Synergistic Plant Toxin Effects: How Oxalates Amplify Lectin Damage in the Gut

Last updated: May 10, 2026
Quick Answer: Oxalates and lectins are two of the most studied plant defense compounds. When consumed together in large amounts, particularly by people with compromised gut barriers or low dietary calcium, the evidence suggests they may interact in ways that are more damaging than either compound alone. However, the picture is more nuanced than most online sources admit — cooking, food pairing, and overall diet context dramatically change the risk profile.
Key Takeaways
- Synergistic plant toxin effects occur when multiple anti-nutrients act together, producing gut damage that is not simply the sum of their individual effects [3]
- Lectins can damage the gut lining, potentially making it easier for oxalates (and other compounds) to enter circulation at higher rates [3]
- A 2025 peer-reviewed study found that chronic lectin exposure in mice elevated oxidative stress markers and triggered neuroinflammatory pathways [2]
- Cooking reduces lectin content by up to 94% and oxalate content by up to 87%, making food preparation the most practical mitigation tool [1]
- Population-level data from Mediterranean and DASH diet research contradicts the idea that lectin-rich diets are broadly harmful [1]
- Oxalate-related kidney stone risk is largely conditional on low dietary calcium intake, not oxalate consumption alone [1]
- The “food matrix” — the full nutritional context of a meal — matters more than any single anti-nutrient in isolation [1]
- Most people eating a varied, well-cooked diet are unlikely to experience clinically significant synergistic toxin effects
- Those at higher risk include people with existing gut conditions, very high intakes of raw high-oxalate or high-lectin foods, and those with low calcium diets
In this guide
- What Are Oxalates and Lectins, and Why Do They Matter Together?
- How Do Lectins Damage the Gut Lining?
- How Do Oxalates Amplify Lectin Damage in the Gut?
- What Does the Research Actually Show — and Where Does It Fall Short?
- What Symptoms Might Suggest Oxalate-Lectin Synergy Is a Problem for You?
- How to Reduce Synergistic Plant Toxin Effects Through Food Preparation
- Does the Overall Diet Pattern Matter More Than Individual Anti-Nutrients?
- Practical Mitigation Protocol: A Stepwise Approach
- Frequently Asked Questions
- Conclusion: What This Means in Practice
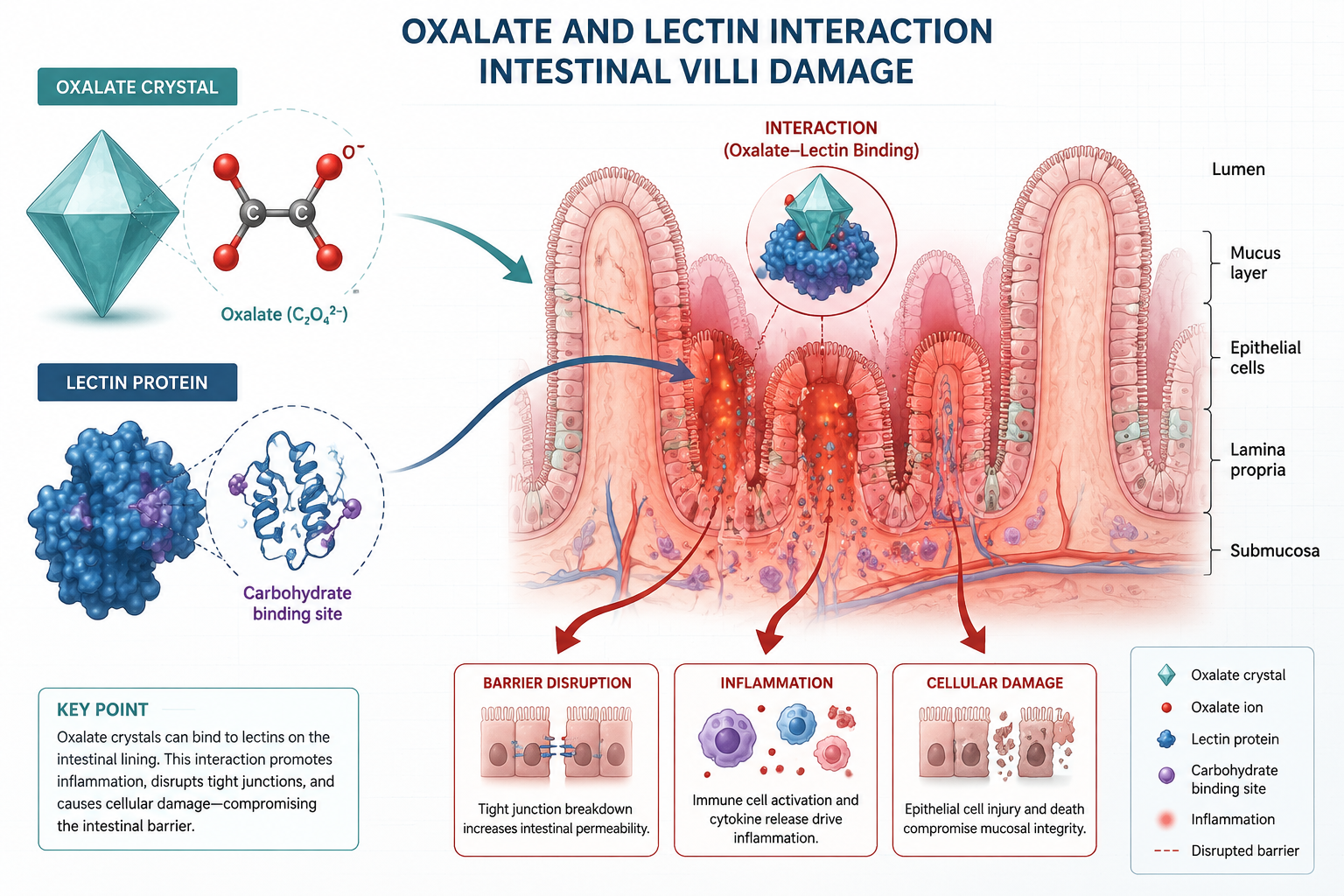
What Are Oxalates and Lectins, and Why Do They Matter Together?
Oxalates and lectins are plant defense compounds that most people consume daily without obvious harm. The concern arises when they are consumed in large amounts, in raw or undercooked form, or in the context of a gut that is already under stress.
Oxalates are naturally occurring organic acids found in spinach, beets, almonds, sweet potatoes, and many other plant foods. Their primary role in plants is structural and defensive. In the human body, oxalates bind to minerals like calcium and magnesium, forming insoluble crystals that can accumulate in tissues and, in susceptible individuals, contribute to kidney stone formation [1].
Lectins are carbohydrate-binding proteins found in legumes, grains, nightshades, and dairy. They evolved as a plant defense mechanism against insects and fungi. In humans, lectins bind to sugar residues on the surface of cells lining the gut, which is where most of the documented biological activity occurs [3].
Here’s the real issue: when you look at these compounds in isolation, the risk for most healthy adults eating cooked food is relatively low. But the research on synergistic plant toxin effects — how oxalates amplify lectin damage in the gut — suggests that studying them separately may give an incomplete picture of what happens when they are consumed together, particularly in raw or minimally processed form [3].
For a broader look at how plant compounds affect the body, see this detailed breakdown of what plant toxins actually do to your body.
How Do Lectins Damage the Gut Lining?
Lectins cause gut damage primarily by binding to the cells of the small intestine — specifically the villi and crypt cells that are responsible for nutrient absorption. This binding can trigger cell death, shorten villi, and reduce the gut’s overall digestive capacity [3].
The most studied mechanism involves a toxic lectin called phytohaemagglutinin (PHA), found in raw kidney beans. Research shows that lectins can enter the bloodstream three to four times more readily than other food proteins, partly because they survive digestion better and partly because they actively disrupt the tight junctions between gut cells — the structures that normally keep the gut barrier intact [3].
This is what connects to the broader concept of leaky gut: when tight junctions are compromised, the gut becomes more permeable, and compounds that would normally stay in the digestive tract — including oxalates — can pass into circulation more easily.
Key lectin damage mechanisms:
- Binding to gut epithelial cells, disrupting normal cell turnover
- Triggering local immune responses and inflammation
- Reducing the surface area available for nutrient absorption
- Increasing intestinal permeability, which may allow other compounds to enter the bloodstream
A June 2025 study published in Nutritional Neuroscience added another layer to this picture. Researchers found that chronic exposure to BS-Gal lectin from bean sprouts induced oxidative stress, metabolic dysfunction, and neuroinflammation in mouse brain regions [2]. Specifically, the study documented elevated hydrogen peroxide, nitric oxide, and malondialdehyde levels — all markers of oxidative damage — alongside activation of NF-κB and pro-inflammatory cytokines including TNF-α, IL-6, and IL-1β [2].
That is a strong claim and needs strong proof. The 2025 study used animal models, not human trials. The findings are worth noting, but they should not be extrapolated directly to human dietary patterns without further research.
How Do Oxalates Amplify Lectin Damage in the Gut?
The synergistic plant toxin effects of oxalates and lectins working together are not fully mapped in human clinical trials — let’s be clear about that. But the mechanistic logic is coherent, and the animal and in-vitro research gives a reasonable basis for concern in specific populations.
Here is how the amplification pathway likely works:
Step 1 — Lectins compromise the gut barrier. As described above, lectins bind to gut epithelial cells, disrupt tight junctions, and increase intestinal permeability [3].
Step 2 — A more permeable gut absorbs more oxalates. Normally, most dietary oxalates are bound to calcium in the gut and excreted in stool. But when the gut lining is compromised, more free oxalate can be absorbed into the bloodstream — a condition sometimes called “enteric hyperoxaluria” in clinical contexts.
Step 3 — Elevated oxalate burden creates systemic stress. Once in circulation, oxalates can form calcium oxalate crystals in tissues, promote oxidative stress, and potentially trigger inflammatory responses in the kidneys, joints, and other organs.
Step 4 — The combined effect exceeds the sum of the parts. Research indicates that when anti-nutrients like lectins, protease inhibitors, and saponins are tested together, the damage is “not simply additive but synergistic” [3]. The same logic may apply to the oxalate-lectin pairing, though direct human evidence for this specific combination is limited.
Who is most likely to experience this effect?
| Risk Factor | Why It Matters |
|---|---|
| Existing gut inflammation (IBS, IBD, Crohn’s) | Gut barrier already compromised before exposure |
| High intake of raw high-lectin foods | Cooking reduces lectins by up to 94% [1] |
| High intake of raw high-oxalate foods | Boiling reduces oxalates by up to 87% [1] |
| Low dietary calcium | Calcium binds oxalates in the gut, reducing absorption [1] |
| Chronic stress or poor sleep | Both impair gut barrier integrity independently |
For people without these risk factors, eating cooked legumes and leafy greens as part of a balanced diet is unlikely to produce clinically significant synergistic damage.
What Does the Research Actually Show — and Where Does It Fall Short?
We need to separate fact from hype here, because this topic attracts strong opinions on both sides.
The case for concern:
- Lectins demonstrably damage gut epithelial cells in animal models and in-vitro studies [3]
- The 2025 Nutritional Neuroscience study showed neuroinflammatory effects from chronic lectin exposure in mice [2]
- Anti-nutrients tested in combination show synergistic, not merely additive, effects [3]
- Increased intestinal permeability from lectins provides a plausible mechanism for enhanced oxalate absorption
The case for caution about overclaiming:
- A comprehensive 2014 review of 304 meta-analyses and systematic reviews found that plant foods high in oxalates, lectins, and phytates are actually protective against diet-related chronic diseases including diabetes and cardiovascular disease [1]
- Mediterranean and DASH diets — both high in lectin-containing foods — are consistently associated with improved gut health and reduced inflammation at the population level [1]
- Most damage studies use isolated, concentrated compounds or raw foods at doses far above typical dietary intake [3]
- Oxalate-related kidney stone risk is largely conditional on low calcium intake, not high oxalate intake alone [1]
The stronger evidence points to this conclusion: context matters enormously. A raw spinach and raw kidney bean smoothie consumed daily by someone with IBS and a low-calcium diet is a very different scenario from a bowl of cooked lentil soup with leafy greens and a glass of milk.
In plain English: the synergistic damage hypothesis is mechanistically plausible and supported by some animal research, but it has not been confirmed in well-designed human trials at typical dietary doses.

What Symptoms Might Suggest Oxalate-Lectin Synergy Is a Problem for You?
There is no clinical test that specifically identifies “oxalate-lectin synergistic gut damage.” But certain symptom patterns may suggest that anti-nutrient load is contributing to gut problems, particularly when they appear or worsen after eating high-oxalate, high-lectin meals.
Gut-related symptoms to watch for:
- Bloating, cramping, or gas that consistently follows meals containing raw or undercooked legumes and leafy greens
- Changes in stool consistency or frequency linked to specific foods
- Persistent gut discomfort that does not resolve with standard dietary adjustments
Systemic symptoms that may reflect increased gut permeability:
- Joint pain or stiffness (oxalate crystal deposition is one possible contributor)
- Brain fog following high-plant-food meals
- Skin reactions or unexplained fatigue
A practical note: these symptoms are non-specific. They can be caused by dozens of other factors, including gut microbiome imbalances, food sensitivities unrelated to anti-nutrients, or chronic stress. Do not assume oxalate-lectin synergy is the cause without ruling out other explanations first.
If symptoms are significant or persistent, working with a registered dietitian or gastroenterologist is the right starting point — not self-diagnosis based on anti-nutrient theory.
How to Reduce Synergistic Plant Toxin Effects Through Food Preparation
The most practical and evidence-supported approach to managing synergistic plant toxin effects is straightforward: cook your food properly. The evidence on this is clear and consistent.
Lectin reduction through cooking:
- Boiling legumes for at least 10 minutes destroys PHA and most other lectins [1]
- Pressure cooking is even more effective and faster
- Sprouting reduces lectin content, though it does not eliminate it entirely
- Fermentation (as in sourdough or fermented legumes) further reduces lectin activity
Cooking reduces lectin content by up to 94% [1]. That single step eliminates most of the risk for most people.
Oxalate reduction through cooking:
- Boiling high-oxalate vegetables (spinach, beets, Swiss chard) for 12 minutes reduces oxalate content by up to 87% [1]
- Discarding the cooking water is important — oxalates leach into it
- Steaming is less effective than boiling for oxalate reduction
Food pairing to reduce oxalate absorption:
- Consuming calcium-rich foods alongside high-oxalate foods binds oxalates in the gut before they can be absorbed
- Dairy products, fortified plant milks, or calcium-set tofu are practical options
- This is why a balanced vegetarian diet, despite being higher in oxalates, has been found to be useful for kidney stone prevention [1]
Practical preparation checklist:
- ✅ Soak dried legumes for 8–12 hours before cooking
- ✅ Discard soaking water and rinse before boiling
- ✅ Boil legumes at a full rolling boil for at least 10 minutes
- ✅ Boil high-oxalate greens and discard cooking water
- ✅ Pair high-oxalate meals with a calcium source
- ✅ Avoid large amounts of raw spinach, raw kidney beans, or raw beet greens as dietary staples
- ✅ Consider fermented versions of grain and legume products where available
Does the Overall Diet Pattern Matter More Than Individual Anti-Nutrients?
Yes — and this is probably the most important point in the entire discussion.
The research consistently shows that the “food matrix” — the full nutritional context of what you eat — is more important than any single compound within it [1]. A diet built around whole, cooked plant foods, adequate protein, healthy fats, and sufficient calcium operates very differently from a diet built around raw, concentrated plant extracts or poorly prepared legumes.
This is why population studies on Mediterranean and DASH diets — both of which are high in lectin-containing foods — show benefits rather than harm [1]. The anti-nutrients in these diets exist alongside fibre, polyphenols, vitamins, minerals, and fermentation products that collectively support gut health rather than undermine it.
For practical guidance on building an anti-inflammatory eating pattern, the best anti-inflammatory foods for gut health guide covers the evidence well. And if you are interested in specific compounds that actively support the gut, the probiotics vs prebiotics guide is a useful companion read.
The main takeaway is this: optimising individual anti-nutrients while ignoring overall diet quality is working on the wrong problem. A sensible starting point is to eat a varied diet, cook your food properly, ensure adequate calcium intake, and address gut health issues with professional guidance if symptoms are persistent.
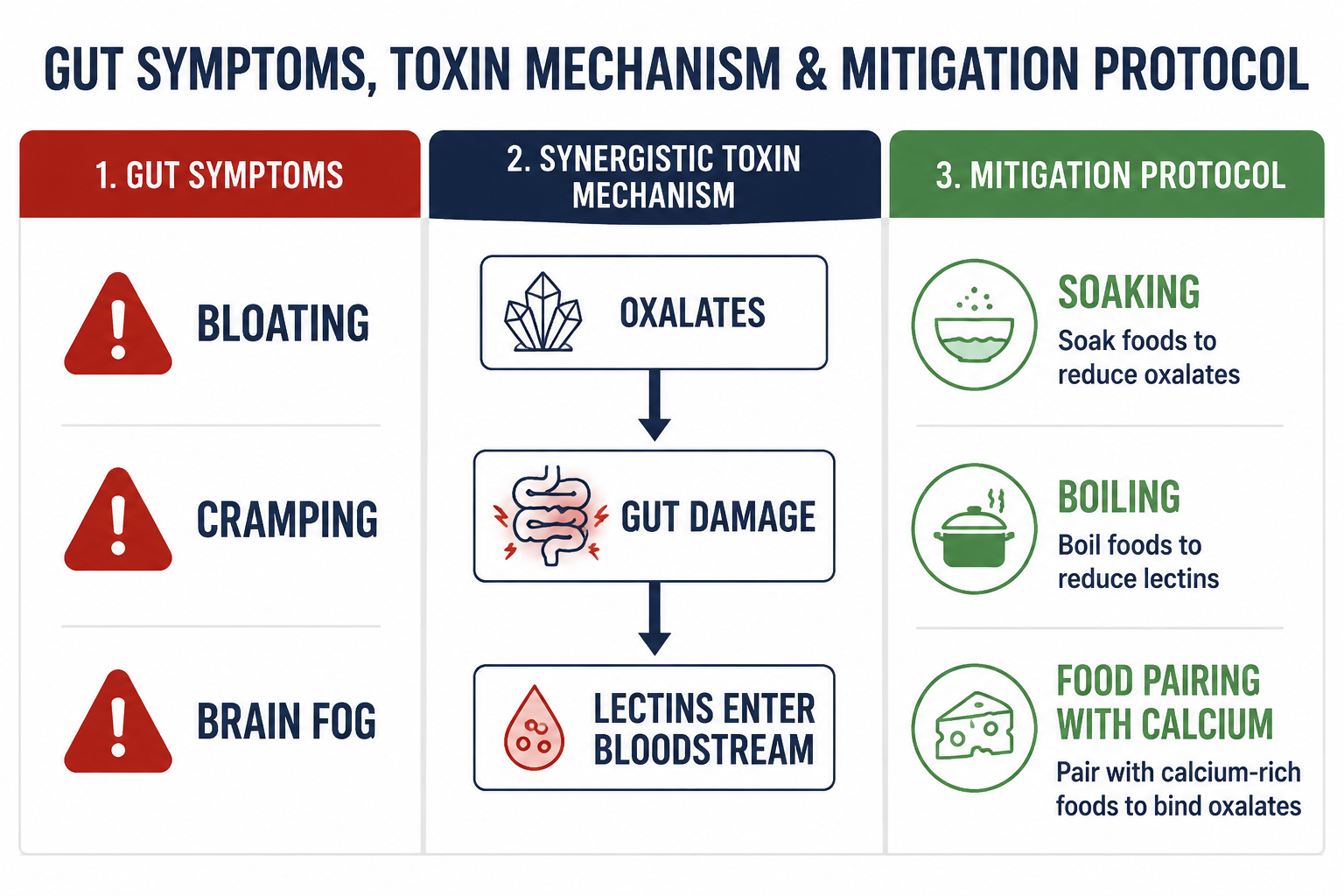
Practical Mitigation Protocol: A Stepwise Approach
Let’s keep this practical. If you are concerned about synergistic plant toxin effects — particularly the combination of oxalates amplifying lectin damage in the gut — here is a stepwise approach based on current evidence.
Step 1: Assess your actual risk
Ask yourself:
- Do you have a diagnosed gut condition (IBS, IBD, Crohn’s, coeliac)?
- Do you regularly eat large amounts of raw legumes or raw high-oxalate greens?
- Is your calcium intake consistently low?
- Do you have a history of kidney stones?
If none of these apply, your risk is low and the changes needed are minimal.
Step 2: Prioritise cooking methods
Boiling and pressure cooking are your most effective tools. They address both lectin and oxalate content simultaneously and require no special equipment beyond a pot and water [1].
Step 3: Pair foods strategically
Add a calcium source to high-oxalate meals. This is not complicated — a glass of milk, some cheese, or calcium-set tofu alongside your spinach salad does the job.
Step 4: Monitor symptoms honestly
Keep a simple food diary for two to three weeks. Note what you ate and how you felt. Look for patterns, not single incidents. If symptoms improve when you reduce raw high-lectin and high-oxalate foods and worsen when you reintroduce them, that is useful information.
Step 5: Seek professional input if needed
If symptoms are significant, persistent, or affecting quality of life, work with a gastroenterologist or registered dietitian. Self-managing gut conditions based on anti-nutrient theory alone is not a substitute for proper diagnosis.
Frequently Asked Questions
Q: Are synergistic plant toxin effects a real, proven phenomenon?
A: The synergistic interaction between anti-nutrients is documented in animal and in-vitro research, with lectins and other compounds showing combined effects greater than their individual impacts [3]. Direct human clinical evidence for the specific oxalate-lectin combination is limited. The mechanism is plausible, but the effect at typical dietary doses in healthy people has not been confirmed in controlled human trials.
Q: Which foods are highest in both oxalates and lectins?
A: Most foods are high in one or the other, not both. Spinach and beets are high in oxalates; kidney beans and wheat are high in lectins. A meal combining raw spinach with raw or undercooked kidney beans would represent a high combined load of both compounds.
Q: Does cooking really eliminate the risk?
A: Cooking dramatically reduces the risk. Boiling reduces lectins by up to 94% and oxalates by up to 87% [1]. It does not eliminate all anti-nutrient activity, but it reduces it to levels that are unlikely to cause harm in most healthy adults.
Q: Can oxalates cause gut damage on their own?
A: Oxalates are not primarily a gut-damaging compound in the same way lectins are. Their main documented risk is contributing to kidney stone formation in susceptible individuals, particularly when dietary calcium is low [1]. The amplification concern is that a lectin-compromised gut may absorb more oxalates than a healthy gut would.
Q: Is the Mediterranean diet safe given its lectin content?
A: Yes, based on current population-level evidence. Mediterranean and DASH diets are consistently associated with improved gut health and reduced chronic disease risk despite being high in lectin-containing foods [1]. The foods in these diets are typically well-cooked and consumed within a nutritionally balanced framework.
Q: Should people with IBS avoid high-lectin and high-oxalate foods?
A: People with IBS often do better with a modified diet, but the specific anti-nutrients to target depend on individual triggers. A low-FODMAP approach is better supported by clinical evidence for IBS than an anti-lectin or anti-oxalate approach. Working with a dietitian is the most reliable path.
Q: What did the 2025 lectin study actually find?
A: A study published in Nutritional Neuroscience in June 2025 found that chronic dietary exposure to BS-Gal lectin from bean sprouts induced oxidative stress markers, metabolic dysfunction, and neuroinflammatory pathways in mice [2]. The findings are notable but were conducted in animal models, not humans, and should not be directly extrapolated to typical human dietary patterns.
Q: Is oxalate sensitivity a real condition?
A: Some clinicians and researchers recognise “oxalate sensitivity” as a functional issue, particularly in people with gut conditions that impair normal oxalate metabolism. However, it is not a formally recognised diagnosis in mainstream medicine, and the evidence base is still developing. If you suspect it, work with a healthcare professional rather than self-diagnosing.
Q: Does calcium supplementation help reduce oxalate absorption?
A: Calcium taken with meals binds dietary oxalates in the gut, reducing absorption. This is the basis for using calcium supplements as part of kidney stone prevention protocols. Food sources of calcium are generally preferred over supplements for this purpose, as the timing with meals is easier to manage.
Q: Are nuts a significant source of both oxalates and lectins?
A: Nuts contain moderate amounts of both compounds, along with other anti-nutrients like phytates. However, the overall anti-nutrient content of nuts is generally considered low relative to their nutritional benefits, and the evidence does not support avoiding nuts for anti-nutrient reasons in healthy individuals [4].
Conclusion: What This Means in Practice
The concept of synergistic plant toxin effects — specifically how oxalates may amplify lectin damage in the gut — is a legitimate area of scientific inquiry. The mechanistic logic is sound: lectins compromise gut barrier integrity, and a compromised gut may absorb more oxalates than it otherwise would. Some animal research supports the idea that anti-nutrients in combination produce effects beyond their individual contributions [3].
At the same time, the population-level evidence is clear: diets high in plant foods, including those containing lectins and oxalates, are associated with better health outcomes, not worse ones [1]. The Mediterranean diet is not making people sick. Cooked lentils are not a public health hazard.
The nuance sits in the details: raw versus cooked, high dose versus moderate dose, compromised gut versus healthy gut, low calcium versus adequate calcium. These conditions change the risk profile substantially.
The practical takeaway:
- Cook legumes and high-oxalate vegetables properly — this is the single most effective step
- Pair high-oxalate meals with calcium-rich foods
- If you have a gut condition, work with a professional rather than self-managing based on anti-nutrient theory
- Do not let concern about individual plant compounds distract from the bigger picture: overall diet quality, food variety, and gut health fundamentals matter more than any single compound
There is no magic in it. The basics still do the heavy lifting.
For more on how gut health connects to broader wellbeing, the gut-brain axis guide is worth reading alongside this article. And if you are looking at the broader landscape of anti-inflammatory foods for health, that context helps put anti-nutrients in their proper place within a whole-diet framework.
References
[1] Oxalates Phytates Lectins Myth Vs Reality – https://www.everydaynutrition.com.au/post/oxalates-phytates-lectins-myth-vs-reality
[2] PubMed — BS-Gal Lectin Neuroinflammation Study (2025) – https://pubmed.ncbi.nlm.nih.gov/40512724/
[3] Plants Bite Back — Weston A. Price Foundation – https://www.westonaprice.org/health-topics/vegetarianism-and-plant-foods/plants-bite-back/
[4] Are Nuts High In Anti-Nutrients — Nuts For Life – https://www.nutsforlife.com.au/resource/are-nuts-high-in-anti-nutrients/
