Kids and Plant Toxins: Antinutrient Impacts on Growth, ADHD, and Developing Brains

Last updated: May 10, 2026
Quick Answer: Many everyday plant foods contain natural compounds called antinutrients — including lectins, phytates, and phytoestrogens — that can interfere with mineral absorption, gut integrity, and hormone signaling. In adults, the risks are generally manageable. In children, whose brains and bodies are still forming, the same compounds deserve more careful attention. The evidence does not say to avoid plant foods. It says preparation, variety, and age-appropriate portions matter more than most parents realize.
Key Takeaways
- Antinutrients are not inherently dangerous, but they become a practical concern when children eat large amounts of poorly prepared legumes, grains, or soy products during critical growth windows.
- Phytates bind zinc, iron, and calcium — three minerals that are essential for brain development, attention regulation, and bone growth in children.
- Zinc, iron, and B6 deficiencies can disrupt dopamine and serotonin systems, which are directly implicated in ADHD and neurodevelopmental conditions [2].
- Lectins in raw or undercooked legumes can irritate the gut lining and impair nutrient absorption, especially in children with already sensitive digestive systems.
- Phytoestrogens in soy are a legitimate area of scientific discussion for infants and young children, though the risk from moderate dietary soy in older children appears low based on current evidence.
- Cooking, soaking, fermenting, and sprouting reduce antinutrient loads significantly — these are practical, low-effort strategies any parent can use.
- The gut-brain connection matters here: a compromised gut lining affects how nutrients reach the developing brain [see our guide on the gut-brain axis].
- No single food is the problem. The real risk comes from dietary patterns that are narrow, heavily processed, and consistently high in unvaried plant staples without adequate preparation.
- Parents should focus on food variety, proper preparation, and ensuring adequate intake of key minerals — not on eliminating plant foods.
In this guide
- What Are Antinutrients and Why Do They Matter for Children?
- How Do Phytates Affect Mineral Absorption in Growing Children?
- Do Lectins Cause Gut Damage in Children?
- What Is the Link Between Antinutrient Impacts on Growth, ADHD, and Developing Brains?
- Are Phytoestrogens in Soy Safe for Infants and Young Children?
- Age-Specific Safe Food Guidelines: What to Prioritize at Each Stage
- What Preparation Methods Reduce Antinutrient Risk for Kids?
- What Are the Warning Signs That a Child May Be Affected?
- Practical Parent Strategies: Reducing Risk Without Removing Plant Foods
- Conclusion: What Parents Actually Need to Do
- Frequently Asked Questions
What Are Antinutrients and Why Do They Matter for Children?
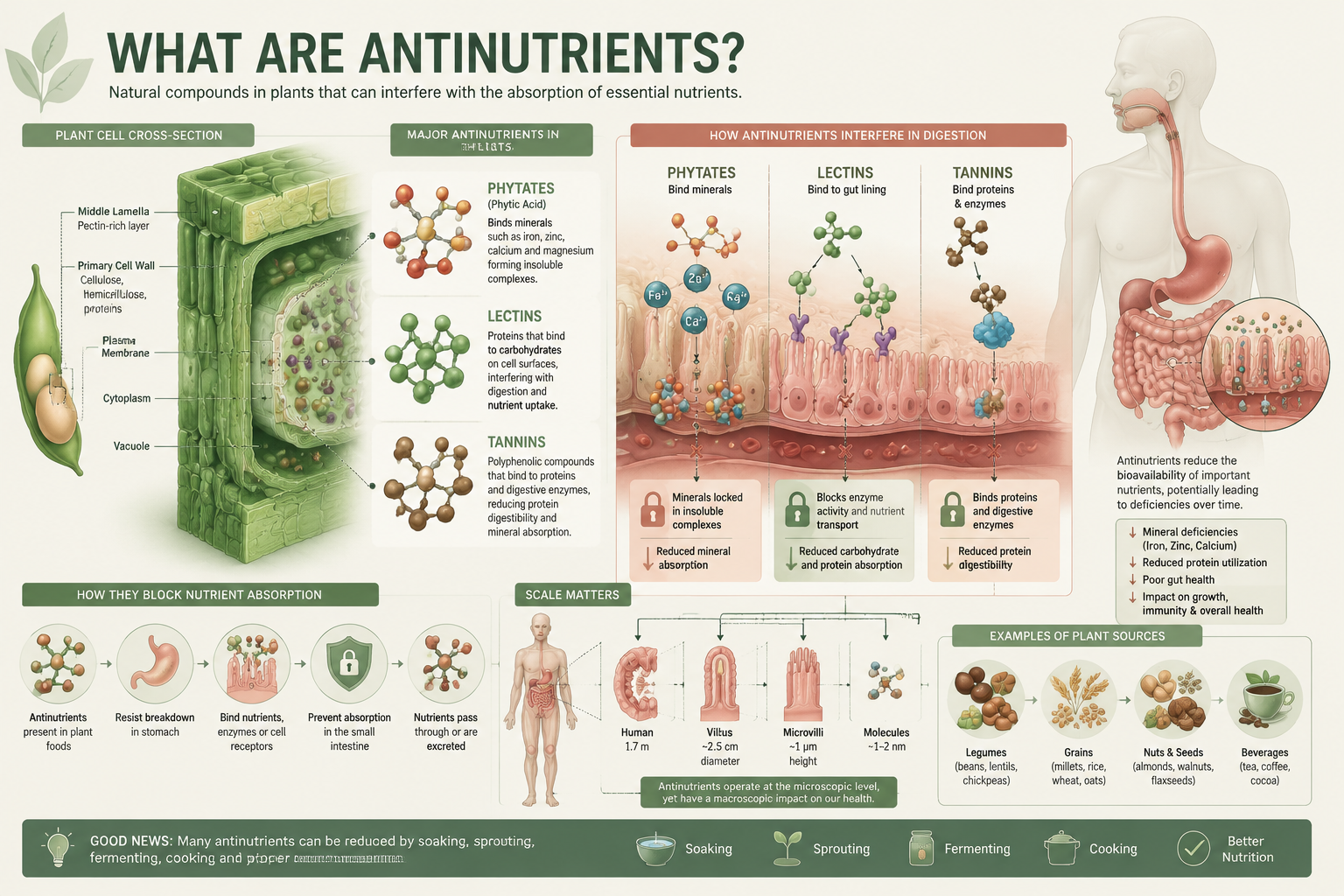
Antinutrients are natural chemical compounds that plants produce as a form of self-defense. They are not toxins in the dramatic sense — they will not poison a child who eats a bowl of lentil soup. But they do interfere with how the body absorbs and uses certain nutrients, and that distinction matters a great deal when the body in question is still developing.
The topic of kids and plant toxins — antinutrient impacts on growth, ADHD, and developing brains — tends to attract either alarm or dismissal. Neither serves parents well. Let’s keep this practical.
The main antinutrients worth understanding in a pediatric context are:
| Antinutrient | Primary Sources | Main Concern for Children |
|---|---|---|
| Phytates (phytic acid) | Whole grains, legumes, nuts, seeds | Binds zinc, iron, calcium — reduces absorption |
| Lectins | Raw/undercooked beans, wheat, nightshades | Gut lining irritation, impaired nutrient uptake |
| Phytoestrogens | Soy, flaxseed, some legumes | Potential hormonal signaling interference in infants |
| Oxalates | Spinach, beets, almonds, sweet potatoes | Binds calcium; high intake may affect bone mineral density |
| Tannins | Tea, legumes, some grains | Reduce iron and protein absorption |
| Saponins | Quinoa, legumes | Gut permeability effects at high doses |
For a deeper look at what these compounds do inside the body, the article on what plant toxins actually do to your body covers the mechanisms in plain detail.
The core issue with children is not that these compounds exist in food. It is that children eat smaller total food volumes, have higher relative nutrient demands per kilogram of body weight, and are in active phases of neurological and physical development. A mineral deficit that an adult absorbs without noticing can, in a child, translate into a measurable gap in growth or cognitive function.
How Do Phytates Affect Mineral Absorption in Growing Children?
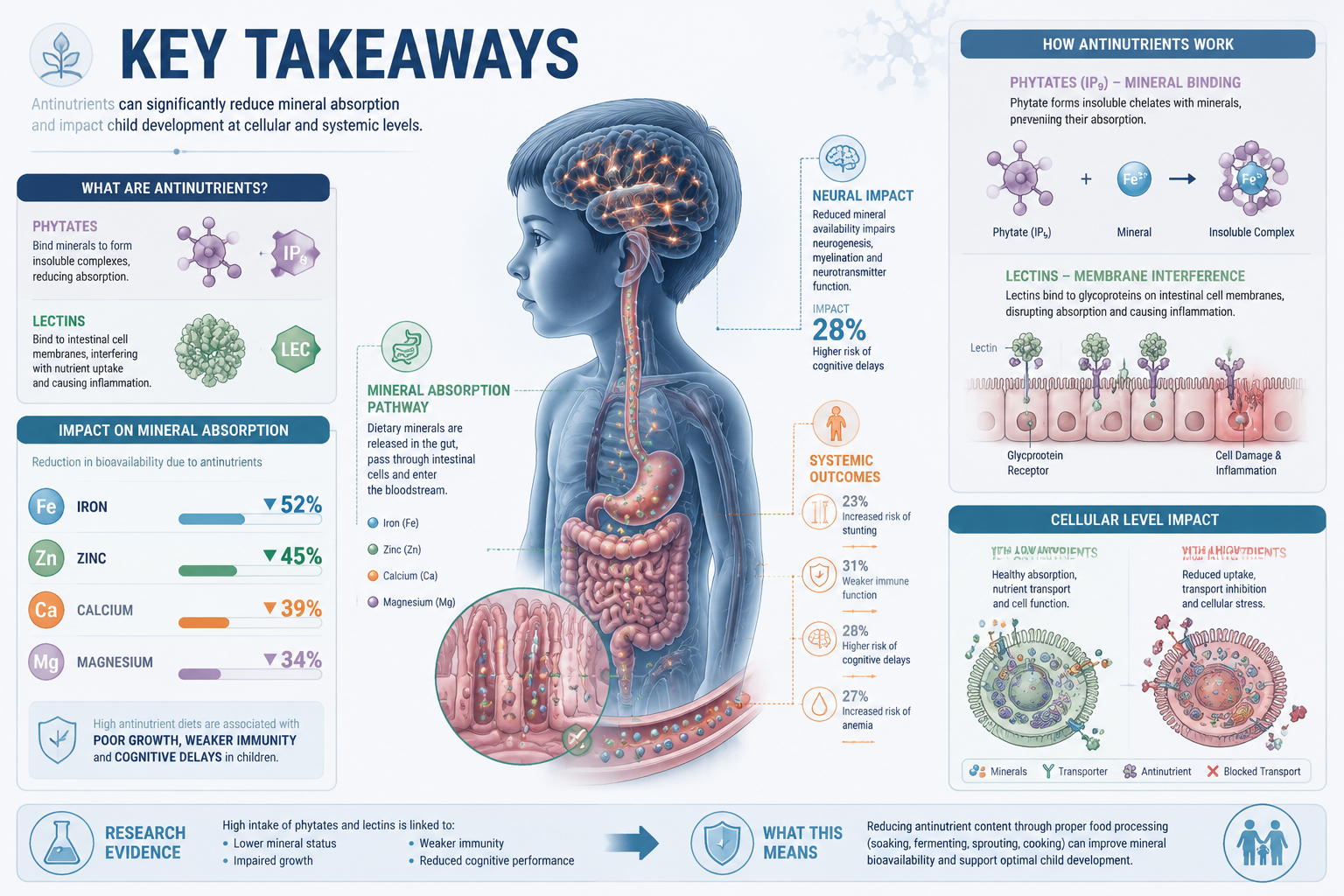
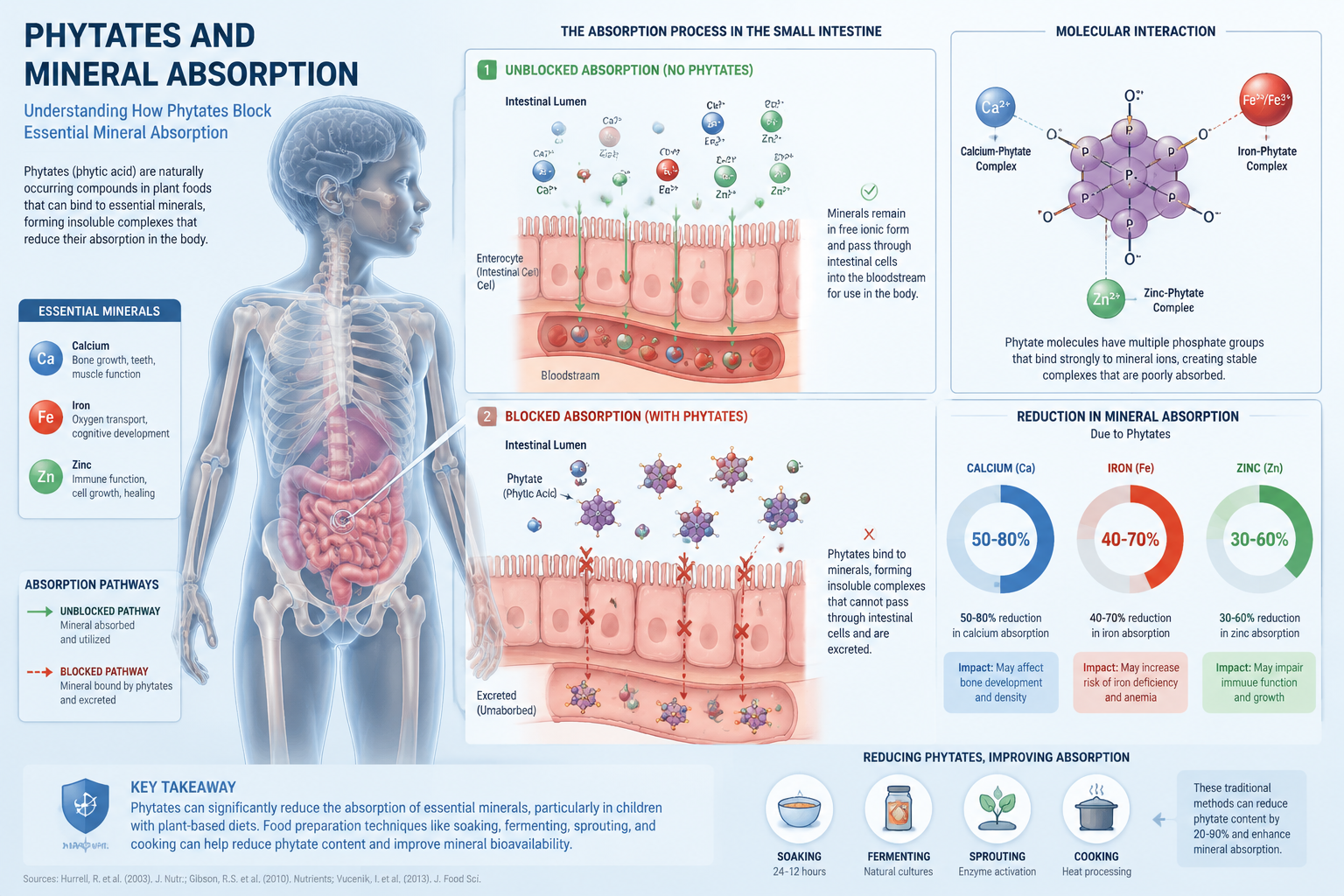
Phytates bind to minerals in the gut before they can be absorbed. In children, this is most concerning for zinc, iron, and calcium — all three are critical during the first decade of life.
Here’s the real issue: a child eating a diet heavy in whole grains and legumes without adequate preparation (soaking, fermenting, or cooking properly) may be consuming what looks like a nutrient-rich diet while actually absorbing significantly less of those nutrients than the food labels suggest.
What the evidence shows:
- Zinc is essential for brain development, immune function, and growth hormone signaling. Deficiency in early childhood is associated with stunted growth and impaired cognitive performance [2].
- Iron deficiency in children under five is one of the most common nutritional deficiencies globally and is strongly linked to attention problems, reduced learning capacity, and behavioral difficulties [4].
- Phytate-to-zinc ratios above 15:1 in a meal are considered high enough to significantly reduce zinc bioavailability — a threshold that is easy to reach in diets built around unsoaked whole grains and legumes.
Practical preparation methods that reduce phytate content:
- Soaking dried beans and grains for 12–24 hours before cooking (discard the soaking water)
- Fermenting — traditional sourdough bread, fermented porridges, and yogurt all reduce phytate load
- Sprouting seeds and legumes before cooking
- Cooking thoroughly — heat degrades phytates, especially in combination with soaking
The good news is that these methods are not complicated. Soaking dried lentils overnight before cooking them cuts phytate content by 30–50%, depending on the grain or legume. That is a meaningful difference for a child eating these foods regularly.
Common mistake: Parents who switch to “whole food plant-based” diets for their children without adjusting preparation methods may inadvertently reduce the bioavailability of key minerals at exactly the wrong time in their child’s development.
Do Lectins Cause Gut Damage in Children?
The short answer is: raw or undercooked lectins can cause real gut irritation, but properly cooked lectins are largely inactivated and pose minimal risk for most children.
Lectins are proteins found in high concentrations in raw kidney beans, wheat germ, and several other legumes. They bind to the gut lining and, at sufficient doses, can disrupt the integrity of the intestinal wall. This is not a fringe claim — raw kidney bean lectin (phytohaemagglutinin) is a well-documented cause of food poisoning, even in adults [see our broader article on plant toxins and antinutrients].
For children, the concern is more nuanced:
- Fully cooked legumes: lectin content is reduced by 90–99% through boiling. A child eating well-cooked beans is not at meaningful risk from lectins in those beans.
- Wheat lectins (WGA): wheat germ agglutinin is more heat-stable than bean lectins and survives cooking to a greater degree. The clinical significance of this in children eating normal amounts of bread and pasta is still debated.
- Children with existing gut issues: children with irritable bowel, leaky gut, or a history of gut inflammation may be more sensitive to even reduced lectin levels. The gut-brain axis is directly relevant here — gut inflammation can impair the absorption of the very nutrients the developing brain depends on.
The bottom line on lectins for parents: cook legumes properly, never serve raw or undercooked kidney beans to children, and be attentive if a child consistently shows digestive discomfort after eating wheat or bean-heavy meals. That is a sensible starting point.
What Is the Link Between Antinutrient Impacts on Growth, ADHD, and Developing Brains?
This is where the science gets genuinely interesting — and where it is easy to overstate the case. Let’s separate fact from hype.
The connection between antinutrients and ADHD is not direct. Antinutrients do not cause ADHD. What the evidence does suggest is that antinutrient-driven mineral deficiencies can worsen or mimic ADHD-like symptoms in some children, and that correcting those deficiencies can improve attention and behavior [2].
The key nutritional pathways:
- Zinc is required for dopamine synthesis and regulation. Low zinc is found more frequently in children with ADHD than in neurotypical children, and several trials have found that zinc supplementation modestly improves ADHD symptoms in zinc-deficient children [2].
- Iron is needed for dopamine transporter function. Iron deficiency — even without full anemia — has been associated with inattention and hyperactivity in children [4].
- Vitamin B6 acts as a cofactor in the production of both dopamine and serotonin. Deficiency disrupts both systems [2].
- Omega-3 fatty acids (not an antinutrient issue directly, but relevant to the same dietary pattern) are essential for prefrontal cortex maturation, which governs executive function and attention regulation [2].
The connection to antinutrients is this: if a child’s diet is high in phytate-rich foods without proper preparation, and low in animal-source foods that provide highly bioavailable zinc and iron, that child is at greater risk of the mineral deficiencies that affect these neurological systems.
Early toxic exposures — including dietary factors that impair brain development during sensitive windows — can have lasting effects on brain architecture [7]. The developing brain between ages 0 and 5 is particularly vulnerable to nutritional gaps because this is when synaptic connections, myelination, and neurotransmitter systems are being established at the fastest rate [7].
What matters most is this: it is not that plant foods cause ADHD. It is that a poorly varied, poorly prepared plant-heavy diet during critical developmental windows can create nutritional gaps that affect the same brain systems involved in attention, impulse control, and learning.
Are Phytoestrogens in Soy Safe for Infants and Young Children?
This is one of the more contested areas in pediatric nutrition, and the honest answer is: it depends on the age of the child, the amount consumed, and the form of soy.
Phytoestrogens are plant compounds that weakly mimic estrogen in the body. Soy is the most concentrated dietary source. The concern for infants is highest because soy-based infant formula provides phytoestrogen exposure at a dose that is, relative to body weight, significantly higher than what adults consume from dietary soy.
What the evidence currently shows:
- Soy-based infant formula has been used for decades and is considered safe by major pediatric bodies for most infants who cannot tolerate cow’s milk formula. However, some researchers have called for more long-term data on hormonal and developmental outcomes [3].
- For older children (ages 3 and above), moderate dietary soy — tofu, edamame, miso — does not appear to cause harm based on current evidence. Asian populations with high lifelong soy intake do not show patterns of hormonal disruption that would suggest a major clinical concern.
- The area of genuine uncertainty is concentrated soy products (soy protein isolates, soy-based snack foods) consumed in large amounts during early childhood, particularly in children with thyroid conditions, since phytoestrogens can interfere with thyroid hormone synthesis.
That is a strong claim and needs strong proof — and the evidence for harm from moderate whole-food soy in children past infancy is not there yet. The stronger evidence points to concerns with high-dose isolated soy protein, not a bowl of edamame.
A sensible approach for parents:
- Avoid making soy-based formula the default for infants without a clear medical reason
- Moderate whole-food soy (2–3 servings per week) in children over 2 appears reasonable based on current evidence
- Avoid relying heavily on processed soy products as a primary protein source for young children
Age-Specific Safe Food Guidelines: What to Prioritize at Each Stage
Different ages carry different levels of risk. Here is a practical framework based on what the evidence supports.
Infants (0–12 months)
- Breast milk or appropriate formula remains the gold standard
- Introduction of solid foods (from around 6 months) should prioritize iron-rich foods: pureed meat, well-cooked lentils, fortified cereals
- Avoid raw or undercooked legumes entirely
- Soy-based formula: use only when medically indicated, not as a default
Toddlers (1–3 years)
- This is a high-risk window for mineral deficiency because food variety is often low and portions are small
- Ensure zinc and iron from bioavailable sources: meat, eggs, fish, well-cooked legumes
- Soak and cook all legumes thoroughly before serving
- Limit high-oxalate foods (raw spinach, beet greens) as primary calcium sources — cooked spinach is better
- Pair plant-based iron sources with vitamin C to improve absorption (e.g., lentils with tomato)
Children (4–10 years)
- Dietary variety becomes the main protective factor
- Fermented foods (yogurt, kefir, miso) support gut health and reduce antinutrient exposure
- Whole grains are fine — but sourdough bread, oats soaked overnight, and properly cooked rice are better choices than raw bran-heavy products
- Watch for consistent digestive complaints after legume or wheat-heavy meals
Adolescents (11–17 years)
- Growth spurts increase zinc and iron demands significantly
- Adolescent girls who begin menstruating have higher iron needs — plant-only iron sources may be insufficient without careful planning
- Phytoestrogen concerns from soy are less significant at this stage; the hormonal environment is already active
What Preparation Methods Reduce Antinutrient Risk for Kids?
Proper food preparation is the most practical tool parents have. The evidence here is consistent and the methods are straightforward.
Most effective methods by antinutrient type:
| Method | Reduces Phytates | Reduces Lectins | Reduces Oxalates | Reduces Saponins |
|---|---|---|---|---|
| Soaking (12–24 hrs) | ✅ 30–50% | ✅ Partial | ✅ Partial | ✅ Yes |
| Boiling/cooking | ✅ Yes | ✅ 90–99% | ✅ Yes (discard water) | ✅ Yes |
| Fermenting | ✅ 50–90% | ✅ Partial | ✅ Partial | ✅ Partial |
| Sprouting | ✅ 30–50% | ✅ Partial | ✅ Minimal | ✅ Yes |
| Rinsing (quinoa) | ❌ Minimal | ❌ Minimal | ❌ Minimal | ✅ Yes |
In real-world terms, the most impactful single habit for parents is soaking dried legumes before cooking and discarding the soaking water. This takes about 30 seconds of active effort the night before. Combined with thorough cooking, it removes the majority of the lectin and phytate concern in one step.
Pairing plant-based iron and zinc sources with vitamin C-rich foods (tomatoes, bell peppers, citrus) is the second most practical strategy — it does not reduce antinutrients but counteracts their absorption-blocking effect.
For families eating significant amounts of anti-inflammatory whole foods, the guide to anti-inflammatory foods for gut health is worth reading alongside this one, since gut health directly affects how well children absorb the nutrients these foods provide.
What Are the Warning Signs That a Child May Be Affected?
No single symptom points definitively to antinutrient-driven mineral deficiency. But there are patterns worth paying attention to.
Signs that may warrant a conversation with a pediatrician:
- Persistent fatigue or low energy that does not improve with adequate sleep
- Pale skin, brittle nails, or frequent infections (possible iron or zinc deficiency)
- Slow growth relative to peers or growth chart expectations
- Attention difficulties, impulsivity, or behavioral changes — especially in children eating narrow, plant-heavy diets
- Frequent digestive discomfort (bloating, loose stools) after legume or grain-heavy meals
- Poor appetite or food aversions that limit dietary variety
What to ask for: a basic blood panel including serum ferritin (iron stores), zinc, and a full blood count is a reasonable starting point. Ferritin in particular is a more sensitive marker of iron status than hemoglobin alone and is frequently overlooked in routine pediatric checks.
Context matters: these symptoms have many possible causes. The goal is not to blame plant foods for every attention problem or growth concern. The goal is to ensure that dietary patterns are not creating preventable nutritional gaps.
Environmental factors also play a role in children’s neurodevelopmental health, and it is worth understanding the environmental factors that affect human health more broadly when evaluating a child’s overall exposure picture.
Practical Parent Strategies: Reducing Risk Without Removing Plant Foods
The main takeaway is not “avoid plants.” It is “prepare them properly, vary the diet, and make sure the key minerals are covered.”
A simple checklist for parents:
- Soak dried legumes for 12–24 hours before cooking; discard soaking water
- Cook legumes thoroughly — never serve undercooked kidney beans
- Rinse quinoa before cooking to remove saponins
- Pair plant-based iron sources (lentils, spinach) with vitamin C-rich foods at the same meal
- Include animal-source foods (eggs, meat, fish, dairy) regularly as high-bioavailability mineral sources, unless there is a specific medical or ethical reason not to
- Use fermented foods where possible: sourdough bread, yogurt, kefir, miso
- Avoid making soy the primary protein source for children under 2
- Vary the diet — no single plant food should dominate every meal
- If the child eats a primarily plant-based diet, discuss zinc, iron, and B12 status with a pediatrician annually
What about supplements? Supplementation is not the first answer, but it is a reasonable safety net for children on restricted diets. A pediatric multivitamin that includes zinc, iron (if deficiency is confirmed), and B12 covers the main gaps without overcomplicating things. More is not always better — iron supplementation in non-deficient children carries its own risks and should not be done without testing.
For parents interested in the broader picture of how nutrition affects long-term health, the health benefits of natural foods and herbs evidence-based guide provides useful context on what the research actually supports.
Conclusion: What Parents Actually Need to Do
Kids and plant toxins — antinutrient impacts on growth, ADHD, and developing brains — is a topic that deserves honest, measured attention. The evidence does not support panic about plant foods. It does support being thoughtful about how those foods are prepared, how varied the diet is, and whether key minerals are genuinely being absorbed.
The practical summary:
- Prepare legumes and grains properly — soaking and cooking are not optional extras; they are the difference between a food that nourishes and one that partially blocks its own nutrients.
- Prioritize dietary variety — the narrower the diet, the greater the risk that antinutrient-driven mineral losses become clinically meaningful.
- Include bioavailable mineral sources — eggs, meat, fish, and dairy provide zinc and iron in forms that antinutrients cannot block. These are not obstacles to a healthy diet; they are practical anchors for children’s nutritional needs.
- Watch for warning signs and get a basic blood panel if a child shows persistent fatigue, attention difficulties, or slow growth on a plant-heavy diet.
- Use proper preparation as the primary strategy — it is free, effective, and requires minimal habit change.
There is no magic in it. The basics still do the heavy lifting. Start with what gives the biggest return: soak your legumes, cook them thoroughly, vary the diet, and make sure the minerals are covered. That is a sensible, evidence-aware approach that does not require removing any food group from a child’s plate.
Frequently Asked Questions
Q: Are antinutrients harmful to all children?
A: No. Antinutrients become a practical concern mainly when children eat large amounts of poorly prepared plant foods with limited dietary variety. Most children eating a varied, well-prepared diet are not at significant risk.
Q: Can antinutrients cause ADHD?
A: Antinutrients do not cause ADHD. However, the mineral deficiencies they can contribute to — particularly in zinc, iron, and B6 — can worsen attention and behavioral symptoms in some children, and correcting these deficiencies may help [2].
Q: Is soy formula safe for infants?
A: Major pediatric bodies consider soy formula safe for most infants who cannot tolerate cow’s milk formula. It should not be the default choice without a medical reason, and parents should discuss options with a pediatrician [3].
Q: How much does soaking reduce antinutrients?
A: Soaking dried legumes for 12–24 hours and discarding the water reduces phytate content by approximately 30–50% and partially reduces lectins. Thorough cooking after soaking removes 90–99% of active lectins.
Q: Should children on plant-based diets take supplements?
A: A pediatric multivitamin covering zinc, B12, and iron (if deficiency is confirmed by testing) is a reasonable safety net for children on primarily plant-based diets. Supplementation should be discussed with a pediatrician rather than started based on assumption.
Q: Are lectins in cooked beans dangerous for children?
A: No. Properly boiled legumes have had 90–99% of their lectins deactivated. The risk from lectins applies to raw or undercooked beans, particularly kidney beans, which should never be served to children in that state.
Q: Which minerals are most affected by phytates in children?
A: Zinc, iron, and calcium are the minerals most significantly blocked by phytates. Zinc and iron are particularly important for brain development and attention regulation.
Q: At what age is phytoestrogen exposure from soy most concerning?
A: The concern is highest in infancy, when soy formula provides phytoestrogen exposure at a high dose relative to body weight. Moderate dietary soy in children over age 2 appears to carry low risk based on current evidence.
Q: What foods are highest in phytates?
A: Whole grains (wheat bran, oats, brown rice), legumes (beans, lentils, chickpeas), nuts, and seeds are the highest sources. Proper preparation significantly reduces their phytate content.
Q: Can gut health affect how antinutrients impact a child?
A: Yes. A compromised gut lining — from inflammation, infection, or poor diet — can make a child more sensitive to lectins and reduce the absorption of minerals even from well-prepared foods. Gut health and brain development are closely connected [see the gut-brain axis guide].
Plant Toxins & Antinutrients reading path
References
[1] The Hidden Impact Of Environmental Toxins – https://foundationscognitive.com/blog/the-hidden-impact-of-environmental-toxins
[2] Environmental chemicals and ADHD scoping review – https://pmc.ncbi.nlm.nih.gov/articles/PMC8910189/
[3] PMC11963292 – https://pmc.ncbi.nlm.nih.gov/articles/PMC11963292/
[4] PubMed 25581143 – https://pubmed.ncbi.nlm.nih.gov/25581143/
[5] Could Environmental Toxins Contribute To ADHD Symptoms – https://chadd.org/adhd-weekly/could-environmental-toxins-contribute-to-adhd-symptoms/
[6] Parental Avoidance Of Toxic Exposures Could Help Prevent Autism ADHD In Children – https://news.uthscsa.edu/parental-avoidance-of-toxic-exposures-could-help-prevent-autism-adhd-in-children-new-study-shows/
[7] Early Exposure To Toxic Substances And Brain Architecture – https://developingchild.harvard.edu/wp-content/uploads/2024/10/Early_Exposure_Toxic_Substances_Brain_Architecture.pdf

