairs calcium absorption regardless of intake)
- Individuals with inflammatory bowel disease or celiac disease (absorption is compromised)
How Much Calcium Do You Actually Need Per Day?
The daily calcium requirement varies by age and life stage. Getting the right amount matters — both deficiency and excessive supplementation carry risks.
According to the National Institutes of Health (NIH) Office of Dietary Supplements, the Recommended Dietary Allowances (RDAs) for calcium are:
| Age Group | RDA (mg/day) |
|---|---|
| Children 1–3 years | 700 mg |
| Children 4–8 years | 1,000 mg |
| Adolescents 9–18 years | 1,300 mg |
| Adults 19–50 years | 1,000 mg |
| Women 51–70 years | 1,200 mg |
| Men 51–70 years | 1,000 mg |
| Adults 71+ years | 1,200 mg |
| Pregnant/lactating teens | 1,300 mg |
| Pregnant/lactating adults | 1,000 mg |
Source: NIH Office of Dietary Supplements, 2024
A practical note on absorption: Your body absorbs calcium most efficiently in doses of 500 mg or less at a time. If you’re aiming for 1,000 mg daily, splitting intake between two or three meals is more effective than consuming it all in one sitting. Vitamin D, magnesium, and vitamin K2 all support calcium metabolism — so a diet rich in these co-nutrients makes your calcium intake work harder.
Which Dairy Foods Are Highest in Calcium?
Dairy products are the most concentrated and bioavailable sources of calcium in the typical Western diet. The calcium in dairy is well-absorbed — roughly 30–35% of the calcium in milk is absorbed by the body, according to NIH data.
Milk
One cup (240 ml) of cow’s milk provides approximately 300 mg of calcium — about 30% of the daily RDA for most adults. Whole, low-fat, and skim milk all contain similar calcium levels; the fat content doesn’t significantly affect calcium concentration. Milk also contains vitamin D (in fortified versions), phosphorus, and protein — all of which support bone health.
Choose milk if: You want a straightforward, well-absorbed calcium source with a broad nutrient profile. Low-fat milk works well for people managing their weight without sacrificing nutritional density.
Yogurt
Plain yogurt is one of the richest calcium sources per serving. A single cup of plain low-fat yogurt can provide 300–400 mg of calcium, depending on the brand. Greek yogurt tends to be slightly lower in calcium than regular yogurt because the straining process removes some whey. Yogurt also delivers probiotics that support gut health and digestion, making it a particularly well-rounded food.
Watch out for: Flavored yogurts often contain significant added sugar. Opt for plain yogurt and add fresh fruit or a drizzle of honey if needed.
Cheese
Hard cheeses are calcium-dense because the manufacturing process concentrates milk solids. Here’s how common cheeses compare per 1-ounce (28g) serving:
- Parmesan: ~330 mg calcium (one of the highest of any food per ounce)
- Cheddar: ~200 mg calcium
- Mozzarella: ~180 mg calcium
- Brie/Camembert: ~50–100 mg calcium (lower due to higher moisture content)
- Cottage cheese: ~70 mg per half-cup (lower concentration, but useful in larger portions)
Grated Parmesan is particularly useful as a calcium booster — a tablespoon or two sprinkled over pasta, salads, or soups adds meaningful calcium with minimal effort.
What Are the Best Non-Dairy Foods High in Calcium?
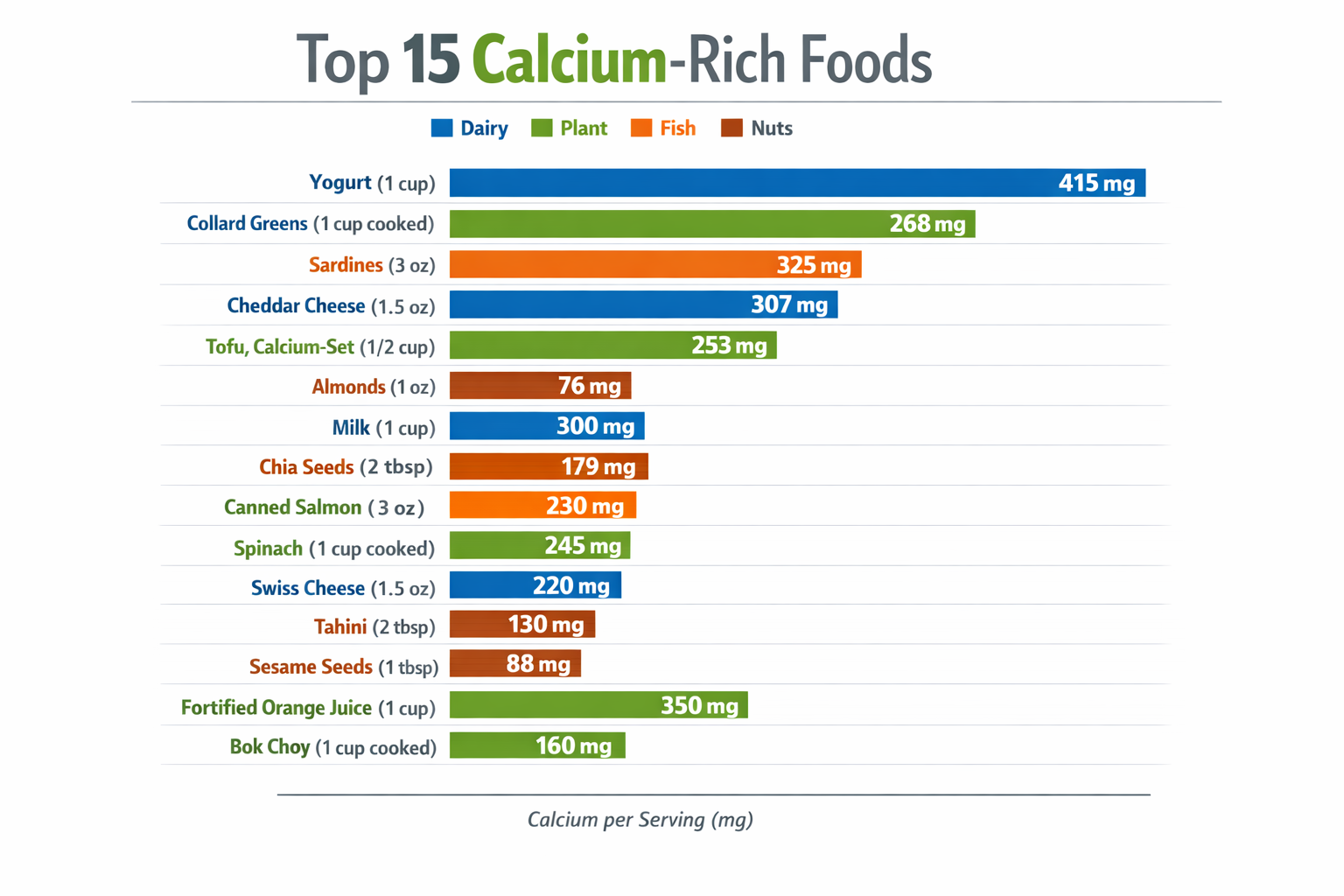
Non-dairy calcium sources are essential for people who are lactose intolerant, vegan, or simply looking to diversify their diet. Bioavailability varies across plant and animal sources, so it’s worth knowing which ones your body can actually use.
Canned Fish with Bones (Sardines and Salmon)
This is one of the most underrated calcium sources available. The key is eating the soft, edible bones — that’s where the calcium is concentrated. A 3.75-ounce can of sardines in oil provides approximately 350 mg of calcium, and a 3-ounce serving of canned salmon with bones delivers around 180–200 mg.
Beyond calcium, canned fish provides omega-3 fatty acids, protein, and vitamin D — a combination that directly supports bone health. Including canned salmon in healthy meals is one of the most efficient ways to hit both your calcium and omega-3 targets simultaneously.
Common mistake: Many people drain canned sardines and discard the bones. The bones are soft enough to eat and are the primary calcium source — don’t skip them.
Leafy Green Vegetables
Not all leafy greens are equal when it comes to calcium. The critical variable is oxalate content — oxalates bind to calcium in the gut and prevent absorption.
High calcium, low oxalates (good absorption):
- Kale: ~180 mg per cooked cup, with absorption rate around 49%
- Bok choy: ~160 mg per cooked cup, absorption rate around 54%
- Collard greens: ~260 mg per cooked cup, strong absorption
- Broccoli rabe: ~100 mg per cooked cup
- Turnip greens: ~200 mg per cooked cup
High calcium, high oxalates (poor absorption):
- Spinach: ~240 mg per cooked cup on paper, but absorption rate is only about 5% due to high oxalate content — making it a poor calcium source despite appearances
- Swiss chard: Similar issue
Practical tip: Cook your greens. Boiling leafy greens reduces oxalate content by 30–87%, improving calcium availability. For people focused on anti-inflammatory eating, leafy greens are valuable beyond calcium alone — they deliver vitamin K, magnesium, and antioxidants.
Seeds
Seeds are a convenient, plant-based calcium source that’s easy to add to any meal.
- Sesame seeds: 1 tablespoon provides approximately 88 mg of calcium — and tahini (sesame paste) is an excellent concentrated source
- Chia seeds: 1 ounce provides approximately 180 mg of calcium, plus fiber and omega-3s
- Poppy seeds: 1 tablespoon provides around 126 mg of calcium
- Sunflower seeds: Moderate calcium (~20 mg per ounce), but a useful addition alongside other sources
Add chia seeds to smoothies or overnight oats, use tahini in dressings and dips, and sprinkle sesame seeds over stir-fries and salads.
Almonds
Almonds are the most calcium-rich nut. A 1-ounce serving (about 23 almonds) provides approximately 76 mg of calcium, along with magnesium, vitamin E, and healthy fats. They’re a practical snack for people looking to boost calcium intake without adding meals. Almond butter is similarly useful — two tablespoons provide around 55–80 mg of calcium depending on the brand.
Legumes and Beans
White beans are among the best legume sources of calcium. A half-cup of cooked white beans provides approximately 130 mg of calcium. Other useful options include:
- Edamame: ~98 mg per half-cup cooked
- Black beans: ~46 mg per half-cup cooked
- Chickpeas: ~40 mg per half-cup cooked
- Canned baked beans: Variable, but often 80–130 mg per half-cup; check labels as calcium content differs by brand
Beans also provide fiber, plant protein, and iron — making them a strong choice for a balanced, healthy diet.
Figs
Dried figs are a surprisingly good calcium source. Five dried figs provide approximately 135 mg of calcium, along with potassium, fiber, and antioxidants. Fresh figs contain less calcium per serving (around 35 mg per medium fig), but are still a worthwhile addition to the diet. Figs also have mild anti-inflammatory properties, which complements their bone health benefits.
Rhubarb
Cooked rhubarb provides around 105–175 mg of calcium per cup, but it’s worth noting that rhubarb also contains oxalic acid, which reduces absorption somewhat. It’s a useful supplementary source rather than a primary one. Rhubarb also provides vitamin K and fiber.
What Are Calcium-Fortified Foods and Are They Effective?
Calcium-fortified foods have calcium added during manufacturing, and they can be just as effective as naturally occurring calcium sources — sometimes more so, because the added calcium is often in a highly bioavailable form.
Common calcium-fortified foods:
- Plant-based milks (soy, almond, oat, rice): Most brands are fortified to match cow’s milk, providing 280–300 mg per cup. Shake the carton before pouring — calcium can settle at the bottom
- Fortified orange juice: One cup typically provides 300–350 mg of calcium, comparable to dairy milk
- Fortified breakfast cereals: Calcium content varies widely — check the label. Some provide 100–1,000 mg per serving
- Fortified tofu: Tofu made with calcium sulfate is an excellent source, providing 200–400 mg per half-cup depending on firmness
- Fortified bread and flour: Common in many countries; provides background calcium throughout the day
Are fortified foods as good as natural sources? Research suggests that calcium from fortified foods is absorbed at rates similar to dairy calcium (around 30%). They’re a legitimate strategy, not a compromise — especially for vegans, people with lactose intolerance, or anyone who simply doesn’t eat much dairy.
How Does Calcium Affect Bone Health and Osteoporosis Risk?
Adequate calcium intake across the lifespan is one of the most evidence-backed strategies for reducing osteoporosis risk. Osteoporosis affects an estimated 200 million people worldwide (International Osteoporosis Foundation, 2023), and dietary calcium deficiency is a significant contributing factor.
How bone calcium works over a lifetime:
- Childhood to early adulthood (up to ~age 30): This is the bone-building window. Higher calcium intake during these years directly increases peak bone mass — the higher your peak, the more reserve you have against age-related loss
- Ages 30–50: Bone mass is relatively stable if calcium intake is adequate. Deficiency during this period accelerates the natural remodeling process toward net bone loss
- Post-menopause and older adulthood: Estrogen decline in women and age-related changes in both sexes accelerate bone loss. Calcium intake of 1,200 mg/day, combined with vitamin D, is recommended to slow this process
Calcium alone isn’t enough for bone health. Vitamin D is essential for calcium absorption in the intestine. Without adequate vitamin D (the NIH recommends 600–800 IU daily for most adults), even a high-calcium diet won’t fully protect bones. Weight-bearing exercise, adequate protein, and vitamin K2 also contribute to bone density.
Common mistake: Relying on calcium supplements without addressing vitamin D status. If your vitamin D is low, your body cannot efficiently absorb the calcium you’re taking in — whether from food or supplements.
Good dental health is also linked to calcium status. Calcium supports the mineralization of tooth enamel, reducing the risk of decay and gum disease. If you’re concerned about gum health, calcium intake is a foundational factor worth reviewing.
How Can You Reach Your Daily Calcium Target Through Food Alone?

Reaching 1,000 mg of calcium daily through food is achievable with some planning. Here’s a practical example of how a day’s eating might add up:
Sample 1,000 mg calcium day (non-dairy-heavy):
| Meal | Food | Approx. Calcium |
|---|---|---|
| Breakfast | 1 cup fortified oat milk + chia seeds in oatmeal | ~350 mg |
| Lunch | Canned sardines on whole grain bread + kale salad | ~400 mg |
| Snack | 1 oz almonds + 5 dried figs | ~210 mg |
| Dinner | White bean and vegetable stew | ~130 mg |
| Total | ~1,090 mg |
Sample 1,000 mg calcium day (dairy-included):
| Meal | Food | Approx. Calcium |
|---|---|---|
| Breakfast | 1 cup plain yogurt with fruit | ~350 mg |
| Lunch | Cheese and vegetable wrap (1 oz cheddar) | ~200 mg |
| Snack | 1 glass milk (240 ml) | ~300 mg |
| Dinner | Salmon fillet + broccoli | ~200 mg |
| Total | ~1,050 mg |
Practical tips for hitting your calcium target:
- Keep canned sardines or salmon in your pantry as a reliable backup source
- Use tahini in salad dressings and dips — it’s calcium-dense and versatile
- Choose fortified plant milk if you don’t consume dairy regularly
- Add chia seeds to smoothies, yogurt, or overnight oats — they’re virtually tasteless and provide meaningful calcium
- Sprinkle Parmesan or sesame seeds over cooked vegetables to add calcium without changing the meal structure
- Pair calcium-rich foods with vitamin D sources (fatty fish, eggs, fortified foods) to maximize absorption
Should You Take Calcium Supplements?
Calcium supplements are a reasonable option when diet consistently falls short, but they’re not a straightforward replacement for food sources. Food comes packaged with co-nutrients — vitamin D, magnesium, vitamin K, protein — that work together with calcium. Supplements deliver calcium in isolation.
When supplements make sense:
- Documented deficiency confirmed by a healthcare provider
- Conditions that impair absorption (Crohn’s disease, celiac disease, bariatric surgery)
- Postmenopausal women who cannot meet needs through diet
- Strict vegans who don’t consume fortified foods consistently
Supplement types:
- Calcium carbonate: Highest calcium concentration (40%), cheapest, but requires stomach acid — take with food
- Calcium citrate: Lower concentration (21%) but better absorbed, especially by older adults or those taking acid-reducing medications — can be taken with or without food
Upper tolerable intake limit: The NIH sets the tolerable upper limit at 2,500 mg/day for adults aged 19–50 and 2,000 mg/day for those over 50. Exceeding these levels long-term may increase the risk of kidney stones and, based on some research, potentially cardiovascular calcification — though evidence on the latter remains debated. Always discuss supplementation with your doctor before starting.
Frequently Asked Questions About Food High in Calcium
Q: What single food has the most calcium per serving?
A: Parmesan cheese is one of the most calcium-dense foods by weight, providing around 330 mg per ounce. Among beverages, fortified orange juice and milk both deliver approximately 300 mg per cup. Among plant foods, cooked collard greens and fortified tofu are top performers.
Q: Is spinach a good source of calcium?
A: Despite its high calcium content on paper (~240 mg per cooked cup), spinach is a poor calcium source in practice. Its high oxalate content binds to calcium in the gut, resulting in an absorption rate of only about 5%. Kale, bok choy, and collard greens are far better options.
Q: Can you get enough calcium without eating dairy?
A: Yes. A combination of fortified plant milks, canned fish with bones, leafy greens (kale, bok choy, collard greens), tofu made with calcium sulfate, seeds, almonds, and legumes can fully meet daily calcium needs without any dairy.
Q: Does cooking vegetables reduce their calcium content?
A: Cooking can reduce total calcium slightly, but it also reduces oxalate content — which actually improves the amount of calcium your body can absorb from high-oxalate vegetables like spinach and chard. For low-oxalate greens like kale, both raw and cooked forms are good sources.
Q: What blocks calcium absorption?
A: Several factors reduce calcium absorption: high oxalate foods (spinach, beet greens), high phytate foods (raw whole grains, legumes), excess sodium (increases calcium excretion in urine), very high fiber intake, caffeine in large amounts, and vitamin D deficiency. Spacing calcium intake across meals and ensuring adequate vitamin D helps counteract most of these.
Q: How much calcium is in an egg?
A: One large egg contains approximately 25–28 mg of calcium — a modest amount. Eggs are not a significant calcium source, but they do provide vitamin D, which supports calcium absorption. For a deeper look at egg nutrition, see our guide on calories and nutrition in hard-boiled eggs.
Q: Are calcium supplements better than food sources?
A: Food sources are generally preferable because they deliver calcium alongside co-nutrients that aid absorption and bone health. Supplements are useful when dietary intake is consistently inadequate, but should be used at appropriate doses under medical guidance.
Q: Does caffeine really deplete calcium?
A: Caffeine causes a small increase in calcium excretion through urine — roughly 2–3 mg of calcium per cup of coffee. For most people with adequate calcium intake, this is insignificant. It becomes more relevant for people who consume very large amounts of caffeine and have low calcium intake simultaneously.
Q: What are signs of calcium deficiency?
A: Early signs include muscle cramps, numbness or tingling in fingers, fatigue, and brittle nails. Long-term deficiency leads to reduced bone density and increased fracture risk. Severe deficiency (hypocalcemia) can cause seizures, cardiac arrhythmias, and tetany — but this level is rare in otherwise healthy people eating a varied diet.
Q: Is plant-based milk as good as cow’s milk for calcium?
A: Most commercial plant-based milks are fortified to match cow’s milk (approximately 300 mg per cup), making them comparable in calcium content. However, shake the carton before use — calcium can settle. Absorption rates are similar to dairy for most fortified plant milks.
Q: Can children get enough calcium from food?
A: Yes, and it’s important that they do — childhood and adolescence are the peak bone-building years. Dairy, fortified foods, leafy greens, and fish with bones are all appropriate sources. Adolescents need 1,300 mg daily, which requires deliberate food choices or fortified foods if dairy is limited.
Q: Does calcium help with weight management?
A: Some research suggests that adequate calcium intake — particularly from dairy — may modestly support fat metabolism, but the evidence is not strong enough to use calcium as a weight loss strategy. The primary reasons to prioritize calcium remain bone health, muscle function, and cardiovascular regulation.
Related Reading
- Anti-Inflammatory Foods: The Ultimate Guide — many calcium-rich foods also have anti-inflammatory properties
- Healthy Meals for Weight Loss — how to build calcium-rich meals that also support a healthy weight
- Gut Health and Digestive Wellness — gut health directly affects how well you absorb calcium and other minerals
- A Comprehensive Guide to Modern Diets — how different dietary patterns affect calcium intake and bone health
Sources
- National Institutes of Health, Office of Dietary Supplements — Calcium Fact Sheet for Health Professionals (2024): https://ods.od.nih.gov/factsheets/Calcium-HealthProfessional/
- International Osteoporosis Foundation — Osteoporosis Facts and Statistics (2023): https://www.osteoporosis.foundation
- USDA FoodData Central — Nutrient database for calcium content per food (2024): https://fdc.nal.usda.gov/



