Explore how to Revamp your Digestion: Complete guide to bland food diets for optimal health.

Last updated: April 8, 2026
Quick Answer: A bland food diet is a short-term eating plan built around easily digestible, low-fiber, low-fat, and non-spicy foods. It’s designed to reduce irritation in the gastrointestinal tract and relieve symptoms like heartburn, nausea, vomiting, diarrhea, and stomach pain. The diet typically includes foods like white rice, plain chicken, bananas, cooked vegetables, and low-fat dairy — while excluding spicy foods, fatty meats, acidic fruits, whole grains, and alcohol. Most people follow it temporarily during a flare-up or after surgery, then gradually reintroduce other foods.
Key Takeaways
- A bland food diet reduces GI irritation by eliminating foods that stimulate excess stomach acid, increase gut motility, or cause inflammation.
- Safe foods include low-fat dairy, cooked vegetables (carrots, spinach, beets), low-fiber fruits (bananas, melons, canned peaches), refined grains (white rice, plain pasta), and lean proteins (skinless chicken, fish, eggs, tofu).
- Foods to avoid include high-fat dairy, acidic or seeded fruits (citrus, berries), whole grains, fatty or fried meats, spicy seasonings, alcohol, and carbonated drinks.
- The diet is particularly useful for people managing gastritis, peptic ulcers, GERD, post-surgical recovery, or acute episodes of nausea and diarrhea.
- It is not a long-term eating plan — most healthcare providers recommend transitioning back to a varied diet as symptoms improve.
- Portion control matters: smaller, more frequent meals reduce pressure on the stomach and prevent symptom flare-ups.
- Hydration is critical, especially when diarrhea or vomiting is involved. Clear fluids, broths, and herbal teas are preferred.
- Always consult a doctor or registered dietitian before starting a bland diet, especially if you have an underlying condition.
- Stress management and weight reduction can amplify the diet’s benefits by reducing baseline GI inflammation.
- Lifestyle factors — meal timing, eating pace, and sleep position — work alongside dietary choices to support recovery.
What Is a Bland Food Diet, and Who Is It For?
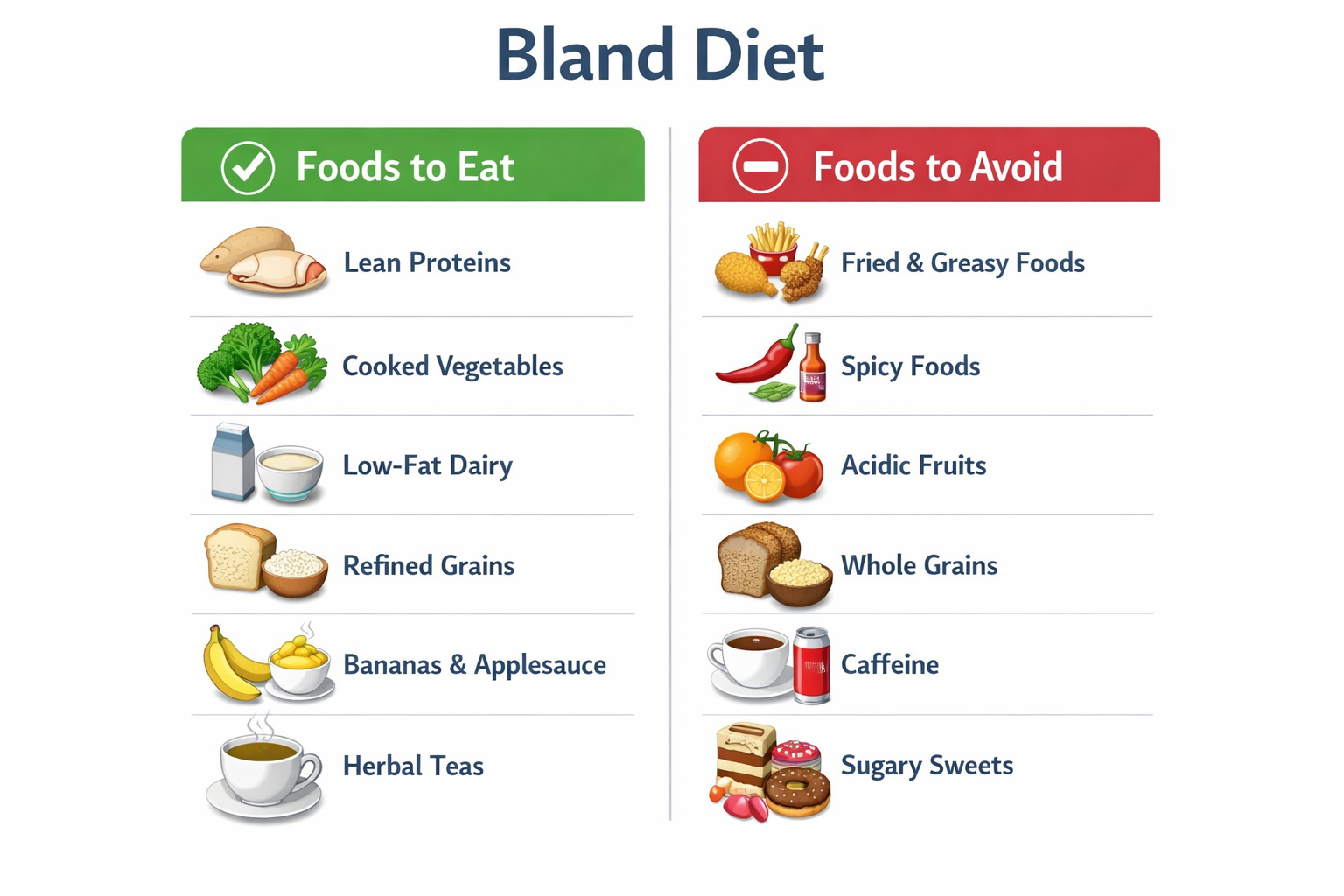

A bland food diet is a medically recognized eating approach that prioritizes foods that are gentle on the digestive system. It avoids anything that stimulates excess stomach acid, causes gas, or is difficult to break down — including spicy seasonings, high-fat foods, raw high-fiber vegetables, and acidic ingredients.
This diet is not a weight-loss plan or a permanent lifestyle change. It’s a therapeutic tool used during periods of gastrointestinal distress.
Who benefits most from a bland diet:
- People recovering from stomach surgery or a gastrointestinal illness (gastroenteritis, food poisoning)
- Individuals managing chronic conditions like gastritis, peptic ulcers, or GERD
- Anyone experiencing acute nausea, vomiting, or diarrhea
- People with inflammatory bowel conditions during a flare (though specific IBD protocols vary — always confirm with your gastroenterologist)
- Post-chemotherapy patients dealing with treatment-related nausea
Who should NOT self-prescribe this diet:
- People with nutritional deficiencies who may worsen their status by restricting food groups without guidance
- Individuals with eating disorder histories, where restrictive eating patterns can be harmful
- Anyone using it as a long-term solution without addressing the underlying cause of their GI symptoms
The bland diet works best as a bridge — a short-term reset that reduces symptoms while your gut heals, not a permanent fix.
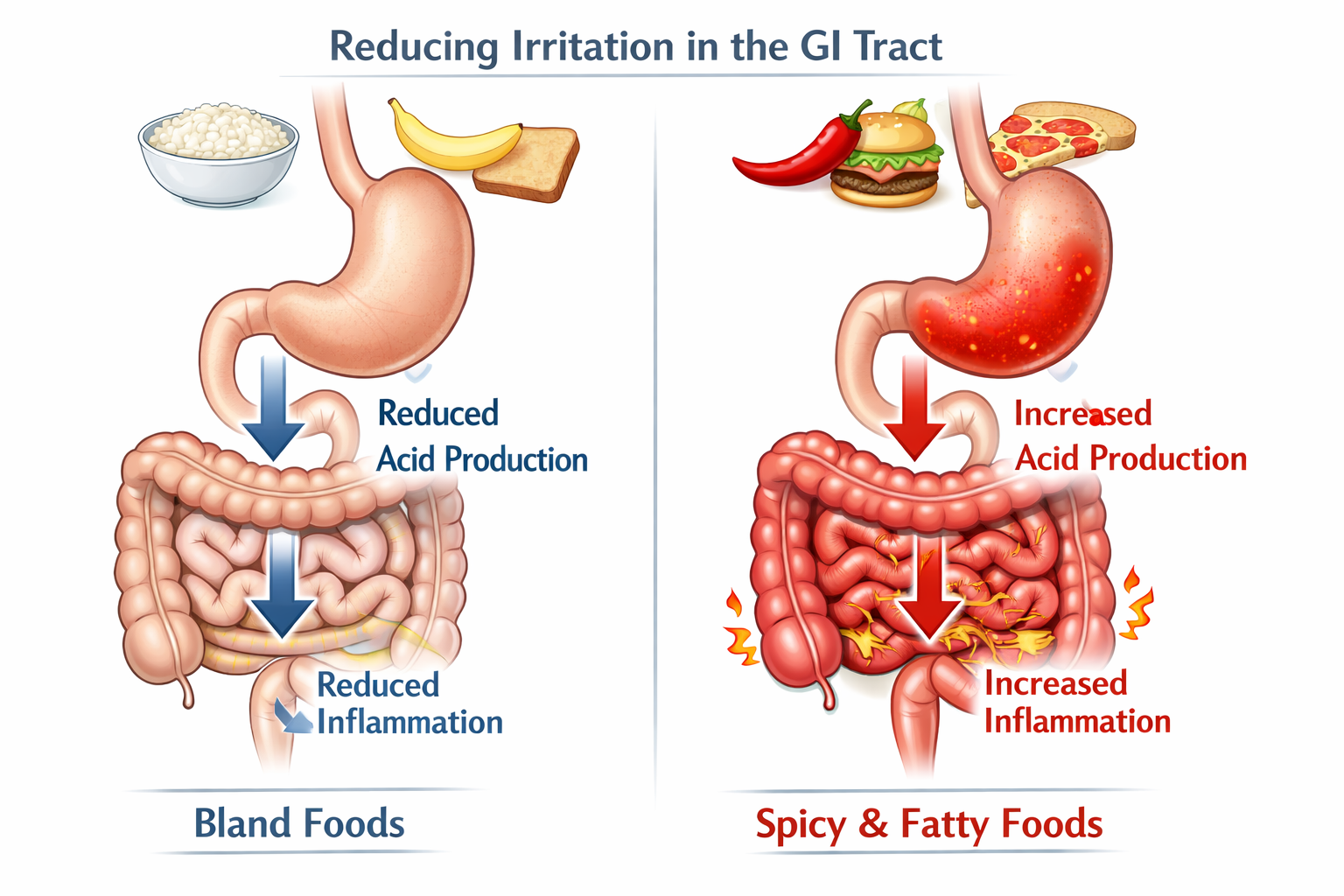
How Does a Bland Food Diet Improve Digestive Health?
The core mechanism is simple: by removing foods that irritate, inflame, or over-stimulate the GI tract, you give the gut a chance to recover. Easily digestible foods require less acid production, less muscular effort from the intestines, and cause less friction against an already-sensitive stomach lining.
Key ways the diet supports digestive recovery:
- Reduces acid production. Spicy foods, caffeine, alcohol, and high-fat meals all trigger increased stomach acid secretion. Removing them lowers the acid load on an irritated esophagus or stomach lining.
- Slows gut motility when needed. Low-fiber, low-fat foods move through the digestive tract at a steadier pace, which helps reduce diarrhea and cramping.
- Minimizes fermentation. High-fiber foods and certain vegetables (broccoli, beans, cabbage) ferment in the colon, producing gas. A bland diet limits this, reducing bloating and flatulence.
- Supports mucosal healing. Soft, non-abrasive foods are less likely to aggravate inflamed or ulcerated tissue in the stomach or intestinal lining.
For a broader look at how food choices affect gut function, our gut health and digestive wellness guide covers the science in more depth.
Common mistake: Many people assume “bland” means “nutritionally empty.” It doesn’t. A well-planned bland diet still delivers adequate protein, carbohydrates, vitamins, and minerals — just from gentler sources. The problem arises when people eat only crackers and white rice for days without including lean protein or cooked vegetables, which can lead to fatigue and slowed recovery.
What Foods Can You Eat on a Bland Diet?
The foods approved for a bland diet share three characteristics: they’re low in fat, low in fiber (or have soluble rather than insoluble fiber), and free from strong spices or acidic compounds.
Low-Fat Dairy
Low-fat dairy provides calcium, protein, and vitamin D without the fat content that can slow digestion and trigger acid reflux. Good options include:
- Skim or 1% milk
- Plain, unsweetened low-fat yogurt (also provides probiotics that support gut flora)
- Cottage cheese (low-fat)
- Mild, soft cheeses in small amounts
Avoid full-fat cheeses, cream, butter in large quantities, and flavored yogurts with added sugar or fruit pieces. If you’re lactose intolerant, lactose-free versions of these products are appropriate substitutes.
Cooked and Low-Fiber Vegetables
Raw vegetables are generally off the table during a bland diet flare-up because their insoluble fiber and tough cell walls are harder to digest. Cooking softens the fiber structure, making vegetables much gentler on the gut.
Best vegetable choices:
- Carrots (boiled or steamed) — high in soluble fiber, which forms a gel in the gut and actually helps regulate bowel movements without irritation
- Spinach (cooked) — provides magnesium, which supports smooth muscle relaxation in the intestines, and vitamin B6, which has anti-inflammatory properties
- Beets (boiled) — contain betaine, a compound that supports stomach acid balance and liver function
- Zucchini (steamed) — mild flavor, soft texture, very easy to digest
- Green beans (well-cooked) — low in fermentable compounds
- Potatoes (boiled or baked, without skin) — excellent source of easily digestible starch and potassium
Vegetables to avoid: Broccoli, cauliflower, cabbage, Brussels sprouts, onions, garlic, peppers, and corn — all of these either produce gas during digestion or contain compounds that irritate a sensitive gut.
Low-Fiber Fruits
Fruit is valuable for vitamins and natural sugars, but high-fiber or acidic fruits can worsen symptoms. The key is choosing fruits that are naturally low in fiber or have been processed to remove skin and seeds.
Approved fruits:
- Bananas — one of the most gut-friendly foods available. They’re low in fiber, easy to digest, rich in potassium (which can be depleted during diarrhea), and contain pectin, a soluble fiber that helps firm up loose stools.
- Cantaloupe and honeydew melon — high water content, gentle on the stomach, provide vitamin A and antioxidants
- Canned peaches or pears in juice (not syrup) — the canning process softens fiber, making them easier to digest than raw versions
- Applesauce (unsweetened) — another pectin-rich option that’s particularly useful for diarrhea management
- Ripe, peeled pears
Fruits to avoid: Citrus fruits (oranges, lemons, grapefruit, limes), berries with seeds (raspberries, strawberries, blackberries), pineapple, and any dried fruits — all are either too acidic, too high in fiber, or both.
Refined and Processed Grains
Whole grains are generally healthy, but during GI distress, their high insoluble fiber content can worsen symptoms. Refined grains have had the bran and germ removed, making them much easier to digest.
Good grain choices:
- White rice (particularly well-cooked)
- Plain white bread or toast
- Plain pasta or egg noodles
- Saltine crackers
- Plain oatmeal (oats contain soluble fiber, which is generally better tolerated than insoluble fiber)
- Cream of wheat or rice porridge
- Plain corn flakes or rice cereal
Grains to avoid: Whole wheat bread, brown rice, quinoa, barley, bulgur, bran cereals, granola, and any grain products with added seeds, nuts, or dried fruit.
Lean Proteins
Protein is essential for tissue repair and immune function — both critical during GI recovery. The key is choosing low-fat sources that don’t require heavy digestive effort.
Best protein options:
- Skinless chicken breast (baked, boiled, or poached — never fried)
- White fish (tilapia, cod, flounder, sole) — mild flavor, very low in fat
- Salmon — slightly higher in fat but rich in omega-3 fatty acids, which have documented anti-inflammatory effects on the gut lining
- Eggs (boiled, poached, or scrambled with minimal butter)
- Tofu (silken or firm, plain)
- Shellfish (shrimp, crab) in small amounts
For reference on the caloric content of common bland diet proteins, our breakdown of calories in hard-boiled eggs is a useful starting point.
Proteins to avoid: Fried chicken, bacon, sausage, hot dogs, fatty cuts of beef or pork, canned fish in oil, and beans or legumes (which produce gas during fermentation in the colon).
What Foods Should You Avoid on a Bland Diet?
Avoiding the wrong foods is just as important as eating the right ones. The following categories are the most common triggers for GI irritation and should be eliminated during the active phase of a bland diet.
| Category | Avoid | Why |
|---|---|---|
| Dairy | Full-fat milk, cream, butter, aged cheeses | High fat slows digestion, triggers acid reflux |
| Fruits | Citrus, berries with seeds, dried fruit, pineapple | High acid content or insoluble fiber irritates GI lining |
| Grains | Whole wheat, brown rice, quinoa, bran | Insoluble fiber increases gut motility and gas |
| Proteins | Fried meats, fatty cuts, beans, lentils | Fat and fermentable fiber worsen symptoms |
| Vegetables | Broccoli, cabbage, onions, garlic, peppers | Gas-producing compounds and irritants |
| Beverages | Alcohol, coffee, carbonated drinks, citrus juices | Stimulate acid production, irritate esophagus |
| Condiments | Hot sauce, mustard, vinegar, ketchup, pickles | Acidic or spicy — direct GI irritants |
| Fats | Deep-fried foods, heavy oils, pastries | Slow gastric emptying, worsen reflux |
One area that surprises many people: coffee. Even decaf coffee stimulates gastric acid secretion, so it’s best avoided during the active phase of a bland diet. If you’re curious about coffee’s broader health effects once you’re recovered, our article on health benefits of coffee covers both sides of the equation.
What Does a Bland Diet Meal Plan Look Like in Practice?
A practical bland diet doesn’t have to be monotonous. The key is rotating through approved foods and preparing them in ways that add some variety without reintroducing irritants.
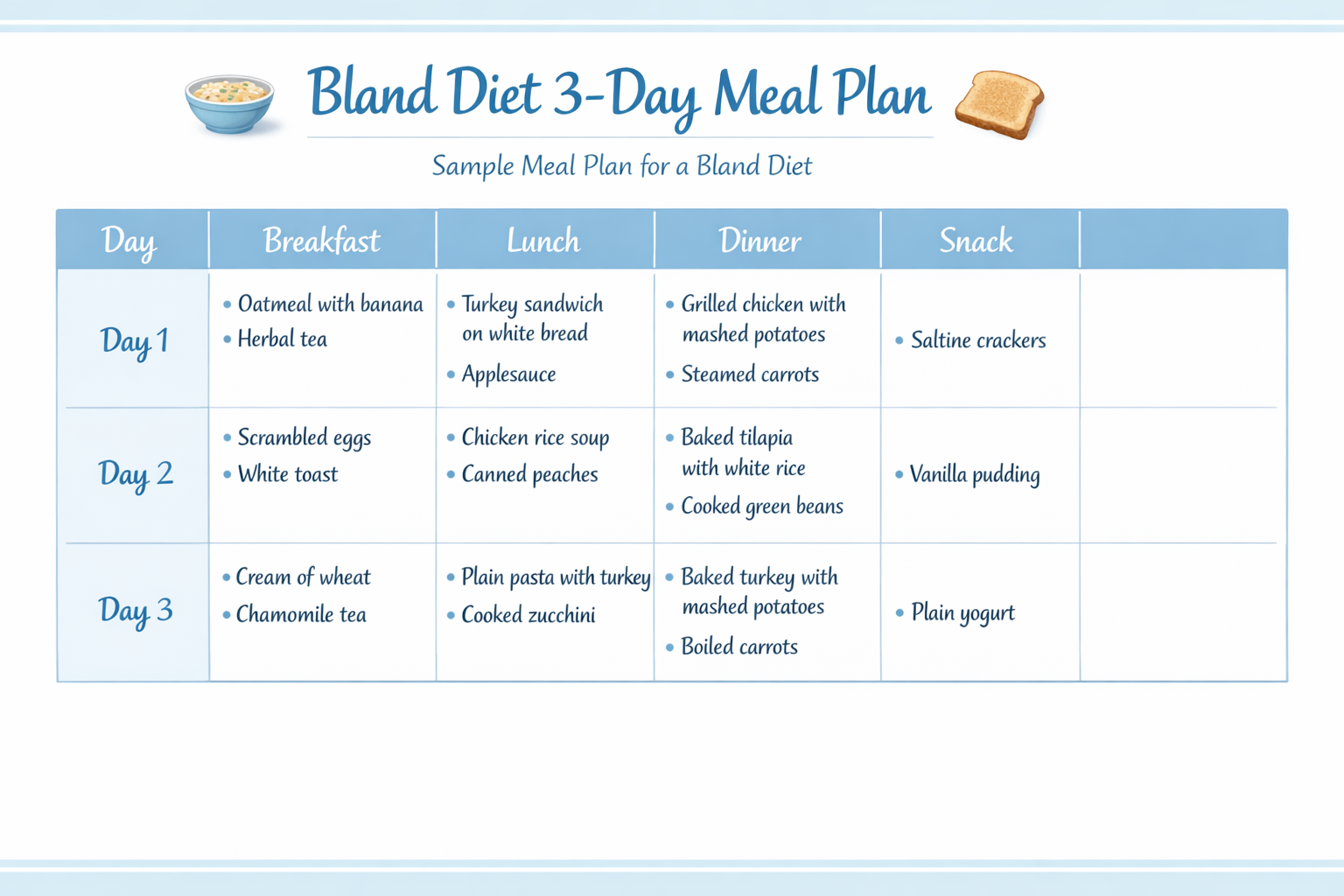
Sample 3-Day Bland Diet Meal Plan
Day 1
- Breakfast: Plain oatmeal with sliced banana and a drizzle of honey; glass of water
- Mid-morning snack: Low-fat plain yogurt
- Lunch: Chicken and white rice soup (homemade, low-sodium broth, diced carrots and celery)
- Afternoon snack: Saltine crackers with cottage cheese
- Dinner: Baked tilapia with boiled potatoes and steamed zucchini
Day 2
- Breakfast: Scrambled eggs (cooked with minimal butter) and white toast
- Mid-morning snack: Applesauce (unsweetened)
- Lunch: Plain pasta with a small amount of olive oil and steamed spinach
- Afternoon snack: Banana
- Dinner: Poached chicken breast with mashed potatoes (made with skim milk) and boiled green beans
Day 3
- Breakfast: Cream of wheat with canned peaches (in juice, drained)
- Mid-morning snack: Low-fat yogurt
- Lunch: Egg salad on white toast (made with low-fat mayo) and a side of cooked carrots
- Afternoon snack: Honeydew melon slices
- Dinner: Baked salmon with white rice and steamed beets
Practical cooking tips:
- Steam, boil, bake, or poach — never fry
- Season with small amounts of salt only; avoid pepper, chili, garlic powder, or vinegar-based sauces
- Use low-sodium broths for cooking grains and soups to add flavor without irritants
- Let hot foods cool slightly before eating — very hot temperatures can irritate an already-sensitive esophagus
For more morning meal ideas that fit within these guidelines, our bland diet breakfast ideas article has a full collection of options.
How Long Should You Follow a Bland Food Diet?
Most people follow a bland diet for a few days to two weeks, depending on the severity of their symptoms and the underlying cause. It is not designed for long-term use.
General timeline guidelines:
- Acute illness (food poisoning, stomach virus): 2–5 days, then gradually reintroduce normal foods as symptoms resolve
- Post-surgery recovery: Follow your surgeon’s specific instructions; typically 1–4 weeks depending on the procedure
- Gastritis or ulcer flare-up: 1–2 weeks during acute phase, with gradual reintroduction guided by a doctor
- GERD management: Some GERD patients maintain a modified bland diet long-term, but this should be tailored individually with a gastroenterologist
How to reintroduce foods: Add one new food every 1–2 days and monitor for symptom return. Start with lower-risk additions (cooked vegetables, low-fat proteins) before reintroducing higher-risk items (raw vegetables, acidic fruits, whole grains). If a food triggers symptoms, remove it and wait another few days before trying again.
Edge case: Some people feel significantly better on a bland diet and want to continue it indefinitely. This is not advisable without medical supervision. Long-term restriction of fiber, healthy fats, and diverse plant foods can negatively affect gut microbiome diversity, which is linked to broader immune and metabolic health.
What Lifestyle Changes Support a Bland Diet?
Diet alone does most of the work, but several lifestyle adjustments can meaningfully accelerate GI recovery and reduce the risk of symptom recurrence.
Eating Habits
- Eat smaller, more frequent meals. Large meals increase gastric pressure and can worsen reflux and bloating. Aim for 5–6 small meals rather than 3 large ones.
- Eat slowly and chew thoroughly. Rushing through meals increases the amount of air swallowed (a contributor to bloating) and puts more digestive burden on the stomach.
- Don’t lie down immediately after eating. Wait at least 2–3 hours before lying down to reduce acid reflux risk. Elevating the head of your bed by 6–8 inches can also help if nighttime reflux is a problem.
- Avoid eating within 2 hours of bedtime.
Hydration
Staying well-hydrated is especially important on a bland diet because low-fiber eating can contribute to constipation, and conditions like diarrhea and vomiting cause fluid loss.
Best fluid choices:
- Plain water (the gold standard)
- Herbal teas (chamomile, ginger, peppermint — all have documented soothing effects on the GI tract)
- Clear broths (low-sodium)
- Diluted fruit juices (apple juice, not citrus)
- Coconut water (natural electrolytes, useful after vomiting or diarrhea)
Avoid: Carbonated drinks (the gas worsens bloating), coffee, alcohol, and full-strength citrus juices.
For additional natural approaches to calming digestive discomfort, our guide on ways to soothe your stomach naturally covers herbal and lifestyle strategies that pair well with a bland diet.
Stress Management
The gut-brain axis is well-established in gastroenterology research. Psychological stress directly affects gut motility, acid secretion, and intestinal permeability. Managing stress isn’t optional for people with chronic GI conditions — it’s part of the treatment.
Practical approaches include:
- Diaphragmatic breathing exercises before meals
- Light physical activity (short walks, gentle yoga) — vigorous exercise during acute GI distress can worsen symptoms
- Adequate sleep (7–9 hours for most adults), since sleep deprivation increases cortisol, which disrupts gut function
- Mindfulness-based stress reduction (MBSR), which has shown benefit in IBS research
Weight Management
Excess body weight, particularly abdominal fat, increases intra-abdominal pressure and worsens GERD and gastritis symptoms. Gradual, sustainable weight reduction can reduce symptom burden for overweight individuals with chronic GI conditions. Our weight loss guide outlines approaches that can be adapted to work alongside a bland diet.
How Does a Bland Diet Compare to Other Therapeutic Diets?
Understanding where the bland diet fits relative to other GI-focused eating plans helps you choose the right approach for your specific situation.
| Diet | Primary Goal | Key Restriction | Best For |
|---|---|---|---|
| Bland diet | Reduce GI irritation | Spice, fat, fiber, acid | Acute GI illness, ulcers, post-surgery |
| Low-FODMAP diet | Reduce fermentable carbs | Specific sugars (fructose, lactose, etc.) | IBS, SIBO |
| GERD diet | Reduce acid reflux | Acidic, fatty, and trigger foods | Chronic acid reflux |
| Soft food diet | Ease chewing/swallowing | Texture only (not flavor) | Dental issues, dysphagia |
| Anti-inflammatory diet | Reduce systemic inflammation | Processed foods, refined sugar | Chronic inflammation, IBD |
The bland diet overlaps with several of these but is the most restrictive short-term option. For people with IBS, the low-FODMAP diet (developed by Monash University researchers) has stronger evidence for long-term symptom management. For chronic inflammation beyond the GI tract, our anti-inflammatory foods guide covers a broader dietary approach.
Choose a bland diet if: You’re dealing with an acute flare-up, recovering from illness or surgery, or need a short-term reset while your gut heals.
Consider alternatives if: Your symptoms are chronic, you’ve already tried a bland diet without lasting improvement, or your condition (like IBS or Crohn’s disease) has a more specific evidence-based dietary protocol.
What Are the Most Common Mistakes People Make on a Bland Diet?
Even well-intentioned bland diet attempts can go wrong. Here are the most frequent errors and how to avoid them.
1. Eating only crackers and white rice
This is the most common mistake. People interpret “bland” as “eat almost nothing” and end up under-eating protein and micronutrients. A proper bland diet includes lean protein at every meal and a variety of cooked vegetables.
2. Continuing to drink coffee or carbonated beverages
Both stimulate gastric acid and worsen reflux. Many people don’t realize that even “just one cup” of coffee can undermine progress, especially in the first few days.
3. Using the diet as a long-term solution
If your symptoms return every time you reintroduce normal foods, that’s a signal to investigate the underlying cause — not to stay on a bland diet indefinitely. Persistent symptoms warrant a gastroenterology referral.
4. Ignoring portion size
Even bland foods can cause symptoms if eaten in large quantities. A large meal of plain chicken and rice can still trigger bloating and reflux if it overfills the stomach.
5. Assuming all “healthy” foods are bland-diet safe
Whole grains, raw vegetables, nuts, seeds, legumes, and high-fiber fruits are all considered healthy in most contexts — but they’re inappropriate during a bland diet flare-up. “Healthy” and “bland-diet appropriate” are not the same thing.
6. Not staying hydrated
Low-fiber eating can slow bowel transit and cause constipation. Drinking adequate water throughout the day is essential to keep things moving at a healthy pace.
Frequently Asked Questions About Bland Food Diets
Q: How long does it take for a bland diet to relieve symptoms?
Most people notice improvement within 24–72 hours for acute conditions like food poisoning or gastroenteritis. For chronic conditions like gastritis or GERD, meaningful symptom reduction typically takes 1–2 weeks of consistent adherence.
Q: Can I eat eggs on a bland diet?
Yes. Eggs are one of the best protein sources for a bland diet. Boiled, poached, or scrambled (with minimal butter) are all appropriate. Avoid fried eggs or eggs cooked with spices, onions, or peppers.
Q: Is oatmeal allowed on a bland diet?
Plain oatmeal is generally well-tolerated on a bland diet because it contains soluble fiber (beta-glucan), which is gentler than insoluble fiber. Avoid adding nuts, seeds, dried fruit, or honey in large amounts during the acute phase.
Q: Can I drink tea or coffee on a bland diet?
Herbal teas (chamomile, ginger, peppermint) are encouraged. Regular coffee — including decaf — stimulates gastric acid and should be avoided. Black tea is also best avoided due to its caffeine and tannin content.
Q: Is a bland diet the same as a soft food diet?
No. A soft food diet restricts texture only (for people with chewing or swallowing difficulties) and doesn’t necessarily limit spice, fat, or acid. A bland diet restricts the chemical and compositional properties of food to reduce GI irritation, regardless of texture.
Q: Can I eat yogurt on a bland diet?
Plain, low-fat yogurt is not only allowed — it’s beneficial. It provides protein, calcium, and live probiotic cultures that support gut microbiome recovery. Avoid flavored yogurts with added sugar, fruit pieces, or granola.
Q: What can I drink besides water on a bland diet?
Good options include herbal teas, diluted apple juice, clear broths (low-sodium), and coconut water. Avoid carbonated drinks, alcohol, coffee, and citrus juices.
Q: Is salmon okay on a bland diet?
Yes, in moderate portions. Salmon is higher in fat than white fish like tilapia or cod, but the fat is primarily omega-3 fatty acids, which have anti-inflammatory effects. Baked or poached salmon without seasonings is appropriate for most people on a bland diet.
Q: Can children follow a bland diet?
Yes, with appropriate portion adjustments. The BRAT diet (bananas, rice, applesauce, toast) is a simplified version of the bland diet commonly recommended for children with stomach illness. Always consult a pediatrician before making significant dietary changes for a child.
Q: Will a bland diet help with IBS?
A bland diet may reduce acute IBS symptoms, but it’s not the most evidence-based long-term approach for IBS. The low-FODMAP diet has significantly stronger clinical evidence for IBS management. If IBS is your primary concern, discuss the low-FODMAP approach with a registered dietitian.
Q: Can I season food at all on a bland diet?
Small amounts of salt are generally acceptable. Some people tolerate mild herbs like parsley or dill without issue. Avoid pepper, chili, garlic, onion powder, vinegar-based sauces, and any “spicy” seasoning blends.
Q: When should I see a doctor instead of just following a bland diet?
See a doctor if symptoms persist beyond 2 weeks, if you experience blood in stool or vomit, if you have unexplained weight loss, if you develop severe abdominal pain, or if you’re unable to keep fluids down for more than 24 hours. A bland diet manages symptoms — it doesn’t diagnose or treat underlying conditions.
Sources
- MedlinePlus (U.S. National Library of Medicine). “Bland Diet.” medlineplus.gov — Accessed 2026.
- Cleveland Clinic. “Gastrointestinal Diseases.” my.clevelandclinic.org — Accessed 2026.
- Harvard T.H. Chan School of Public Health. “Whole Grains.” The Nutrition Source. hsph.harvard.edu — Accessed 2026.
- Healthline. “Lean Protein Foods.” healthline.com — Accessed 2026.
Related reading: Gut Health and Digestive Wellness | 10 Ways to Soothe Your Stomach Naturally | Bland Diet Breakfast Ideas | Anti-Inflammatory Foods Guide | Healthy Meals for Weight Loss




