Antinutrients and Skin Health: How Tannins and Phytoestrogens Trigger Eczema Flares

Last updated: May 10, 2026
Quick Answer
Certain plant compounds — particularly tannins and phytoestrogens — can contribute to eczema flares in sensitive individuals by disrupting gut barrier function, promoting low-grade inflammation, and interfering with immune signalling. The connection is real but not universal: it depends on individual gut health, immune reactivity, and overall dietary load. This article explains the mechanisms, identifies the highest-risk foods, and outlines a practical 30-day protocol for testing whether dietary antinutrients are a factor in your skin symptoms.
Key Takeaways
- Antinutrients and skin health are connected through gut inflammation pathways, not direct skin contact
- Tannins can bind to proteins in the gut lining, reducing nutrient absorption and triggering localised immune responses
- Phytoestrogens (found in soy, flaxseed, and legumes) may disrupt hormonal signalling that influences skin barrier function
- Not everyone reacts to these compounds — individual gut microbiome composition plays a significant role
- Recent research [2] confirms that immune cell reactivity is a primary driver of eczema, and dietary factors can amplify or dampen that reactivity
- A structured elimination and reintroduction approach is the most reliable way to identify personal food triggers
- Cooking, soaking, and fermentation significantly reduce antinutrient load in most plant foods
- Stress hormones independently worsen eczema flares [1][3], meaning diet is one piece of a larger picture
- Anti-inflammatory foods can actively support skin recovery alongside any elimination approach
- Professional medical guidance matters — this article is educational, not a substitute for dermatological care
In this guide
- What Are Antinutrients and Why Do They Matter for Skin?
- How Do Tannins Contribute to Eczema Flares?
- How Do Phytoestrogens Affect Skin and Eczema?
- What Does the Research Actually Say About Diet and Eczema Triggers?
- Which Foods Are Most Likely to Trigger Eczema Through Antinutrient Pathways?
- The Gut-Skin Axis: Why Your Digestive Health Determines Your Skin’s Response
- The 30-Day Skin Clearance Protocol: A Practical Framework
- Practical Ways to Reduce Antinutrient Load Without Eliminating Healthy Foods
- FAQ: Antinutrients, Tannins, Phytoestrogens, and Eczema
- Conclusion: What Actually Matters Here
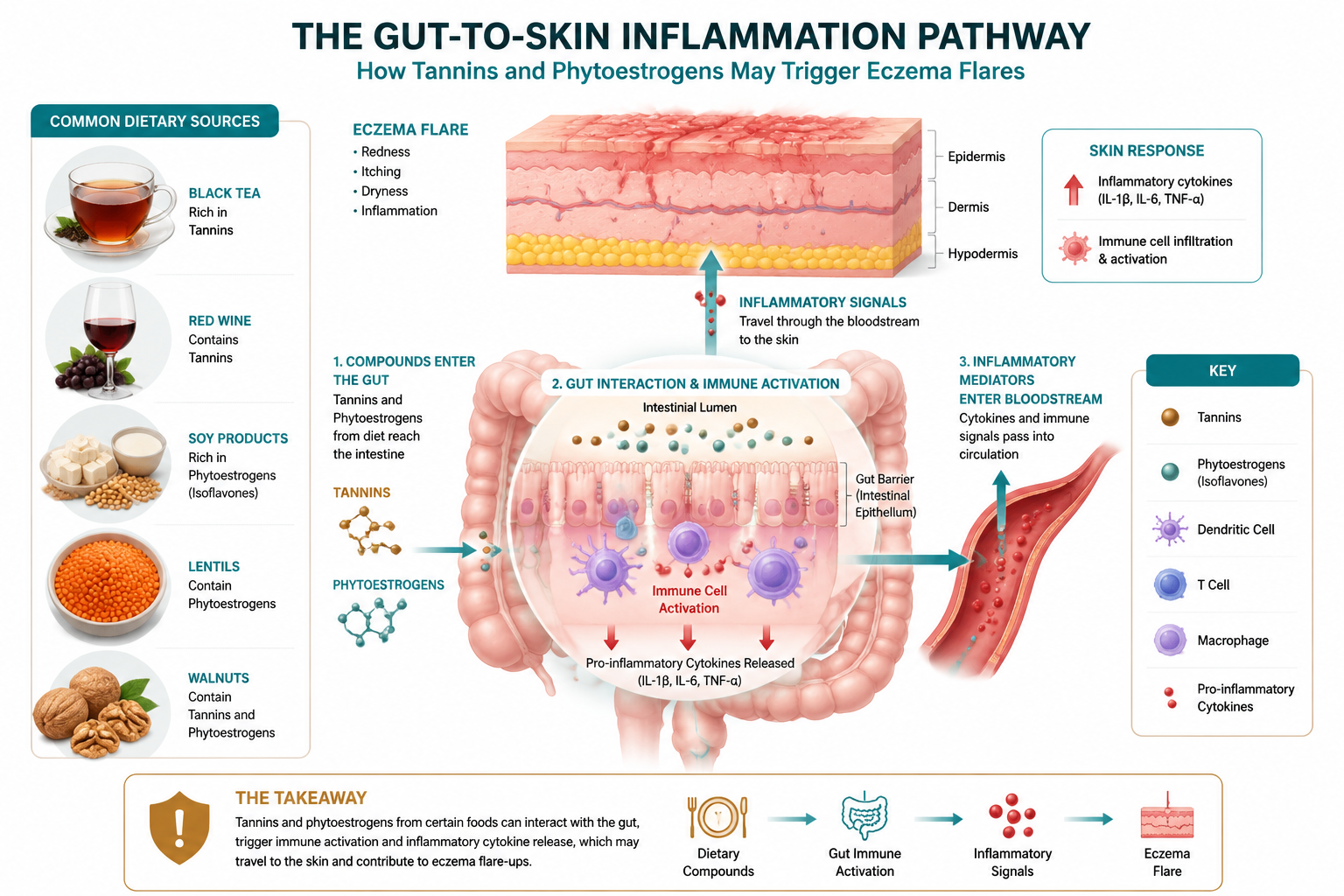
What Are Antinutrients and Why Do They Matter for Skin?
Antinutrients are naturally occurring compounds in plant foods that interfere with the absorption of nutrients or trigger immune responses in the gut. In plain English, they are the plant’s own defence chemicals — evolved to discourage insects and animals from eating them.
The most relevant to eczema are:
- Tannins — polyphenolic compounds found in tea, coffee, red wine, pomegranates, walnuts, and many legumes
- Phytoestrogens — plant-based compounds that mimic oestrogen, found primarily in soy, flaxseed, chickpeas, and lentils
- Lectins — proteins that bind to gut wall cells and can increase intestinal permeability
- Oxalates — found in spinach, almonds, and beets; can contribute to inflammatory load in sensitive individuals
The link between antinutrients and skin health — specifically how tannins and phytoestrogens trigger eczema flares — runs through the gut, not through the skin directly. When the gut lining is compromised, immune activation follows, and that immune response shows up in the skin for people with pre-existing atopic conditions.
Context matters. Antinutrients are not inherently harmful. For most people eating a varied diet, they cause no noticeable problems. The issue arises when intake is high, gut health is already compromised, or immune reactivity is elevated — all of which are common in people with chronic eczema.
For a broader look at how plant compounds interact with the body, the guide on plant toxins and antinutrients covers the foundational science in useful detail.
How Do Tannins Contribute to Eczema Flares?
Tannins bind to proteins and minerals in the digestive tract, which is how they earn their “antinutrient” label. But their effect on immune function is where the skin connection becomes relevant.
The mechanism works like this:
- Tannins consumed in high amounts bind to digestive enzymes and gut wall proteins
- This binding can reduce the gut’s ability to maintain a healthy mucosal barrier
- A weakened barrier allows partially digested food particles and bacterial fragments to enter the bloodstream
- The immune system responds to these particles as foreign — triggering low-grade systemic inflammation
- In people with atopic dermatitis, this systemic inflammation amplifies existing skin reactivity
Common high-tannin foods:
| Food | Tannin Content | Notes |
|---|---|---|
| Black tea | Very high | Highest per cup of common beverages |
| Red wine | High | Also contains histamines |
| Pomegranate | High | Often overlooked |
| Walnuts | Moderate-high | Skin of the nut is the main source |
| Dark chocolate | Moderate | Also contains flavonoids with anti-inflammatory effects |
| Coffee | Moderate | Chlorogenic acids are the primary tannin-type compounds |
| Lentils | Moderate | Significantly reduced by soaking and cooking |
Common mistake: Assuming that because tannins are polyphenols, they are always beneficial. The evidence suggests they can be — at moderate intake, in a healthy gut. But for someone with compromised gut integrity and active eczema, the same compounds can tip the balance toward inflammation rather than away from it.
The health benefits of dark chocolate article is worth reading here — it illustrates how the same plant compound can be beneficial in one context and problematic in another. That nuance is exactly what gets lost when people chase simple answers.
How Do Phytoestrogens Affect Skin and Eczema?
Phytoestrogens are plant compounds that weakly bind to oestrogen receptors in the body. This hormonal mimicry is the source of both their potential benefits and their potential problems for people with eczema.
The skin-hormone connection:
Oestrogen plays a documented role in skin barrier function. It supports collagen production, regulates sebum output, and influences the activity of mast cells — immune cells that release histamine during allergic reactions. When phytoestrogens occupy oestrogen receptors, they can either weakly activate or block those receptors depending on the tissue type and the individual’s existing hormone levels.
For people with eczema, the concern is this: disrupted oestrogen signalling can alter mast cell behaviour and skin barrier integrity, potentially making flares more frequent or more severe.
Key phytoestrogen sources:
- Soy products (tofu, soy milk, edamame) — isoflavones are the primary compound
- Flaxseed — lignans, which convert to phytoestrogens in the gut
- Chickpeas and lentils — lower levels but still relevant at high intake
- Red clover — often found in herbal supplements
- Sesame seeds — lignans present in meaningful amounts
Who is most likely to be affected?
- Women in perimenopause or menopause (already experiencing hormonal shifts)
- People with a history of hormone-sensitive conditions
- Individuals consuming very high amounts of soy-based products daily
- Those with gut dysbiosis, since gut bacteria convert phytoestrogens into their active forms — meaning microbiome composition determines how much phytoestrogen activity actually occurs
It is not that simple to say “soy causes eczema.” The evidence does not support that as a blanket statement. What the evidence does suggest is that for a subset of eczema sufferers — particularly those with hormonal sensitivities or gut dysbiosis — high phytoestrogen intake is worth investigating as a contributing factor.
What Does the Research Actually Say About Diet and Eczema Triggers?
Let’s keep this practical and be honest about what the research does and does not show.
What is well-established:
- Eczema is primarily an immune-mediated condition, and early childhood immune cell reactivity is a key factor in its onset [2]
- Stress hormones — particularly cortisol and adrenaline — have a documented role in triggering and worsening eczema flares [1][3]
- Gut barrier function influences systemic immune activity, and diet directly affects gut barrier integrity
- Natural plant compounds including flavonoids and polyphenols show promise as therapeutic agents for atopic dermatitis in recent reviews [5]
What is less certain:
- Whether tannins specifically, in typical dietary amounts, cause measurable eczema flares in controlled trials
- The exact threshold of phytoestrogen intake that triggers hormonal disruption in eczema-prone individuals
- Whether elimination diets produce long-term skin improvement beyond the short-term reduction in inflammatory load
What the research does NOT support:
- The idea that antinutrients are the primary cause of eczema — they are not
- Blanket elimination of all plant foods containing these compounds
- Treating dietary change as a replacement for medical management
A nationwide survey [4] found that a significant proportion of eczema patients are concerned about the long-term effects of standard treatments, which partly explains why dietary approaches attract so much attention. That concern is understandable. But it should not lead people toward unproven elimination protocols that strip their diet of nutritious foods without clear evidence of benefit.
The stronger evidence points to a multi-factor model: immune reactivity sets the baseline, stress amplifies flares, and dietary factors — including antinutrients — can modulate the severity for some individuals.
For a deeper look at how gut health connects to systemic inflammation, the gut health and digestive wellness guide is a useful companion read.

Which Foods Are Most Likely to Trigger Eczema Through Antinutrient Pathways?
A sensible starting point is identifying the foods most likely to contribute to eczema flares through antinutrient mechanisms — and distinguishing them from foods that trigger eczema through other pathways (like direct IgE-mediated allergy).
Highest-risk foods via antinutrient pathways:
- Strong black tea consumed multiple times daily — high tannin load, particularly problematic on an empty stomach
- Large daily servings of soy milk or tofu — phytoestrogen load becomes relevant above roughly 50–100mg isoflavones per day (based on available estimates; individual thresholds vary)
- Unsoaked, uncooked legumes — lectins and tannins both present at higher levels
- Red wine — combines tannins, histamines, and sulphites, making it a multi-pathway trigger
- Walnuts eaten with the skin — the papery inner skin contains the highest tannin concentration
- Flaxseed in large daily amounts — lignan content converts to active phytoestrogens in the gut
Lower-risk but worth monitoring:
- Green tea (lower tannin than black, but still present)
- Pomegranate juice (concentrated tannin source)
- Chickpea-heavy diets (moderate phytoestrogen, but cumulative with other sources)
Foods that are often blamed but have weaker evidence:
- Spinach and oxalate-rich vegetables — relevant mainly in people with specific metabolic issues
- Coffee — the tannin-type compounds are different from tea tannins and the evidence for skin effects is mixed
A practical decision rule: If you are consuming more than three high-tannin or high-phytoestrogen foods daily, and your eczema is poorly controlled, it is worth a structured 30-day reduction trial before drawing conclusions.
The anti-inflammatory foods guide provides a useful framework for building a diet that actively supports skin health rather than just removing potential triggers.
The Gut-Skin Axis: Why Your Digestive Health Determines Your Skin’s Response
The gut-skin axis is the biological link that makes dietary antinutrients relevant to eczema. In plain English: what happens in your gut does not stay in your gut.
Here is how the pathway works:
- Gut microbiome composition determines how antinutrients are metabolised. A diverse, healthy microbiome can break down tannins and phytoestrogens efficiently, reducing their inflammatory potential
- Intestinal permeability — sometimes called “leaky gut” — allows food-derived compounds and bacterial fragments to enter systemic circulation when the gut lining is compromised
- Systemic immune activation follows, with inflammatory cytokines circulating throughout the body
- Skin immune cells (particularly Th2 lymphocytes and mast cells) respond to this systemic signal, worsening atopic dermatitis in predisposed individuals
The evidence for this pathway is mechanistically sound, even if the specific role of tannins and phytoestrogens within it is still being characterised in clinical research [5].
What affects gut barrier integrity:
- Chronic stress (independently documented to worsen both gut permeability and eczema [3])
- Antibiotic use and its effect on microbiome diversity
- Low dietary fibre intake
- High alcohol consumption
- Sleep quality (poor sleep increases intestinal permeability)
This is why addressing only diet without looking at stress, sleep, and gut microbiome support tends to produce limited results. The leaky gut science guide separates the evidence from the hype on intestinal permeability — worth reading before drawing firm conclusions.
The 30-Day Skin Clearance Protocol: A Practical Framework
This protocol is designed as an investigative tool, not a cure. The goal is to determine whether antinutrient load is a meaningful contributor to your eczema, and to reduce overall inflammatory burden while doing so.
Before starting:
- Inform your dermatologist or GP
- Continue any prescribed topical treatments
- Keep a daily symptom log (skin score 1–10, sleep quality, stress level, foods eaten)
Week 1–2: Targeted Reduction Phase
Reduce or eliminate for 14 days:
- Black tea (switch to rooibos or herbal alternatives)
- Soy milk, tofu, edamame (replace with oat milk or almond milk)
- Red wine and other tannin-rich alcoholic drinks
- Unsoaked legumes (soak all beans and lentils for 12 hours before cooking)
- Large daily flaxseed servings (reduce to 1 teaspoon or less)
- Walnuts eaten raw with skin intact
Add in:
- Oily fish (salmon, mackerel) 3–4 times per week — omega-3 fatty acids support skin barrier
- Cooked and peeled vegetables over raw where possible
- Probiotic-rich foods: plain yoghurt, kefir, sauerkraut
- Adequate hydration: 1.5–2 litres of water daily
Week 3: Gut Support Phase
Focus on rebuilding gut integrity:
- Add a prebiotic fibre source daily (oats, garlic, onion, leek)
- Consider a broad-spectrum probiotic supplement if fermented foods are not tolerated
- Reduce processed food intake to lower overall inflammatory load
- Prioritise 7–8 hours of sleep — sleep deprivation measurably increases gut permeability
- Implement one stress management practice daily (walking, breathing exercises, or structured relaxation)
The probiotics vs prebiotics guide explains which approach is most appropriate depending on your current gut health status.
Week 4: Structured Reintroduction
Reintroduce one food at a time, every 3–4 days:
- Reintroduce the food in a moderate serving
- Monitor skin response for 72 hours before adding the next food
- Record any change in itch intensity, redness, or new lesions
- If a clear reaction occurs, remove that food and wait 5 days before testing the next
What a positive result looks like: Measurable improvement in skin score during weeks 1–3, with identifiable worsening when specific foods are reintroduced. That is useful, actionable information.
What a negative result means: If skin scores do not improve during the reduction phase, antinutrient load is likely not a primary driver of your flares. Redirect attention to stress management, sleep quality, environmental triggers, or medical treatment optimisation.

Practical Ways to Reduce Antinutrient Load Without Eliminating Healthy Foods
The goal is not to avoid plant foods — that would be counterproductive. Most plant foods with antinutrients also contain fibre, vitamins, and compounds that actively support health. The goal is to reduce antinutrient load through preparation and portion management.
Effective reduction methods:
| Method | Antinutrients Reduced | Best Applied To |
|---|---|---|
| Soaking (12–24 hours) | Tannins, lectins, phytates | Legumes, beans, lentils |
| Cooking/boiling | Lectins, tannins (partial) | All legumes, grains |
| Fermentation | Phytates, tannins, phytoestrogens | Soy (tempeh, miso), grains |
| Sprouting | Lectins, phytates | Lentils, chickpeas, seeds |
| Peeling | Tannins | Walnuts, grapes, tomatoes |
| Dilution | All | Spreading intake across meals |
In real-world terms: Switching from raw lentils to soaked and well-cooked lentils can reduce their tannin content by 30–50% (based on food science estimates). Choosing tempeh over raw soy milk significantly reduces phytoestrogen bioavailability. These are not dramatic changes, but they are worth making if you are managing active eczema.
For people managing dry, reactive skin alongside dietary changes, practical topical support matters too. The guide on the best oils for dry skin covers evidence-based options that complement dietary management.
FAQ: Antinutrients, Tannins, Phytoestrogens, and Eczema
Q: Do tannins directly cause eczema?
No. Tannins do not directly cause eczema, but they can contribute to gut inflammation and immune activation that worsens flares in susceptible individuals. The relationship is indirect and dose-dependent.
Q: Is soy bad for eczema?
Not universally. Soy is a common eczema trigger in children with food allergies, but in adults the phytoestrogen pathway is more relevant. High daily soy intake may worsen eczema in individuals with hormonal sensitivities or gut dysbiosis. It is worth testing individually rather than assuming it is a problem.
Q: Can green tea worsen eczema?
Green tea contains tannins but at lower levels than black tea, and its anti-inflammatory polyphenols (particularly EGCG) may partially offset any pro-inflammatory effect. In moderate amounts, green tea is unlikely to be a significant trigger for most people.
Q: How long does it take to see skin improvement after reducing antinutrients?
Most people who respond to dietary changes see measurable improvement within 2–4 weeks. Skin cell turnover takes approximately 28 days, so a 30-day trial is a reasonable minimum timeframe.
Q: Should I avoid all polyphenols if I have eczema?
No. This is where hype gets in the way. Many polyphenols — including those in olive oil, turmeric, and ginger — have documented anti-inflammatory effects that support skin health. The goal is to reduce high-load sources of tannins and phytoestrogens, not to eliminate polyphenols altogether.
Q: Are antinutrients the main cause of my eczema?
Almost certainly not. Recent research [2] identifies immune cell reactivity as the primary driver of eczema onset, and stress hormones play a documented role in flares [1][3]. Diet is a modifying factor, not the root cause.
Q: Is the 30-day protocol safe to follow?
For most adults, yes — provided it is done alongside, not instead of, medical treatment. People with a history of eating disorders, nutritional deficiencies, or complex medical conditions should consult a healthcare professional before starting any elimination protocol.
Q: What about coffee — does it trigger eczema through tannins?
Coffee contains chlorogenic acids rather than classical tannins, and the evidence for coffee as an eczema trigger is weak. Some people react to coffee through histamine or caffeine pathways rather than tannin mechanisms. Individual testing is the most reliable approach.
Q: Can fermented soy products like miso and tempeh be eaten safely?
Generally yes. Fermentation significantly reduces phytoestrogen bioavailability and changes the isoflavone profile. Fermented soy is less likely to cause hormonal disruption than unfermented soy milk or raw edamame.
Q: Does stress make antinutrient effects worse?
Yes, and this is an important point. Stress increases gut permeability independently [3], which means the same dietary antinutrient load will have a greater inflammatory effect during high-stress periods. Managing stress is not optional if you are trying to control eczema through diet.
Conclusion: What Actually Matters Here
The relationship between antinutrients and skin health — specifically how tannins and phytoestrogens trigger eczema flares — is real, mechanistically plausible, and worth investigating for people with poorly controlled eczema. But it needs to be kept in proportion.
Antinutrients are not the primary cause of eczema. Immune reactivity is [2]. Stress hormones amplify flares [1][3]. Gut barrier function modulates severity. Diet — including antinutrient load — is one adjustable variable within a more complex picture.
The main takeaway is this: If you have chronic eczema and have not considered whether high tannin or phytoestrogen intake is contributing, a structured 30-day reduction trial is a low-risk, practical step worth taking. Soak your legumes. Reduce strong black tea. Monitor your soy intake. Support your gut with probiotic-rich foods and adequate fibre. And track your results honestly.
What you should not do is abandon a nutritious, plant-rich diet based on fear of antinutrients, or treat dietary change as a substitute for proper medical management.
Actionable next steps:
- Keep a 7-day food and symptom diary before making any changes — establish your baseline
- Identify your top three high-tannin or high-phytoestrogen foods and reduce them for 30 days
- Apply the food preparation methods above (soaking, cooking, fermentation) to reduce load without eliminating foods
- Support gut health with probiotic foods and adequate sleep alongside dietary changes
- Reintroduce foods systematically in week 4 to identify specific triggers
- Review results with your dermatologist — dietary findings are useful clinical information
For broader context on how plant compounds interact with the body, the article on what plant toxins actually do to your body is a useful next read. And if stress is a significant factor in your flares — which the evidence suggests it often is — the stress management guide covers practical approaches that complement everything discussed here.
There is no magic in it. But there is genuine value in understanding the mechanisms, testing systematically, and making changes based on your own results rather than someone else’s anecdote.
← What Plant Toxins Actually Do to Your Body: Effects on Digestion, Absorption and Inflammation
View the full Plant Toxins & Antinutrients cluster page →
References
[1] The Math Behind Eczema Flare Ups May Finally Add Up – https://www.powershealth.org/about-us/newsroom/health-library/2026/03/19/the-math-behind-eczema-flare-ups-may-finally-add-up
[2] New Research Sheds Light On Why Eczema So Often Begins In Childhood – https://www.mountsinai.org/about/newsroom/2026/new-research-sheds-light-on-why-eczema-so-often-begins-in-childhood
[3] PubMed — Stress and Eczema Flare Research – https://pubmed.ncbi.nlm.nih.gov/41857217/
[4] Nationwide Survey Underscores Concerns With Topical Steroids – https://nationaleczema.org/blog/nationwide-survey-underscores-concerns-with-topical-steroids/
[5] Natural Compounds in Atopic Dermatitis — Wiley Online Library – https://onlinelibrary.wiley.com/doi/10.1002/ptr.70056

